Globally, depression is the most common psychiatric disorder and is frequently associated with somatic symptom disorders, including pain as a physical symptom. There is a current need to improve the detection and management of the individuals in which depression and pain coexist. Hence, the aim of this document is to provide recommendations in the diagnosis and management of patients with major depressive disorder (MDD) who have pain as a physical symptom (PPS), in order to reduce the variability of clinical practice.
Material and methodsThe methodology used is based on the internationally recognized RAND/UCLA consensus method. The scientific committee, consisted of a group of eight multidisciplinary experts, defined 12 clinically relevant questions. After the systematic review of the literature, the scientific committee assessed the evidence and developed recommendations. The panel group with 15 participants validated these recommendations using a single Delphi round. To conclude, there was a final consensus meeting held to redefine with minor modifications the final recommendations.
ResultsThe scientific committee developed a total of 19 recommendations on the diagnosis and detection, impact of PPS in MDD, treatment of MDD with associated PPS, use of healthcare resources, additional recommendations, and care coordination of these patients. Globally, a substantial level of agreement (≥80%) was reached on all items during the Delphi round. All the 19 achieved consensus, seven of them (37%) were agreed with unanimity during the Delphi round. The recommendations with higher consensus were in relation to diagnosis, impact of PPS in MDD, treatment and use of healthcare resources.
ConclusionsCurrently, the evidence base for patients with MDD and PPS is still being developed and this consensus statement aims to bridge that gap by providing practical recommendations.
According to the World Health Organization (WHO), depressive disorders affect about 280 million people worldwide, which represents 3.8% of the global population.1 In Spain, the prevalence of depressive disorders is about 5.4%, which means 2.1 million people, of which almost 1 million people suffer from major depressive disorder (MDD).2 During the past three years, with the outbreak of the Covid-19 pandemic, it is estimated that the health situation and the subsequent social life changes have led to a 27.6% increase (95% CI: 25.1–30.3) in cases of MDD.2,3
Studies showed that symptoms of pain of unclear origin or disproportionate intensity associated with a depressive disorder were one of the most frequent causes of consultation in primary care centres.4,5 Indeed, it was observed that 69% of subjects with chronic pain followed by general practitioners meet diagnostic criteria for MDD.6 Moreover, it was found that even though diagnostic criteria for MDD generally emphasize mood and vegetative symptoms, between 45% and 60% of patients with MDD report physical pain symptom (PPS).7,8 Even if the causal link remains unclear, there is increasing evidence that chronic pain as a physical symptom (PPS) (e.g., headache, neck pain, back pain) and psychiatric disorders are not only common comorbidities, but psychiatric disorders may modify the risk of chronic pain and vice versa.9,10
In the Diagnostic and Statistical Manual of Mental Disorders-5 (DSM-5) diagnostic criteria of depression, pain is briefly mentioned as a possible symptom, but is not considered as a defining symptom, such as low mood does.11,12 It is common for patients suffering from depression to report somatic symptoms, such as physical pain. With this, there is still a lack of clarity about the causal relationship, as pain could be associated as a symptom, a cause, or as a consequence of depression. The exact causal relationship between depression and pain as a physical symptom is yet to be fully determined.11 The existence of these comorbidities interferes with the patients’ search for treatment and the diagnosis of MDD itself. As a result, the quality of care received as well as the treatment required and the adherence to treatment can decline. It also negatively impacts the results of the treatment of the associated medical conditions, including an increase in disease-related mortality.10
As shown in previous studies and consensus4,10 there is a need to improve the detection and diagnosis of patients in whom depression and pain coexist, as well as coordination between the different professionals involved, such as general practitioners, psychiatrists and other specialists. The direct application of solutions from this scenario remains a challenge in healthcare and public health. The need to establish the causal relationship between depression and pain and understand its impact in terms of burden of the disease justifies raising a reflection based on the available evidence and expert opinion. In this context, this consensus was conducted, with the aim of reducing the variability of clinical practice in the diagnosis and management of patients with major depressive disorder (MDD) who express pain as a physical symptom (PPS). The document includes recommendations on the prevention, diagnosis, and treatment of depression associated with pain based on the available evidence and expert opinion.
