Radiotherapy is part of the standard therapeutic management of women with breast cancer. However, at high doses (>40Gy), it can lead to the development of certain tumors, such as angiosarcoma.1,2 The incidence of this cancer is low (0.07%)2,3; however, increased patient survival and indication of breast-conserving surgery have resulted in its growing frequency. The predisposition of patients to develop radiation-induced tumors multiplies in certain hereditary syndromes, particularly in Li-Fraumeni syndrome (LFS).4,5 The characteristic TP53 mutation of this syndrome causes genetic instability due to inappropriate recombination of DNA and a greater susceptibility to ionizing radiation.5,6
Radiation-induced angiosarcoma (RIA) has a poor prognosis, with an estimated 5-year overall survival (OS) of 43%.7 Due to the low frequency of RIA, evidence is limited. Nonetheless, curative treatment is only possible through surgical resection with wide margins, making early diagnosis essential.
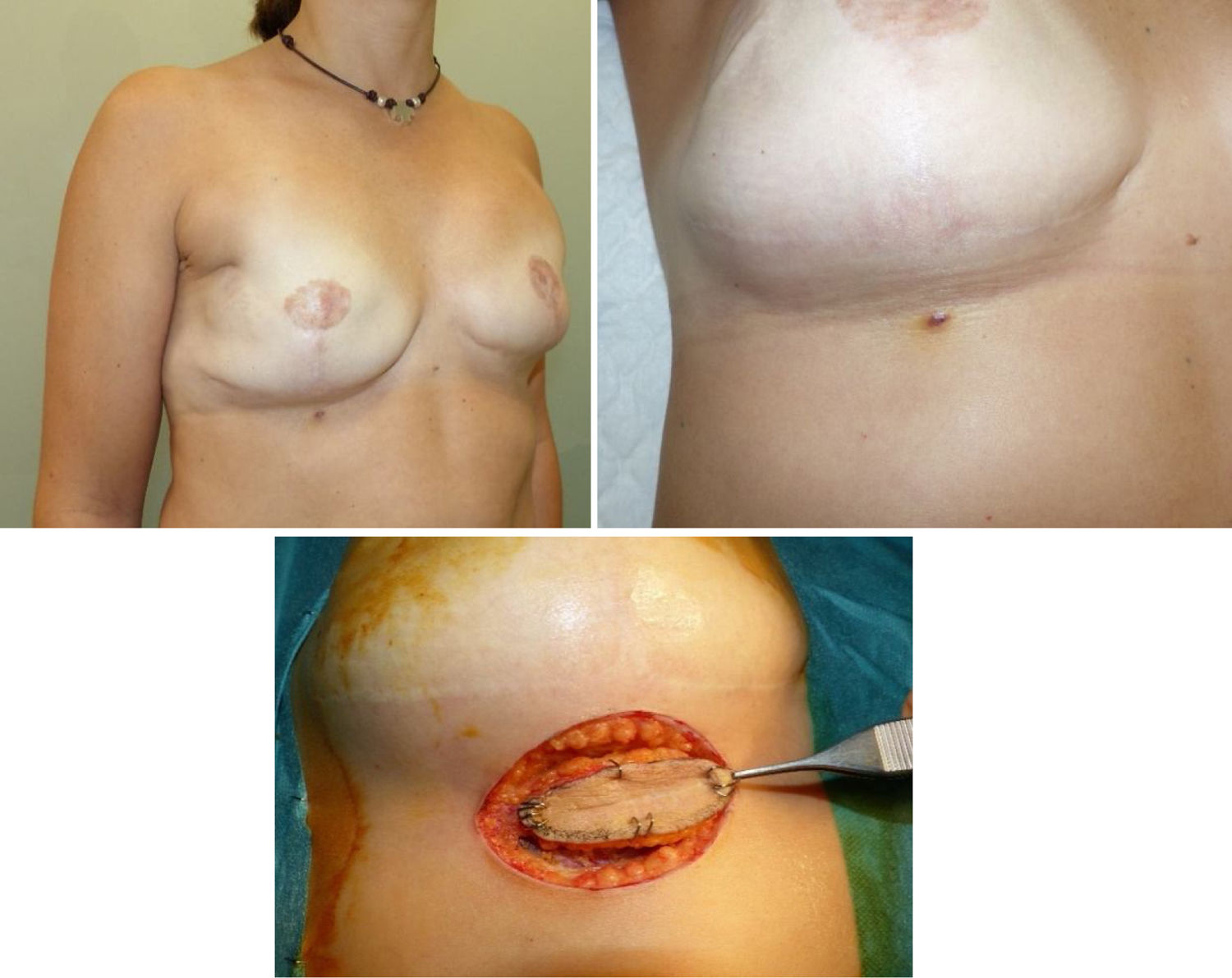
We present the case of a 37-year-old woman who consulted for a palpable nodule in the right breast. Her mother had died from metastatic breast cancer at the age of 36, and her sister was diagnosed with breast cancer at the age of 35. Mammography, magnetic resonance imaging and core-needle biopsy confirmed the diagnosis of bilateral invasive ductal carcinoma (IDC) (grade III, luminal B, HER2 positive). Skin and nipple-sparing mastectomy was conducted with bilateral sentinel lymph node biopsy and immediate reconstruction. The definitive pathology study demonstrated a 2-cm IDC in the right breast (pT2N0) and an 8-mm IDC in the left breast (pT1bN0). The treatment was completed with chemotherapy (carboplatin, docetaxel and trastuzumab), then hormone therapy (tamoxifen and Zoladex®). Due to the family history and the early diagnosis of bilateral breast cancer, a genetic study was requested, which demonstrated the mutation of TP53, compatible with LFS. Although it was not indicated, the patient requested radiotherapy and, after a third opinion, underwent radiation of the thoracic wall and right lymph node chains. Four years later, the patient consulted for a 5-mm wine-red bump with a shiny halo in the right inframammary fold (Fig. 1), whose surgical biopsy demonstrated an atypical vascular lesion suggestive of RIA, with free margins.
