To identify the correlation between nurse's perception of the continuing professional development (CPD) and the satisfaction of nursing career ladder system (NCLS) implementation.
MethodA non-experimental survey design was used for this study. The respondents were selected using proportional random sampling technique with the total sample size of 149 nurses. Data were measured using proportion, central tendency and Pearson product-moment correlation.
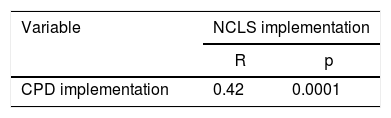
ResultsThere was a moderate, positive correlation between the CPD and the NCLS satisfaction (R: 0.42, p= 0.0001).
ConclusionsThe results of this research should be used as recommendation for improving CPD at the hospitals in Indonesia.
Nursing is the pivotal element of health care service quality. Nurses are the frontier of health care delivery as they work with the patients on 24/7 basis, thus making them most likely to leave tangible impacts on patient outcome and experiences during hospitalization1,2. Nurses make up the largest part of the multidisciplinary health care team, aiming at addressing a wide array of patient's needs, covering the biological, psychological, social, cultural, and spiritual extents3. Therefore, nurse's competency must meet certain standards to ensure quality and safe care for patients4,5.
Nurses also have the principles of professional and ethical conduct to prevent or minimize errors. Nurses play the most critical contribution to patient safety6 by coordinating and integrating the multiple dimensions of quality of care provided by nurses and other health professionals6. As the safety net on patient care, nurses must be competent not only in undertaking the clinical procedures but also in the cognitive, attitude, and skill capacities, as well as in clinical judgment5. As a consequence, nurses need to keep up with the updates on knowledge, technology, and evidences pertinent to nursing practice6.
Improving nurse competence can be achieved through various continuing professional development (CPD) activities. The old concept of CPD was mostly concerned with how to make every nurse get the training on the basis of hospital's predesigned programs, without considering the existing need, competence gap, or even the clinical assignment of the nurse. CPD is ideally conducted according to the training assessment and the clinical assignment of the nurse, to effectively hit the CPD target7. For instance, a maternity nurse should have CPD related to her role in the maternity unit and her career ladder, while the ICU nurse would have a critical care-related CPD.
Nursing career ladder system (NCLS) program incorporates the involvement of nurses in CPD programs, the development of competences and authority standards, clinical indicators, and the performance evaluation. A CPD program is inseparable with the NCLS program, since CPD is essentially a tool for the health care management in increasing the professional competence according the career ladder8,9. This program is expected to be able to shape the caring nature, ethical values, a desire to help, and adequate competences of the nurses. CDP aims to improve competencies, safety, and professionalism6,10. CPD should be in line with the career level, therefore, those with higher clinical position will have more specific and advanced CPD based on their clinical assignments.
The implementation of NCLS in hospitals is relatively new in Indonesia. Despite the non-established national standards on the implementation of the nursing career system, some hospitals have already implemented NCLS and a set of CPD programs by their local standard. Without a national standard, the implementation of career ladder is often problematic because the nurse competence levels differ across different hospitals and the CPD programs are mostly irrelevant with the nurse career ladder.
To our best knowledge, little has been known about the issues on career ladder implementation and CPD in Indonesia in spite of the existing phenomena regarding the mismatch of CPD and career ladder and clinical duty. It is also common that the CPD programs being conducted with no evaluation or follow up. CPD programs which are irrelevantly assigned may lead to unsatisfied nurses and eventually decrease their work performance. In terms of patient care, lower nurse performance may also affect patient safety. Nurses may also experience burnout because their CPD programs are not of their work scope or interest. This may end up with a management problem of nurse turnover. High level of nurse turnover is a vast loss of health care management as nursing staff takes much infestation, such as in staff orientation, utilization, and CPD.
This research was conducted as a part of a larger partnership project. We developed a career ladder system in this hospital in collaboration with the hospital, Faculty of Nursing, Universitas Indonesia, Ministry of Health of the Republic of Indonesia, and Japan International Cooperation Agency (JICA). At this particular hospital, the NCLS was introduced in 2012, but it has not been evaluated yet. This research objective was to identify the characteristics of the nurses’ educational level, the implementation of NCLS, CPD, and the nurse satisfaction. We also assessed the correlation between the implementation of CPD and the satisfaction of NCLS.
MethodA descriptive quantitative approach was used in this study. Survey was conducted at a hospital serving as the top referal for respiratory problems in Jakarta, Indonesia. We carried out the study through the stages of: a) exploring the nurses perception on CPD implementation; b) identifying the work satisfaction, and c) examining the relationship of the CPD and NCLS that have been explored on the first stage.
