SARS-CoV-2, the virus responsible for the current pandemic, is associated with high mortality rates, especially in elderly patients and those with chronic diseases.1 Respiratory complications constitute the most common cause of death due to amyotrophic lateral sclerosis (ALS)2; management at multidisciplinary ALS units is known to increase the life expectancy of these patients.3 Therefore, it seems reasonable to suggest that patients with ALS are at increased risk from COVID-19 and that they constitute a vulnerable population in view of the potential consequences of lockdown on their daily care. However, no epidemiological data are currently available to confirm this hypothesis.
MethodsWe created a survey to gather data on the impact of lockdown on the care provided to patients with ALS. The Miquel Valls Foundation (the main care platform for patients with ALS in Catalonia) used e-mail and mobile messaging to distribute the survey among patients with ALS and their caregivers. All respondents were ≥ 18 years old, had been diagnosed with ALS according to the revised El Escorial criteria,4 and gave informed consent to participate. The study was approved by the local ethics committee.
ResultsWe collected data on 57 patients, although the survey was sent to a total of 169 patients with ALS. The questions referred to the period of lockdown following the declaration of a state of alarm in Spain (14 March to 21 June 2020). During this period, mobility was restricted and hospital care was largely focused on managing patients with COVID-19. According to our data, 19 patients with ALS died due to the natural course of the disease during lockdown. Previous studies estimate the number of deaths of these patients in Catalonia during a 3-month period at 29.5 Although this is a rough estimate, it seems to suggest that mortality did not increase during lockdown.
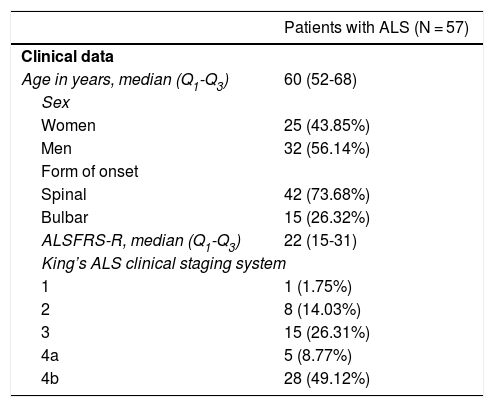
Table 1 presents the clinical and epidemiological characteristics of our sample. Although only a small percentage of all patients receiving the survey actually completed it, they represent a cohort of patients with severe ALS and dependence: median ALSFRS-R score was 22 (Q1–Q3, 15–31), most were on stages 3 (26.31%) and 4b (49.12%) of the King’s ALS clinical staging system, and 43.86% of patients (n = 25) required non-invasive mechanical ventilation. None of the patients or their households presented COVID-19. Only 5 (8.77%) reported symptoms compatible with SARS-CoV-2 infection (fever, cough, headache, hyposmia), but diagnosis could not be confirmed in any of them.
Demographic and clinical characteristics of our sample of patients with amyotrophic lateral sclerosis.
| Patients with ALS (N = 57) | |
|---|---|
| Clinical data | |
| Age in years, median (Q1-Q3) | 60 (52-68) |
| Sex | |
| Women | 25 (43.85%) |
| Men | 32 (56.14%) |
| Form of onset | |
| Spinal | 42 (73.68%) |
| Bulbar | 15 (26.32%) |
| ALSFRS-R, median (Q1-Q3) | 22 (15-31) |
| King’s ALS clinical staging system | |
| 1 | 1 (1.75%) |
| 2 | 8 (14.03%) |
| 3 | 15 (26.31%) |
| 4a | 5 (8.77%) |
| 4b | 28 (49.12%) |
ALS: amyotrophic lateral sclerosis; ALSFRS-R: Revised Amyotrophic Lateral Sclerosis Functional Rating Scale.
