Complete oncological resection (R0) is the main determinant for survival in pancreatic cancer. In order to achieve R0 resection, vascular reconstruction is sometimes required.
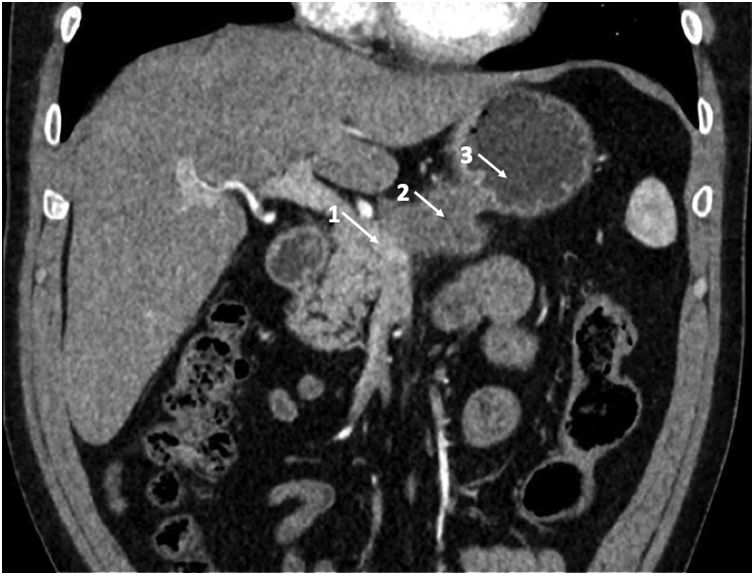
We present the case of a 50-year-old male patient diagnosed by computed tomography (CT) (Fig. 1) and abdominal magnetic resonance scans with a tumor in the pancreatic body measuring 53×29mm, with involvement of the splenoportal confluence and gastric antrum. An endoscopic ultrasound was performed to obtain a sample for histology study, which was compatible with adenocarcinoma of biliopancreatic origin. Positron emission tomography ruled out distant disease.
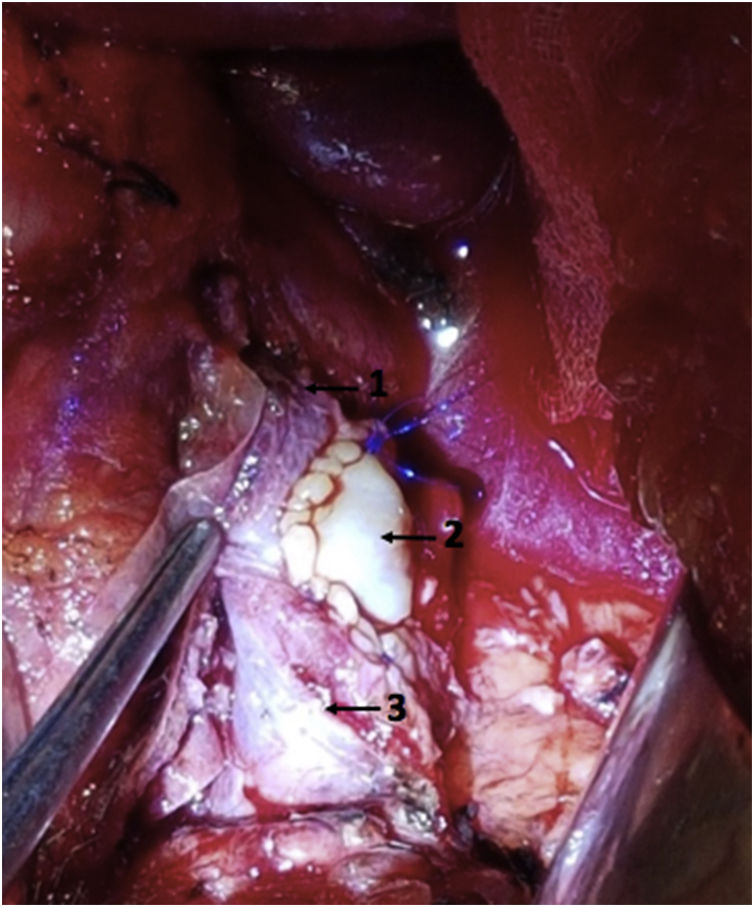
During surgery, involvement of the lateral side of the portal vein was confirmed. An en bloc resection of the body and tail of the pancreas was performed with lateral resection of the portal vein, subtotal gastrectomy and splenectomy. Vascular reconstruction was carried out with a lateral autograft from the falciform ligament using continuous 5/0 prolene suture (Fig. 2).
The definitive pathology result confirmed pancreatic ductal adenocarcinoma with infiltration of the gastric wall and lateral wall of the portal vein, with free resection margins. Two peripancreatic ganglia were affected (2/11), pT4N1.
The patient presented no postoperative complications and was discharged on the sixth day. He was administered thromboembolic prophylaxis with low-molecular-weight heparin for one month. The CT scan performed one month after the surgery demonstrated permeability of the vascular graft.
Porto-mesenteric infiltration is common in tumors of the head and body of the pancreas. In these cases, venous resection is necessary to achieve complete removal of the tumor.1
Venous reconstruction can be performed in most cases by primary anastomosis. When this is not possible, an autologous graft can be used in cases of small defects or prosthetic material after major resections.2
Numerous autologous graft options have been described, including venous grafts (saphenous, femoral, external iliac, jugular, umbilical, etc.) and peritoneal grafts.1 The use of the latter was described by Kurbangaleev in 1965. Peritoneal autologous grafts are non-thrombogenic and have some advantages, including being easily obtainable and low in cost.1
A recently described alternative is the use of the falciform ligament,3 which has an advantage over peritoneal grafts as it is a double membrane structure that lends greater strength1 and can be used on both sides.
In our patient, the use of the falciform ligament as a graft provided for reconstruction of the venous defect in a simple, economical manner, with excellent functional results and free of complications. The falciform ligament can be considered an alternative in venous reconstruction when a graft is necessary during pancreatic surgery.
Please cite this article as: Galofré-Recasens M, Herrero Fonollosa E, Camps Lasa J, García-Domingo MI, Cugat Andorrà E. Injerto autólogo de ligamento falciforme para la reconstrucción vascular en cirugía oncológica de páncreas. Cir Esp. 2019;97:54–55.