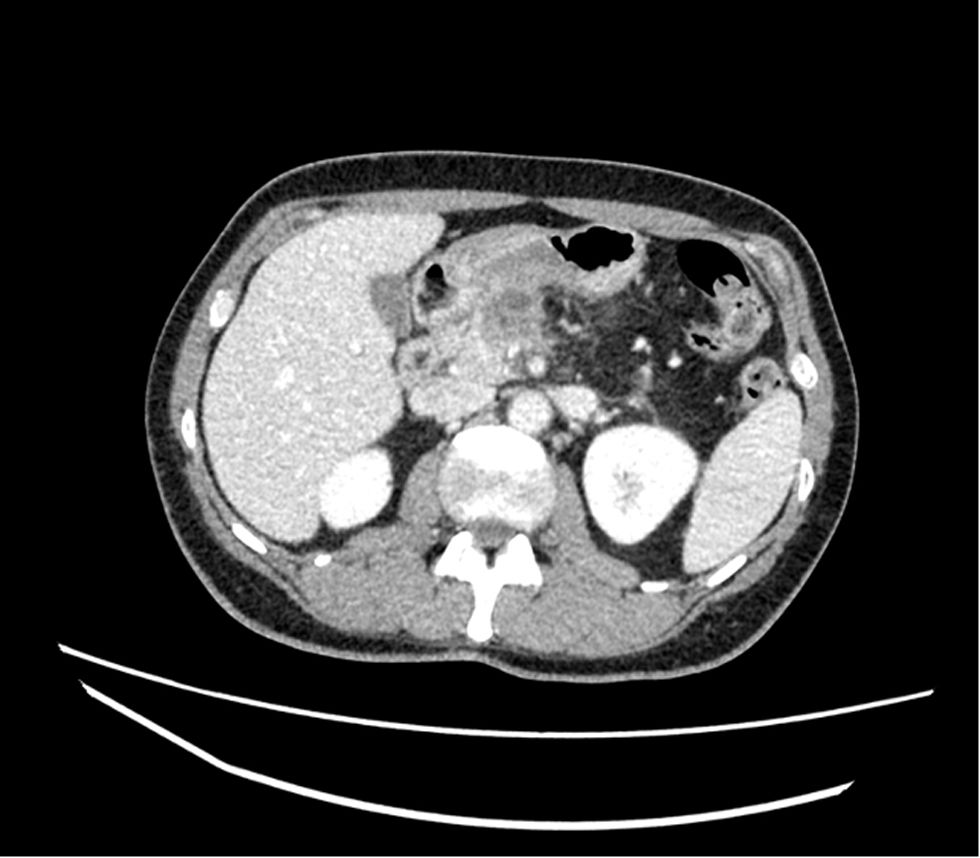
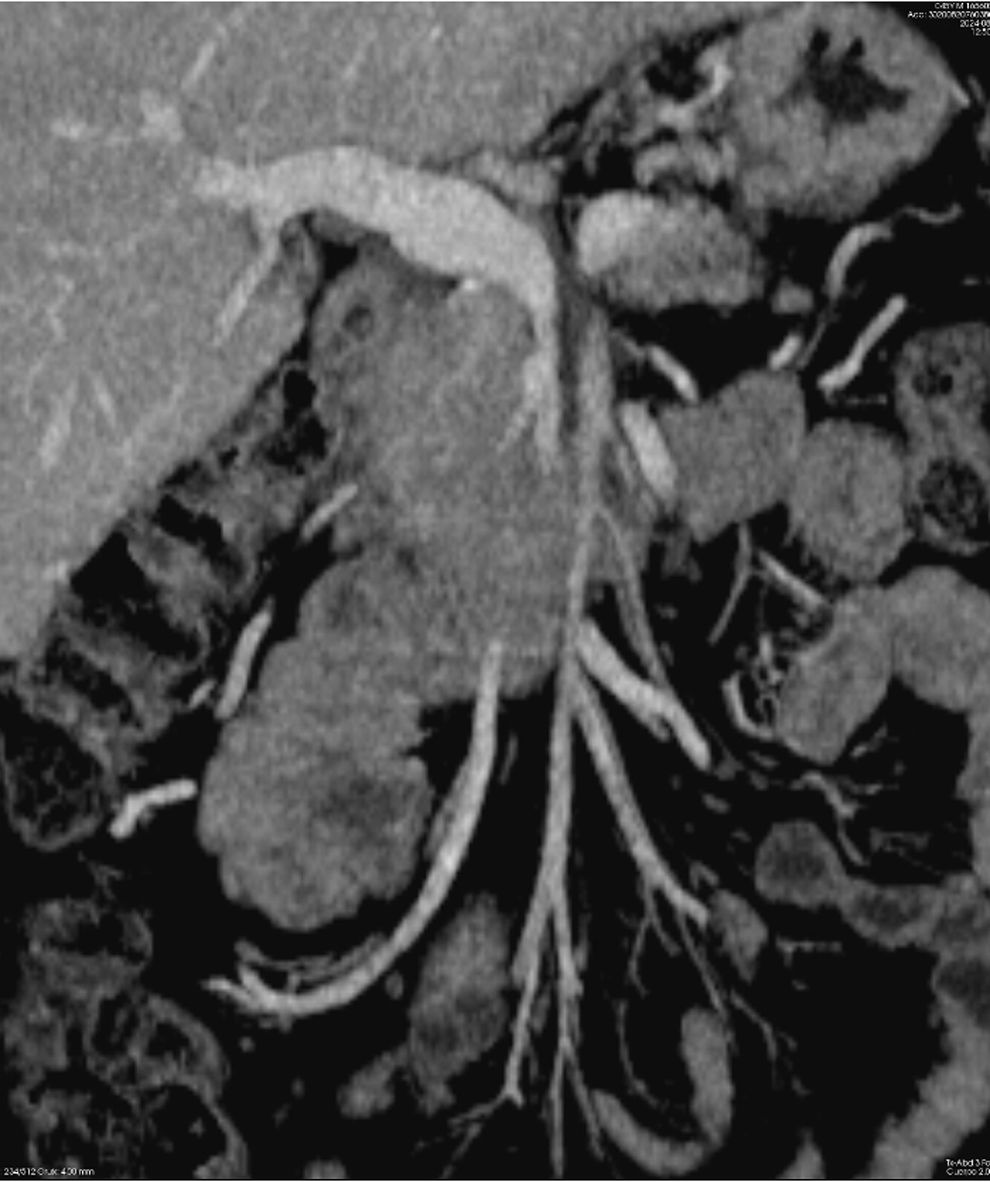
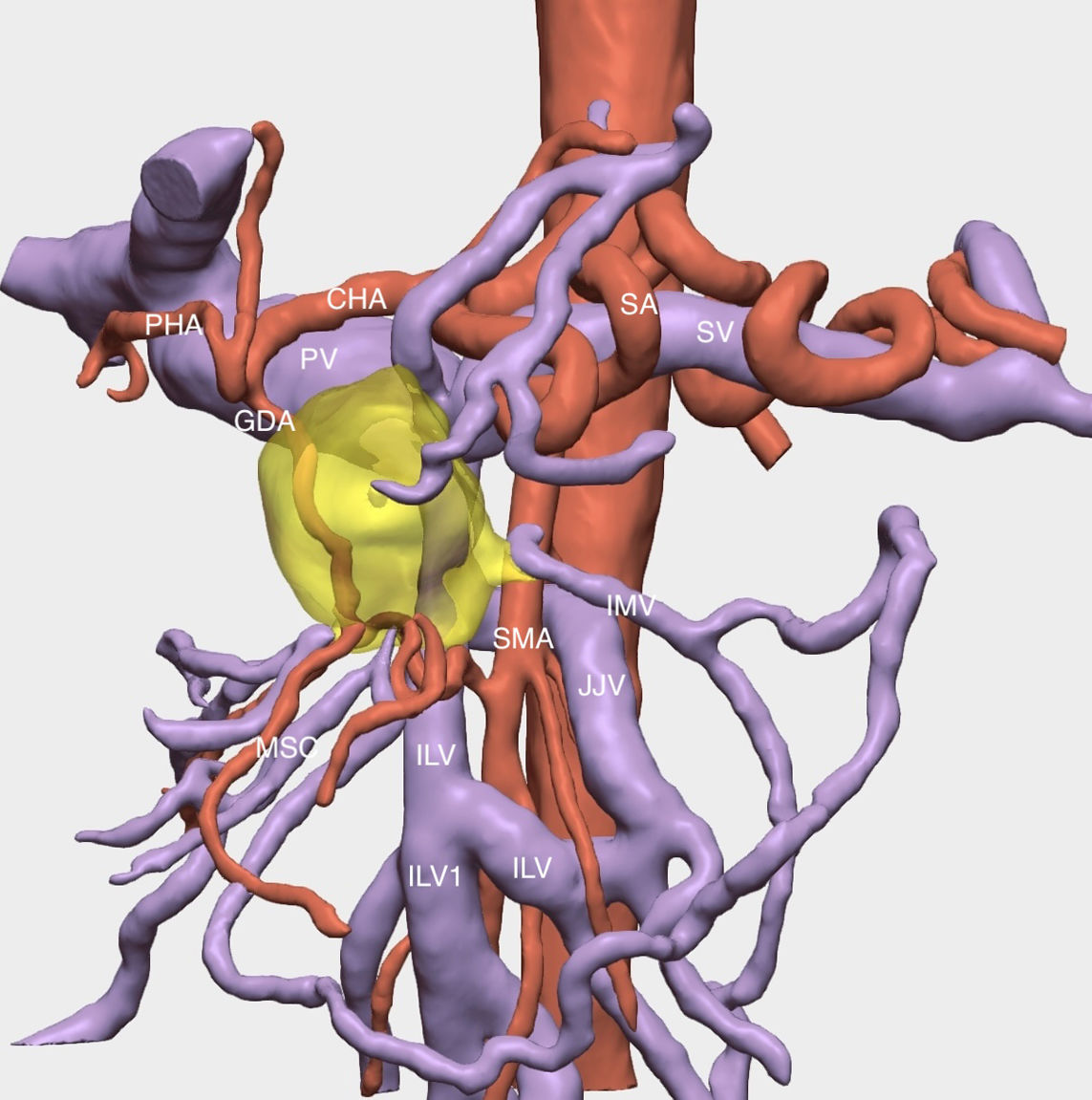
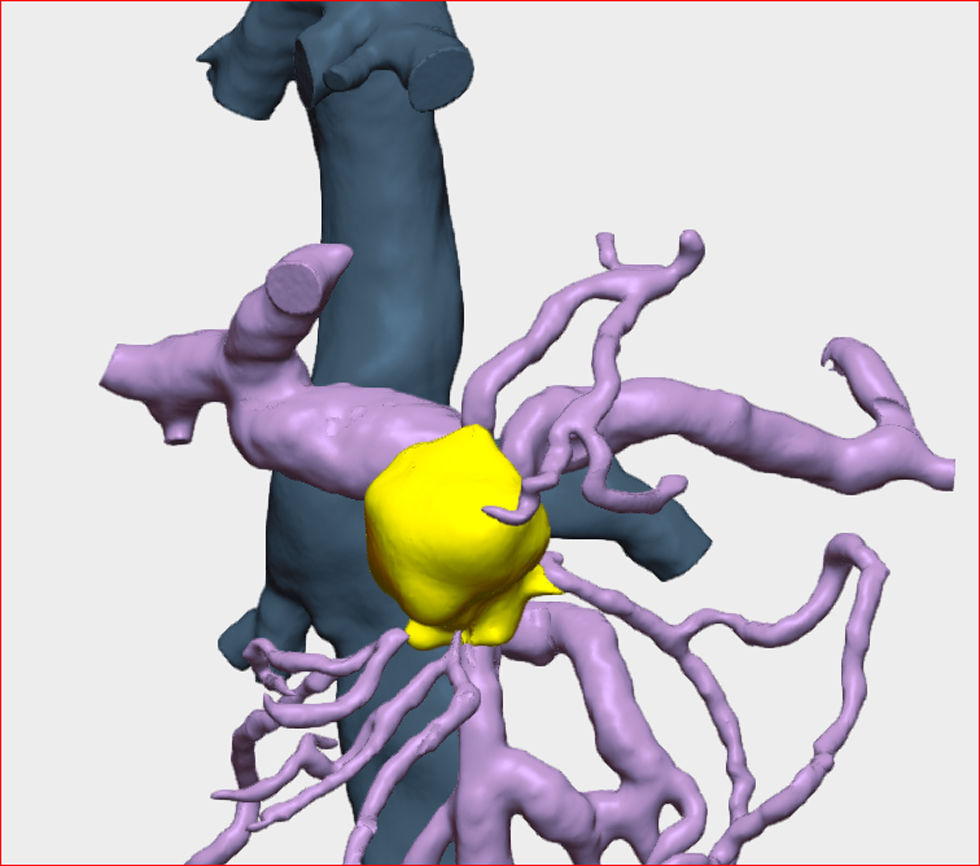
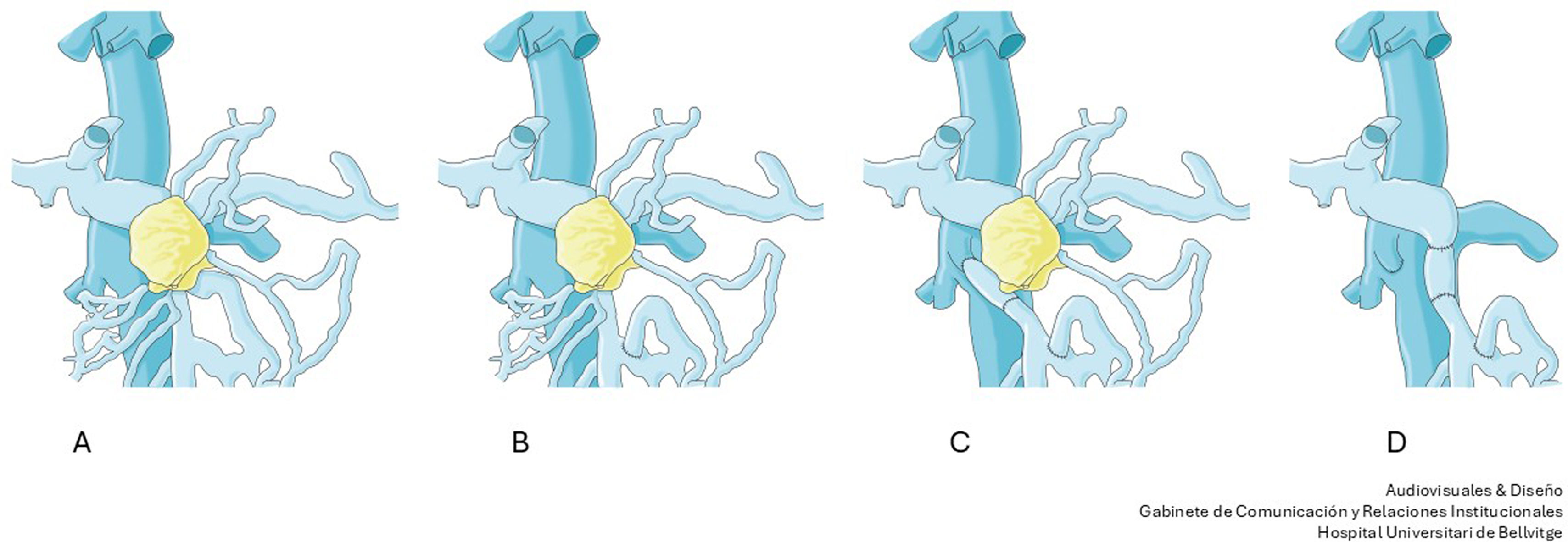
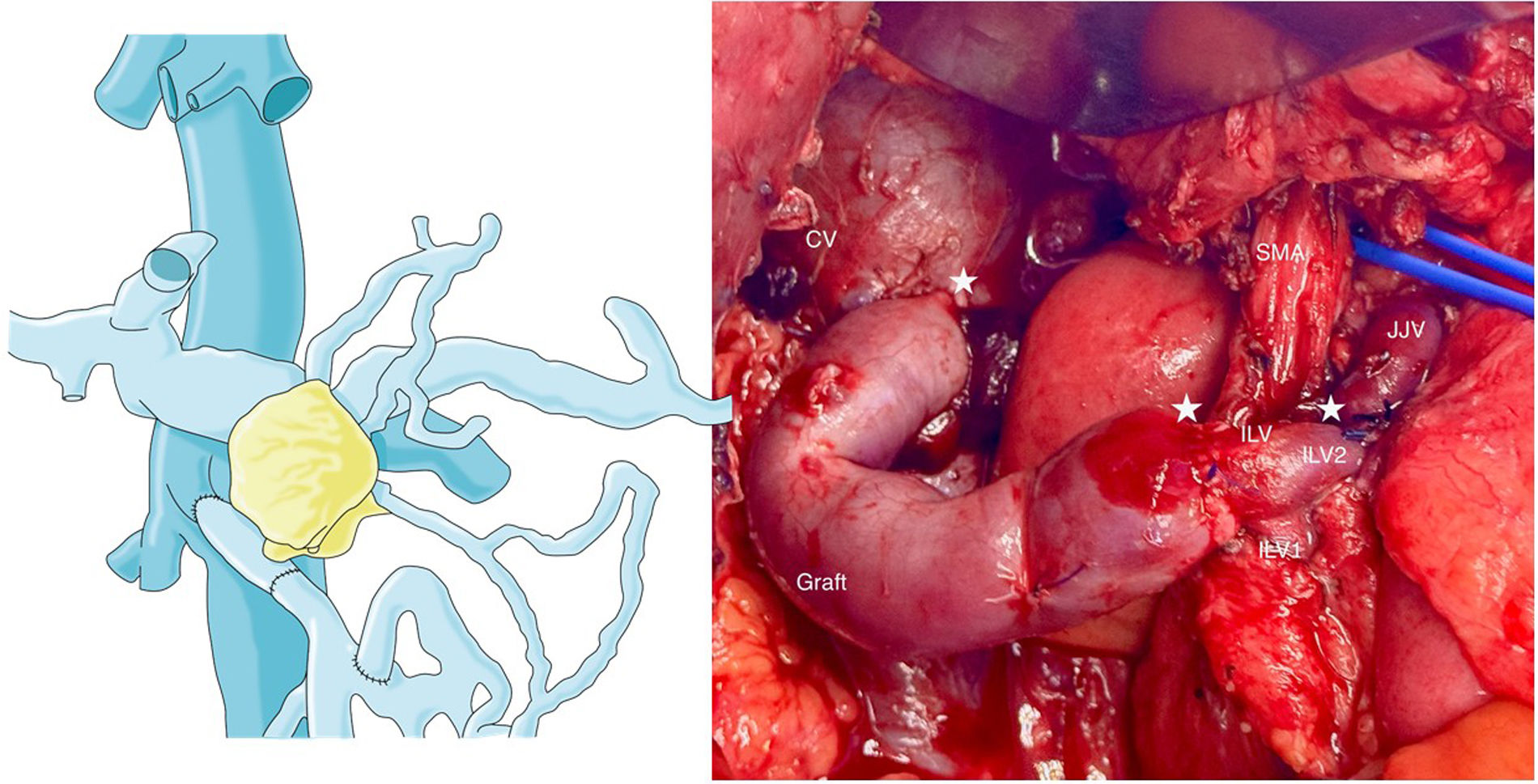
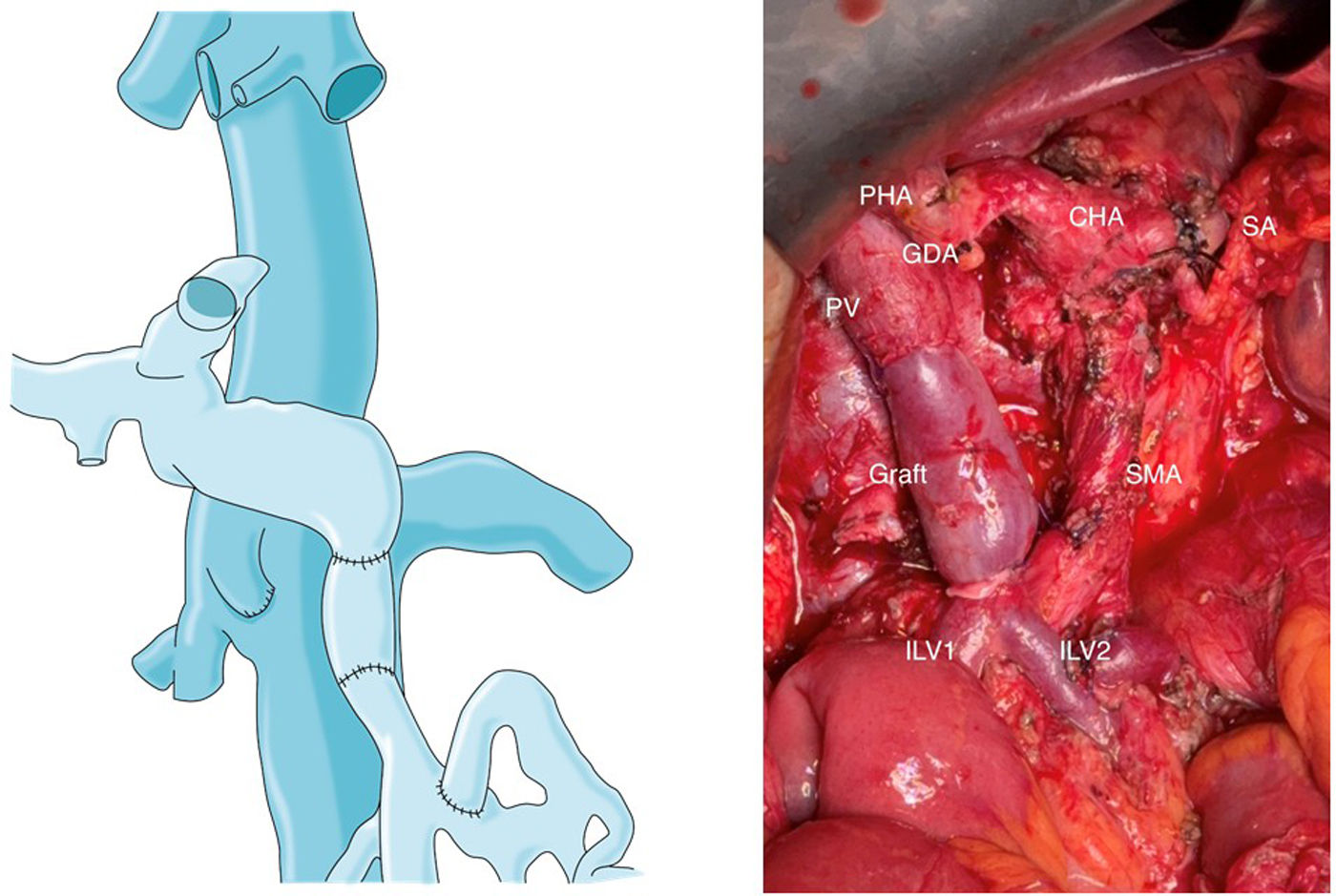
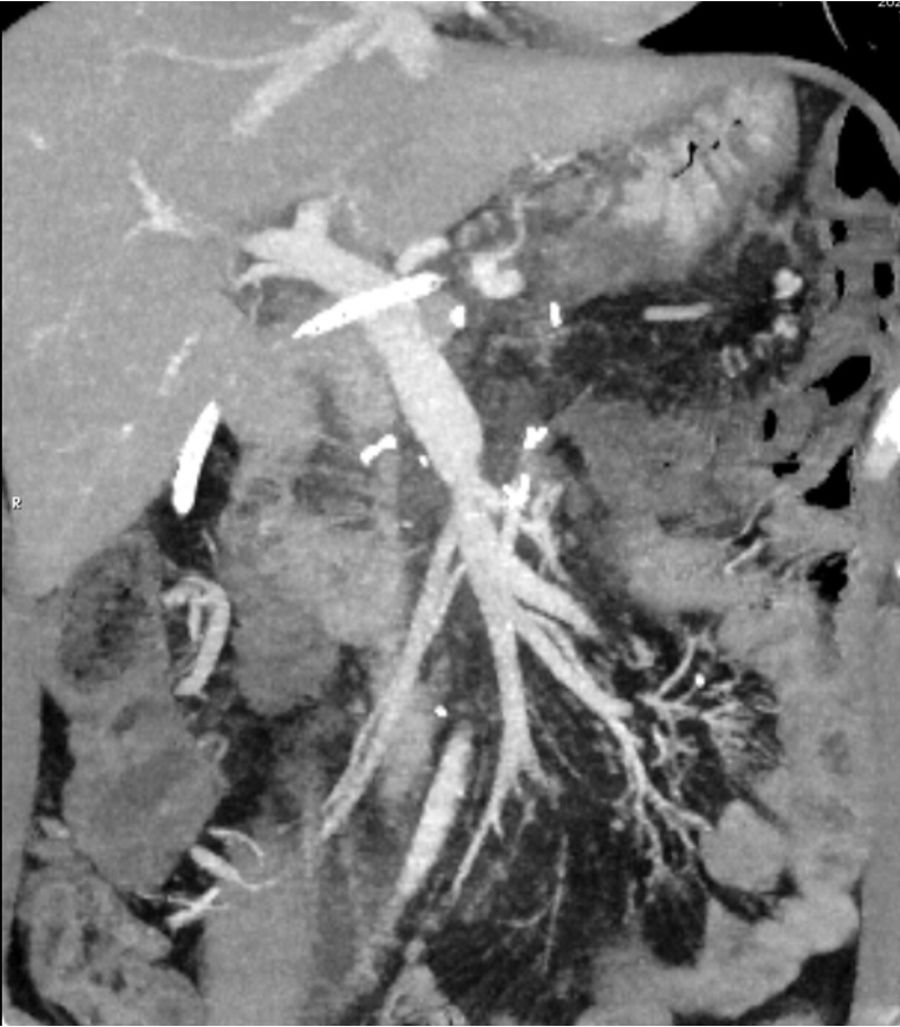