We recruited 149 clinical nurses by using purposive sampling method. Our samples were selected from those working at the medical-surgical nursing wards to restrict factors that might influence the work satisfaction. All participants met the eligibility criteria of having completed the work orientation period and not undertaking a degree education.
Data were collected using self-administered questionnaires with embedded psychometric scales to identify: a) nurses’ educational background; b) perceptions on the CPD implementation; c) satisfaction of the implementation of the NCLS, and d) correlation between CPD and satisfaction of the NCLS implementation.
We used a standard instrument from Minnesota to measure satisfaction of NCLS. This 18-item tool has sufficient internal-consistency reliability with Cronbach's alpha of 0.914. On the other hand, we developed a questionnaire to assess the CPD implementation through a procedure of tool construction. The pilot test results of this CPD questionnaire indicated its validity and reliability of 0.963.
The data analysis began with the descriptive statistics using percentage, central tendency: mean, median, standard deviation, and continued with the analysis of Pearson product-moment correlation. We ensured all participants had received complete information with regards to the study's objective, purpose, procedures, and the rights of the participants prior signing the consents. Participants filled out the questionnaires voluntarily, in good conscience, and without any forces to do otherwise. Anonymity was guaranteed in all data involved in this study. All data is kept and treated in the strictest manner and is only used for the research purpose.
ResultsNursing education backgroundTable 1 shows that majority of nurses are vocational/diploma degree (89.9%). Only 9.4 percent of them are BSN (Bachelor of Science in Nursing) or professional. It indicates that hospital is still lacking in professional education and dominated by vocational degree.
Continuing professional development and satisfaction with the implementation of career ladder systemTable 2 indicates satisfaction with the implementation of the career ladder and CPD. Mean of satisfaction perceived with career ladder system implementation was 66.2 out of 88 items or equal to 75%. Satisfaction rate ranged between 62.8-69.6 out of 88 items or equal to 71.36-79.2. Work satisfaction with career ladder system implementation was below 80%. Mean of implementation of CPD perceived was 80% (80/100) and in majority ranged between 70.9%-83.4%. Mean of implementation perceived was rather greater than mean of satisfaction, which is 75%.
Perception of continuing professional development and satisfaction with the implementation of career ladder (n=149).
| Variable | Mean/total | Standard deviation | Maximum-minimum | 95%CI |
|---|---|---|---|---|
| CPD | 80.12/100 | 16.85 | 37-100 | 70.9-83.4 |
| NSLS | 66.2/88 | 10.56 | 38-88 | 62.8-69.6 |
95%CI, 95% confidence interval; CPD, continuing professional development; NCLS, nursing career ladder system.
Table 3 indicates significant correlation between CPD implementation and satisfaction with career ladder implementation. The result stated a significant positive correlation between perception of CPD and satisfaction with the implementation of career ladder with a moderate strength. Thus it can be concluded that the better nurse's perception of CPD implementation in hospital, the greater perception of satisfaction with career ladder implementation will be. A moderate strength correlation means that satisfaction is also affected by other factors besides CPD.
DiscussionThe results of CPD implementation perceived has a mean of 80% and distributed between 70-83%. Therefore, it can be concluded that the result is quite well, albeit it is still far from prime. Theoretically, nurses should improve their own competencies due to diversity and complexity in health service. Nurses should have an advanced skill to be able to manage varied group of patients, a complex cluster of care, and acutely ill. Nurses are also obliged to conduct a continuous professional development for the sake of patient safety11.
CPD is necessary since science and technology continuously develops over time, patient needs are improving, and patient safety demand. Nurse is a health professional who is responsible for patient's well-being on 24/7 basis, thus makes a guaranteed competencies crucial. CPD is a part of career ladder implementation that may answer the gap in competencies obtained during competency assessment and on-going professional performance evaluation12.
There are several types of CPD, namely continuing nurse education (CNE), nursing practice, discussing a reflection case, innovating changes, developing preceptorship and mentorship, conducting studies, community service, and applying evidence based practice13. CNE is one of CPD implementation carried out by implementing in job training, off job training, and online learning14,15. In job training is a type of CNE performed within hospital milieu where nurses are able to follow the course while he is still able to perform his duty6, on the contrary, off job training is performed over the working hours and outside the hospital6.
