Sertraline (SRT) is an antidepressant that has proven its activity in vitro against Cryptococcus, Coccidioides, Trichosporon and other fungi. Disseminated sporotrichosis, although rare, has a high mortality and its treatment is difficult and prolonged, often relying in combining two or more antifungals.
AimsIn our study we evaluate the antifungal activity of SRT, alone and in combination with itraconazole (ITC), voriconazole (VRC) and amphotericin B (AMB), against 15 clinical isolates of Sporothrix schenckii.
MethodsWe used the broth microdilution method as described by the CLSI to test the susceptibility to antifungals, and the checkerboard microdilution method to evaluate drug interactions.
ResultsThe minimum inhibitory concentration (MIC) with SRT was in the range of 4–8μg/ml, while for AMB, VRC and ITC were 0.5–4μg/ml, 0.5–8μg/ml and 0.125–2μg/ml, respectively. In addition, SRT showed synergy with ITC in one strain, mainly additivity with VRC, and indifference with AMB in others.
ConclusionsThe MIC values with SRT for the isolates studied show the potential role of this drug as an adjuvant in the treatment of sporotrichosis, especially in disseminated or complicated cases.
La sertralina (SRT) es un antidepresivo que ha demostrado actividad in vitro contra Cryptococcus, Coccidioides, Trichosporon y otros hongos. La esporotricosis diseminada, aunque rara, tiene una mortalidad elevada y su tratamiento es complicado, requiriendo, a menudo, la combinación de dos o más antifúngicos.
ObjetivosEn este estudio evaluamos la actividad antifúngica de SRT, sola y en combinación con itraconazol (ITC), voriconazol (VRC) y anfotericina B (AMB), frente a 15 aislamientos clínicos de Sporothrix schenckii.
MétodosSe usó la técnica de microdilución en caldo para evaluar la sensibilidad a los antifúngicos y el método de tablero de damas para las interacciones entre estos fármacos.
ResultadosLa concentración mínima inhibitoria (CMI) de SRT estuvo en el rango de 4-8μg/ml, mientras que para AMB, VRC e ITC fue de 0,5–4 μg/ml, 0,5–8 μg/ml y 0,125–2 μg/ml, respectivamente. La SRT mostró sinergia con ITC frente a una cepa, efecto aditivo principalmente con VRC, e indiferencia con AMB.
ConclusionesLos valores de la CMI de SRT para los aislamientos ensayados son indicativos del potencial de este fármaco como adyuvante en el tratamiento de la esporotricosis, especialmente en casos complicados o de enfermedad diseminada.
Sporotrichosis is a deep subcutaneous mycotic infection caused by Sporothrix schenckii species complex that usually presents as localized cutaneous or subcutaneous disease. The drugs of choice include itraconazole, potassium iodide, amphotericin B and terbinafine, but their adverse effects, high price or restricted distribution represent a challenge.4,9,13,14
Disseminated sporotrichosis has been associated with HIV/AIDS, uncontrolled diabetes and, in general, with impaired cellular immunity. Infection of the central nervous system (CNS) is one of the deadliest presentations of this disease. The usual treatment is based on the use of amphotericin B, but some studies have reported resistance. In HIV/AIDS-associated disease therapy varies when compared with immunocompetent patients, relying in the use of combination treatment, but mortality as high as 30% has been described.1–3,7,18,21 Sertraline (SRT) is an antidepressant with a worldwide distribution and an excellent tolerability profile. A certain antifungal activity has been recently found in this agent.8,20,23,24
Combination therapy is a common standard in the management of multiple diseases, and the combination agents are chosen empirically. In this sense, synergy testing methods evaluate the combination of two or more drugs in comparison to its individual components.16,19 In this study we seek to study the activity of SRT against clinical isolates of S. schenckii and its combination with antifungals often used for the treatment of this infection.
Fifteen clinical isolates of S. schenckii collected from patients from the following states of Mexico, Puebla, Oaxaca, San Luis Potosi, Coahuila, Nuevo Leon, and Mexico City, were evaluated. Ten strains were isolated from male patients and five from females. One of them (16-021) belonged to a patient with disseminated sporotrichosis. These were previously identified by standard phenotypical procedures and sequencing of the calmodulin gene fragment (sequences are available in GenBank, refer to Table 1 for accession numbers).15 Sequences were compared using NCBI-BLAST (https://blast.ncbi.nlm.nih.gov/Blast.cgi). The strains were stored as suspensions in sterile distilled water at room temperature, cultured for 7 days on Sabouraud-dextrose agar (SDA) at 30°C, and then sub-cultured before use. Conidia were collected by scraping gently the surface of the plate and then suspended in sterile water. The turbidity of the supernatants was spectrophotometrically measured at 530nm (UNICO Basic Visible Spectrophotometer 1100RS. Princeton, NJ, USA), and the transmittance was adjusted to 80–82%. Each suspension was diluted 1:50 in RPMI 1640 with l-glutamine and buffered with 165mM MOPS (Hardy Diagnostics) to obtain two times the final inoculum size.
