The central nervous system (CNS) may be the target of detrimental cellular and humoral immune responses in the case of autoimmune disease. These immune-mediated autoimmune disorders occur in paraneoplastic and non-paraneoplastic contexts, creating a vast and heterogeneous distribution.1 One of the most common paraneoplastic neurological syndromes (PNS) is paraneoplastic cerebellar degeneration (PCD), including various neurological disorders presenting with cerebellar dysfunction. It is characterized by subacute pan-cerebellar symptoms in patients who usually begin with gait ataxia followed by dysarthria, nystagmus, and appendicular ataxia.2 Neurological dysfunction may occur before detecting the underlying cancer or up to several years after detection.3 Therefore, neurologists need to have a high level of suspicion, leading to early detection of associated cancer. Early detection and localization of the primary malignancy are necessary to eliminate the underlying cause and prevent metastasis.4 Positron emission tomography (PET) using 18 F-fluorodeoxyglucose (FDG) is an effective diagnostic tool in the early detection of primary tumors.5 On the other hand, many recently published studies have reported that PET has significantly high sensitivity and specificity to detect primary malignancies and thus high accuracy in confirming the diagnosis of PCD.6 To the best of our knowledge, we discuss an anti-YO antibody positive female patient, one of the anti-onconeural antibodies found in PCD patients, presenting with acute PCD symptoms as the first manifestation of malignancy. The value of PET in the diagnosis and follow-up of PCD and long-term outcomes of the disease will be highlighted in a patient in whom we had difficulty detecting the primary malignancy.
A 43-year-old woman who presented with eight weeks of progressive vertigo, diplopia, and ataxia was admitted to our clinic. Her initial complaints were dizziness, nausea, and vomiting, and they were progressed within a month. Over time, she had trouble keeping her balance and mobilized with assistance. Contrast-enhanced brain magnetic resonance imaging (MRI) showed no features (Fig. 1G-H). In cerebrospinal fluid (CSF) analysis, anti-YO antibodies were detected in CSF. Tumor markers were negative, and there was no weight loss. Chest and abdomen CT were performed, and left axillary lymphadenopathies were observed (Fig. 1A). Mammography and breast ultrasound were evaluated as within normal limits; axillary ultrasound confirmed pathological lymph nodes in the left axilla. Fine needle and tru-cut biopsy were performed from the pathological axillary lymph node. Malignant epithelial cells were observed in cytology, and the immunohistochemical study supported primary breast carcinoma. Pathological FDG uptake in the left axilla was confirmed in the FDG-PET examination (Fig. 1A, C–D). However, right cerebellar asymmetric hypermetabolism was noted (Fig. 1E–F). After neoadjuvant chemotherapy and rituximab immunotherapy, left modified radical mastectomy and axillary lymph node dissection were performed. There was no significant improvement in cerebellar findings, and the patient could not be ambulated after treatments. Currently, the patient continues chemoimmunotherapy and adjuvant radiotherapy treatment. Although early-stage brain MRI was evaluated within normal limits, cerebellar atrophy was observed in the control brain MRI examination one year later (Fig. 2D–E). Similarly, although cerebellar hypermetabolism was noted in the early period PET examination, it showed cerebellar hypometabolism in the one-year follow-up (Fig. 2A–C).
