Spinal anesthesia involves the administration of a dose of local anesthesia into the intrathecal space of the lumbar spine, using spinal needles with varying characteristics and design. When completing the administration of spinal anesthesia, you may check the volume of fluid remaining inside the spinal needle.
ObjectiveTo measure and compare the volume of residual fluid following the administration of spinal anesthesia using three different brands of 27 gauge spinal needles.
MethodsThis is an observational analytical cross-section trial for which tree types of 27 gauge commercial needles were selected: BD Whitacre pencil point, Spinocan Quincke sharp point, and Disposable spinal needle. Following the administration of spinal anesthesia, the same operator, without detaching the syringe from the needle, deposited the residual volume into a collection tube so that a second operator quantifies the volume using a precision micropipette.
ResultsThe residual volume obtained from the 27G spinal needles showed a statistically significant difference in favor of the BD Whitacre needles (P<0.01), compared against Spinocan Quincke and Disposable spinal needle.
ConclusionsThe BD Whitacre pencil point proved to lodge less residual volume following spinal anesthesia. No clinical implications can be made from this finding and new studies are required to ratify these results.
La anestesia raquídea consiste en la aplicación de una dosis de anestésico local en el espacio intratecal de la columna lumbar, por medio de agujas espinales cuyas características varían en calibre como en diseño. Al terminar la aplicación de una anestesia raquídea se puede comprobar un volumen remanente de líquido al interior de la aguja espinal.
ObjetivoMedir y comparar del volumen remanente de líquido posterior a la aplicación de anestesia raquídea en tres marcas comerciales de agujas espinales de calibre 27.
MétodosEste es un estudio observacional analítico de corte transversal, se escogieron tres tipos comerciales de agujas calibre 27: BD Whitacre punta de lápiz, Spinocan Quinke punta cortante y Disposable spinal needle. Posterior a la aplicación de una anestesia raquídea, el mismo operador sin desconectar la jeringa de la aguja, depositó el volumen residual en un tubo de recolección, para que un segundo operador con una micropipeta de precisión cuantificara el volumen.
ResultadosEl volumen residual obtenido de la agujas espinales 27G demostró tener una diferencia estadísticamente significativa a favor de las agujas BD Whitacre (P<0.01), comparadas con agujas Spinocan Quinke y Disposable spinal needle.
ConclusionesSe comprobó que las agujas BD Whitacre pencil point alojan menor volumen residual posterior a una anestesia espinal. No se pueden hacer implicaciones clínicas derivadas de este hallazgo. Son necesarios nuevos estudios para corroborar estos resultados.
Spinal anesthesia is the anesthetic technique of choice in a range of surgical procedures: general surgery, ObGy, orthopedics and urology. It is based on the injection of one dose of local anesthetic into the subarachnoid space at the level of the lumbar spine. The spinal needles used vary in their design and gauge.
Following the administration of spinal anesthesia, a residual volume may be observed in the needle. This volume may vary depending on the needle manufacturer. There are no publications researching how significant this volume is.
An inadequate dose selection is a cause for failed spinal anesthesia and according to the literature ranges between 1 and 17% of the spinal anesthesia.
The purpose of this post-interventional trial was to measure the residual volume contained inside the chamber of three 27 gauge spinal needles from three different manufacturers and to assess whether there are any statistically significant differences.
MethodsAn observational, analytical, cross-section, non-randomized trial was designed, in which spinal needles used for the administration of spinal anesthesia were successively recruited.
Three brands of 27 gauge needles available in the Colombian market were collected:
- a.
BD Whitacre pencil point spinal needle (BD Medical Franklin Lakes, NJ. USA), 27 GA 0.40×90mm.
- b.
Spinocan Quinke sharp tip (Braun Medical Inc., Bethlehem, PA, USA) 27 GA 0. 42×88mm.
- c.
Disposable spinal needle (Dr.J Tianjin Hanaco Medical Co. Tianjin, China). 27 GA 0.38×90mm.
