Introduction
There is evidence that influenza vaccination in older people in developed countries prevents from 30% to 40% of all hospital admissions and deaths from diseases related with this viral infection.1,2 In Spain, vaccination has been shown to prevent 37.4% of all such hospitalizations.2
Influenza vaccination in people older than 65 years is an effective and efficient strategy for primary prevention.3-5 Nevertheless, a considerable proportion of these persons go unvaccinated each year, with figures of around 30% to 50% in different regions of Spain and in developed countries.6-9
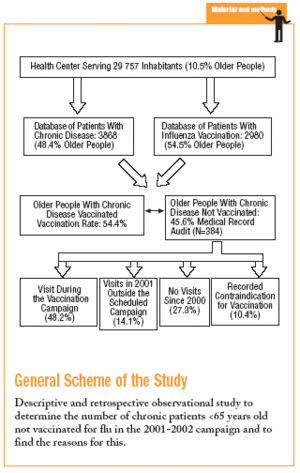
Our aims in this study were to determine the proportion of older patients (>=65 years) with chronic diseases served by our health center who were not vaccinated during the 2001-2002 influenza vaccination campaign, and to find out why they were not vaccinated.
Methods
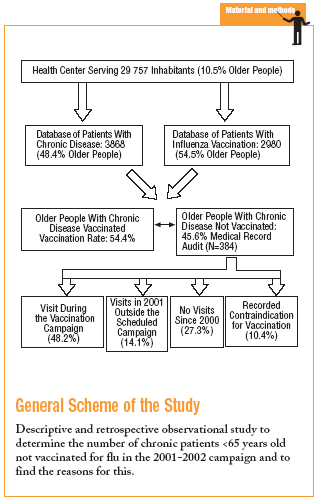
Observational, descriptive, retrospective study in an urban health center serving Area 19 in the Community of Valencia (eastern Spain), chosen randomly from among similar centers. This health center serves a population of 29 757 users, which includes 3116 older persons (10.47%) according to figures obtained in February 2002 from the Sistema de Información Poblacional (Population Information System).
We included patients registered with chronic disease care programs and the influenza vaccination program at our center. The chronic care programs covered hypertension, diabetes mellitus, hyperlipidemia, obesity, chronic medication, and limited mobility. At the time of the study these programs served 3868 patients, 1872 (48.4%) of whom were older than 65 years in 2001. The influenza vaccination register comprised 2980 patients vaccinated during the 2001-2002 campaign, 1624 (54.5%) of whom were older than 65 years in 2001.
The 2 databases were merged and carefully purged of duplicate patients and other errors with the Windows® ACCESS program. This yielded a list of 1019 older patients with chronic diseases who had been vaccinated during the 2001-2002 influenza vaccination campaign.
The level of statistical significance was set at P<.05, and 95% confidence intervals (95% CI) were calculated.
The medical records of all older patients with chronic diseases who were not vaccinated were audited. A representative sample of 384 medical records (95% CI, 0.05 precision, 0.50 expected proportion), was studied to determine why these patients were not vaccinated, and to determine how many visits to the health center they made during 2001 and the months while the influenza vaccination campaign was in progress. The following hypotheses were used to investigate the causes of nonvaccination:
Motive 1: the patient did not visit the health center during the vaccination campaign (October 2001-February 2002) but did come to the center during 2001 before October.
Motive 2: the patient was seen at least once at the health center during the vaccination campaign, but for reasons other than vaccination.
Motive 3: the patient had not visited the center since the year 2000.
Motive 4: the patient declined to be vaccinated, according to information entered in the medical record.
Motive 5: physician's express contraindication because of allergy or other motive.
Motive 6: any other cause that resulted in nonvaccination.
Results
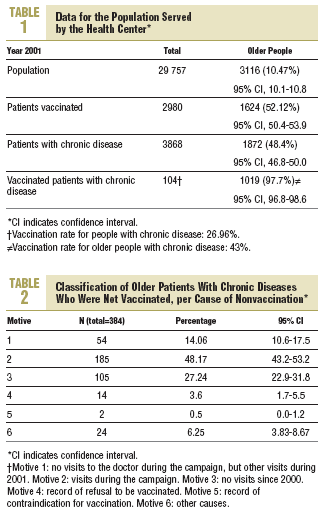
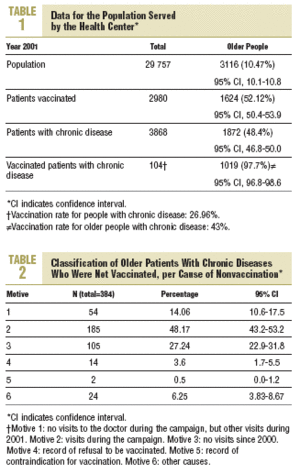
Table 1 shows data for the population studied, patients with chronic diseases and patients who were vaccinated at the health center. The rate of influenza vaccination at the center was 52.12% (95% CI, 50.4-53.9) for all older patients and 54.43% (95% CI, 51.4-57.5) for older patients with chronic diseases.
