Arachnoid cysts of spine are a very rare occurrence. The aetiology still remains unclear, but the most accepted explanation is the existence of areas of weakness in the spinal dura. Symptoms depend on the location in the spine. Magnetic resonance imaging is used for its diagnosis. Management depends of clinical presentation, and the surgery is reserved for patients with neurological impairment.
Clinical caseA case is described of 67 year-old male with myelopathy and radiculopathy symptoms, both diagnosed simultaneously. The magnetic resonance imaging was used to diagnose a thoracolumbar extradural arachnoid cyst from T12-L2 and lumbar spinal canal stenosis. The patient was treated with a puncture procedure to empty the cyst and decompress the neural elements. There was a clinical improvement of myelopathy syndrome after puncture procedure. One month later, the patient underwent a minimally invasive surgical approach to decompress the neural elements in lumbar spine, achieving improvement of the radiculopathy syndrome and neurogenic claudication in both legs.
ConclusionThere is currently no standard minimally invasive approach to surgically treat these cysts, but if the patient has mild symptoms, clinical observation is recommended.
Los quistes aracnoideos son enfermedades raras de la columna vertebral. Su etiología continua siendo incierta y la explicación más aceptada es la existencia de áreas de debilidad en la duramadre espinal. Los síntomas dependen de su localización en el raquis. La resonancia magnética es usada para su diagnóstico. El tratamiento depende de su presentación clínica y la cirugía está reservada para pacientes con deterioro neurológico progresivo.