To measure the residual volume, an Automatic Micropipette of 100 to 1000lU was used, (volume measurement capacity 0.1μl up to 10ml) EASY40+ LABBOX.
A convenience sample of 13 measurements per manufacturer of spinal needles was selected, for a total of 39 samples. For the administration of spinal anesthesia, hypodermic disposable 3ml/cc needles were used, connected through a thread to the spinal needles.
The specimens that during their use showed evidence of failure for the administration of the drug, any defective specimens or with defects or deformities after threading the syringe to the spinal needle, were all excluded.
The involvement of anesthesiologists was required. The anesthesiologist who administered the spinal anesthesia was informed about the intention to measure the residual volume so that after preparing the dose, without disconnecting the syringe from the spinal needle, the residual volume inside the needle shall be placed in a plastic measuring tube.
The volume of the dose administered in the anesthesia, and the number of barbotages was not taken into account.
The second independent and trained anesthesiologist measured the residual volume in each needle with the micropipette (precision volumes from 0.1μl to 10ml).
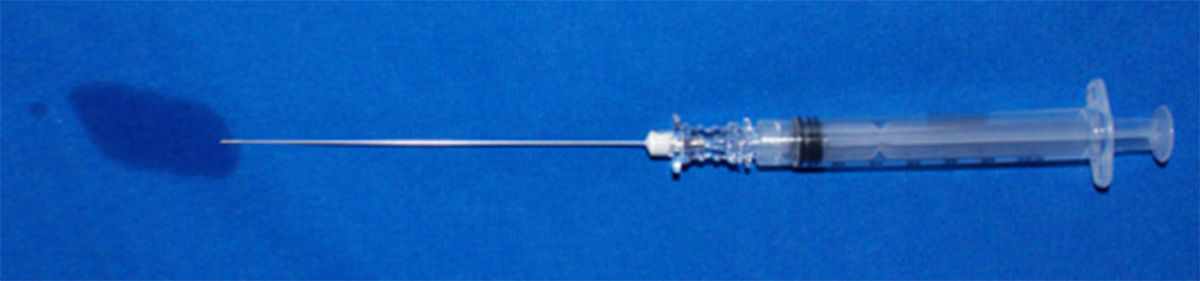
The process was repeated with the 39 samples collected. In order to take the measurements and analyze them, the spinal needles were classified in accordance with the manufacturer and the residual volumes identified inside (Fig. 1).
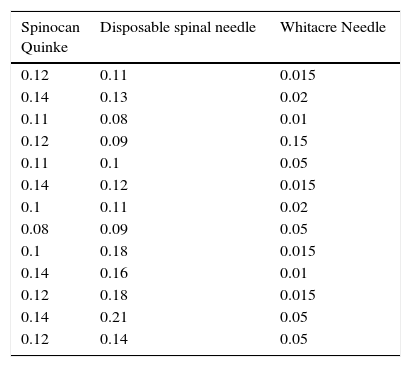
ResultsThis observational trial did not require patient intervention. Thirteen non-randomized samples were taken per each type of 27G spinal needle (BD Whitacre, Spinocan Quinke and Disposable spinal needle) for a total of thirty-nine (39) samples (Table 1).
Measurement of residual volume in the spinal needles chamber #27.