Online learning is an alternative option of CNE that provides more flexible learning potential. By ‘flexible’, it means nurses are able to learn anytime and anywhere. Online learning is a solution for nurses with a tight shift schedule and having difficulties to perform CNE in real time. Online learning also develops awareness to learn for a life time, time management, and independent learning. Several hospitals have developed learning management support which is held on their own to meet their staff requirement. The Previous studied also stated that technology based learning is easier, more flexible, and facilitates communication between health professionals teams11,14,15.
Type and method of CPD conducted in this study is mostly conventional, some are performed by in job training but mostly off job training; in the other hand, due to majority of nurses are vocational means all of them should have a sufficient CPD. Since a conventional CPD generally costs a greater expenses, conventional off job training is held by attending workshop and symposium provided by trainers, and low budgeting factor will cause only a few number of nurses capable of following CPD.
Satisfaction with CPD implementation depends on several factors, such as organization planning, pertinence of selected CPD, and flexibility of CPD implementation. The result revealed that nurses need CPD to improve their own competencies and develop new skills16. Perception on CPD implementation is not at its best owing to the fact that it is not well-planned, as well as an unpublished training schedule to nurses. Ineffectiveness of CPD is also resulted from its implementation which is outside nurse's working hours that leads them to fatigue. Follow-up and evaluation of CPD also needs some improvements. Therefore, it can be concluded that nurses perceive CPD as a necessity to improve their competencies but its implementation is mostly conventional and just for a routine which causes its satisfaction rate is below 80%. The result coincides with previous study which stated that majority of nurses need CPD for technical knowledge and nursing skills6,17 and the congruency of selected CPD with assessment need as well as its type and method will improve CPD implementation in nursing practice18.
Work satisfaction is a perception when a nurse feels comfortable and is able to improve and implement his professionalism at work10,19. Satisfaction correlates with productivity that satisfaction also correlates with work load and cause of increasing turn over19. Satisfaction does not always correlate with appreciation but it is affected by opportunity given to staff to develop himself. Mean of satisfaction in this study was 75% which falls into fair category. Work satisfaction may be related to opportunity that is given to develop oneself, as usually known as continuous professional development. The hospital where authors collect the data have implemented career ladder system which made several CPDs had been put in motion to fill the gaps in competencies.
This study signified a moderate significant correlation between perception of CPD implementation system and satisfaction with the implementation of career ladder which means a good perception of CPD implementation will improve NSLS satisfaction. CPD correlates moderately with satisfaction means there are other factors affecting nurse's satisfaction. Appreciation, remuneration, autonomy, and environment contribute to improvement of satisfaction rate. Career ladder with CPD component is also evidently improving nurse's satisfaction10. This result corresponds to previous finding that stated that CPD system is able to improve nurses’ satisfaction and decrease their turn over20. The career ladder system can affect nurse's CPD satisfaction and competencies positively, such as in clinical skill and judgment17,21.
Some studies claimed that career and competencies pathway were effective to improve the recruitment and retention of experienced staffs, foster professional development, establish an effective reward system to advance clinical performance, strengthen the quality of nursing practice and appreciate staff nurses who provide excellence in patient care. In other hand, clinical ladder were developed to improve competence22 and increase nurse's satisfaction. Implementation of CNL results in a good collaboration and communication with health provider and decrease care expenses. In addition, career for clinical provider also improved nurse satisfaction rate, nurse retention rates and reduced nurse turnover22.
An increased satisfaction rate also effects on decreasing rate of burnt out and turn out10, while contrarily, an increase in dissatisfaction will reduce productivity which compromises patient safety. Nursing manager should be able to sense symptoms of his staff's dissatisfaction. One of means to reduce dissatisfaction is by implementing CPD, according to this study result. CPD can be executed by supervising professional nursing practice, fostering professional development through discussion of case reflection, and providing opportunity to innovate in nursing care and practice. CPD is not only implemented by providing training or opportunity to attend workshop but also opportunity to develop oneself by attending formal education and conducting researches. The study result showed that majority of nurses educational background are vocational thus demand management to afford a formal continuing nurse education. Formal education of CNE will improve competencies in knowledge, skill, attitude, and particularly critical thinking and clinical judgment7.
Nurses’ satisfaction is expected to leverage their productivity, quality, and patient safety thus makes role of manager in implementing career ladder system should be optimum. A clear career pathway, competency regulation, and giving appreciation correspondingly to one's career will clarify nurse competencies10. Granting clinical privilege and CPD accordingly to career level will also improve patient satisfaction10. Implementation of CPD in particular and career ladder system in general can improve nurse's competencies, confidence in collaboration, clinical judgment9, as well as his satisfaction. An improved quality of care and patient safety also affect patient satisfaction.