Optic neuropathy is a possible, although very infrequent, complication of orbital decompression surgery.
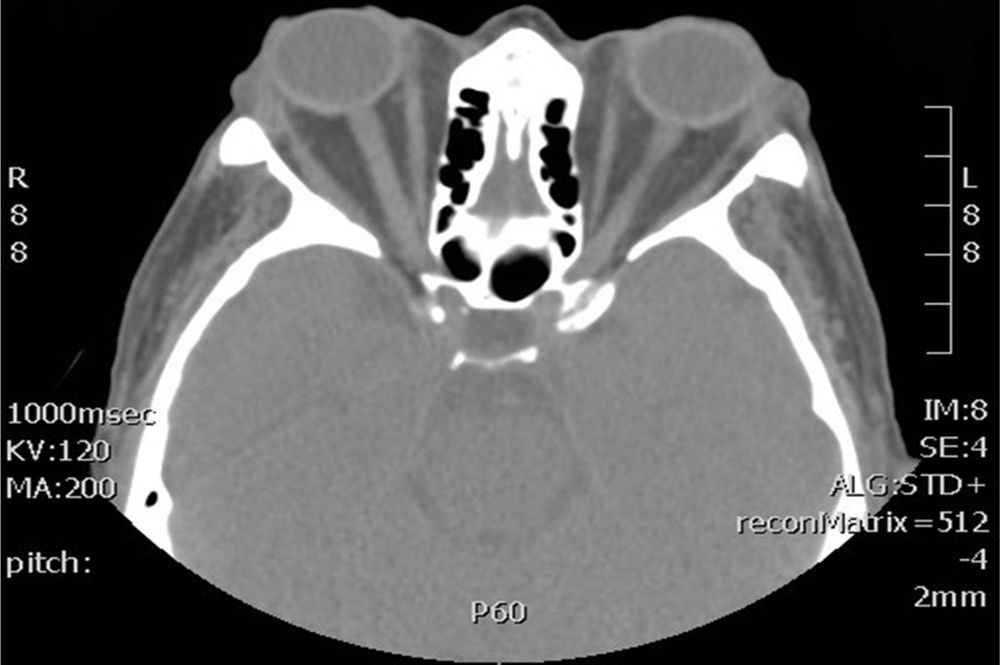
We present the case of a 62-year-old woman with hyperthyroidism and long-standing thyroid-associated orbitopathy due to diffuse and nodular hyperplasia of the thyroid gland. The patient had been previously treated with steroids and total thyroidectomy to control symptoms. Exophthalmos was measured at 25mm in the right eye (RE) and 23mm in the left eye (LE) (Fig. 1). We also observed mild lid retraction and a bilateral supraduction deficit. At that time, our patient was being treated with topical ocular hypotensive medication for chronic bilateral open-angle glaucoma that had been stable for 4 years.
In her last examination before surgery, we recorded intraocular pressure (IOP) of 18mmHg in both eyes, as well as optic disc cupping of 0.6 and 0.4mm in the RE and LE, respectively. Results from both the campimetry study and the optical coherence tomography (OCT) performed before surgery were normal.
The patient underwent orbital decompression surgery of the RE; the medial wall and orbital floor were removed endoscopically through the nasal cavity while the lateral wall was removed by the external approach. There were no complications.
