Laparoscopic surgery has won out over open surgery in the treatment of morbid obesity. This has contributed to less surgical trauma for the patient and has made surgery easier for surgeons. We are currently faced with the need to improve treatment by optimizing techniques and minimizing stress and patient complications. One of the options that we have been exploring is reducing the number of surgical wounds by the development of single-port techniques.
After having tried several single-port devices and having performed a variety of techniques, including appendectomy, cholecystectomy, Hartmann's procedure, right hemicolectomy, left hemicolectomy, gastric sleeve or gastric bypass, we decided to perform laparoscopic biliopancreatic diversion without gastrectomy. The indications for this procedure are common to all bariatric surgery procedures, regardless of sex or BMI. However, we do not recommend this procedure in cases of super obesity due to the high level of technical difficulty.
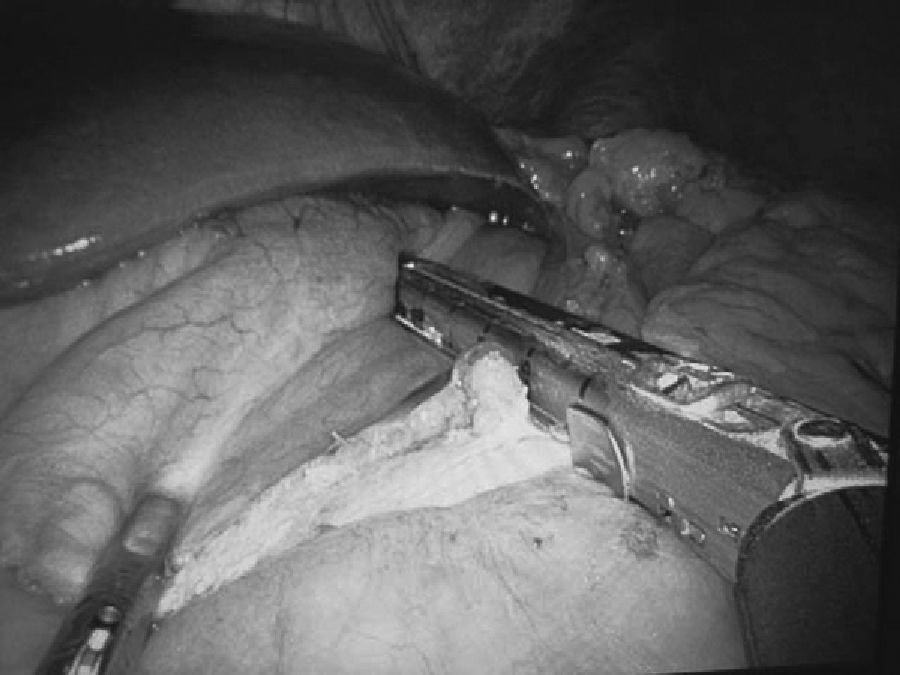
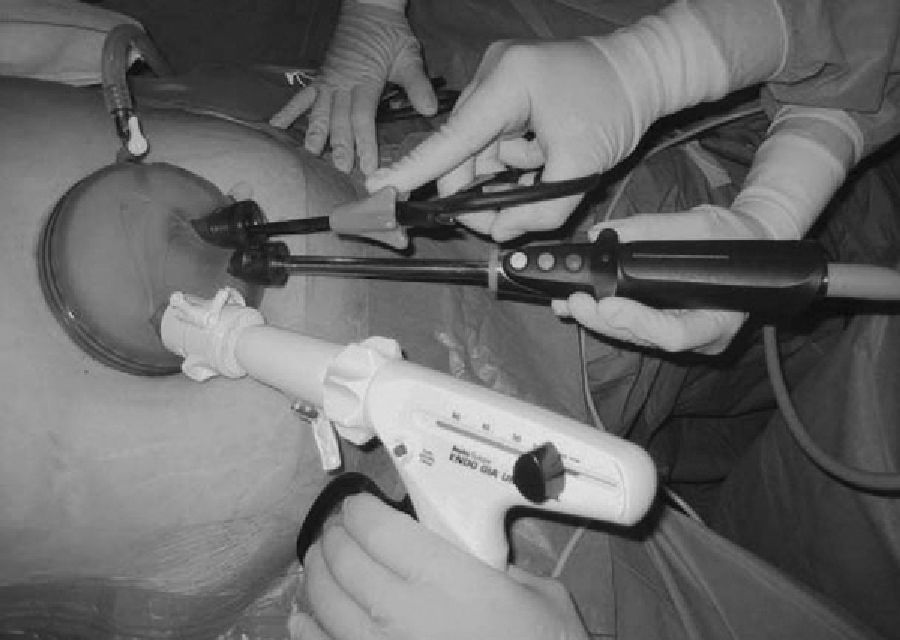
TechniqueThe patient is placed in an open-leg position with the left arm next to the body and the monitor above the right shoulder. The surgeon stands between the patient's legs while the assistant is on the patient's left side. A 3-cm abdominal incision is made around the left side of the navel. In all the procedures performed, the GelPort was used, a single-port device with a gel membrane that is flexible and allows for the use of conventional materials due to its easy triangulation. The system includes an Alexis wound protector/retractor, which is inserted first. Over the gel and before anchoring the retractor, we insert the triangulated trocars: one 5-mm trocar for the right hand, one 10-mm optical trocar (30°) and one 12-mm trocar for the left hand. The intervention is initiated in the anti-Trendelemburg position; grasping the stomach at the lesser curvature, a small window is made with the harmonic scalpel in the lesser omentum, near the gastric wall. Afterwards, the greater curvature of the stomach is dissected in order to comfortably insert the endostapler with our left hand diagonally towards the window of the lesser curvature. Three Roticulator 60-mm blue load endo-linear staplers are needed (Figs. 1 and 2). The stomach is then opened along the edge of the greater curvature, 1cm from the staple line.