LFS is an autosomal dominant hereditary disorder with a penetrance of 100% that is more susceptible to radiation.5 Therefore, the indication of radiotherapy in these patients is controversial, and mastectomy is the treatment of choice in breast cancer. However, unlike hereditary breast and ovarian cancer syndromes, prophylactic mastectomy is not indicated. First of all, because the estimated risk of breast cancer is lower than in patients with BRCA1 and BRCA2 mutation (22% vs 60%–80%). And second, because other neoplasms may appear in patients with LFS, and prophylactic mastectomy will not impact OS.8
Although breast RIA is more frequent in conservative surgery, this tumor can appear in the radiated chest wall, as in the case of our patient. The presumptive diagnosis is clinical, and in the initial stage RIA can present as a hematoma, eczematous rash, atypical telangiectasia or one or multiple elevated reddish-purple nodules. Therefore, a lesion with these characteristics in the field of radiation requires a biopsy to confirm the diagnosis.
The treatment of RIA is radical surgery with free margins. Obtaining negative surgical margins is more important than the type of surgery. In women with previous lumpectomy, a mastectomy will usually be performed; however, a second breast-conserving surgery is also possible. There is no consensus on the appropriate resection margin, but distances less than 1cm are associated with early local recurrence, so 2–3cm margins are recommended. Lymph node staging is not indicated, as these tumors tend to metastasize through the blood stream and the incidence of lymph node involvement is low.9 Axillary lymphadenectomy is performed only in patients with histological involvement of the axilla, with no distant metastatic disease.
The role of chemotherapy is not clear,2,9 but case series report responses of 20%–60% to taxanes and anthracyclines in locally advanced inoperable or metastatic disease. Other therapeutic options are monoclonal antibodies, including bevacizumab, sorafenib or pazopanib. However, the results of various clinical trials are contradictory. Although pazopanib therapy seems promising, current clinical guidelines10 only accept its palliative use.
Three conclusions can be drawn from this review. First, the indication for radiotherapy should be limited in patients with LFS as the probability of a radiation-induced tumor is very high (48%). Second, RIA can appear after a mastectomy and, although they are rare, a suspicious lesion in the field of radiation should always be biopsied. Lastly, surgery with wide margins is the curative treatment of this disease, for which early diagnosis is essential.
Please cite this article as: García Novoa A, Acea Nebril B, Bouzón Alejandro A, Cereijo Garea C, Antolín Novoa S. Angiosarcoma radioinducido de mama en paciente con síndrome de Li-Fraumeni. Cir Esp. 2019;97:114–116.