Mastocytosis is a genodermatosis of unknown etiology, considered among the rare or infrequent. It is characterized by local or systemic accumulation of mast cells, originating mainly cutaneous manifestations. Bone manifestations are part of the clinical picture of this rare condition, although their discovery is usually rare. In this paper, the case of a 7-year-old diagnosed with cutaneous mastocytosis who presents skeletal manifestations of this disease occurs, which we believe is of importance for understanding the medical community.
La mastocitosis es una genodermatosis, de etiología desconocida, considerada entre las enfermedades raras o poco frecuentes. Se caracteriza por acumulación local o sistémica de células cebadas, originando principalmente manifestaciones cutáneas. Las manifestaciones óseas forman parte del cuadro clínico de esta rara afección, aunque su hallazgo suele ser infrecuente. En este trabajo se presenta el caso de un paciente de 7 años de edad, diagnosticado de mastocitosis cutánea, quien presenta manifestaciones óseas de esta enfermedad, cuyo conocimiento, consideramos, es de importancia para esta enfermedad.
Cutaneous mastocytosis (CM) is described as a genodermatosis of unknown etiology, mentioned for the first time in 1869 by Nettleship and Tay, but it was not until 1949 when the systemic affectation of CM was demonstrated by Ellis.1–3
Due to its low incidence, this disease is included into the group of rare or infrequent diseases. An incidence of around 2 cases per 300,000 patients per year is reported. Usually, its onset is described around the birth or during childhood and its relationship with processes of hypersensitivity and chronic or neoplastic diseases is known.4–6
Studies on this condition report that the predominant clinical manifestations are cutaneous, which are described as macules, papules and brownish hyperpigmented nodules, single or multiple, fundamentally affecting the trunk, the back, and the proximal portion of the limbs, respecting the face and the distal portion of the limbs; these lesions can be accompanied by pruritus of variable intensity that may lead to insomnia, affecting the sleep of the patients and causing extreme tiredness, which considerably diminishes the perception of health-related quality of life (HRQOL) of the patients who suffer from it.7–9
The release of immunological mediators together with the organ infiltration by mast cells are reported as possible causes of appearance of the systemic manifestations of the disease, among which are described, with higher incidence and prevalence, the presence of anorexia, asthenia, diarrhea, dyspepsia and osteomyoarticular disorders.4–6
Among the manifestations of the osteomyoarticular system are reported arthralgias, myalgias, muscle cramps and monoarthritis or oligoarthritis affecting mainly the medium and large-sized joints, causing bone erosions in a high percentage of cases of CM. Other bone alterations described are the presence of sclerosis and osteoporosis, which along with the cutaneous manifestations, further compromise the patient's perception of HRQOL.7–9
Although it has been suggested that the cutaneous lesions and the disease itself may regress spontaneously, studies carried out report that their prognosis is variable and it depends on several factors such as age, frequency and number of cutaneous eruptions, as well as on the scope, magnitude and severity of the bone lesions, which play a key role in the evolution of the CMs.6–8
That is why, taking into account that CMs are infrequent diseases, that the osseous manifestations during the course of this disease cause a decrease in the perception of the quality of life of the patients who suffer from it and condition its prognosis, and the lack of reports of similar cases in Ecuador, we decided to carry out this work in order to recognize the osseous manifestations that occur in the course of the CM, which will be useful as a tool for the diagnosis of the disease.
Case presentationA 7-year-old male patient with mestizo skin color, antecedents of good personal health and familial pathological history of a paternal grandfather with dermatological lesions in the form of hyperpigmented macules. The patient is brought to the Dermatology outpatient clinic of the Andino Chimborazo Hospital by his mother, who reports that the child has had hyperpigmented skin lesions of 6 years of evolution, for which he has received multiple treatments without evidence of improvement. In addition, she points out that these lesions were accompanied by pruritus of variable intensity which was exacerbated by extreme temperature changes and local pressure and, especially at night, making the child's sleep impossible; these lesions respect the palms, soles and mucous membranes. She also reports that the child, since about 2 years ago, has complained of fatigue, joint pain in knees, hips and ankles, which sometimes was accompanied by increased volume of both knees; as well as the presence of occasional muscle cramps and contractures in both legs. Finally, she states that the child exhibited, occasionally, facial flushing and irritability, which had caused him behavioral problems at school. The diagnosis of CM is made and interconsultation to the Rheumatology department is decided because of the presence of osteomyoarticular manifestations.