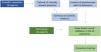
MethodsThe current document has been developed using a methodology based on the internationally recognized RAND/UCLA13 method that incorporates expert opinion and evidence available from a systematic review of the literature. Fig. 1 shows the outline of the consensus process.
The scientific committee consisted of eight specialists (five psychiatrists, two general practitioners, and one neuropharmacologist) from different Spanish centres involved in the management of adult patients with MDD and PPS.
Initially, from six topics proposed (diagnosis and detection, impact of PPS in MDD, treatment of MDD with associated PPS, use of healthcare resources, additional recommendations, and care coordination) each member of the scientific committee individually suggested several clinical questions of interest to be discussed, which led to the development of 12 clinically relevant questions. These questions were adapted to the PICO format14 (Patient, Intervention, Comparison, Outcomes) to form the final questions.
Systematic literature reviewIn order to respond to the clinical questions, a systematic literature review was developed. The search was carried out firstly in databases specialized in clinical practice guidelines such as Medline, Ovid, GIN and the National Guideline Clearinghouse. Then a systematic electronic search of MEDLINE (Ovid), EMBASE, PsycINFO, and the Cochrane Central Register of Controlled Trials (CENTRAL) was performed from the inceptions of the databases up to the 19th November 2021. Since this review included a large heterogeneous group of study designs and sources, the results were synthesized using a narrative approach. As proposed by the current methodological manuals to formulate health recommendations, the GRADE system (Grading of Recommendations, Assessment, Development and Evaluations) was used to assess the certainty of the evidence and the strength of the recommendations.15 For that reason, the quality of evidence is assessed based on the following factors: risk of bias, inconsistency, indirectness, impressions, publication bias, effect and confounders, and defined as “high”, “moderate”, “low” or “very low” accordingly. The GRADE system sets out also recommendations based on a series of considerations such as the risk-benefit balance and the quality of evidence defining as strong or weak the recommendation being not applicable for statements developed based only on expert opinion.
Delphi roundThe scientific committee assessed the evidence identified by the systematic review and created a questionnaire with 19 preliminary statements. Using a Delphi round, a validation of the recommendations was carried out by a group of 15 experts from different regions in Spain including 10 psychiatrists from tertiary hospitals and 5 general practitioners from public health centres. The experts were selected based on specific inclusion criteria, which required them to have more than 20 years of experience, conduct visits with 10–20 patients diagnosed with the condition per month, and have authored or co-authored publications related to the topic. For each response to the questionnaire, the panelists had a free text box to justify their response or provide further questions. For this consensus, we applied a unique Delphi round as all the statements reached consensus in the first round.
Final consensus meetingAfter the single Delphi round, the results and the comments left by the panellists during the Delphi round were analyzed and discussed, and the pertinent minor modifications were incorporated to the statements and recommendations through a final consensus meeting with the scientific committee.
Statistical analysisThe percentages of agreement and disagreement were calculated for each of the items in the questionnaire, based on a Likert scale ranging from 1 to 4 (1: “strongly disagree”, 2: “moderately disagree”, 3: “moderately agree”, 4: “strongly agree”), considering values of 3 and 4 as agreement and 1 and 2 as disagreement. For the purpose of this study, consensus was defined as greater than or equal to 80%. Consensus through unanimity was defined by 100% agreement. Discrepancy was defined as an agreement percentage between 66% and 79%. It was defined that any recommendation with a percentage of agreement less than 66% will be rejected. Descriptive statistics for categorical variables included percentages, and mean, median and range for continuous data.
ResultsSystematic literature reviewThe report of systematic literature review was compiled by the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA).16 The search results yielded a total of 5820 articles, of which a total of 22 articles were selected to be included in the evidence synthesis. Fig. S1 in Supplementary Material shows the PRISMA flowchart for the identification of studies.