The surgeon then moves to the left side of the patient, in the Trendelemburg position and, while focusing the camera on the cecum, 60cm of ileum are measured and marked with a suture. We continue measuring until a total of 3m are reached; an opening is made on the antimesenteric side, and at the initial position a 60-mm blue load endo-linear stapler is inserted in the small bowel and stomach to perform the gastrojejunal anastomosis. The intestine is sectioned and the orifice of the anastomosis is closed with another blue endo-linear stapler. We recover the ileum at the 60-cm mark with forceps as well as the distal end of the biliopancreatic limb. The GelPort is removed and the intestine is brought out in order to perform the intestinal anastomosis through the retractor of the device, which can be done either by hand or with endo-linear staples.
Once the anastomosis is finished, the mesentery is closed laparoscopically with a continuous Prolene suture.
The surgery is completed by removing the GelPort and closing the wound with continuous suture in the aponeurosis and skin staples. A Jackson-Pratt drain is always left in the left upper cuadrant.
If difficulties are encountered, the placement of a trocar in the left upper cuadrant (where the drain is later inserted) makes the intervention much easier and provides a wide range of possibilities.
DiscussionIn our opinion, laparoscopic surgery had been at a standstill, and new ideas needed to arise in order for advances to be made. The advent of devices that allow us to reduce the number of incisions to just one orifice opens a whole new set of possibilities, and we now differentiate between traditional laparoscopic surgery and single-port laparoscopic surgery.
We prefer techniques that avoid complex situations that may prolong the operation. We have tried to describe the method that currently seems to be the simplest for performing single-port laparoscopic biliopancreatic diversion. No surgeon should be criticized for using an additional trocar if this is able to reduce surgical time, improve safety and avoid complications.
Using a GelPort allows us to take advantage of the retractor in order to perform a manual extracorporeal anastomosis, which is faster and cheaper, and conventional materials can be used (without requiring articulated forceps). The umbilical location is less traumatic and more aesthetically pleasing, and we have found no access problems.
At present, we are following a new path and are not quite sure where it leads. When single-port devices were designed, their application in advanced laparoscopic surgery had not been considered. Nevertheless, some of us believe that these products are perfectly indicated in obesity surgery, especially when surgical specimens should be extracted but also due to the reduced trauma that produces a beneficial psychological effect in patients due to aesthetic advantages. Time will tell if there are any other advantages.
Please cite this article as: Resa Bienzobas J, et al. Bypass biliopancreático laparoscópico sin gastrectomía por puerto único. Cir Esp. 2013;91:202-4.