The findings from our audit of the medical records are shown in Table 2. Among the patients who were not vaccinated, 48.2% visited the health center during the vaccination campaign. The reason for nonvaccination was given in only 10.4% of the medical records we audited.
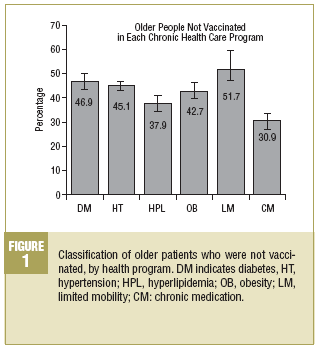
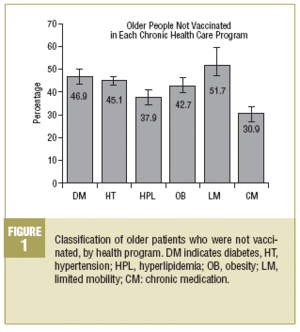
The chronic care program with the highest proportion of patients who were not vaccinated was the program for patients with limited mobility (51.7%), followed by the program for diabetes (46.9%). The highest proportion of patients who were vaccinated was found for the chronic medication program (30.9% not vaccinated) (Figure 1).
Discussion
In our health area, influenza vaccination coverage in older people for the 2001-2002 campaign was 61.3% according to official figures (Source: Dirección General de Salud Pública, data from the Statement of Doses Used, checked against the municipal census). The goal set by the contract for services for the year 2001 was to vaccinate more than 60% of all older people.
At the health center studied here, the influenza vaccination rate was 52.12% (95% CI, 50.4-53.9) for all older people, and 54.43% (95% CI, 51.4-57.5) for older people with chronic diseases. It is nevertheless surprising that coverage was similar in these 2 groups since it might be expected to be significantly higher in patients with chronic diseases, who attend a number of scheduled check-up visits.
It was notable that only 26.9% of all patients with a chronic disease (regardless of age) were vaccinated (95% CI, 25.6-28.4). Some chronic care programs such as chronic medication or obesity might be considered not to be directly related with risk groups for vaccination, but this would hardly account for the low figures we found.
Nearly half (45.6%) of the older patients with chronic diseases were not vaccinated. When we investigated the causes by auditing the medical records (taking into account the biases from underreporting) we found the following:
Among older people who were not vaccinated, 14.06% did not visit the center during the vaccination campaign, although they did come to the center for check-ups as part of their health program in other months during 2001 outside the campaign. There was no record that they had
been advised during these visits to come in for vaccination.
Of greater concern was the fact that almost half of the older people with chronic diseases who were not vaccinated did come to the center during the campaign (for an appointment with the physician or a nursing appointment as part of their chronic care program), but were not advised to get vaccinated. This means that once we rule out refusal to be vaccinated, oversight or physician's contraindication, the apparent reason for nonvaccination is that these patients were not advised to be vaccinated. We feel this is a clear opportunity to improve coverage for influenza vaccination, as it would be easy to ensure that these patients are vaccinated once they come to the center for any other reason.
Approximately one out of every 4 older persons with chronic diseases who was not vaccinated (27.34%) had not come to the health center for more than 1 year, for reasons that have not been determined. Further studies are needed to determine whether these patients are noncompliers or whether the database was not entirely up to date regarding diagnoses or patient-related information.
Only 3.6% of the patients refused vaccination, according to the medical records. Only 2 patients (0.5%) were not vaccinated because of medical contraindications. A small percentage of patients (6.25%) were not vaccinated for a number of other reasons. Thus the clinical motives for nonvaccination were recorded for only 10.35% of the patients. Vaccination is thus a potential goal for all remaining nonvaccinated patients.