The evidence identified through the systematic literature review was assessed using the GRADE system.13 The GRADE system initially classifies the evidence into high or low, coming from experimental or observational studies; subsequently and following a series of considerations, the evidence is classified into high, moderate, low, or very low. The strength of recommendations is based not only on the quality of the evidence, but also on a series of factors such as the risk/benefit balance, values, and preferences of the individuals and professionals, and the use of resources or costs. The recommendation strengths and the quality of evidence for each of the statements and recommendations are shown in Table S1 in Supplementary Material.
Consensus process resultsAll the invited panellists (n=15) responded to the questionnaire on the Delphi round. All the statements and recommendations (n=19) reached consensus during the Delphi round. Results of the Delphi round are presented in each specific topic respectively (see Tables S2–S7).
Topic 1: Diagnosis and detectionThe detection of depression can provide clinically significant information that facilitates the identification of patients at high risk of suffering from MMD and PPS, and with a combined pathology diagnostic approach it could lead to a more effective, specific, and early treatment choice.
The PHQ-9 threshold of ≥20 was strongly associated with pain interference symptoms (OR 21.6, 95% CI 17.5–26.7) but PHQ-9 score of ≥10 still showed significant associations with pain interference symptoms (OR 6.1, 95% CI 5.4–6.9).17 Depression screening using short questions in patients with chronic pain found areas under the curve (AUC) with values between 0.79 and 0.81.18 These findings support the use of simple and frequently used depression screening tools and can provide information regarding the probability of this condition in patients with chronic pain.17
When we compared the clinical presentation of MDD between genders, women were associated with a higher prevalence of depression and with a higher prevalence of pain. They reported this symptom more intensely and sometimes with a lower response to analgesics.19
The European SHARE study included 22,280 participants, 58.2% (n=12,962) women and the mean age was 64.2 years (SE 10.1). The study showed that the presence of the two entities (pain and depression) was more frequent in women than in men (25.3% vs. 14%) with an OR 2.3 (95% CI 2.2–2.6). In women undergoing follow-up, untreated depression was associated with the presence of persistent pain OR 1.3 (95% CI 1.1–1.6).20 These data corroborate results of previous studies that showed that women were more likely to have symptoms of chronic pain when they suffered from MDD. De facto, they are more prone to opioid use, which can cause side effects and worsen depressive disorder.21 Overall, it was found that in women, functional impairment, but not pain intensity, was significantly associated with the initial severity of depressive symptoms.
In the elderly population, the diagnosis of depression can be uncertain, since changes in behavior may represent symptoms of underlying cognitive dysfunction.22
In the Netherlands Study of Depression in the Elderly (NESDA) among persons aged 60 years and older, it was found that older adults with depressive disorders reported pain with greater severity and more frequently than controls. The direct effect of pain severity and the indirect effect of pain perception on depression was OR 1.1 95% CI (0.98–1.25) and OR 1.24 (1.15–1.35) respectively.23Table S2 in Supplementary Material presents the results of the Delphi round for topic 1.
Topic 2: Impact of the pain as a physical symptom on major depressive disorderUncontrolled chronic pain impacts on the probability of remission of the depressive disorder, with an increased risk of relapse. Likewise, in patients with partially or uncontrolled major depression, therapeutic adjustments aimed at achieving control of the disease positively impacted on the response to pain control.
