Cat scratch disease (CSD) usually presents with a regional sub-acute lymphadenopathy after a cat scratch or bite. It is more frequent in children and teenagers, and usually it is a self-limited condition. Atypical and systemic clinical forms have been described in 5–20% of patients. Several organs including parotid gland and central nervous system (CNS) can be involved.1,2 Herein, a case of a patient with CSD presenting a parotid abscess with aseptic meningitis is detailed.
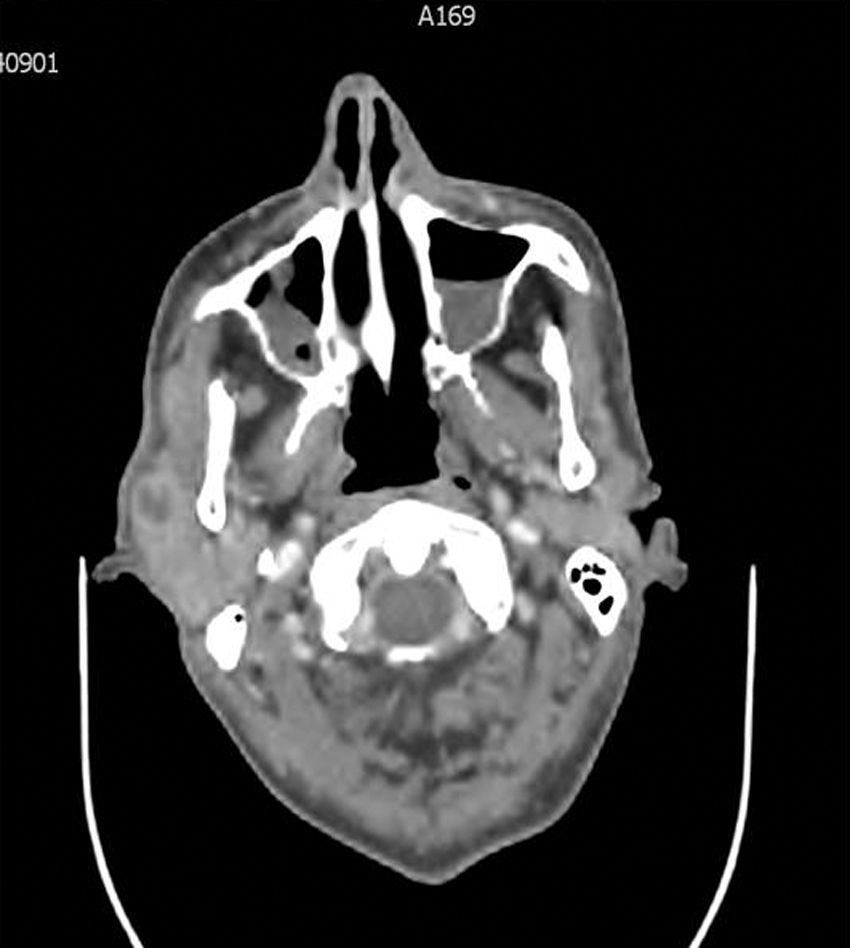
A 74 year-old man, previously healthy, was admitted to the hospital because of fever, chills, night sweats and malaise for 2 weeks. Besides, he reported cervical pain 24h before. He had been evaluated in the emergency room the previous day because of fever and diagnosed of respiratory infection, and was treated with azithromycin. The patient had a cat, although he did not remember any bite or scratch. Physical examination showed axillary temperature of 39°C with normal heart rate and blood pressure. A cervical deviation to the right (torticollis) and small adenopathies were found in the neck. Meningeal signs were not assessable. No other alterations were observed. The white blood count (WBC) was 15,500/mm3, and C reactive protein (CRP) was 48mg/L. The remaining analysis was normal. Chest radiography and abdominal ultrasounds scan were normal. A lumbar puncture was performed and the cerebrospinal fluid (CSF) showed 27cells/mm3 (100% mononuclear) and 0.55g/L of proteins with normal values of glucose and ADA. CSF Gram and auramine staining did not demonstrate microorganisms. Ceftriaxone, vancomycin and ampicillin treatment was started. Three days later the fever and the cervical pain disappeared. A painful tumor on the right parotid gland that was hot and erythematous and a pre-auricular adenopathy were detected. A cervical CT-scan revealed a hypodense lesion with uptake of contrast in the right parotid and bilateral maxillary sinusitis (Figure 1). Magnetic resonance imaging (MRI) of cervical region demonstrated the same findings. Blood cultures were negative. CSF culture and polymerase chain reaction (PCR) assays for Borrelia burgdorferi, Mycobacterium tuberculosis and Bartonella spp. were negative. Serological studies against HIV, Brucella spp., Borrelia burgdorferi and Coxiella burnetti were negative and showed Toxoplasma gondii past infection. An immunofluorescence assay (IFA) against Bartonella henselae showed an IgM titer of 1:200 and IgG titer of 1:3200. Treatment was changed to oral doxycycline and rifampicin. Four days later the patient was discharged with a diagnosis of atypical CSD with parotid abscess and aseptic meningitis. Patient completed treatment for 2 weeks, and 1 month later he had fully recovered. A cervical CT-scan did not show abnormalities and CRP was within the normal range. Six months later, the IgG titer against B .henselae had decreased to 1:800.
To our knowledge, this is the first case reported of B. henselae infection that appeared as parotid abscess and aseptic meningitis. Some clinical aspects are worth mentioned.
Only 6% of CSD patients are elderly people. CSD is more frequent in women at this age, and atypical and severe forms are more frequent.3
Parotid involvement is present in 6% of cervical and head location in CSD4,5 and generally appears in the context of Parinaud's syndrome but this is very rare in elderly patients.1–3 The patient did not show the typical eye affectation and only had a parotid abscess that is the typical involvement of parotid in CSD.5 A rare sign was the presence of torticollis that has been reported in only 1% of cases in cervical CSD, generally associated with deep tissue involvement 4 and that was excluded in our patient by MRI and CT-scans. Encephalitis and neuroretinitis are the most frequent CSD neurologic manifestations.1,2 Encephalitis is more frequent in elderly patients.3 Our patient did not develop convulsions, disorder of consciousness or any signs of focal neurological involvement that are typical of encephalitis. Meningitis is a very rare manifestation, and normally appears in the context of neuroretinitis.6–8 In our patient, the assessment of meningeal signs was difficult in context of neck stiffness and pain secondary to torticollis, but the CSF analysis was indicative of meningeal injury with findings of aseptic meningitis. This fact was essential for the choice of antimicrobials and duration of the therapy. Moreover, our patient did not show ocular involvement or loss of vision suggesting neuroretinitis.
In this case, the diagnosis was made by serologic assays. PCR tests were negative. This fact may be due to the low sensitivity of PCR in some samples and the previous use of antimicrobials. Doxycycline and rifampicin were prescribed since this is the option that experts recommend for CNS involvement.9,10 Our patient favorably evolved, probably due to the early instauration of the treatment. It is known that delayed treatment is a prognosis factor, especially for elderly people.6,9,10