Epstein-Barr virus infections mainly occur during childhood and can cause fever, malaise, lymph node enlargement and hepatosplenomegaly. Although liver function tests alterations are frequent, mainly an increase in the serum transaminase levels, gallbladder involvement is very rare, and most cases have been described in infants. We describe a case of a young adult male who developed acalculous cholecystitis as the first manifestation of infectious mononucleosis, successfully treated with conservative measures.
A 20-year old man from Los Angeles (California, United States of America) was admitted to hospital due to abdominal pain. He referred to having no chronic underlying diseases. Ten days prior to admission he complained of malaise, low-grade fever and myalgia. Five days later, he developed progressively increasing pain in the upper-right quadrant of abdomen, accompanied with nausea.
In the emergency room he had a blood pressure of 110/75mmHg, heart rate of 110 beats per minute, and axillary temperature of 37.5° C. Physical examination revealed bilateral exudative tonsillitis and enlargement of submandibular lymph nodes. He had tenderness in the upper right quadrant of the abdomen, with a palpable liver 2 centimetres under the costal margin. Murphy sign was positive.
Blood analysis showed an increase in aspartate aminotransferase (AST) and alanine aminotransferase (ALT) (125/199 IU/L respectively), total bilirubin of 4.4mg/dL. Renal function was normal. C-reactive protein was within the normal range (1.8mg/dL) and white cell blood count was 9,200 cells per microlitre with 43% lymphocytes.
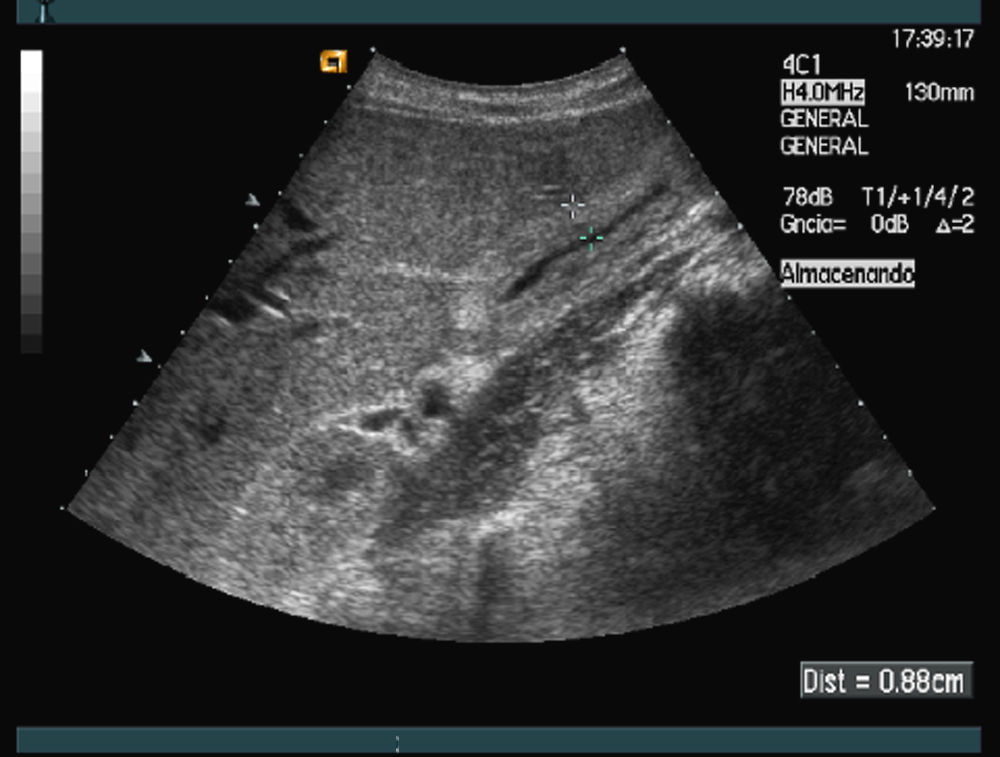
An abdominal ultrasound showed thickening of the gallbladder wall with echogenic material inside and positive echographic Murphy sign. There was some perivesicular fluid, and all these findings were compatible with the diagnosis of acute cholecystitis (Fig. 1).
Heterophile antibodies against Epstein-Barr virus were positive. With the diagnosis of infectious mononucleosis and acute cholecystitis, a conservative management with intravenous fluids, intravenous ceftriaxone, analgesia and avoiding food intake was decided. The patient remained symptomatic for the following 48hours, with pain in the upper-right quadrant of the abdomen and blood analysis revealed an increase in the serum transaminase levels (AST 235 IU/L, ALT 287 IU/L), bilirubin (5mg/dl) and alkaline phosphatase (627 IU/L). A new abdominal ultrasound showed hepatosplenomegaly with a significant amount of intraperitoneal fluid. The wall of the gallbladder was severely thickened (1 centimetre).
Serologies confirmed the clinical diagnosis of infectious mononucleosis (IgM M antibodies against Epstein-Barr virus positive and negative IgG G antibodies). Nucleic acid testing for Epstein Barr virus in blood was positive (386 DNA copies/mL). Other serologies (hepatitis virus A, B and C) and nucleic acids testing for CMV DNA in blood were negative.
Although the patient was clinically stable, he persisted with pain in the upper-right quadrant of the abdomen and blood analysis worsened (bilirubin 7.8mg/dL, alkaline phosphatase 1,429 IU/L, gamma-glutamyl-transpeptidase 572 IU/L), as well as leucocytosis (13,000 cells/mm3) with 42% lymphocytes and 17% reactive lymphoid cells. For these reasons the antibiotic was switched to piperacillin-tazobactam and intravenous steroids (1mg/kg/day) and acyclovir (750mg/8hours) were initiated.
Twenty-four hours later the abdominal pain improved and progressive food intake was started. Ten days after admission the patient was discharged in a good clinical condition. Two weeks later, blood analysis was normal.
Acalculous cholecystitis secondary to viral infections are rare, although 11 cases have been reported in the last 3 years associated with Epstein-Barr virus primary infection1–4. This complication is a marker of more severe disease and clinical and ultrasound monitoring must be performed5,6. Most cases described are healthy young patients and infants. Interestingly, 10 out of 11 cases published were female.
The pathophysiology of this complication is controversial. One hypothesis is a direct viral invasion of the gallbladder mucosa7, while another is based on the cholestasis induced by the infection, which leads to a release of proinflammatory molecules that induce gallbladder inflammation2. Unfortunately, these theories have not been proved as none of the published cases required surgical intervention. All published cases had a very good outcome without surgery. However, if ultrasound alterations persist, or there are signs of gallbladder perforation, cholecystectomy should be performed.
The use of steroids in patients with infectious mononucleosis is also controversial. There is a formal indication in cases of upper airway obstruction or aplastic anaemia and should be evaluated in cases of severe liver dysfunction8,9. In the reported cases, there is no mention of the use of steroids for the treatment of this complication. The use of acyclovir has been show to inhibit oropharyngeal Epstein-Barr virus replication, although with no clinical benefits of its use8. However, although there is no available data from randomised studies, data from review of case series and case reports suggest that acyclovir should be considered as an adjunctive therapy to steroids in the treatment of severe mononucleosis10. The rapid improvement of symptoms of our patient suggests that the effect of intravenous steroids probably had more weight than intravenous acyclovir in his clinical outcome.
In conclusion, acalculous cholecystitis is a possible complication of infectious mononucleosis. Most cases had good prognosis without surgery, but steroids should be considered in cases of persistence of symptoms.