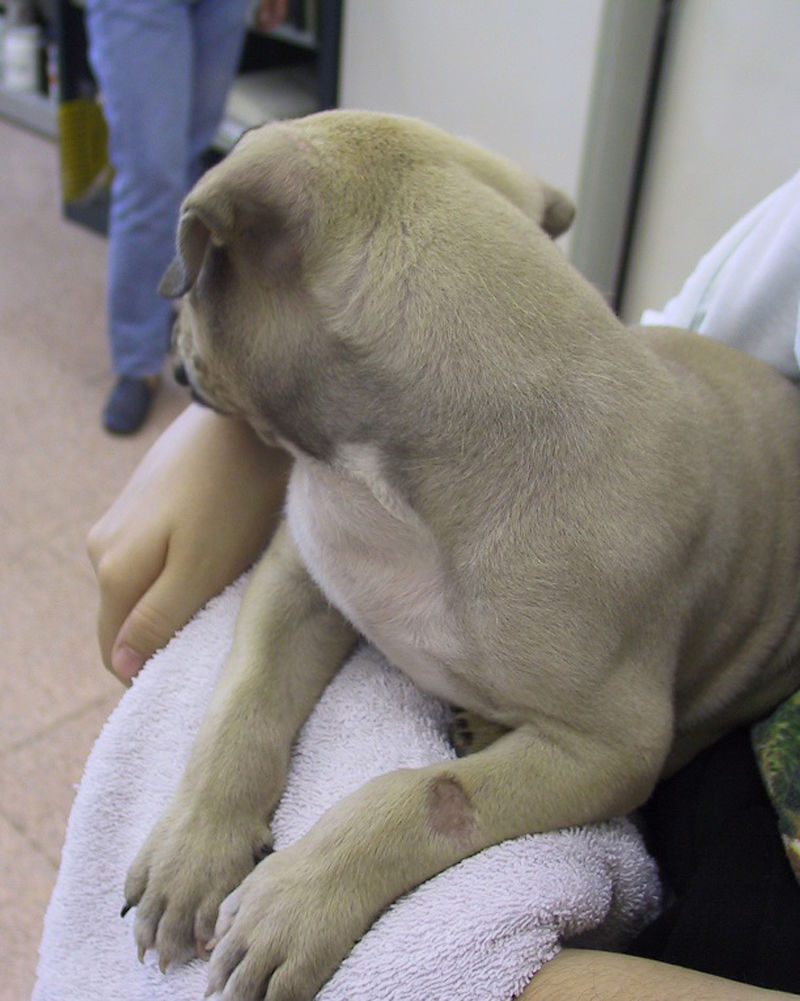
Dermatophytes continue to be cited as one of the most common causes of skin problems in domestic animals. However, only a small percentage of these fungal species usually cause ringworm in them.1 As I recently mentioned in an article of this Animal Mycology forum series,2 the names of some of the species that cause dermatophytosis have changed and are now included in the genera Lophophyton, Nannizzia, Microsporum and Trichophyton. It should be noted that animals are reservoir hosts of the so-called zoophylic dermatophytes and their infections have considerable zoonotic importance as they are transmitted to humans with some frequency. For example, the cat is the main reservoir of Microsporum canis. This species is the most common cause of ringworm in dogs and cats. In cats, the percentage of isolation of M. canis is usually over 90%. In both animal species dermatophytosis is a frequent disease in young individuals (Fig. 1).
As stated in the latest consensus recommendations on the diagnosis and treatment of dermatophytosis in cats and dogs3, provided within the scope of the World Association of Veterinary Dermatology, M. canis is among the main microorganisms along with Campylobacter spp., Salmonella spp., and Toxoplasma gondii, which are often considered of greater concern to be transmitted by pets to high-risk owners.
However, as outlined in these guidelines, despite being dermatophytosis a known zoonosis that causes skin lesions in humans, it is treatable and curable. Nevertheless, these authors point out that there are few studies that have accurately investigated the rate of human dermatophytosis attributable to pets. Pet-associated diseases can occur in any individual, but children under the age of 5, adults over 65, pregnant women and people with immunocompromised conditions are at greater risk.
This disease is mainly transmitted by contact with the fur or skin lesions of an infected animal. Scales and hair from these animals can accumulate in the environment and are possible sources of infection. This is mainly due to the large number of arthroconidia formed in the hair of animals with dermatophytosis, which generally have diameters of less than 5 micrometers and are the cause of the infection (Fig. 2). However, it is difficult to determine the true prevalence of this disease, as it is not considered a reportable infectious disease. Although in these recommendations none of the commonly used diagnostic tests is considered the “gold standard”, it is pointed out that it is important to know which techniques allow us to confirm the presence or absence of an active infection in the animal. Laboratory diagnosis includes traditional techniques such as direct microscopic examination of hairs (Fig. 2), a test characterized by an unquestionable specificity but with moderate sensitivity. Diagnosis is usually confirmed by culture of hairs in proper media, a test that has high sensitivity and also allows the identification of the species involved. Culture also allows the detection of transient mechanical carriers, asymptomatic initial infections and monitoring response to antifungal therapy. PCR techniques can be useful, although it should be remembered that they can give false positive results in cases of non-active infections by detecting DNA from non-viable fungal elements. As it is mentioned in these guidelines, successful treatment requires the concurrent use of systemic oral antifungals, such as itraconazole or terbinafine, and a topical disinfection of the hair coat.
Direct microscopic examination of an area near the hair bulb. Numerous arthroconidia can be seen around the hair, which are the infectious fungal elements responsible for the spread of the disease. This infection pattern is common in animal dermatophytoses and is called ectothrix. Lactophenol blue stain.
Author has no conflict of interest.
Financial support came from Servei Veterinari de Bacteriologia i Micologia of the Universitat Autònoma de Barcelona.
These Mycology Forum articles can be consulted in Spanish on the Animal Mycology section on the website of the Spanish Mycology Association (https://aemicol.com/micologia-animal/).