The rates of recurrence of depression are high with reports between 25–60%. It is very important to identify risk factors for recurrence, with the aim of guaranteeing a long-term therapeutic response. Chronic pain is a potentially modifiable risk factor for the recurrence of depression.24 The NESDA study found that neck pain with a HR of 1.45 95% CI (1.12–1.89), chest pain HR 1.65 (1.14–2.39), and abdomen pain HR 1.52 (1.16–2.02) were associated with an increased recurrence of depression, as well as an increase in the number of locations that experience pain. An increase in the number of pain locations and pain severity increased the risk of depression recurrence with a HR of 1.1 and 1.18 respectively.25 Regarding the therapeutic response, it was found that the patients who experienced more pain were more likely to have severe depression, greater risk of suicide, functional alterations and poor response to treatment.26
One evidence-based structured review showed the negative effect of pain in response to depression treatment. The study showed how pain reduction revealed an impact on increasing the probability of remission.27 Another study found that patients with MDD who did not respond or partially responded to serotonin reuptake inhibitors (SSRI) treatment had clinically significant pain. This pain improved significantly after switching to duloxetine, regardless of the exchange method used (direct switch or start-taper switch).28
Both, pain and depression have been independently associated with suicidal behaviour,29 and it has also been suggested that pain could have an effect on suicidal behavior through depression. A network meta-analysis explored the association between suicidal ideation and pain to see if the association between pain and suicide was greater in adolescents tested for depression. The study founded a significant association between suicidal ideation and pain, with an OR of 4 (95% CI 2.75–4.31), and with no gender differences. This association continued to be significant after controlling for depression and anxiety.29Table S3 from Supplementary Material presents the recommendations and the results of the Delphi round for topic 2.
Topic 3: Treatment of major depressive disorder (MDD) associated with pain as a physical symptomWe have generated recommendations from the review of the literature and expert consensus for patients with somatic symptoms as a comorbid condition with regards to the most appropriate antidepressant for optimal symptom control. The recommendation was adopted from the Canadian guidelines (CANMAT) for the treatment of major depressive disorder: “In patients with major depression and somatic symptoms, treatment recommendations include duloxetine for pain management (Level I evidence), other serotonin and norepinephrine reuptake inhibitors for pain management (Level II evidence), and serotonin reuptake inhibitors for fatigue management (Level II evidence).”
Despite this, a systematic review showed that all classes of antidepressants studied had significant antidepressant effects compared to placebo: serotonin–norepinephrine reuptake inhibitors (SNRI)=0.28 (95% CI 0.22–0.34 I2 4%); SSRI=0.27 (95% CI 0.09–0.45 I2 13%).30 Both SNRIs and SSRIs were found to be superior to the placebo with respect to analgesic effect: SNRI=0.27 (95% CI 0.21–0.33 I2 0%); SSRI=0.24 (95% CI 0.13–0.36 I2 0%).31 The SNRIs reported a strong positive correlation between the effectiveness in pain relief and the positive effect on depression symptom control, mainly mood of the patients.
Non-pharmacological interventions such as cognitive behavioural therapy and psychological interventions have shown to be effective in managing depression, anxiety, and chronic pain. A self-help program based on the principles of cognitive behavioural therapy has shown through Cox regression that the intervention reduced the risk of major depressive episodes by 52% (HR 0.48 (95% CI 0.28–0.81 p<0.001)). At 12 months, 21 participants (14%) in the intervention group and 41 participants (28%) in the control group experienced major depressive episodes. The number needed to treat to prevent 1 new case was 2.84 (95% CI 1.79–9.44).32 Non-pharmacological therapies based on cognitive behavioural therapy administered with e-coaching strategies reduce the risk of depressive episodes, and the effect is maintained in the long term. Table S4 from Supplementary Table presents the results of the Delphi round for topic 3.
Topic 4: Use of healthcare resourcesChronic pain treatment for patients with depression had a total healthcare cost of £731 (95% CI 646–817) for a three-month period, compared to £448 (95% CI 366–530) in subjects without depression. Appropriate treatment of depression could improve the health and functioning of patients with chronic pain. Controlling both health issues may reduce the burden on health systems, taking into account the documented cost increases in patients with chronic pain and comorbid depression.
With regards to the consumption of healthcare resources, effective treatment of depression could improve the health and functioning of patients with chronic pain and reduce the burden on health systems. The Pan study was a cross-sectional study to determine the prevalence and impact of depression on health costs in patients with complex chronic pain refractory to treatment that included 1204 patients attending a specialized interdisciplinary pain management unit. Two-thirds of the sample were women, with an average age of 47 years (interquartile range of 38–53 years), and the median duration of pain was 7 years. The study showed that in patients with depression and pain, there was a cost-utility advantage of SSRIs over tricyclic antidepressants (TCAs) that varied according to the willingness-to-pay threshold. The presence of pain may be an effect modifier in cost-utility comparisons. Table S5 from Supplementary Table presents the recommendations and the results of the Delphi round for topic 4.