The causes of noncompliance with influenza vaccination are multiple and often complex. Mulet et al10 reported, in their evaluation of compliance with influenza vaccination, that the main causes of nonvaccination were the belief that it was unnecessary (63.5%), unawareness of the influenza vaccination campaign (35.7%), fear of reactions to the vaccine (24.3%), and oversight (10.4%). In the present study, two motives stood out:
The patient had not come to the center during at least 1 year (motive 3) even though he or she was registered in a continuing care program.
The patient came to the center at least once during the campaign, but we missed the opportunity to offer vaccination ("We let this one get away.")
One way to analyze nonvaccination is to ask patients why they did not get vaccinated. In this study we analyzed why the health center staff did not try to vaccinate the patient.
If the patient did not visit the center for more than 1 year despite being enrolled in a chronic care program, we
clearly could not offer him or her vaccination opportunistically. If the patient was allergic to the vaccine or declined to be vaccinated, this justifies nonvaccination. But the remaining causes are amenable to intervention by providing information or simply by prescribing vaccination.
Different authors have tried a number of strategies to increase influenza vaccine coverage in older people, including telephone or personalized letter reminders, more extensive information campaigns, and a more active role of nursing staff.12-16 Costa et al17 concluded from their study that nursing staff have a positive influence on compliance with influenza vaccination, and are also a useful element in strategies intended to persuade patients with negative attitudes toward vaccination. Puig Barberá et al14 showed that coverage in the preceding year, human resources, written, or telephoned invitations, the nursing staff being ordered to provide vaccination, and discussion of the findings of external evaluations were independently associated with higher vaccination rates. A study from Switzerland reported that systematic intervention with health professionals before they saw the patient led to coverage rates of up to 85% for vaccination in older people.18 This study gives us an idea of what might be accomplished for the group of patients we studied.
We believe that interventions to implement vaccination should be aimed initially at the groups at greatest risk and who are most accessible, as this would result in an efficient intervention in terms of the effort required in time and human and material resources. Common sense dictates that the most easily identifiable risk group is older patients, since patients with chronic diseases must first be diagnosed. However, if a register of chronic disease patients is available at the health center, this identifies another accessible target group for vaccination with the advantage, in comparison to older patients, that visits to the center are scheduled regularly. These visits offer inestimable opportunities for intervention, which we unfortunately are failing to take advantage of.
When we analyzed the results for our older patients who participated in different chronic disease programs (Figure 1) we found that nearly half of the patients with hypertension or diabetes had not been vaccinated.
We were surprised to discover that somewhat more than half of the patients with limited mobility were not vaccinated; in contrast, the program with the largest percentage of vaccinated patients was the program for chronic medication, and the difference between these 2 programs was statistically significant. This indicated a problem with accessibility of vaccination that was not remedied by a programed care intervention such as home vaccination. In other words, the vaccination process was not integrated into any specific program, and all indications pointed toward on-demand vaccination. As a result, the patients with the best access (who are usually the healthiest patients) were the ones vaccinated most often.
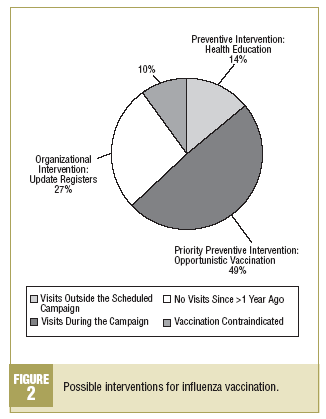
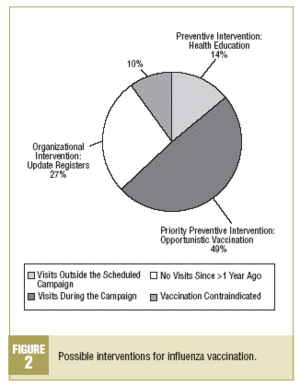
Obviously, additional measures to implement influenza vaccination are needed. The optimum approach would be to use automated registers of influenza vaccination, but the present analysis suggests several proposals that are applicable at any health center regardless of whether computerized registers are available (Figure 2):
Organizational intervention: updating registers of patients with chronic diseases who have not visited the center in more than 1 year.
Priority preventive intervention: systematic opportunistic vaccination for patients who come to the center for a chronic disease program appointment during the campaign, and who made up nearly half of the patients who were not vaccinated.
Preventive intervention in health education: recommending vaccination systematically to all patients with chronic diseases who come to the center for a scheduled appointment even if the appointment falls outside the dates of the campaign.