Thymic cysts account for 1%–5% of anterior mediastinal masses,1 and may be congenital or acquired. Acquired thymic cysts have been associated with such systemic diseases as lupus erythematosus, Sjögren syndrome, rheumatoid arthritis, Hashimoto thyroiditis, HIV infection, and in very rare cases, with myasthenia gravis (MG).2
We present an extremely rare case of MG associated with thymic cyst.
The patient was a 34-year-old former smoker with no history of disease. He attended our department due to a 2-month history of fatigue of the facial muscles, with no additional symptoms. The physical examination revealed mild left ptosis, which did not increase with maintained vertical gaze, as well as weakness of the tongue and the left orbicularis oculi and oris muscles.
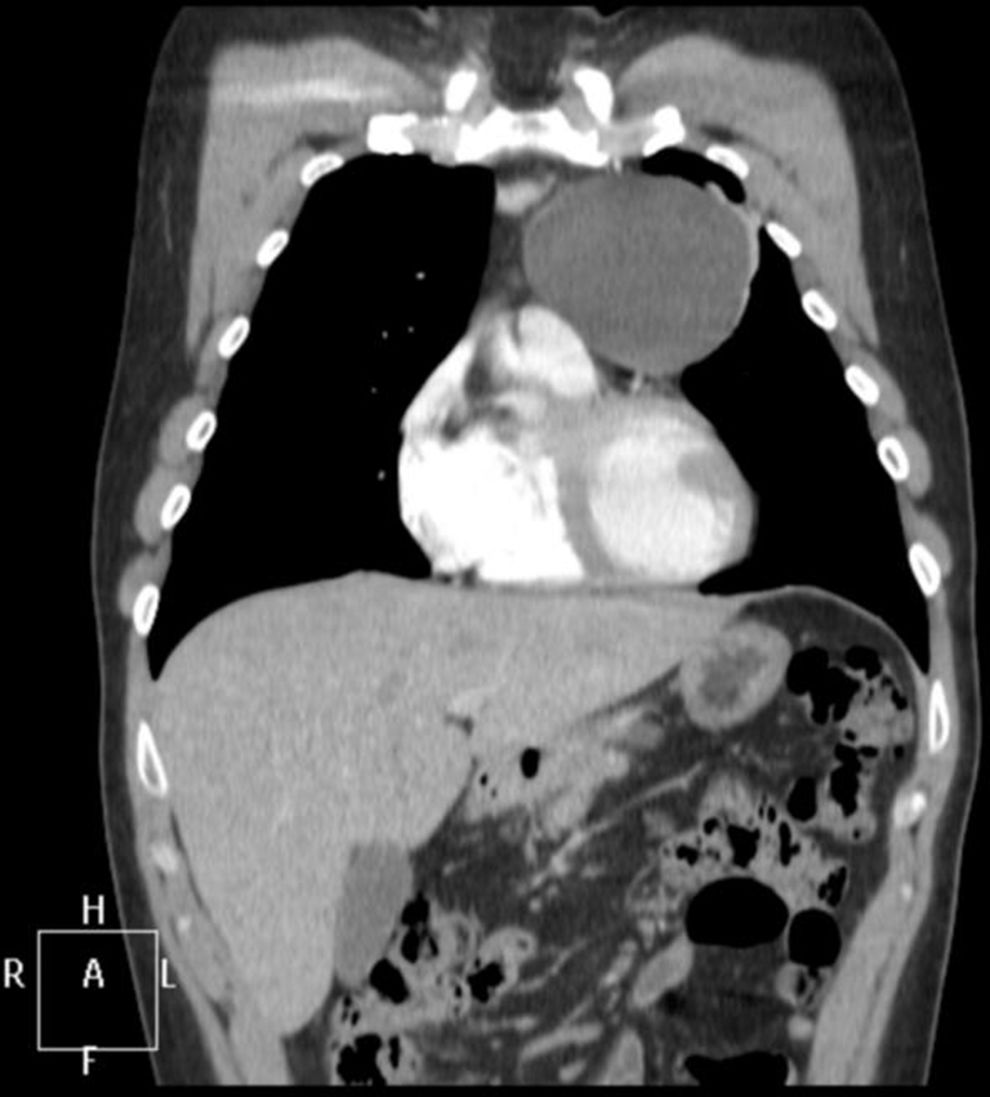
We made a diagnosis of MG; this was confirmed by the results of an anti-acetylcholine receptor (anti-AChR) antibody analysis (22.1nmol/L) and a single-fibre EMG in the left orbicularis oculi muscle (semi-pathological jitter; 47% blocking). These findings are compatible with a postsynaptic alteration in neuromuscular transmission. A mediastinal computerised tomography (CT) scan revealed a cystic lesion in the prevascular space, measuring 78×79×77mm, with well defined contours and thin walls, of liquid density, showing no contrast uptake and no evidence of lymph node involvement (Fig. 1).
