Cytoreductive surgery (CRS) and hyperthermic intraperitoneal chemotherapy (HIPEC) has become the gold standard treatment for selected peritoneal surfaces malignancies. This procedure is considered a major surgery with high non-negligible morbi-mortality rates.1 Laparoscopic approach has shown encouraging improvements versus open surgery with similar oncological results in different cancer origins such as colorectal, hepatic and early stage esophageal-gastric cancer.2
Several experienced centers3,4 have reported minimally invasive CRS+HIPEC procedures demonstrating the feasibility and safety of this approach in highly selected patients with low grade or borderline tumors associated with a limited dissemination in abdominal cavity.
We present this interesting laparoscopic approach with a new HIPEC delivery system for a limited low-grade pseudomyxoma peritonei.
A 60-year-old woman with symptoms of abdominal discomfort was studied for findings of free fluid in the abdominal cavity in a regular gynecological examination. No liver disease was present. No abnormalities were found in ultrasonography or colonoscopy. Relevant tumor markers were normal. Abdominal CT scan found a 27×22mm unspecific lesion next to the cecum with a moderate amount of free peritoneal fluid. Due to lack of a diagnosis, an exploratory laparoscopy was performed in her hospital of origin, and the patient underwent an appendectomy, being diagnosed in the posterior anatomopathological study with a low-grade perforated mucocele.
The patient was submitted to our Unit for evaluation of cytoreductive surgery plus hyperthermic intraperitoneal chemotherapy. As signs of neither significant intraabdominal dissemination nor carcinoma in the anatomopathological study were found, a laparoscopic approach was offered. Informed consent was signed.
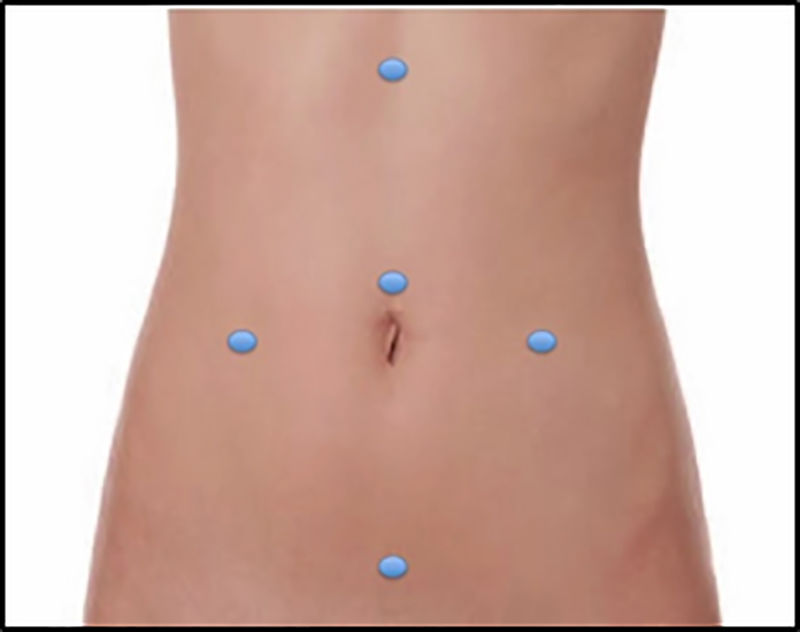
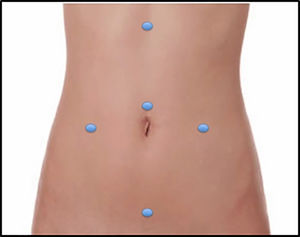
ProcedureFive 10mm laparoscopic ports were placed (Fig. 1). Beginning with a complete exploration of the abdominal cavity, intraoperative findings were limited pseudomyxoma on the right pelvic and right parietal peritoneal surfaces and a moderate amount of free mucin and implants on the left ovary and greater omentum. No gross miliary dissemination or mucinous ascites were present. The PCI was 3/39 and therefore a laparoscopic CRS and HIPEC was indicated.