The resection of locally advanced adenocarcinoma of the pancreatic head with occlusion of the superior mesenteric vein and involvement of the splenomesenteric portal confluence (EMP) sometimes requires prolonged venous clamping with risk of intestinal ischemia. The use of intraoperative venous shunts has been published by reference groups to allow successful resection. In our centre we performed a total pancreatoduodenectomy for locally advanced pancreatic head adenocarcinoma with superior mesenteric vein occlusion (SMV) and splenomesenteric portal confluence. The use of a temporary ileo-caval shunt via a venous graft allowed resection of the tumour without repercussion on the bowel. The surgery ended with closure of the shunt, anastomosis of the graft to the portal vein and digestive reconstruction. The patient presented good tolerance to surgery and was discharged on the 7th postoperative day. The pathology report described pancreatic adenocarcinoma ypT1N0(R0) regression grade GRT2/IIa, with 0/30 affected adenopathies.
La resección de adenocarcinoma de cabeza de páncreas localmente avanzado con oclusión de la vena mesentérica superior y afectación del confluente esplenomesentéricoportal (EMP) obliga en ocasiones a un clampaje venoso prolongado con riesgo de isquemia intestinal. La utilización de shunts venosos intraoperatorios ha sido publicado por grupos de referencia para permitir la resección con éxito. En nuestro centro realizamos una duodenopancreatectomía total por adenocarcinoma de cabeza de páncreas localmente avanzado con oclusión de vena mesentérica superior (VMS) y confluente esplenomesentéricoportal. El uso de un shunt ileo-caval transitorio mediante un injerto venoso permitió la resección del tumor sin repercusión en el intestino. La cirugía finalizó con el cierre del shunt, anastomosis del injerto a la vena porta y reconstrucción digestiva. El paciente presentó buena tolerancia a la cirugía, siendo dado de alta el 7 ° día postoperatorio. El estudio anatomopatológico describió adenocarcinoma pancreático ypT1N0(R0) grado regresión GRT2/IIa, con 0/30 adenopatías afectas.