The mediastinal lesion was surgically resected 4 months after diagnosis. The anatomical pathology study identified it as a unilocular thymic cyst with follicular hyperplasia. A cytology study of the pleural fluid was negative for malignant cells, suggesting a cyst of lymphoid content.
Following diagnosis, the patient was started on treatment with pyridostigmine dosed at 60mg every 8hours. This partially improved the ptosis and the strength of the orbicularis oris muscle. One month later, the patient started a slow tapering course of prednisone, beginning at a weight-adjusted dose of 80mg/48hours. In the second month of treatment, the orolingual weakness showed a marked improvement; the orbicularis oculi muscle weakness persisted until 3 months later, with the patient receiving prednisone at 30mg/48hours. The surgical intervention enabled the gradual reduction of the corticosteroid dosage over the following 4 months, reaching 5/2.5mg on alternating days. Symptoms reappeared at this point, resulting in corticosteroid dosage being increased once more to 10/5mg on alternating days, and the introduction of azathioprine. The patient remained asymptomatic following the withdrawal of prednisone, although pyridostigmine continues to be necessary.
Thymic cyst is a well defined, water-density lesion of the anterior superior mediastinum. The mass may be congenital or acquired. Congenital cysts are unilocular, with thin, translucent walls and atrophic tissue with no inflammation. Acquired thymic cysts tend to be multilocular, with thicker, potentially fibrous walls and hyperplastic thymic tissue. These lesions are usually asymptomatic, although they occasionally cause dyspnoea, coughing, or chest pain due to compression of adjacent structures.3
Thymoma, which accounts for 95% of cases of thymic epithelial tumours, presents as a homogeneous, solid, soft-tissue mass with well-defined borders, occasionally displaying uniform contrast uptake and calcification.4 Up to 40% of cases of thymoma may involve a cystic component; however, it is very rare for the cyst to account for almost the entire mass.5
Radiological differential diagnosis of thymic lesions can be complex. Thymic cysts complicated by bleeding or infection may be mistaken for solid masses due to the increased density in CT images.6 Thymomas may also develop haemorrhagic, ischaemic, or cystic areas, simulating simple thymic cysts.7,8 Chest MR images may be of assistance. In MR images, thymoma appears as a homo- or heterogeneous mass. It is hypointense on T1-weighted and slightly hyperintense on T2-weighted sequences, showing restricted diffusion and contrast uptake, whereas thymic cysts are hypointense on T1-weighted and hyperintense on T2-weighted sequences and do not display restricted diffusion or contrast uptake. If the diagnosis remains uncertain, an 18F-FDG PET scan may be helpful, as this technique provides information regarding metabolism.9 However, precise classification of a cystic mediastinal lesion requires a histopathology study, particularly if the wall is focally thickened.10
Thymic abnormalities affect up to 85% of patients with MG (follicular hyperplasia affects 70% and thymoma 15%)11; however, a literature search only identified 6 cases published to date of patients with MG associated with thymic cyst. In 1957, Fongi et al.12 described a case of myasthenic crisis following excision of a thymic cyst. In 1993, Peacey and Belchetz10 presented a patient with ocular MG and thymic cyst. In 1995, Okumura et al.13 reported a case of MG associated with multilocular thymic cysts. In 2012, Mishra et al.14 described 3 cases of MG with unilocular thymic cysts.
Little is known about the progression of MG following surgery in these cases. In the series reported by Mishra et al.,14 2 patients clinically improved and one worsened following resection of the cyst. In other cases, one patient had a myasthenic crisis following surgery,15 and another did not improve.10 Our patient experienced a temporary improvement, lasting less than 6 months, and eventually received long-term immunosuppression.
Thymectomy is included in the treatment protocol for MG and has been demonstrated to achieve clinical improvement, although the benefits of the intervention are not fully understood.16 The results of the “Thymectomy trial in non-thymomatous myasthenia gravis patients receiving prednisone therapy”,17 currently underway, will provide information on these benefits in non-thymomatous patients.
Although thymic cyst occurs very infrequently, we believe it should be included in the spectrum of MG-associated thymic conditions. Our patient's transient improvement following the excision of the cyst seems to confirm its involvement in the pathophysiology of this autoimmune disease.
Thymectomy would therefore be indicated in these cases in order to rule out the presence of tumours in the cyst walls and/or to delay the start of prolonged immunosuppression.
Please cite this article as: Morollón N, Guerrero P, Duarte J. Quiste tímico asociado a miastenia gravis. Neurología. 2018;33:405–407.