Topic 5: Additional recommendationsEducational and information intervention programs administered by healthcare systems might generate self-management skills that can improve outcomes related to chronic pain.33
The study by Damush et al. founded that an educational intervention, as explained below, by nurses increased patient self-care behaviours and self-efficacy to control symptoms of chronic musculoskeletal pain and depression, with a relation to dose (number of sessions) response.34
The educational intervention had several steps. Firstly 6 training sessions on self-control of pain were carried out, and then the second step was to promote self-efficacy. The program then began with patient education on the natural history of pain, emphasizing the potential for improvement with time. This was designed to increase patients’ optimism for improved function and coping but provided realistic expectations regarding disability. Table S6 from Supplementary Material presents the recommendations and the results of the Delphi round for topic 5.
Topic 6: Care coordinationThe use of an integrated approach to the management of depression and chronic pain appears to be a reasonable strategy that could have synergistic effects in achieving better clinical outcomes. Previous studies of patients with depression have shown how multidisciplinary approaches positively impact on clinical outcomes.35 The study by Aragones 2019 et al. presented the DROP (DepRessiOn and Pain) programme which included a variety of components based on the premises of the chronic care model such as optimised management of MDD, care management and a psychoeducational intervention programme for patients with chronic pain and depression. There were no statistically significant differences regarding pain severity.36 No evidence on the effect of multidisciplinary management was found. It showed that the response rates to antidepressant treatment in the intervention group receiving the multicomponent program were 18.9% higher (39.6% vs 20.7%, OR 2.74, 95% CI 1.12–6.67) and depression remission rates were 9% higher (20.1 vs 11.1%, OR 2.13, 95% CI 0.94–4.85) compared to the usual care group. Table S7 from Supplementary Material presents the recommendations and the results of the Delphi round for topic 6.
After the validation round and based on the comments of the experts, the final recommendations were redefined with minor modifications during a final consensus meeting as presented below.
Final statements and recommendations1.1. It is suggested to screen patients with chronic PPS for depression, especially if it interferes with functionality, through the use of short questions or short depression scales.
2.1. The concomitant presentation of PPS and MDD is more common in women, and pain-related functional impairment is greater.
2.2. Given the high frequency of comorbidity in women, their mutual influence should be evaluated, and a joint and early therapeutic approach should be carried out.
3.1. In the elderly patients with pain, it is suggested to perform depression screening through the use of brief questions or short geriatric depression scales.
3.2. In the elderly patient, disproportionate pain and/or the presence of multiple somatic/painful complaints should lead to investigation of an underlying depressive disorder.
4.1. In patients with MDD and PPS, the response to antidepressant treatment is lower in patients who experience more pain (less symptom reduction, more recurrences, less functional improvement).
4.2. When choosing antidepressant treatment, the presence of pain as a comorbid symptom should be taken into account.
5.1. In patients with MDD and PPS, it is suggested to treat pain and maintain it under control in order to achieve remission of the depressive disorder and avoid relapses.
5.2. In the absence of response or partial response to antidepressant treatment, the presence of pain should be evaluated as a comorbid or residual symptom.
6.1. Given the increase in suicidal behaviours associated with pain, its risk should be assessed even in the absence of depression.
7.1. In patients with MDD and PPS, the use of SNRIs or with less evidence, SSRIs is recommended.
7.2. In patients with MDD and somatic symptoms, the use of SNRI drugs for pain management is recommended.
7.3. The use of duloxetine is recommended in preference to other SNRIs for the management of pain associated with MDD.
8.1. In patients with PPS and depression, the use of cognitive-behavioural therapy has high scientific evidence.
8.2. Clinical experience suggests that mindfulness or acceptance and commitment therapy is effective in treating chronic pain.
9.1. In patients with PPS and MDD, detection and adequate treatment of comorbidity is recommended, in order to reduce the economic burden for health systems.
