Most cases of acute otitis media resolve with antibiotics and imaging is not required. When treatment fails or a complication is suspected, imaging plays a crucial role. Since the introduction of antibiotic treatment, the complication rate has decreased dramatically. Nevertheless, given the critical clinical relevance of complications, the importance of early diagnosis is vital.
Our objective was to review the clinical and radiological features of acute otitis media and its complications. They were classified based on their location, as intratemporal or intracranial.
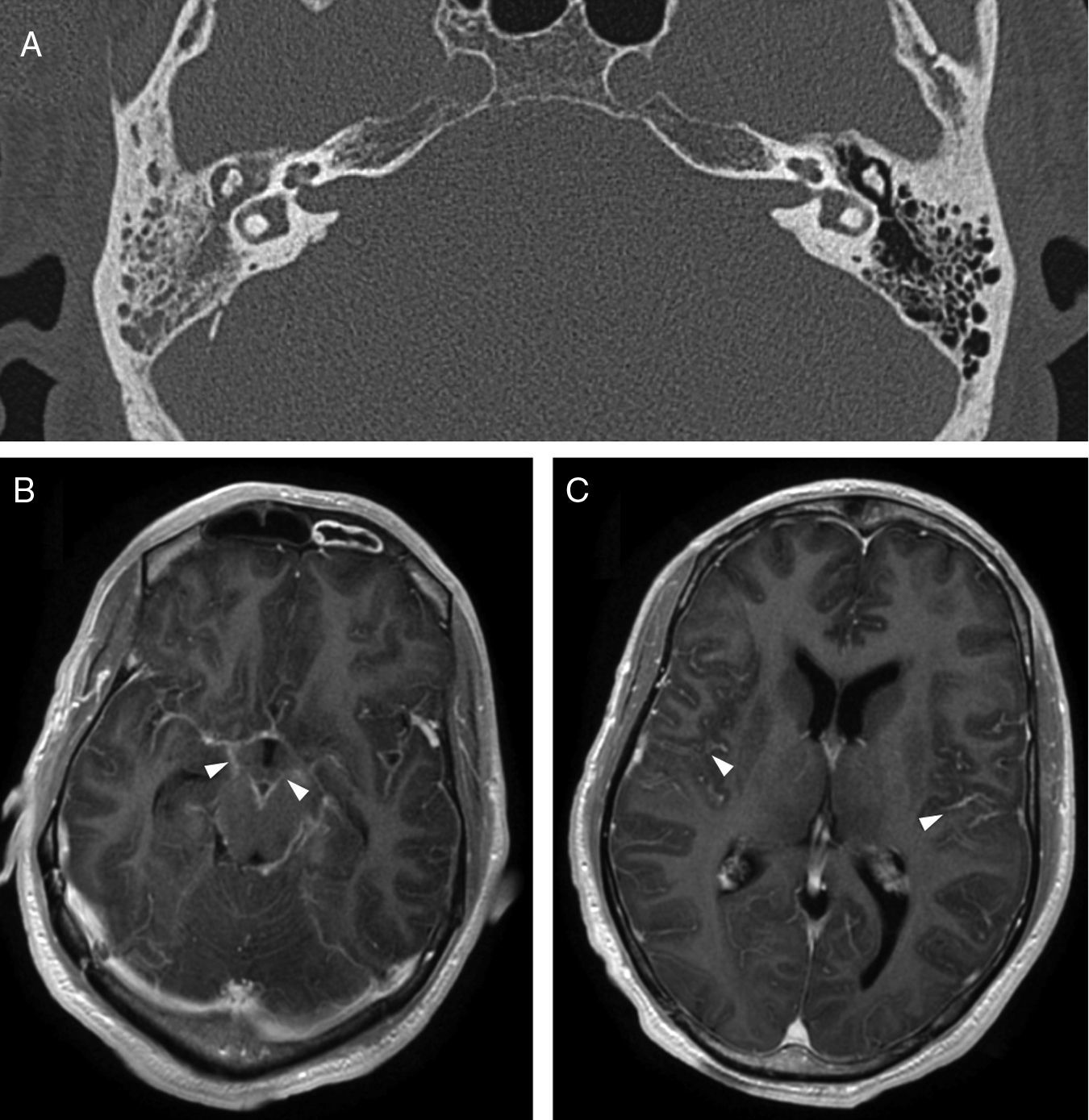
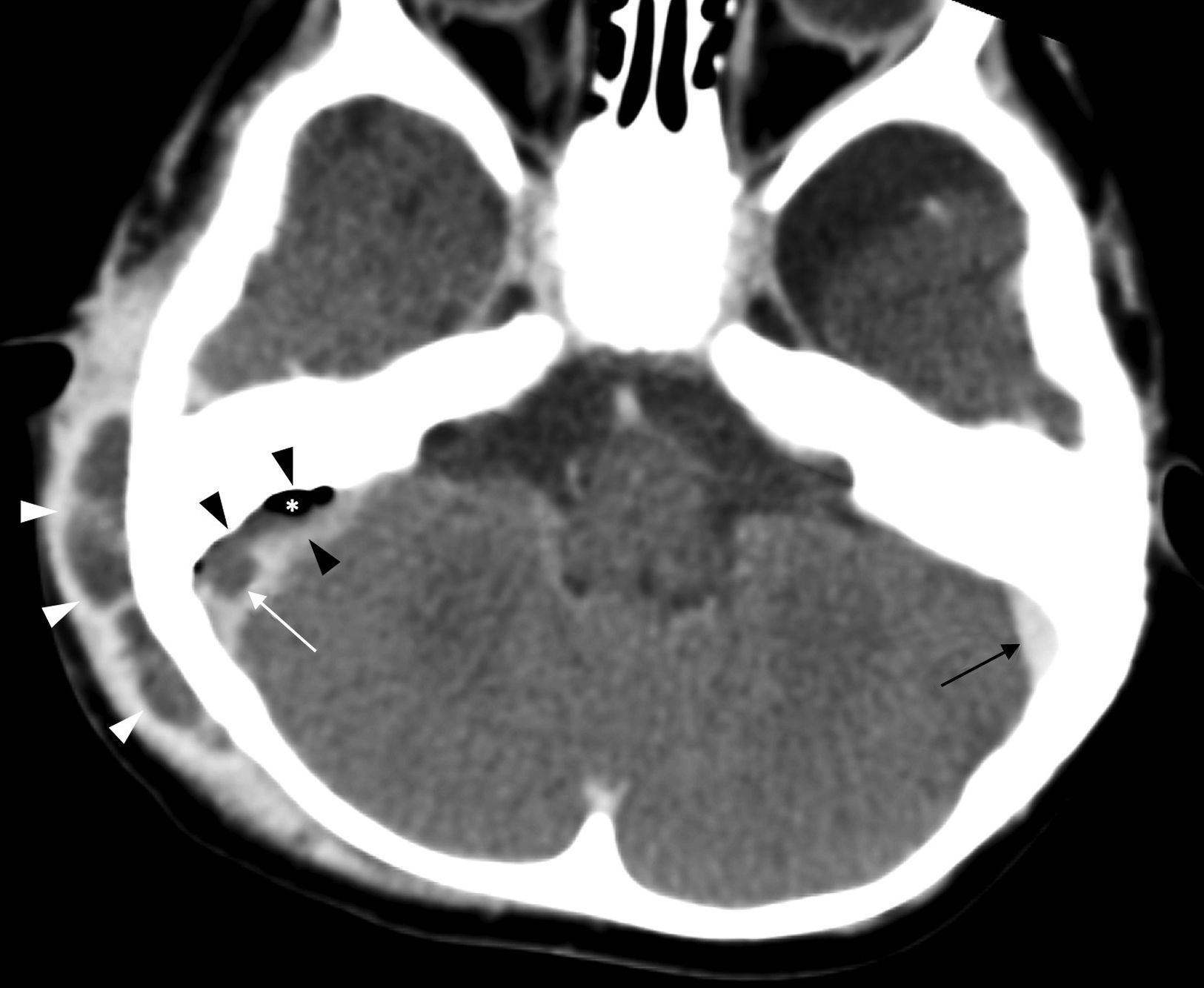
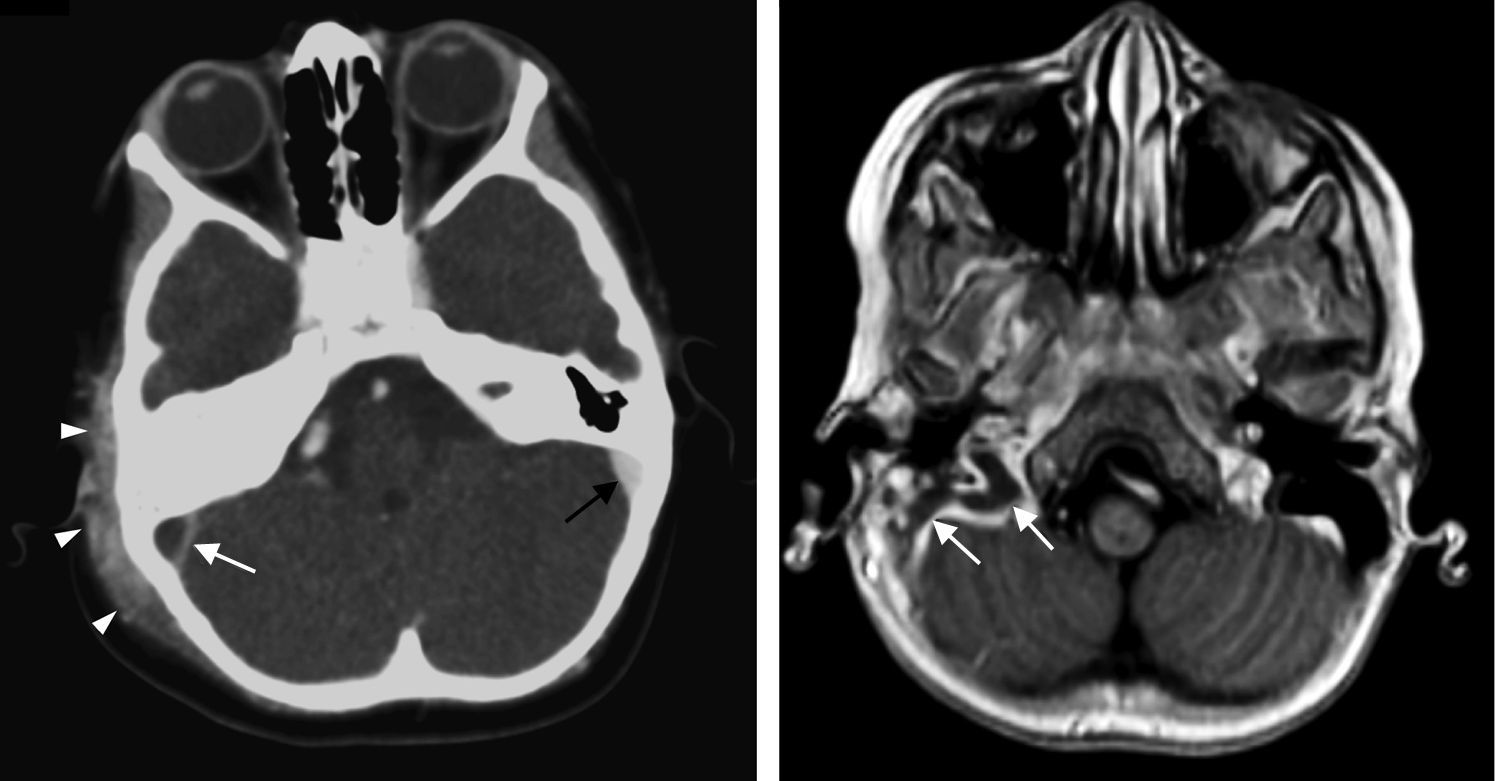
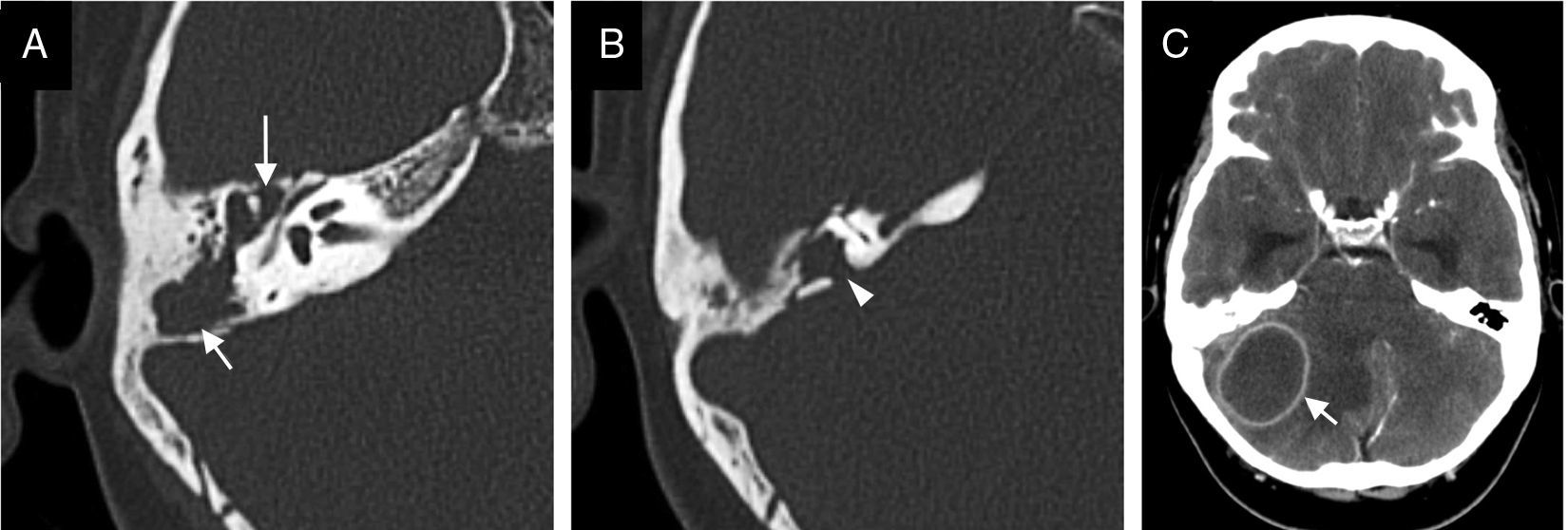
Imaging makes it possible to diagnose the complications of acute otitis media and to institute appropriate treatment. Computed tomography is the initial technique of choice and, in most cases, the ultimate. Magnetic resonance is useful for evaluating the inner ear and when accurate evaluation of disease extent or better characterisation of intracranial complications is required.
La mayor parte de casos de otitis media aguda se resuelven con el tratamiento farmacológico, y los estudios de imagen no están indicados. En los casos en los que el tratamiento fracasa o se sospecha complicación, las pruebas de imagen tendrán un papel fundamental. Desde la introducción del tratamiento antibiótico la frecuencia de complicaciones ha disminuido drásticamente. No obstante, dada su relevancia clínica crítica, es de vital importancia su diagnóstico precoz.
Nuestro objetivo es revisar las manifestaciones clínicas y radiológicas de las complicaciones de la otitis media aguda, que clasificaremos según su localización en intratemporales e intracraneales.
Las pruebas de imagen permiten diagnosticar la complicaciones de la otitis media aguda y establecer el tratamiento idóneo de forma precoz.
La tomografía computarizada es la técnica de elección inicial, y en la mayor parte de casos la definitiva. La resonancia magnética se reservará para la valoración del oído interno y para los casos en los que sea necesaria una delimitación o caracterización más precisa de las complicaciones intracraneales.