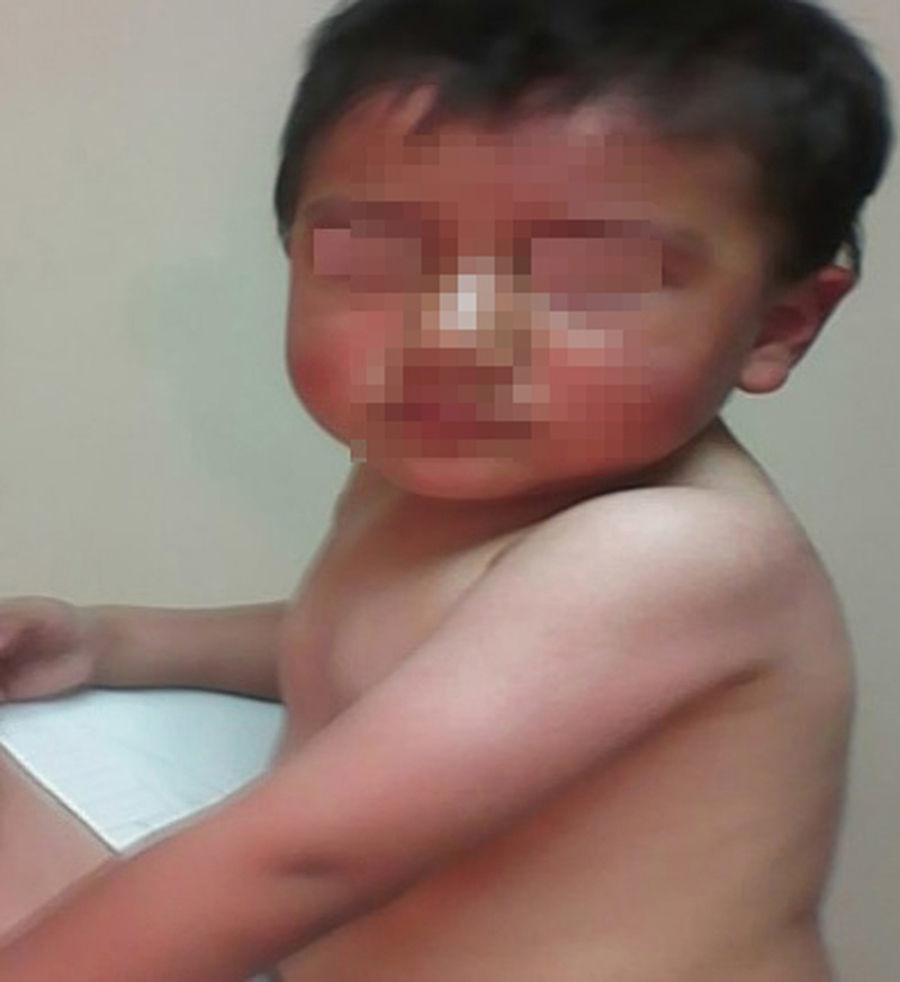
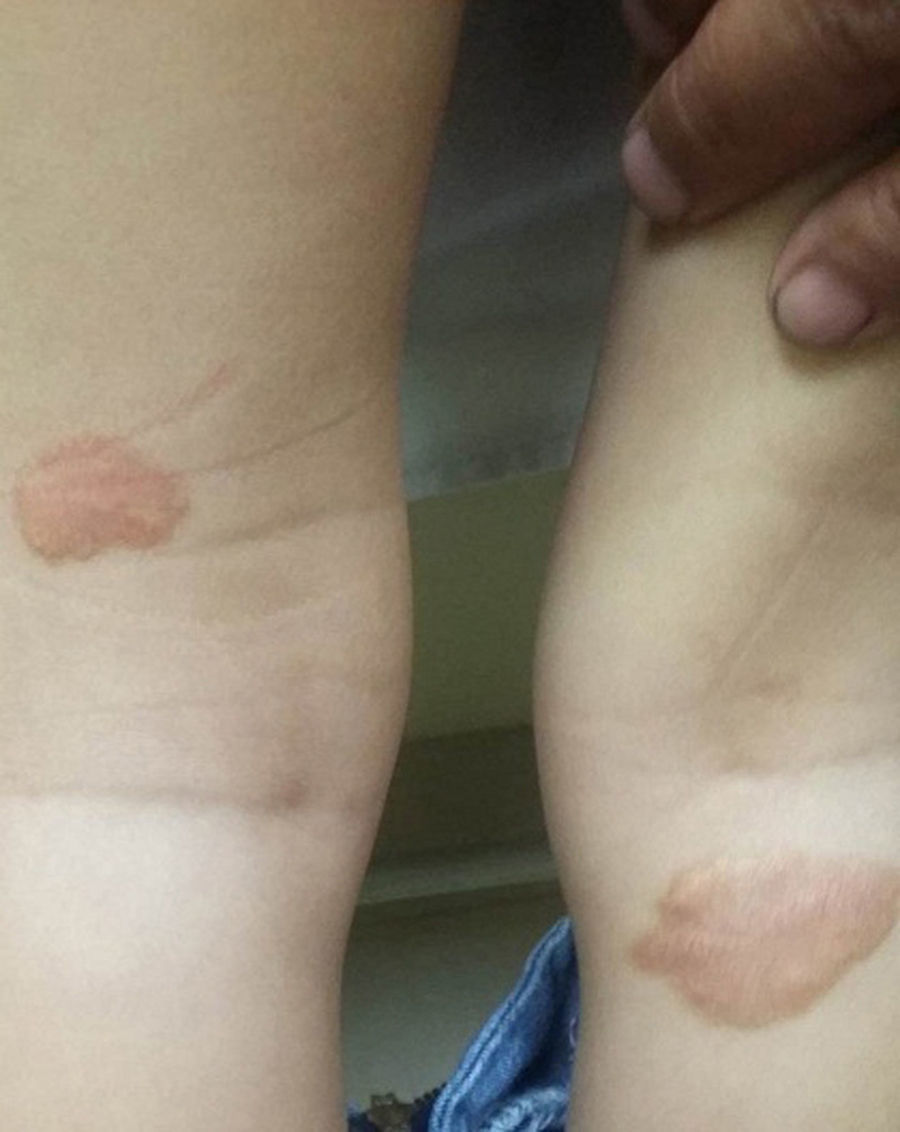
When assessed by the specialty of Rheumatology, on the physical examination was found pain on movement of both knees, observing bilateral femoral quadriceps hypotrophy, without verifying arthritis at this time. On the physical examination stands out the presence of hyperpigmented tumoral lesions of different sizes, located in the upper trunk, the back and the upper limbs; and xeroderma in the arms and the upper trunk. Negative dermographism (Figs. 1 and 2).
In order to confirm the diagnostic suspicion and to know the patient's status, as well as to rule out chronic and neoplastic conditions that might be related with this disease, a series of complementary tests were carried out, that only showed, as a significant data, eosinophilia of 0.098mmol/l; the rest of the laboratory tests were within normal parameters.
The imaging tests showed acetabular sclerosis at the level of the left hip, sclerosis in both femoral condyles of the right knee, without the presence of erosions, and osteopenia in both hips, finding a T score of −1.8 in the left hip and −2.1 in the right hip; the bone mineral density in the vertebral column was normal showing T score values of −0.2. The ultrasound of both knees did not show other alterations.
The histopathological study carried out reported elements that confirm the diagnosis of CM, informing, after staining with giemsa: fragments of skin covered by squamous epithelium, mature and thinned; dermis constituted by proliferation of cells with aspect of mast cells with round, small and medium sized nuclei, without atypia, wide granular acidophilic cytoplasm, scattered and arranged in a solid pattern accompanied by some eosinophils, with the presence of congestive blood vessels.
The patient has shown a satisfactory evolution despite the short time that has been receiving the therapeutic scheme that includes, from the dermatological point of view, treatment with mast cell inhibitors, as well as symptomatic treatment. The specialty of Rheumatology proceeded to treat symptomatically the affections that were found with analgesics and emphasizes on the use of nutritional supplements to correct the deficit in bone mineral density that he presents, being followed up periodically by both specialties jointly, maintaining a strict monitoring on possible symptoms and signs that can suggest the presence of an associated tumoral or rheumatic disease.