10.1. Appropriate treatment of depression with PPS shows a gain in quality-adjusted life years (QALYs) and therefore improves the cost-utility ratio.
11.1. In patients with MDD and PPS, it is recommended to associate interventions through educational programs, based on learning self-care measures directed by health professionals.
12.1. In patients with MDD and PPS, it is recommended to use interventions with multicomponent programs, in order to improve the response rate to antidepressant treatment and the remission rate of depression.
This consensus aimed to reduce the variability of clinical practice in the diagnosis and management of patients with major depressive disorder (MDD) who express pain as a physical symptom (PPS). The statements and recommendations included in the Delphi's round questionnaire were based on the evidence identified through a systematic review of the literature and expert opinion. A substantial level of agreement (≥80%) was reached on all recommendations. The resulting document aims to be a useful tool in the therapeutic decision-making within routine clinical practice.
In the presence of chronic pain, screening for depression should be part of usual practice. Although pain does not appear among the diagnostic criteria for depression in the DSM-5, the treatment and management of MDD and pain should be more integrative and individualized in usual clinical practice. We would remind that the latest update of the diagnostic criteria of the DSM-5 was controversial.37 In addition, the importance of pain in the therapeutic response and the evolution of depression must be considered. Moreover, suicidal behaviour risk assessment should be also incorporated in the habitual practice. Because in usual clinical practice chronic pain and depression go hand in hand, and therefore, and in a situation that is going to be maintained over time and complex to manage, we must assess the risk of suicide to prioritize interventions and/or referrals. Urgently or preferentially both to emergencies in the face of imminent risk or to mental health units. Most of these cases will be detected in the field of Primary Care and it is necessary to think about it to detect and act. As limitations, I would indicate the lack of training to proactively address suicidal ideation as well as the lack of time in the consultations that cause there to be a certain inertia in its management and we forget these details.
Regarding the treatment not all antidepressants are equally effective in treating patients with depression and the associated chronic pain. Also, the use of non-pharmacological therapies, such as psychotherapeutic intervention, is recommended as a complement to pharmacological treatment. I would mention if they see fit very cost-effective non-pharmacological interventions such as exercising and prescribing health assets in the community or basic health area where the patient lives, since many of them, due to economic limitations, will not have access to psychotherapeutic interventions or they will do it late and little.
The scientific committee highlighted that a personalized diagnosis and treatment must be used. The self-management of the disease by the patient adds positivity to any clinical action, promotes adherence, collaboration and finally a favourable result. If the patient is the centre of the process, multidisciplinary and collaborative care is vital for a new concept of care. This model proposes a relationship of equality and horizontality between professionals and with and for the patient. This model enriches the care and improves it remarkably. On the other hand, as a limitation the low awareness of the disease and the difficulties at the cognitive and educational level that the patient may have to carry it out. In this sense, health education is of great importance, both for the patient and for their social environment.
It is very important, because we must assess psychosocial aspects such as socioeconomic level (can you afford private psychotherapy and are you willing to do so??), patient preferences (prefer non-pharmacological interventions if you can afford it), social and family support, environment in which you live (urban, rural, semi-rural etc. This can hinder access to professionals and other resources that do not exist in the environment where you live). Social determinants are of great importance and must be kept in mind. And based on this, personalize the treatments. The limitations once again are time and the lack of knowledge on the part of the professional who cares for the environment where the patient resides and its possibilities or limitations.
With regards to the strengths of the document, this consensus used the GRADE methodological approach for rating the quality of evidence found in the systematic search. This method is extremely robust and reliable. The internationally recognised RAND/UCLA method was selected for this project which is based on the integration of evidence from the literature review and expert opinions. The final consensus meeting allowed the experts to discuss the ratings and judgements adding significant value to the method.
