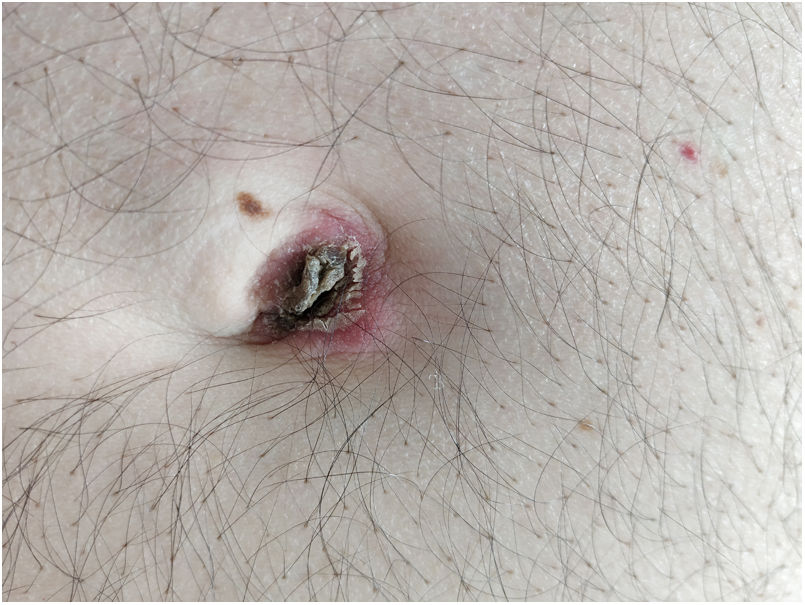
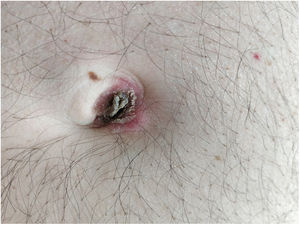
Recently, a patient with a Sister Mary Joseph nodule (SMJN), first reported in 1949, prompted us to conduct a brief clinical–epidemiological review. The patient, a 62-year-old man, presented with abdominal pain, constitutional syndrome and a nodular umbilical lesion that, months earlier, had been classified as an umbilical hernia (Fig. 1). Endoscopy revealed an unresectable gastric neoplasm. Metastatic gastric adenocarcinoma cells were identified in the nodule sample.
SMJN is a clinical sign in the form of a hard, irregular, purplish/reddish umbilical mass smaller than 5 cm. It is rarely painful (except when fissured/ulcerated, in which case it may also have serous, purulent or bloody discharge). The development of an SMJN should alert the clinician to a occult primary tumour in the abdominopelvic region and peritoneal metastases,1 though this only occurs in 1%–3% of these tumours. The manner in which metastatic spread occurs is unknown; contiguous, haematogenous and lymphatic metastatic spread (through remaining embryonic structures) have been posited.2
In this review of 68 cases with SMJN, 56% were female and the mean age was 63. The main histological type was adenocarcinoma (81%): stomach (17.7%), pancreas (17.7%), ovary (16.2%), colon (10.2%) and endometrium (8.8%), followed by haematological origin (7.4%) and, to a lesser extent, other types (sarcomas, mesotheliomas, etc) and locations (bladder, lung, etc). In 27% of cases, the site of the primary tumour was never found. Detection of an SMJN renders a prognosis bleaker, reflected in the fact that 52.5% of the patients died. The mean survival rate calculated in 40 out of the 68 cases was seven months.
Our patient had an SMJN for months which was wrongly diagnosed as an umbilical hernia. Therein lies the usefulness of reporting this case and highlighting the clinical importance of this sign. It is very easy to recognise on routine abdominal examination, with no need for sophisticated technical resources. It is associated with high morbidity and mortality rates and, if detected, radically changes the diagnostic, therapeutic and prognostic approach.
Please cite this article as: Berdugo-Hurtado F, Caballero-Mateos AM, Vidal-Vílchez B. Nódulo de la hermana María José: un signo histórico que no debemos olvidar. Gastroenterol Hepatol. 2020;43:538–539.