The Leave Your Mark (DTH) program launched recommendations for HIV screening in emergency departments (ED) when patients presented with certain conditions. It is unknown whether the profile of patients diagnosed in the ED is similar to those reported for general population in epidemiological reports.
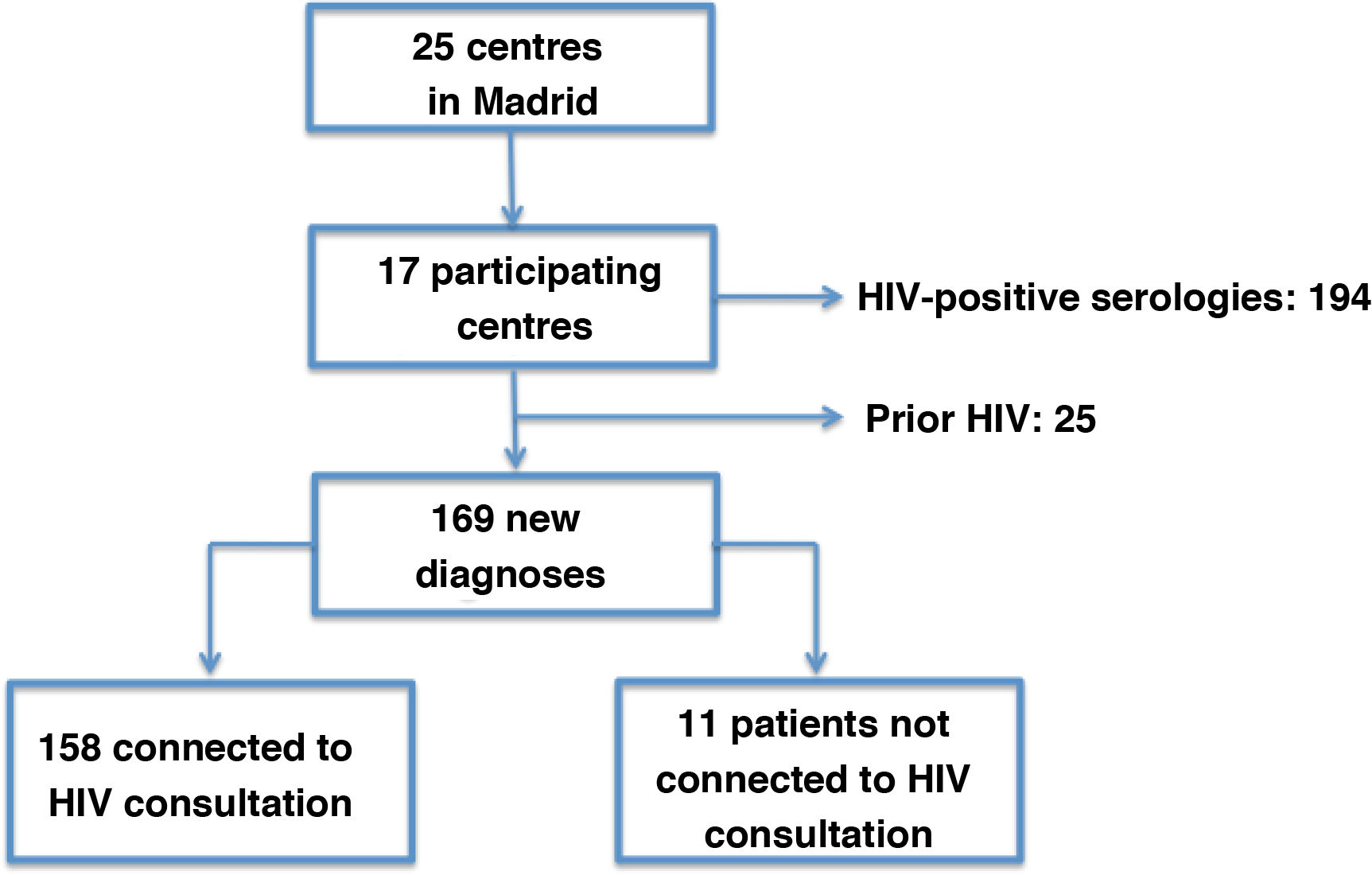
MethodsRetrospective study evaluating the characteristics of patients with new HIV diagnosed in 17 ED over a one-year period was developed. Demographic data (sex at birth, age, country of birth), sexual and risk behaviour, diagnosis in ED, number of emergency visits in previous five years, time from the ED to the specific HIV consultation, and from ED to start antiretroviral treatment were recorded. Information on the first CD4 and viral load was also collected.
ResultsA total of 169 patients were included. There were 122 (72.2%) migrants, 57 (32.5%) heterosexual, and injection drug use was the transmission route in 14 (8.3%) cases. Data reported for the general population were 49.8%, 25.7%, and 1.7%, respectively. Late diagnosis was found in 80 (47.3%) patients (reported figures by the Ministry, 48.7%). Compared to Spanish, migrant were more frequently women (13.1% vs. 6.4%), heterosexual (38.5% vs. 21.3%), and had worse immunological status [median CD4 count of 310 (IQR 132–457) vs. 444 (IQR 215−607)].
ConclusionED can play a key role in diagnosing a different patient profile that may not seek care at other healthcare levels.
El programa Deja Tu Huella (DTH) publicó unas recomendaciones para el cribado de VIH en los servicios de urgencias hospitalario (SUH) cuando los pacientes presentaban ciertas condiciones. Se desconoce si el perfil de los pacientes diagnosticados en los SUH es similar a no a los generales comunicados por las autoridades sanitarias.
MétodoEstudio retrospectivo que evalúa las características de pacientes diagnosticados de VIH en 17 SUH durante un período de un año. Se registraron datos demográficos (sexo al nacer, edad, país de nacimiento), conducta sexual y de riesgo, el diagnóstico en el SUH, el número de asistencia en urgencias en los 5 años anteriores, el tiempo desde la asistencia hasta la consulta específica de VIH y desde la atención hasta el inicio del tratamiento antirretroviral. Se recopiló información sobre el recuento de CD4 y carga viral.
ResultadosSe incluyeron 169 pacientes. Hubo 122(72,2%) pacientes migrantes, 57(32,5%) eran heterosexuales y la vía de trasmisión fue la inyección de drogas en 14(8,3%). Los datos para población general eran de 49,8%,25,7% y 1,7%, respectivamente. Presentaron un diagnóstico tardío 80(47,3%) pacientes, similar a lo comunicado previamente por el Ministerio (48,7%). Los pacientes migrantes, respecto a los nacidos en España, son con más frecuencia mujeres (13,1% vs 6,4%), heterosexuales (38,5% vs 21,3%) y tienen una peor situación inmunológica al diagnóstico [mediana de CD4 de 310 (RIC 132–457) vs 444 (RIC 215−607)].
ConclusiónLos SUH pueden ser claves para el diagnostico de un perfil distinto de paciente que puede no acudir a otro nivel asistencial.
Article
Socio de la Sociedad Española de Enfermedades Infecciosas y Microbiología Clínica

Para acceder a la revista
Es necesario que lo haga desde la zona privada de la web de la SEIMC, clique aquí
Para realizar los cursos formativos
La actividad estará abierta para socios de la SEIMC. IMPORTANTE, recuerde que requiere registro previo gratuito. Empezar aquí