As a limitation, on the consensus method the interpretation of the study results is highly dependent on responder expertise. For this, we added a validation process including a panel of 15 key opinion leaders from different regions in Spain with a strong clinical background, all of which responded to the questions independently. This number of experts increased the reliability of the group judgements made. Nevertheless, the anonymity of panellist in the survey rounds and controlled feedback reduced dominance and group conformity. As another limitation, it can be emphasized that this consensus document focuses on the relationship between MDD and PPS but does not address the comorbidity relationship between bipolar disorder depression and PPS. However, previous studies have reported that chronic pain is common in bipolar depressed patients, highlighting the importance of paying more attention to study the presence of pain in bipolar depressed patients, in order to achieve more accurate diagnoses and to provide better treatment options.38,39 Therefore, it would be interesting to open the question of the existence of PPS to a wider range of depressive disorders.
ConclusionIn conclusion, this consensus was conducted with the aim of reducing the variability of clinical practice in the diagnosis and management of patients with MDD who express pain as a physical symptom. Overall, a substantial level of agreement (≥ 80%) was reached on all recommendations formulated following the systematic review. Currently, the evidence base for patients with MDD and PPS is still being developed and this consensus statement aims to bridge that gap by providing practical recommendations. In conclusion, pain as a physical symptom is quite common in MDD patients and the recommendations provided in this consensus can help in the detection and management.
FundingThis study was founded by Esteve Pharmaceuticals S.A.
Conflict of interestsVPS has received Research funding from the Institute Salud Carlos III, UE H2020, Cibersam, Janssen and Compass. He has two patents, Psicopatapp and Cuidas Cuidad. He owns Bipek SL and in the last 5 years, he has agreements or received fees as a speaker from Otsuka, GSK, Exeltis, ABBVIE, Abbot, Lundbeck, Esteve, Novartis, Angelini, Novartis, Janssen. JGC has received research funding from Carlos III Health Institute (FIS scholarships), the Government of Aragon and Lundbeck (Friesgod and suicide analysis scholarship through Twitter). In the last 5 years, he has received funding as a speaker from Exeltis, Lundbeck, Esteve, and Janssen. JMO has received research funding from the Carlos III Health Institute, the ACIS (Galician Health Knowledge Agency) and the National Drug Plan. He received fees as speaker and/or consultant in the last 5 years from Janssen, Lundbeck, Adamed, Esteve, Oryzon Genomics and Angelini. LAO has received agreements or fees as a speaker in the last 5 years from Exeltis, Lundbeck, Esteve, Angelini, Janssen, Neuraxfarm, Pfizer, and Servier. EVC has had agreements or received fees as a speaker from GSK, Lundbeck, Esteve, Novartis, Menarini, Teva, AstraZeneca, Boehringer, Menarini, Servier. JMM has received Research funding from Janssen, Carlos III Health Institute and Otsuka-Lundbeck. In the las 5 years, he has had agreements or received fees as a speaker from Exeltis, Lundbeck, Angelini, Janssen, Neuraxfarm, Pfizer, Servier and Recordati. VGM has had agreements or received fees as a speaker in the las 5 years from Lundbeck, Pfizer, Esteve, Servier, Organon and Schwave. She has received funding to attend the SEMERGEN National Congresses and the SEMERGEN Valencian Community Congresses of the last three years. EBD has received royalties from the patents GB_Sciences and has received research funding from Research project of the State Research Agency, Junta de Andalucía Project, National Drug Plan Project, ITN (H2020).
We would like to thank the panellists for their participation in the Delphi questionaire (Luis Caballero, Narcis Cardoner, Diego J. Palao, Josefina Pérez Blanco, Juan Ramon Castaño Asins, Ricard Navines de la Cruz, Yolanda Morant Lujan, María Luisa Zamarro, Luis Gutiérrez Rojas, María Teresa González Salvador, Pedro Ibor Vidal, Silvia Lopez Chamon, Lorenzo Armenteros, Alberto Freire, Manuel J. Mejías Estévez). We would like to give a special mention to Dr. Juan Antonio Micó for his participation as a member of the scientific committee. The authors acknowledge GOC Health Consulting for the coordination of the project and methodological assistance throughout it and writing of the manuscript. We would like to thank Esteve Pharmaceuticals for giving logistal support during the consensus development.