DiscussionDue to the non-specificity of the symptoms and signs, as well as to its initial indolent course, CM is considered as an enigmatic disease of difficult diagnosis. In this case, the affected patient belongs to the masculine gender, which is reported with a higher frequency in the reviewed literature, while acknowledging that the disease can affect both sexes.6,10
Although there is a predominance of cutaneous affectation in these patients, involvement of other organ systems of the human body is also reported, for example Blanco, in his study published in 2013, concludes that 99% of the CMs are cutaneous, while only 1% corresponds to systemic forms, usually accompanied by cutaneous affectation, other authors agree with this proposal.6,7
It is described a tendency to hemorrhages, such as ecchymosis, hematemesis and melena; related with the increase of heparin in blood, but not demonstrable in this patient; the presence of anemia, leukopenia and thrombocytopenia is also reported and, although less frequent, and mast cell leukemia can occur. Manifestations that compromise the prognosis and the evolution of the patient.6–8,10–12
Among the systems that are described as being affected in CM stands out the osteomyoarticular system. In the case presented here, there were arthralgias, myalgias, muscle contractures, and is described the antecedent of mono and oligoarthritis, which was not confirmed on the physical examination. Other studies also report similar joint involvement.6–8,10–15 These symptoms and signs can be explained by the release of proinflammatory substances due to the cutaneous affectation predominant in the disease, with hyperreactivity of macrophages and mast cells as the cells responsible for the production of these proinflammatory cytokines, which upon entering the bloodstream would trigger the whole immunological process, with the subsequent appearance of the inflammatory signs.8,10,14,16
The results of the different complementary exams showed a marked eosinophilia, which coincides with other reports in the literature, where its presence is mentioned in 40% of cases of CM, but it must also be added in this case that we are in a underdeveloped country, where despite the great advances that have been achieved in the matter of health promotion and prevention, there are still high indexes of parasitosis that could have an influence on the eosinophilia that this patient shows, although we highlight that the rest of the exams to detect parasitosis were negative.6,8,11–13
The imaging studies showed the highest significance evidencing, firstly, the presence of osteopenia in both hips and, secondly, the presence of sclerosis in both right femoral condyles and in the left hip. These findings evidence, in addition to the systemic involvement of the CM, the presence of a persistent or maintained inflammatory process despite not having been corroborated on the physical examination. Sclerosis should not exist in the case of patients of this age, since it appears as one of the signs that show persistent articular inflammatory process which induces degenerative changes and, at the same time, are precursors of the appearance of bone erosions, which has been reported by other authors without having been observed in this case.7,12,13,17
Osteopenia at this age is not frequent and is usually secondary to another affection, constituting a warning sign of an inadequate mechanism of bone remodeling; in this case, an hypothesis for its appearance is the presence of the inflammatory picture, persistently or intermittently, which negatively affects the bone remodeling and, therefore, the bone mineral density.12,18,19
The treatment, in general, and from the rheumatic point of view in this case, is symptomatic and does not alter the course of the disease. It is addressed to maintain the patient's HRQOL, avoiding the action of agents that can trigger the release of chemical mediators by the macrophages and mast cells. The prevention of their effects on the tissues constitutes the key to treatment, with the prescription of inhibitors of tyrosine kinases and other molecules targeted at the biochemical mechanisms of the activated signal transduction pathways of the mast cell. Analgesics and anti-inflammatories are used if an articular inflammatory process is confirmed; emphasis is made on doing exercises that help maintaining an adequate muscle tone and trophism in order to prevent muscle contractures and reduce the joint microtraumas; there is also an insistence on a proper nutritional intake to reverse the osteopenia presented by the patient and avoid its evolution toward osteoporosis.10–12,16,20
As it can be seen, despite being an infrequent disease, the clinical manifestations of CM can go beyond the cutaneous affectation, appearing involvement of other organ systems that not only decrease the perception of HRQOL, but can affect in a significant way the evolution and prognosis of the patient, so that being acquainted with the clinical elements for its diagnosis as well as with the possible systemic affectations is of vital importance to prevent disability and achieve better indexes of quality of life of the affected patients.
ConclusionsArthralgias, arthritis, muscle contractures and osteoporosis are the osteomyoarticular manifestations that affect the patients with CM, and therefore it becomes necessary their identification and treatment in order to minimize the early joint, bone and muscle damage that can be caused by this disease.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that they have followed the protocols of their work center on the publication of patient data.
Right to privacy and informed consentThe authors have obtained the written informed consent of the patients or subjects mentioned in the article. The corresponding author is in possession of this document.
Conflict of interestThe authors declare they do not have any conflict of interest.
Please cite this article as: Solis Cartas U, Valdés González JL, Hidalgo Cajo BG, Betancourt Jimbo C, Choca Alcoser E, Muñoz Balbín M. Manifestaciones óseas de la mastocitosis cutánea. Presentación de un caso. Rev Colomb Reumatol. 2016;23:266–270.