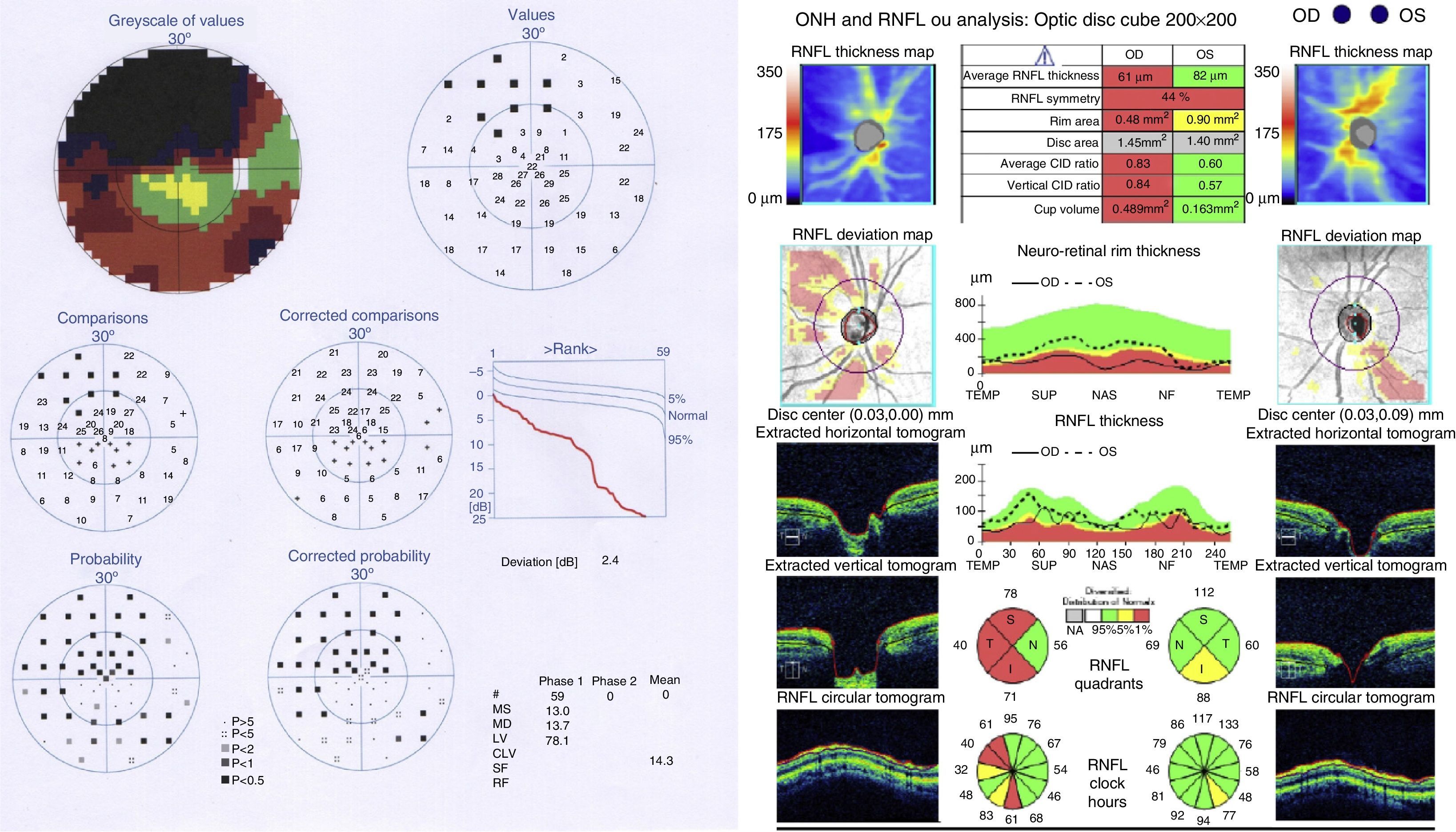
One week after the surgery, the patient reported loss of visual acuity, but findings from the ophthalmological examination were identical to those from the previous one except for decreased IOP in the RE (14mmHg). We performed tendency oriented perimetry (TOP) of the central 30° visual field, which revealed an altitudinal scotoma of the LE visual field. An OCT of the optic nerve fibre layer showed reduced thickness of that layer (Fig. 2). In light of these data, our diagnosis was ischaemic optic neuropathy possibly associated with the orbital decompression surgery.
Orbital decompression surgery is a therapeutic option for thyroid orbitopathy.1 This procedure is generally performed after failure of corticosteroid treatment or radiotherapy during the active phase of the disease when vision is highly impaired, mainly due to compressive optic neuropathy. This procedure is also performed during the inactive phase to surgically correct sequelae, mainly consisting of keratitis due to corneal exposure, proptosis causing diplopia, and cosmetic disfigurement.2,3 The procedure involves surgically opening orbital walls to create more space for the eye4,5 and thus reduce proptosis and IOP.6 Some of its more frequent complications are (generally) transient infraorbital nerve hypaesthesia,2 sinusitis, epistaxis, oedema, and haematoma of the lids. New diplopia can occasionally develop and it usually resolves, although strabismus surgery may be required.2
Ischaemic optic neuropathy has been described as an infrequent complication of orbital decompression surgery.6,7 Studies have suggested that this may be due to a direct intraoperative lesion to the optic nerve or to intraoperative increased IOP.7
Please cite this article as: Asorey-García A, Martínez-Chico R, Santos-Bueso E, García-Feijoo J. Neuropatía óptica tras la cirugía de descompresión orbitaria. Neurología. 2016;31:62–64.