Adequate medication intake affects treatment effectiveness. The aim of this study was to establish the impact of prescription and secondary adherence to beta-blockers on medium term and long-term cardiovascular outcomes, after a first type 1 ST-elevation myocardial infarction (STEMI) episode without heart failure or left ventricular ejection fraction ≥ 40%.
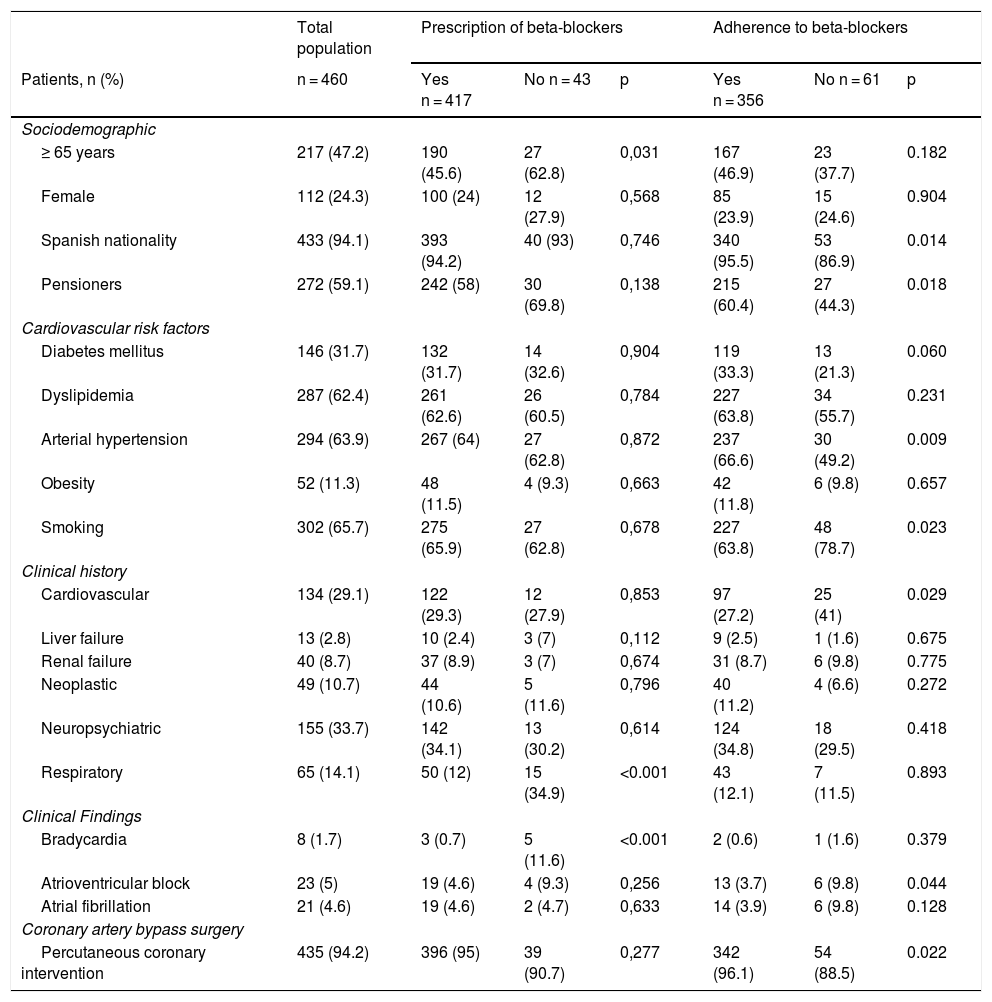
MethodsA retrospective observational study was conducted in a cohort of patients admitted from 2008 to 2013 to the University Clinical Hospital in Valencia. Competing risk analysis assessed the relationship between cardiovascular mortality or new vascular event with beta-blocker prescription and secondary adherence, defined as a proportion of days covered.