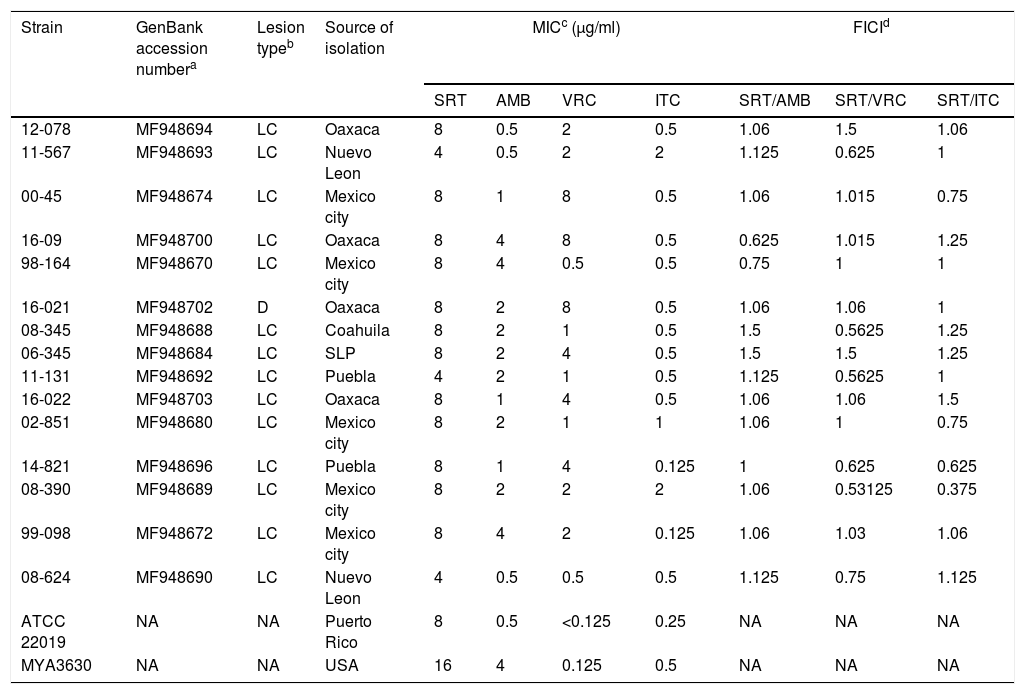
Antifungal susceptibility and synergistic effect of SRT against clinical isolates of Sporothrix schenckii.
| Strain | GenBank accession numbera | Lesion typeb | Source of isolation | MICc (μg/ml) | FICId | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| SRT | AMB | VRC | ITC | SRT/AMB | SRT/VRC | SRT/ITC | ||||
| 12-078 | MF948694 | LC | Oaxaca | 8 | 0.5 | 2 | 0.5 | 1.06 | 1.5 | 1.06 |
| 11-567 | MF948693 | LC | Nuevo Leon | 4 | 0.5 | 2 | 2 | 1.125 | 0.625 | 1 |
| 00-45 | MF948674 | LC | Mexico city | 8 | 1 | 8 | 0.5 | 1.06 | 1.015 | 0.75 |
| 16-09 | MF948700 | LC | Oaxaca | 8 | 4 | 8 | 0.5 | 0.625 | 1.015 | 1.25 |
| 98-164 | MF948670 | LC | Mexico city | 8 | 4 | 0.5 | 0.5 | 0.75 | 1 | 1 |
| 16-021 | MF948702 | D | Oaxaca | 8 | 2 | 8 | 0.5 | 1.06 | 1.06 | 1 |
| 08-345 | MF948688 | LC | Coahuila | 8 | 2 | 1 | 0.5 | 1.5 | 0.5625 | 1.25 |
| 06-345 | MF948684 | LC | SLP | 8 | 2 | 4 | 0.5 | 1.5 | 1.5 | 1.25 |
| 11-131 | MF948692 | LC | Puebla | 4 | 2 | 1 | 0.5 | 1.125 | 0.5625 | 1 |
| 16-022 | MF948703 | LC | Oaxaca | 8 | 1 | 4 | 0.5 | 1.06 | 1.06 | 1.5 |
| 02-851 | MF948680 | LC | Mexico city | 8 | 2 | 1 | 1 | 1.06 | 1 | 0.75 |
| 14-821 | MF948696 | LC | Puebla | 8 | 1 | 4 | 0.125 | 1 | 0.625 | 0.625 |
| 08-390 | MF948689 | LC | Mexico city | 8 | 2 | 2 | 2 | 1.06 | 0.53125 | 0.375 |
| 99-098 | MF948672 | LC | Mexico city | 8 | 4 | 2 | 0.125 | 1.06 | 1.03 | 1.06 |
| 08-624 | MF948690 | LC | Nuevo Leon | 4 | 0.5 | 0.5 | 0.5 | 1.125 | 0.75 | 1.125 |
| ATCC 22019 | NA | NA | Puerto Rico | 8 | 0.5 | <0.125 | 0.25 | NA | NA | NA |
| MYA3630 | NA | NA | USA | 16 | 4 | 0.125 | 0.5 | NA | NA | NA |
Voriconazole (VRC; Pfizer, Inc., New York, NY, USA), amphotericin B (AMB; Bristol-Myers Squibb, Princeton, NJ, USA), sertraline (SRT, TCI Chemicals Inc., New York, NY, USA) and itraconazole (ITC; Wako Pure Chemicals, Osaka, Japan) were obtained in reagent grade powder. Stock solutions of the drugs were made at 5mg/ml in dimethyl sulfoxide and stored at −80°C.
Antifungal susceptibility testing was conducted using the plate microdilution method according to document M38-A3 of the CLSI.5 The final drug concentrations ranged from 0.125 to 16μg/ml for VRC, ITC and AMB, and from 0.5 to 32μg/ml for SRT. Candida parapsilosis ATCC-22019 and Paecilomyces variotii MYA-3630 were used as quality control organisms. The checkerboard microdilution method was used to evaluate the activity of the combination of SRT and the antifungals (AMB, VRC and ITC). Drug interactions were defined in the basis of the fractional inhibitory