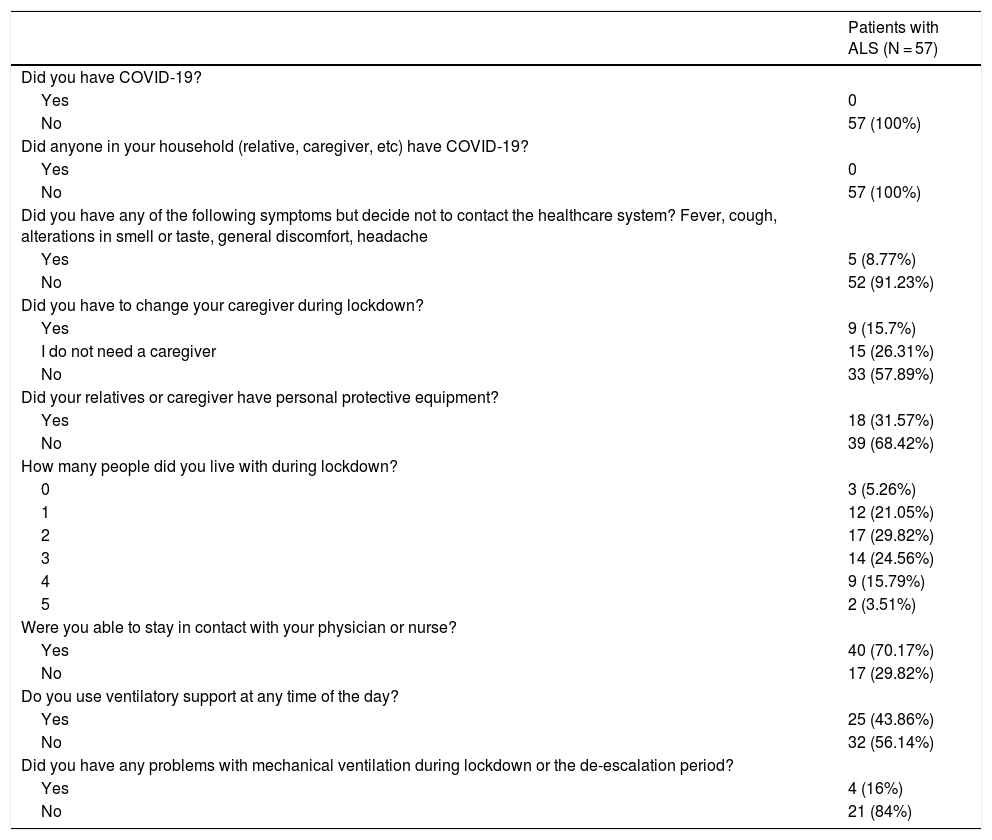
Of the 42 patients requiring daily care, 9 (21.43%) had to change their caregivers due to lockdown (Table 2). Seventeen patients (29.82%) were unable to contact their physicians or nurses. This is particularly relevant considering that most patients in our sample (84.31%) were on stages 3 and 4 of the King’s ALS clinical staging system. Most patients (68.42%, n = 39) reported that none of their relatives or caregivers were able to procure personal protective equipment. Furthermore, 25 patients (43.86%) reported that they lived with ≥ 3 people during lockdown.
Results of a survey sent to patients with amyotrophic lateral sclerosis during lockdown.
| Patients with ALS (N = 57) | |
|---|---|
| Did you have COVID-19? | |
| Yes | 0 |
| No | 57 (100%) |
| Did anyone in your household (relative, caregiver, etc) have COVID-19? | |
| Yes | 0 |
| No | 57 (100%) |
| Did you have any of the following symptoms but decide not to contact the healthcare system? Fever, cough, alterations in smell or taste, general discomfort, headache | |
| Yes | 5 (8.77%) |
| No | 52 (91.23%) |
| Did you have to change your caregiver during lockdown? | |
| Yes | 9 (15.7%) |
| I do not need a caregiver | 15 (26.31%) |
| No | 33 (57.89%) |
| Did your relatives or caregiver have personal protective equipment? | |
| Yes | 18 (31.57%) |
| No | 39 (68.42%) |
| How many people did you live with during lockdown? | |
| 0 | 3 (5.26%) |
| 1 | 12 (21.05%) |
| 2 | 17 (29.82%) |
| 3 | 14 (24.56%) |
| 4 | 9 (15.79%) |
| 5 | 2 (3.51%) |
| Were you able to stay in contact with your physician or nurse? | |
| Yes | 40 (70.17%) |
| No | 17 (29.82%) |
| Do you use ventilatory support at any time of the day? | |
| Yes | 25 (43.86%) |
| No | 32 (56.14%) |
| Did you have any problems with mechanical ventilation during lockdown or the de-escalation period? | |
| Yes | 4 (16%) |
| No | 21 (84%) |
Four of the 25 patients requiring non-invasive mechanical ventilation (16%) presented complications, which they were able to solve in remote medical consultations. Finally, 2 of the 9 patients with gastrostomy tubes reported problems during lockdown; one of these had to attend hospital.
DiscussionThe absence of cases of COVID-19 in our sample may be explained by the fact that these patients are highly dependent and present mobility problems, requiring assistance with daily living activities; therefore, their living conditions were already somewhat similar to lockdown. Our results show that these patients frequently live in large family units and that their relatives or caregivers frequently lack personal protective equipment. This is particularly relevant considering that the main source of infection in these patients is caregivers and household members.
According to data from the United States published by the Northeast ALS Consortium, the current pandemic has significantly limited the number of in-person consultations with new and returning patients.6 Our findings provide further evidence of this phenomenon and underscore the need to expand telemedicine services. Lockdown rules have accelerated the implementation of telemedicine; prior to the outbreak of the pandemic, telemedicine infrastructure was suboptimal.
Finally, the fact that a considerable percentage of patients had to change their caregivers is also noteworthy, given the associated emotional and organisational implications. In fact, the incidence of anxiety and feelings of loneliness has increased among patients with ALS and their relatives/caregivers during the pandemic.7,8
The current situation has revealed weaknesses in the healthcare network involved in the management of patients with ALS; this infrastructure should be strengthened to protect these patients in such adverse circumstances. The COVID-19 pandemic has underscored the need for greater professionalisation of caregivers, the huge importance of promoting telemedicine at multidisciplinary units, and the need for greater availability of personal protective equipment.
We would like to thank Esther Sellés and Anna Rigola of the Miquel Valls Foundation, and our patients and their families and caregivers.
Please cite this article as: Bertran Recasens B, Povedano Panadés M, Rubio MA. Impacto de la pandemia de COVID-19 en una cohorte de pacientes con ELA en Cataluña. Neurología. 2021;36:187–189.