Gonococcal keratoconjunctivitis is a rapidly progressing and aggressive infection caused by Neisseria gonorrhoeae. We report a case of a patient who presented keratoconjunctivitis with an opacity in the left cornea that progressed into an ulcerative lesion despite initial treatment with antibiotic eye drops. Gram stains from the purulent discharge of the left eye showed gram-negative diplococci, and the culture from the ocular discharge was positive for Neisseria gonorrhoeae. Resolution was achieved with the administration of 2g of intramuscular ceftriaxone in a single dose, and the patient had no sequelae.
La queratoconjuntivitis gonocócica es un infección agresiva y de rápida progresión causada por Neisseria gonorrhoeae. Reportamos el caso de un paciente quien presentó queratoconjuntivitis con opacidad corneal izquierda, la cual progresó a lesión ulcerativa a pesar del tratamiento inicial con antibiótico en gotas oftálmicas. La tinción de Gram y el cultivo a partir de la secreción purulenta del ojo izquierdo mostró diplococos gramnegativos y crecimiento de Neisseria gonorrhoeae, respectivamente. La curación del paciente se logró tras la administración de 2 g de ceftriaxona intramuscular en dosis única; el paciente no presentó secuelas.
Gonococcal keratoconjunctivitis is a rapidly progressing and aggressive infection caused by Neisseria gonorrhoeae.1 Clinical course typically causes acute pain, conjunctival injection, chemosis and a profuse purulent discharge that can progress to perforation and vision loss.1 Treatment must be initiated as soon as possible, even before the result of the culture due to the aggressive nature of the infection; this includes intramuscular antibiotics, in addition to topic ones.1
We report a case of a patient who presented keratoconjunctivitis with an opacity in the left cornea that progressed into an ulcerative lesion.
Case descriptionA 30-year-old white male, professional soldier, with no relevant previous medical history, presented to the emergency room in July 2013 with decreased visual acuity, photophobia and purulent discharge in left eye for 5 days; the patient denied other symptomatology, history of recent travel, ocular trauma or immersion in pools or lakes. He referred monogamous sexual activity.
On physical examination the patient had a temperature of 37.3°C, blood pressure of 118/75mmHg, heart rate of 85bpm, respiratory rate of 22 and Glasgow coma scale 15/15, left eye with conjunctival injection, purulent discharge and no visible foreign body, posterior segment examination showed no alteration; oral mucosa, genital and anal area had no alterations, there were no other relevant systemic findings.
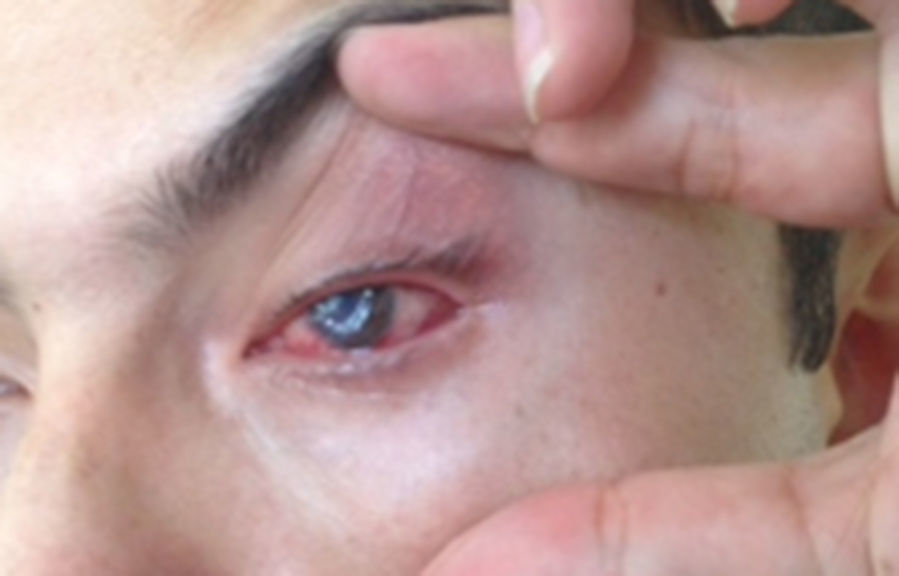
He was evaluated by the service of ophthalmology who diagnosed keratoconjunctivitis and initiated topic ophthalmic treatment with antibiotic eye drops (Polymyxin B [5000U], Gramicidin [0.025mg] and Neomycin [1.75mg]). Despite the established treatment, 48h later the patient continued with impaired visual acuity and anterior ophthalmological examination showed an opacity in the left cornea that progressed into an ulcerative lesion (Fig. 1) in the following 24h, for that reason the Infectious Diseases department was called upon for further evaluation and treatment.
The patient's complete blood count showed a leukocyte count of 11,000cells/μL with neutrophil count of 6421cells/μL, erythrocyte count of 5,300,000cells/μL and platelet count of 254,000platelets/μL; HIV rapid test was negative.
Gram stain from the left eye purulent discharge showed Gram negative diplococci and the culture from the ocular discharge was positive for Neisseria gonorrhoeae, confirming the diagnosis of gonococcal keratoconjunctivitis. The patient was given 2g of intramuscular ceftriaxone single dose as treatment, with a satisfactory resolution of his clinical course and no sequelae. We were able to reach the patient's sexual partner; she had no ocular, oral, genital or anal alterations, and the rest of her physical examination was completely normal, however, as they had sexual intercourse within the last 60 days before diagnosis, she received 250mg of intramuscular ceftriaxone single dose; she had no other sexual transmitted diseases tested.