The procedure involved right parietal and right pelvic peritonectomy, bilateral salpingo-oophorectomy with section at the origins of the Fallopian tubes with no need of hysterectomy as no gross involvement was identified, partial cequectomy including the line of staples of the appendiceal stump, resection of the hepatic round ligament, and total greater omentectomy with gastroepiploic vessel preservation. During the entire surgery, several mucinous lesions macroscopically identified were electrofulgurated. A complete cytoreduction CC0 was achieved. We performed a Pfannenstiel laparotomy for specimens retrieval, protected with a wound retractor.
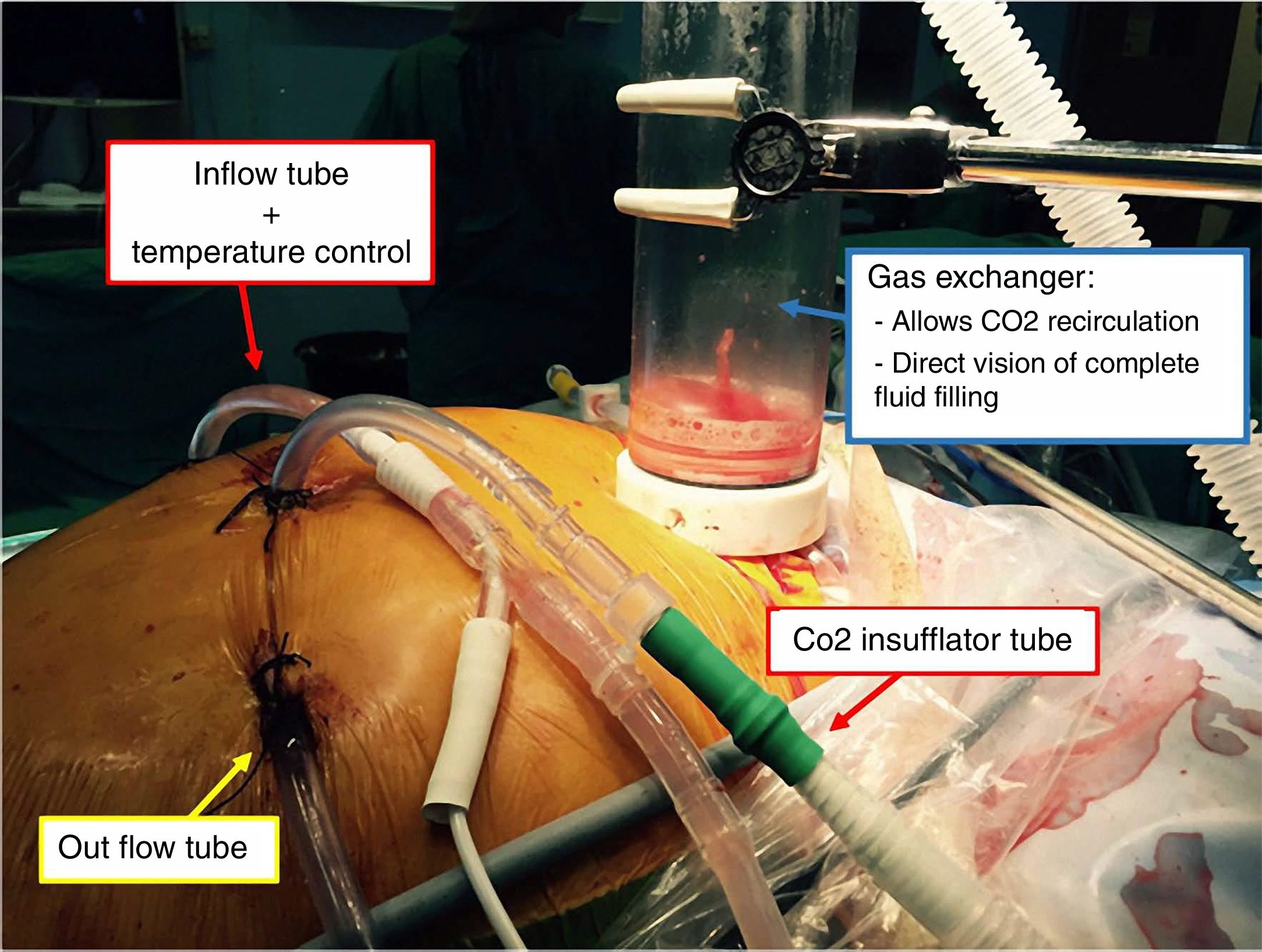
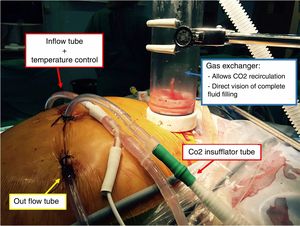
A closed-circuit system with CO2 turbulent flow (Biosurgical®) was used for hyperthermic intraperitoneal chemotherapy with 50mg Mitomicin C during 60min at 42°C in the intraabdominal cavity. Two inflow and two outflow perfusion catheters were placed using the laparoscopic ports (Fig. 2).