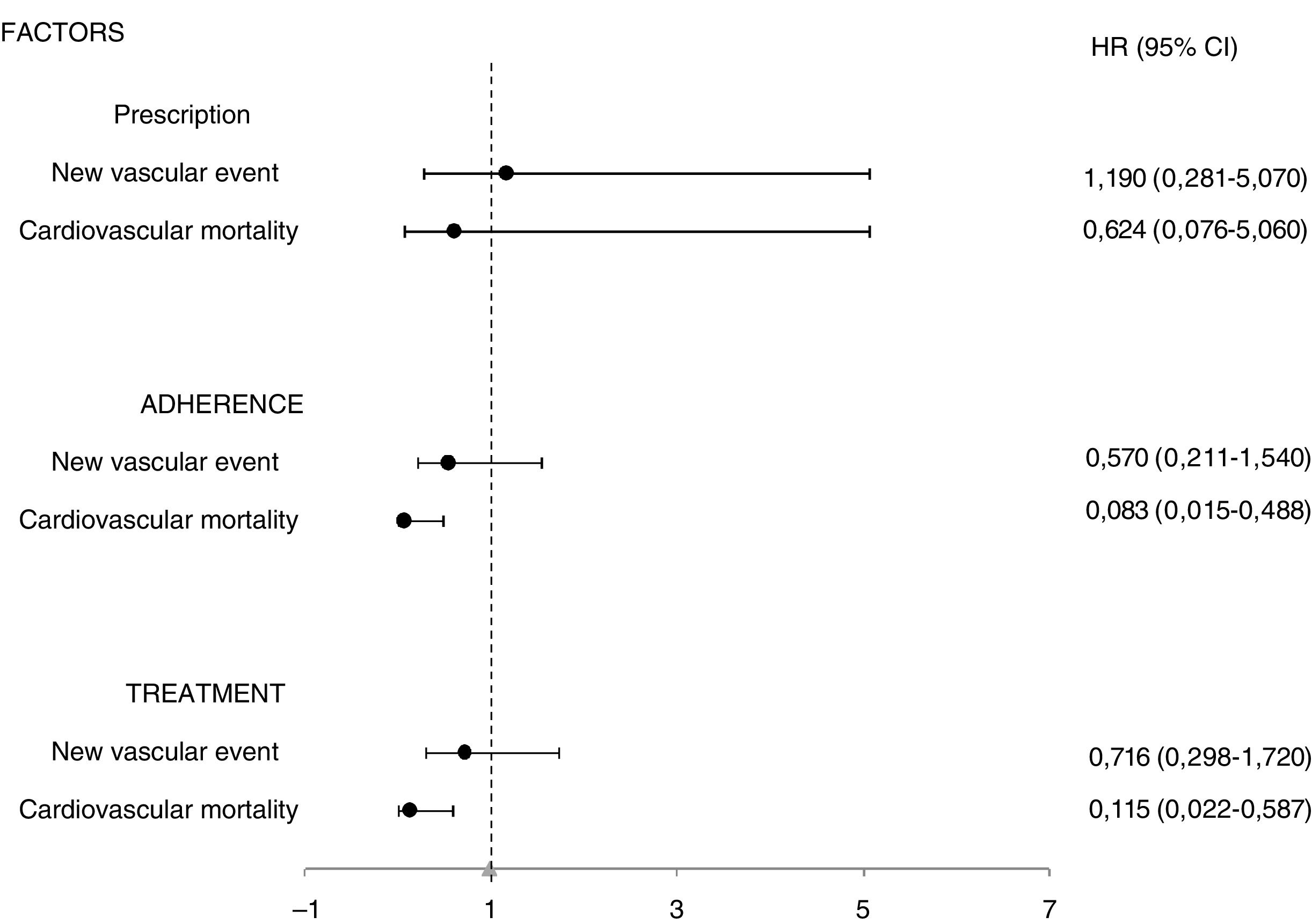
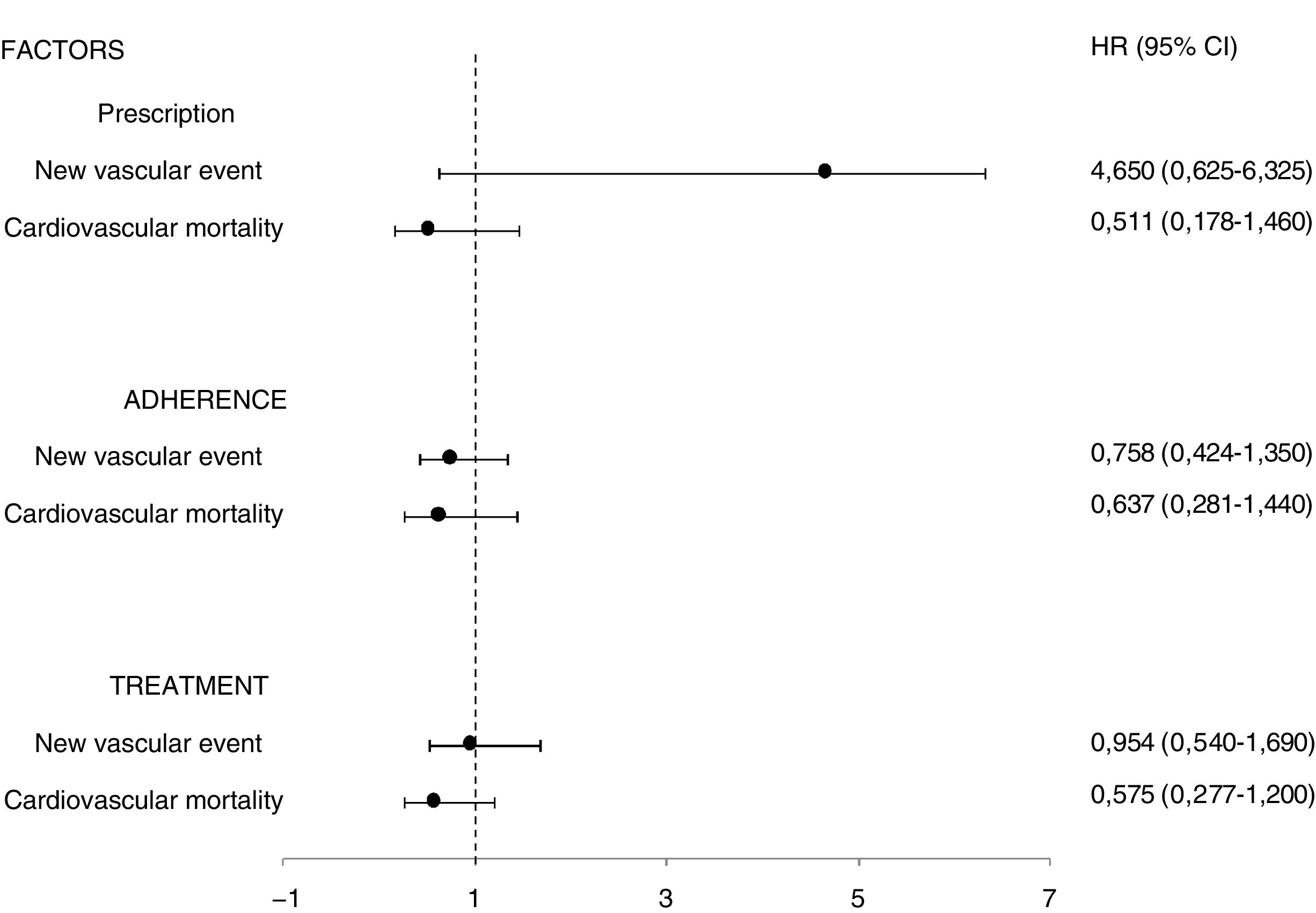
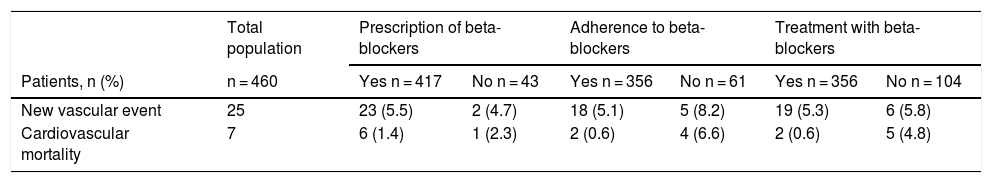
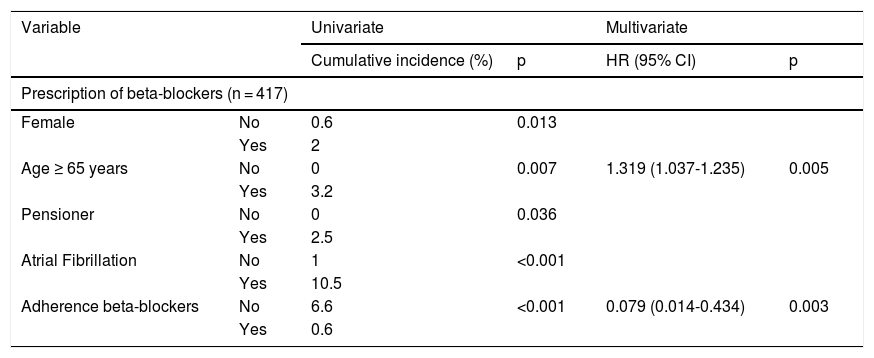
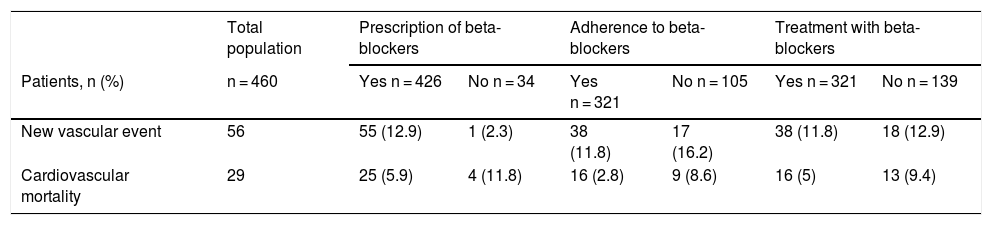
ResultsDuring after the first year following discharge, beta-blocker prescription was not significantly associated with better health outcomes in the 460 patients included. However, cardiovascular mortality was lower in adherent patients compared to non-adherent patients, at .6% vs. 6.6% (HR = .083; 95% CI, .015-.448; p = .003), and in adherent patients compared to those who did not receive the treatment due to lack of prescription or lack of adherence, with .6% vs. 4.8% (HR = .115; 95% CI, .022-.587; p = .009). These results were not observed when the complete follow-up period was analysed (median 46.7 months).