| Spinocan Quinke | Disposable spinal needle | Whitacre Needle |
|---|---|---|
| 0.12 | 0.11 | 0.015 |
| 0.14 | 0.13 | 0.02 |
| 0.11 | 0.08 | 0.01 |
| 0.12 | 0.09 | 0.15 |
| 0.11 | 0.1 | 0.05 |
| 0.14 | 0.12 | 0.015 |
| 0.1 | 0.11 | 0.02 |
| 0.08 | 0.09 | 0.05 |
| 0.1 | 0.18 | 0.015 |
| 0.14 | 0.16 | 0.01 |
| 0.12 | 0.18 | 0.015 |
| 0.14 | 0.21 | 0.05 |
| 0.12 | 0.14 | 0.05 |
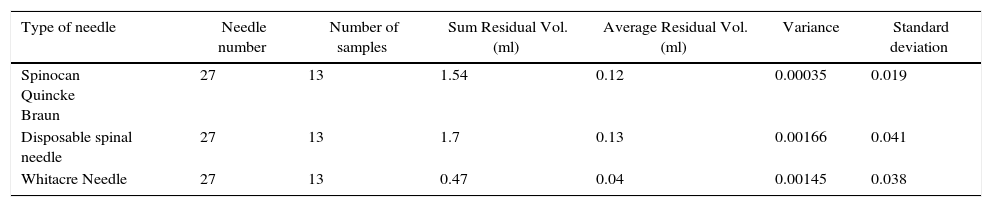
A statistical analysis was completed using the t-test function, Microsoft Excel data analysis tool (Table 2).
Statistical analysis of the samples.
| Type of needle | Needle number | Number of samples | Sum Residual Vol. (ml) | Average Residual Vol. (ml) | Variance | Standard deviation |
|---|---|---|---|---|---|---|
| Spinocan Quincke Braun | 27 | 13 | 1.54 | 0.12 | 0.00035 | 0.019 |
| Disposable spinal needle | 27 | 13 | 1.7 | 0.13 | 0.00166 | 0.041 |
| Whitacre Needle | 27 | 13 | 0.47 | 0.04 | 0.00145 | 0.038 |
The residual volume obtained from the Whitacre 27 G pencil tip needles (average residual volume of 0.04ml), manufactured in the United States, showed a statistically significant difference as compared against the residual volume in the Disposable spinal needle (average residual volume 0.13ml) manufactured in China and Spinocan Quinke manufactured by Braun in the United States (average residual volume 0.12ml), with a P value of less than α=0.01.
Although the length of the Whitacre needle is 90mm, 2mm longer than the Quinke 88mm needle, there was not a favorable difference for Quinke. The Whitacre needle has an inner diameter of 0.40mm, 0.02mm larger than the Disposable spinal needle 0.38mm needle, but showed no advantage either.
DiscussionSpinal anesthesia is used to perform different surgical procedures in general surgery, ObGy, orthopedics, and urology.1–3 In Colombia we have different brands of 27 G spinal needles. This is the most common smaller gauge found. This paper results from the observation of a residual volume found after spinal anesthesia in those spinal needles after use. The purpose of the trial was to determine whether there are any volume differences, regardless of the technical data sheet of each needle.
The dose of local anesthetic, the use of opioids, and barbotage were not considered in each sample. Therefore, he constitution of the volume collected may not be implied. To do so, high-efficient liquid chromatography techniques are required, but these are beyond the scope of this study.4 The collection and measurement techniques in each sample taken were standardized. A significant difference in favor of the BD Whitacre pencil tip needle was shown. These are the needles with the smallest residual volume at the end of the administration of anesthesia.
There is a trend to use low volumes in short procedures or in some patients in whom peripheral vasodilatation could compromise the cardiac output, with negative effects on vital organs.5–8 One of the causes of failed spinal anesthesia is a mistake in selecting the anesthetic dose.9,10 The use of smaller residual volume needles could be a determining factor when selecting a low dose technique.
This trial has some weaknesses worth mentioning: the number of cases recruited per each group, the lack of previous studies to determine the sample size, the percentage of residual volume versus the general volume administered, and the measured composition of the residual volume measured.
ConclusionsThe study showed that the BD Whitacre pencil point needles retain less residual volume following spinal anesthesia. No clinical implications may be derived from this finding. New studies are needed to ratify these results.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that they have followed the protocols of their work center on the publication of patient data.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
FundingThe authors did not receive sponsorship to undertake this article.
Conflicts of interestThe authors have no disclosures to make.
Please cite this article as: Luna CA, Tulcán-Toro R, Romero F, Luna MF. Medición del volumen residual en las agujas espinales tras anestesia raquídea. Rev Colomb Anestesiol. 2017;45:12–15.