concentration index (FICI): FIC A (MIC drug A in combination/MIC drug A alone)+FIC B (MIC drug B in combination/MIC drug B alone). Synergy was defined as a FICI≤0.5, additivity as a FICI >0.5 and ≤1.0, antagonism as a FICI>4.0, and no interaction as a FICI >1.0 and ≤2.0. The fractional inhibitory concentration (FIC) was determined as the concentration in the well that showed complete inhibition of growth compared visually with the controls; if more than one well showed similar inhibition, the well with the lowest FIC value was selected.17,19
The MIC for SRT was in the range 4–8μg/ml. The susceptibility of AMB ranged 0.5–4μg/ml, 0.5–8μg/ml for VRC, and 0.125–2μg/ml for ITC. The combination of SRT and ITC showed a FICI value considered synergistic in one strain, and the other combinations presented additivity for many of the isolates assayed. None of the combinations tested presented antagonism (Table 1).
In our study, all isolates of S. schenckii exhibited MICs comparable to those previously reported for Cryptococcus, Trichosporon and Coccidioides immitis, and the antifungal activity was greater than that described for Aspergillus and Candida.6,10,11,22,24 In the combination study no antagonism was shown with the antifungal combinations tested; one strain exhibited synergism with ITC and an additive effect was observed in many other strains for different antifungal combinations. In other in vitro studies SRT showed a fungicidal activity proven by time-course assays of cell viability, and a higher potency in combination with azoles.24 In our study, SRT alone showed an evident antifungal effect. Although we did not find any relevant combinatory activity in all the tested strains, synergy has been described in vivo even though it was not present in vitro. Moreover, SRT has the ability to reach 40–60 times its normal serum concentration in the CNS and the lung tissue.12,17,19 In conclusion, due to the potent antifungal activity SRT presented in this study, we can hypothesize that SRT could be a viable option as an adjuvant in the treatment of sporotrichosis, especially in the disseminated disease where lung and CNS involvement is common and the therapeutic approach is complicated. Further studies must be performed in order to determine the utility of this drug.
Funding sourcesThis work was supported by internal resources of the Department of Microbiology, School of Medicine, UANL.
Conflict of interestThe authors declare they have no conflict of interest.
Special thanks to Christian L. Campos Cortés, M.Sc. for her technical assistance.