ConclusionsSecondary adherence to beta-blockers improves 1-year prognosis after STEMI with preserved left ventricular function.
La toma correcta de medicación condiciona la efectividad de un tratamiento. El objetivo del presente trabajo ha sido determinar el impacto de la prescripción y la adherencia secundaria a betabloqueantes en la morbimortalidad cardiovascular a medio y largo plazo, tras un primer episodio de infarto de miocardio con elevación del segmento ST (IAMCEST) tipo 1 sin insuficiencia cardiaca o con fracción de eyección del ventrículo izquierdo ≥ 40%.
MétodosEstudio observacional y retrospectivo en una cohorte de pacientes ingresados entre 2008 y 2013 en el Hospital Clínico Universitario de Valencia. El análisis de incidencia acumulativa estableció la relación entre la mortalidad cardiovascular o la aparición de un nuevo evento vascular con la prescripción de betabloqueantes y la adherencia secundaria, definida como proporción de días cubiertos.
ResultadosDurante el primer año tras el alta, la prescripción de betabloqueantes no influyó significativamente sobre los resultados en salud de los 460 pacientes incluidos. Sin embargo, la mortalidad cardiovascular fue menor en los pacientes adherentes respecto a los no adherentes, 0,6% frente a 6,6%, (HR = 0083; IC 95%, 0,015-0,448; p = 0,003), y en los pacientes adherentes respecto a los que no recibieron el tratamiento por ausencia de prescripción o por falta de adherencia, 0,6% frente a 4,8% (HR = 0,115; IC 95%, 0,022-0,587; p = 0,009). Estos resultados no se objetivaron cuando se analizó todo el periodo de seguimiento (mediana 46,7 meses).
ConclusionesLa adherencia secundaria a betabloqueantes mejora el pronóstico durante el primer año tras un IAMCEST con función ventricular izquierda conservada.