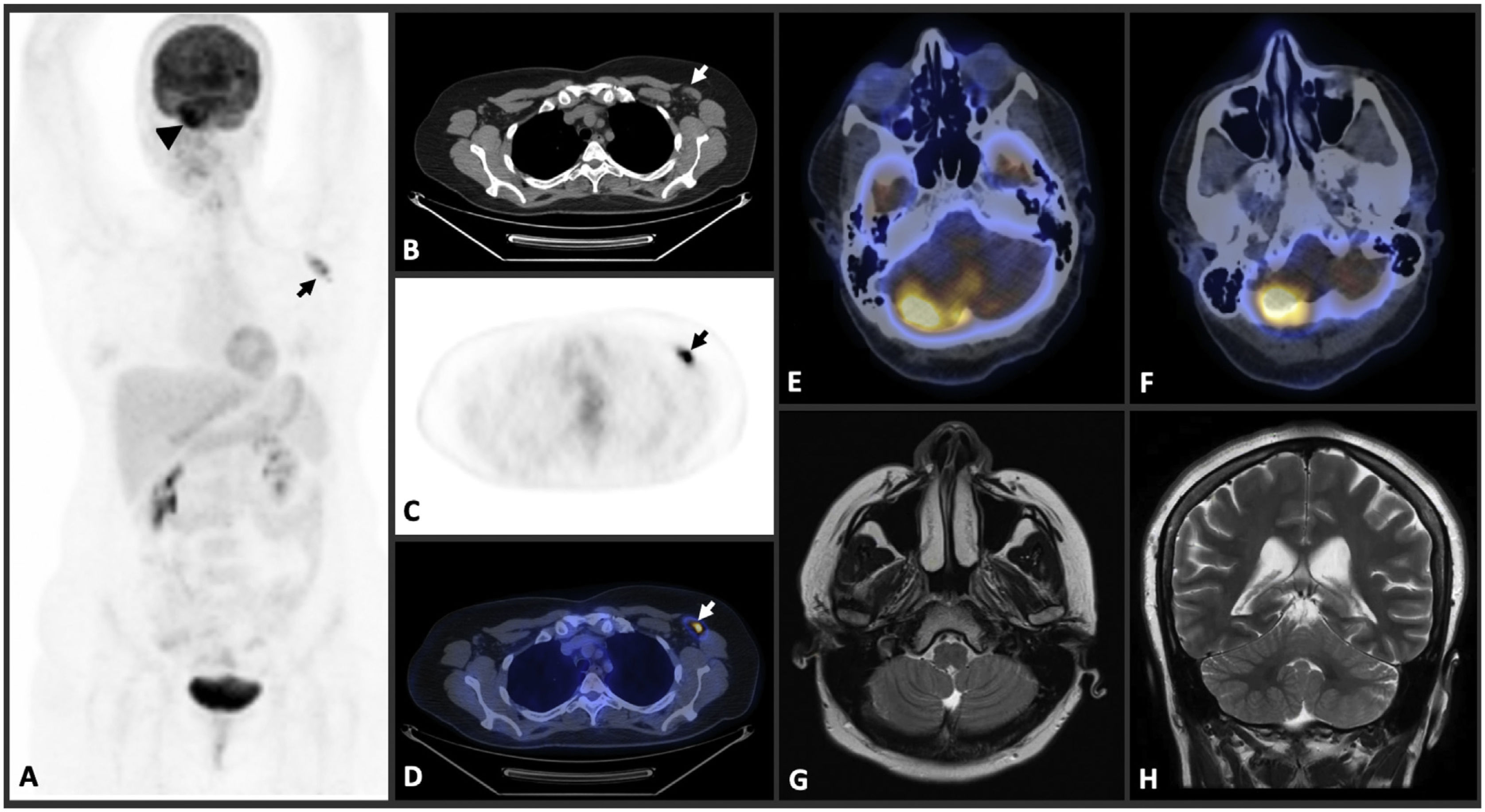
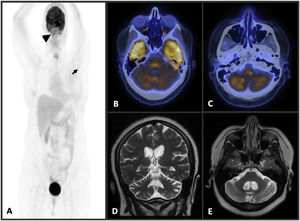
A maximum intensity projection (MIP) PET image (A) shows increased 18 F-fluorodeoxyglucose (FDG) uptake in right cerebellum (SUV max:20) (arrowhead) and left axillary lymph node (SUV max:7) (arrow). Axial thorax CT (B), PET (C), and fusion PET-CT (D) images reveal increased FDG uptake in left axillary lymph node. Fusion PET-CT images of brain (E, F) demonstrate increased FDG uptake in right cerebellum. T2W coronal (G) and axial (H) brain MR imaging show no features.