After the perfusion, the peritoneal cavity was explored to assure lack of bleeding and visceral injuries and the Pfannestiel laparotomy was closed with a running suture. A Penrose drain was placed in the pouch of Douglas.
Pathological findings were mucinous pools and occasional epithelial lesions on parietal the peritoneum with no cellular atypia, compatible with disseminated peritoneal adenomucinosis (DPAM). The cecum and appendicular base, both ovaries, the round ligament and the greater omentum were free of disease.
The patient recovered uneventfully and was discharged at postoperative day 5. At eighteen-month follow-up the patient is free of tumor and asymptomatic.
Although the experience in laparoscopic cytoreductive surgery followed by HIPEC in humans still remains limited, lately some experienced cytoreductive groups, such as Esquivel4–6 and Passot,3 have extended the indications for a laparoscopic approach to borderline and limited peritoneal surface diseases with a low peritoneal carcinomatosis index, including limited DPAM and benign multicystic mesothelioma with encouraging results. These procedures allowed a safe complete macroscopic cytoreduction and HIPEC with faster recovery and a shorter hospital stay.
The limitations of laparoscopic approach are the difficulty exploring the whole abdominal cavity, especially in obese patients, and a prolonged learning curve which requires advanced laparoscopic skills. A limitation attributed to the HIPEC closed technique is the heterogeneity of drug distribution. This problem could be solved with a “jacuzzi” drug infusion through a CO2 turbulent flow system, as we used in our case. A more homogeneous drug distribution with this technique has been demonstrated in animal models using methylene blue, reaching a complete drug distribution over all abdominal surfaces.7
The most validated predictors of outcome are preoperative tumor burden measured in terms of the PCI and postoperative completeness of cytoreduction.8 Delivery of hyperthermic intraperitoneal chemotherapy can be safely performed using either the open or the closed technique, without significant differences in operative time or efficacy,9 and several studies have even demonstrated increased drug diffusion with the laparoscopic technique, associating the increased intra-abdominal pressure induced by pneumoperitoneum on drug pharmacokinetics, with faster absorption and higher penetration of the chemotherapy drug in tissues.10
CRS and HIPEC by laparoscopic approach is a feasible and safe technique that allows a faster recovery than a xipho-pubic laparotomy approach, allowing a complete cytoreduction in highly selected patients performed by experience oncological surgeons. Obviously, longer follow-up and additional studies are required to evaluate its long-term efficacy.
Please cite this article as: Arjona-Sánchez Á, Rodríguez-Ortiz L, Rufián-Peña S, Sánchez-Hidalgo JM, Briceño-Delgado J. Abordaje laparoscópico en la cirugía citorreductora completa y la quimioterapia intraperitoneal hipertérmica mediante un sistema cerrado de CO2 en un pseudomixoma peritoneal de bajo grado. Cir Esp. 2018;96:656–658.