DiscussionGonococcal keratoconjunctivitis typically occurs in males, especially with promiscuous life style1 by direct inoculation with infected body fluids1–3; it is usually unilateral,1 with an incubation period after contact between 3 and 19 days.4
Clinical course typically causes acute pain, conjunctival injection, chemosis and a profuse purulent discharge that can rapidly progress to perforation and vision loss.1 Other findings at physical examination include keratitis, corneal thinning, anterior segment inflammation, periorbital edema and pre-auricular lymphadenopathy.1
The particular ability of Neisseria gonorrhoeae of invading intact corneal and conjunctival epithelium is due to the presence of pili in certain strains of the bacteria, as nonpiliated gonococci are not able to adhere to the corneal epithelium. Once the bacteria has successfully adhered to the epithelium, they are engulfed by epithelial cell protrusions; approximately after 8–24h of exposure, the superficial infected cells tend to desquamate into the medium, facilitating the infection of deeper layer cells, as transcellular migration of the bacteria does not occur. The release of toxins does not seem to be an important factor in the initial stage of gonococcal infection of the human cornea.5
With ocular gonococcal infection in adults not being frequent, diagnosis can be delayed in many cases2; initially, conjunctival scraping samples can be taken for a Gram stain, in which intracellular diplococci may be evident, however the early realization of a culture of the ocular discharge for the isolation of this microorganism confirms the diagnosis.3,4 A study conducted in a referral center in Bangkok, Thailand by Sirikul et al. with the objective of determining predisposing factors, demographic characteristics, and etiology of ulcerative keratitis, with a total of 130 isolates, obtained as a result that among the various pathogens capable of causing corneal alterations (i.e., bacteria, fungi, viruses, or parasites), Pseudomonas spp. was the most frequent bacteria isolated with 55% of bacterial isolates, followed by Streptococcus spp. with 15% of bacterial isolates; Fusarium spp. and Aspergillus spp. were the most common fungal pathogens isolated with 26.5% and 18% of fungal isolates respectively; from the overall number of isolates, 3 were Acanthamoeba spp.6
Coinfection between Neisseria gonorrhoeae and Chlamydia trachomatis in conjunctivitis is a rare pathology and information about its incidence is not yet available, however genital coinfection incidence goes up to 45.7% in the United States7; Arvai et al. presented a case of a 33-year-old man with yellow purulent discharge, photo sensibility, and blurred vision of 3 weeks, who had received eye drops plus anti-histaminic drugs with no response. Neisseria gonorrhoeae and Chlamydia trachomatis were identified using cultures and polymerase chain reaction, the patient received ceftriaxone, cefixime, azithromycin and eye drops containing tetracycline presenting slow clinical improvement, with a full recovery of visual acuity.8
Treatment must be initiated as soon as possible,2 even before the result of the culture due to the aggressive nature of the infection3; this includes intramuscular and/or to topic antibiotics.2 If patients are treated appropriately before the corneal perforation, risks of sequelae are less, and visual acuity will be preserved.1
The CDC recommends that patients with gonococcal keratoconjunctivitis should receive treatment with ceftriaxone 1g intramuscular in a single dose based on a study where 13 confirmed cases of gonococcal conjunctivitis responded appropriately, with negative cultures 6 and 12h after treatment.9,10
In 1990 the World Health Organization (WHO) called for a global surveillance network for gonococcal antimicrobial susceptibility in order to identify new forms of resistance and to guarantee efficacy of recommended treatments, in which several countries from Latin America and the Caribbean, including Colombia, participated through 2011. A total of 21,592 Neisseria gonorrhoeae isolates were tested for antimicrobial susceptibility; from 5171 isolates tested for ceftriaxone susceptibility between 2007 and 2011, 0.4% were reported to have reduced susceptibility; from 12,730 isolates tested for ciprofloxacin susceptibility resistance was 14.8% overall, resistance was permanently over 15% after 2006, with 42.1% in 2010; from 11,135 isolates tested for azithromycin susceptibility resistance was 10% overall, resistance remained above 6% between 2000 and 2009; penicillin resistance remained above 24% of isolates tested throughout 1990–2011, with 35.2% in 2011; the contribution of plasmid-mediated penicillin resistance was higher compared with chromosomally mediated penicillin resistance to overall penicillin resistance from 1990 to 2009; the last one steeply increased in 2010 and 2011; the overall percentage of resistant isolates to tetracycline remained above 21% throughout the surveillance period.11
Additionally, saline eyewash and topical antibiotics have been recommended as adjunctive therapy in this type of conjunctivitis; however, these are not essential for the therapeutic success in adults.12
Finally, the large amount of microorganisms capable of causing similar pathologies makes gonococcal keratoconjunctivitis diagnosis a complete challenge to the physician, as an earlier and appropriate management is crucial. Taking into account this particular pathology is caused by a sexually transmitted microorganism, a thorough physical examination is needed, as well as laboratory testing, in order to rule out other sexually transmitted diseases, including HIV infection.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this investigation.
Confidentiality of dataThe authors declare that they have followed the protocols of their work centre on the publication of patient data.
Right to privacy and informed consentThe authors declare that no patient data appears in this article.
FundingNone.
Conflict of interestThe authors have no conflicts of interest to declare.
We would like to thank the patient for his cooperation and for providing the necessary information for writing this manuscript.