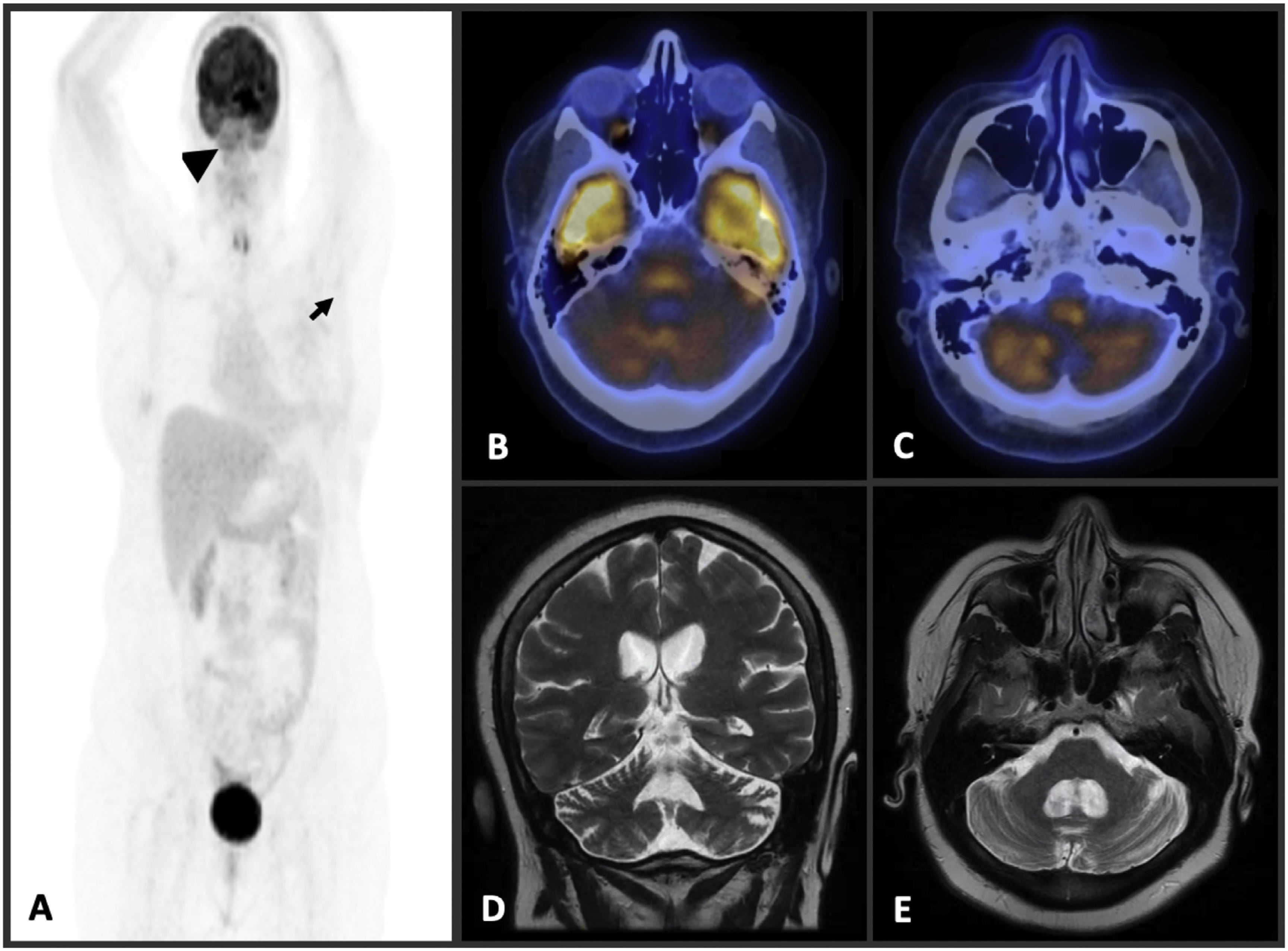
A maximum intensity projection (MIP) PET image (A) reveals no sign of residual malignant disease (arrows). Fusion PET-CT images of brain (B, C) show diffuse bilateral decreased 18 F-fluorodeoxyglucose (FDG) uptake in cerebellum. T2W coronal (D) and axial (E) brain MR imaging demonstrate diffuse cerebellar atrophy.
PCD is a heterogeneous group, and cases differ in clinical features, prognosis, associated tumor, and associated antibodies. Cerebellar degeneration seems to be the predominant presentation and its pathophysiology is based on the formation of autoantibodies.7 Brain MRI is usually normal at the onset of the disease, as in our case report, and does not help diagnose PCD. In some cases, cerebellar atrophy has been demonstrated on MRI at later stages.3 The role of FDG-PET in PNS is under development. Increasingly, the potential of this modality is being highlighted in various reports.5,6 Choi et al. have reported a case with cerebellar hypermetabolism instead of hypometabolism consistent with FDG-PET. It was assumed that this was due to an acute inflammatory process associated with an immunological reaction.8 Additionally, Sharma et al. have also reported an antibody negative unique PCD case who had normal brain MRI.9 They showed the role of FDG-PET by demonstrating diffuse intense cerebellar hypermetabolism.9 Similarly, in our case, cerebellar hypermetabolism was observed in the early phase of PCD. This is probably related to the inflammatory response observed in the early stage, which could not be detected in brain MRI.10 In one-year follow-up of our case, cerebellar atrophy accompanied with cerebellar hypometabolism occurred. Development of cerebellar atrophy has been reported in patients with PCD; however, this finding is far from being diagnostic since it only occurs in the advanced stages of the disease. The use of PET in the early stage of PCD appears to be an alternative biomarker for antibody negative or MRI normal early-stage patients.
Ethics statementInformed written consent was obtained from the patient.
DisclosuresThe authors report no disclosure relevant to the manuscript.
FundingNone.
Declaration of interestThe authors have no conflict of interest.
None.