Caso clínicoPaciente masculino de 67 años de edad con síntomas mielopáticos y radiculares en miembros pélvicos. Se encontró en resonancia magnética un quiste aracnoideo extradural espinal de T12 a L2 asociado a canal lumbar estrecho. Se le realizó una punción evacuatoria dirigida al quiste para descomprimir los elementos neurales, obteniendo mejoría clínica del síndrome mielopático. Un mes después se sometió a una cirugía mínimamente invasiva descompresiva en el canal lumbar estrecho, presentando mejoría del síndrome radicular y claudicación neurogénica de ambas extremidades inferiores.
ConclusiónActualmente no existe un abordaje mínimamente invasivo estandarizado para el tratamiento quirúrgico de estos quistes. Sin embargo si el paciente tiene síntomas leves se recomienda manejo clínico conservador.
Spinal extradural arachnoid cysts are very rare expansive lesions of the vertebral column. They present clinically with signs of compression of the spinal cord depending on their location inside the spinal canal.1 Sixty-five percent present in the lower thoracic region, 13% at lumbar level, 12% in the thoracolumbar transition, 7% at the level of the sacrum, and 3% in the cervical spine.2 Extradural arachnoid cysts develop from protrusions through small defects in the dura.3 They have a pedicle through the dural defect that communicates the spinal subarachnoid space with the extradural space; their content is cerebrospinal fluid.4 They are suspected to be congenital in origin, however they might be acquired through trauma, infections, inflammation or other causes.5 In this article we describe the case of a patient with myelopathy and radiculopathy symptoms. An incidental diagnosis was made of spinal extradural arachnoid cyst in the thoracolumbar spine as the cause of the myelopathy syndrome and a narrow lumbar canal as the cause of the radiculopathy and neurogenic claudication.
ObjectiveThe aim of this manuscript was to undertake a thorough review of spinal arachnoid cysts and to describe a clinical case as an example.
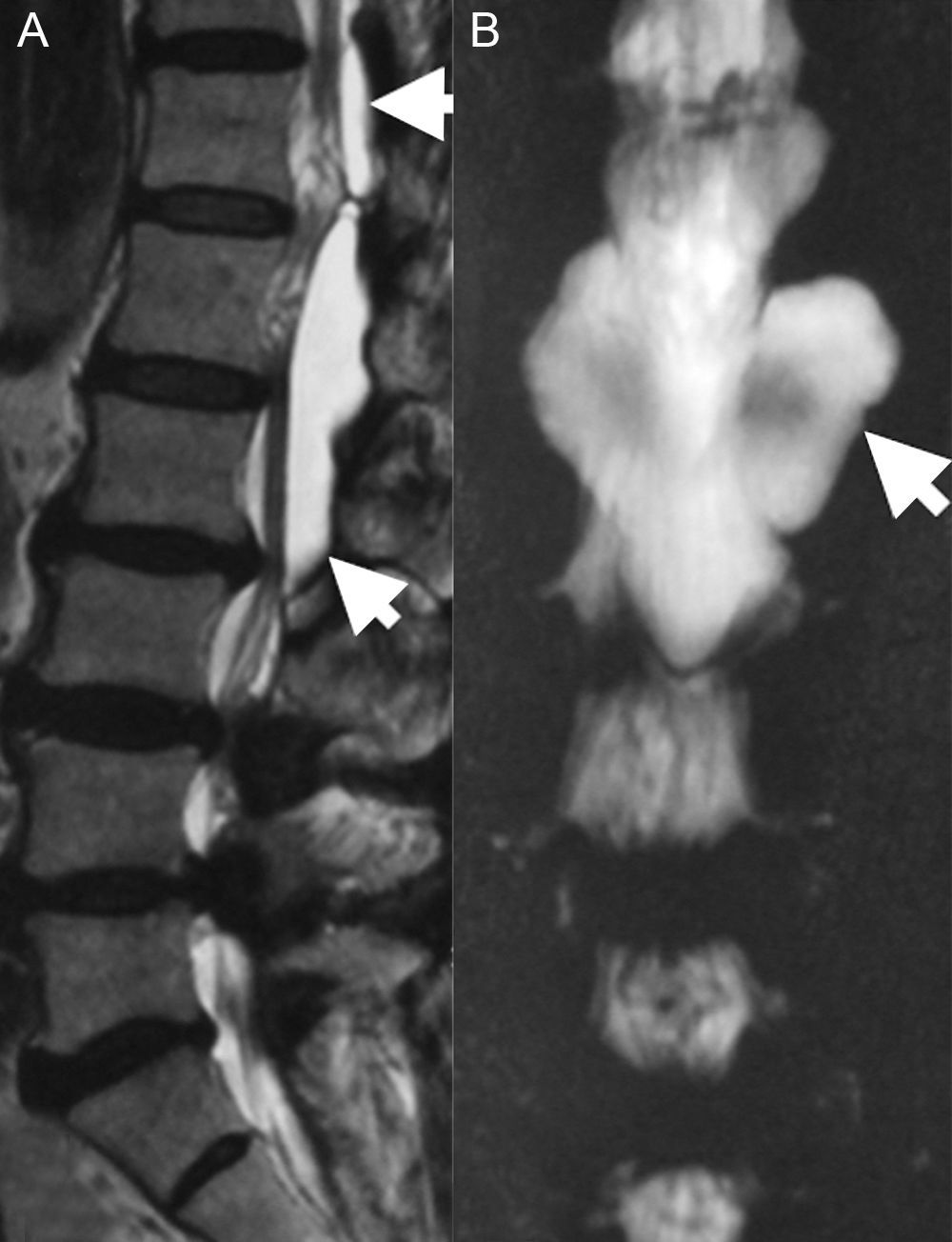
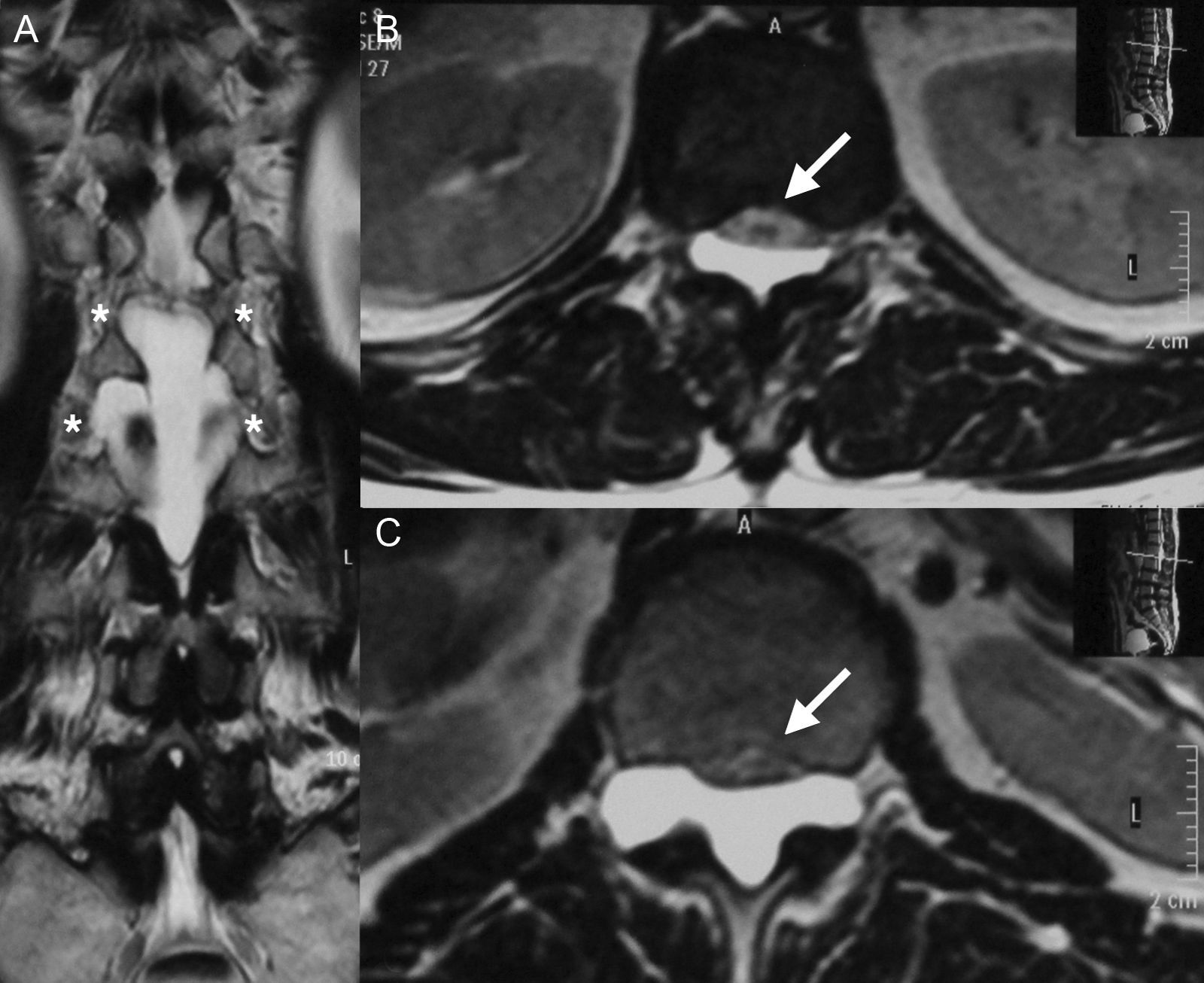
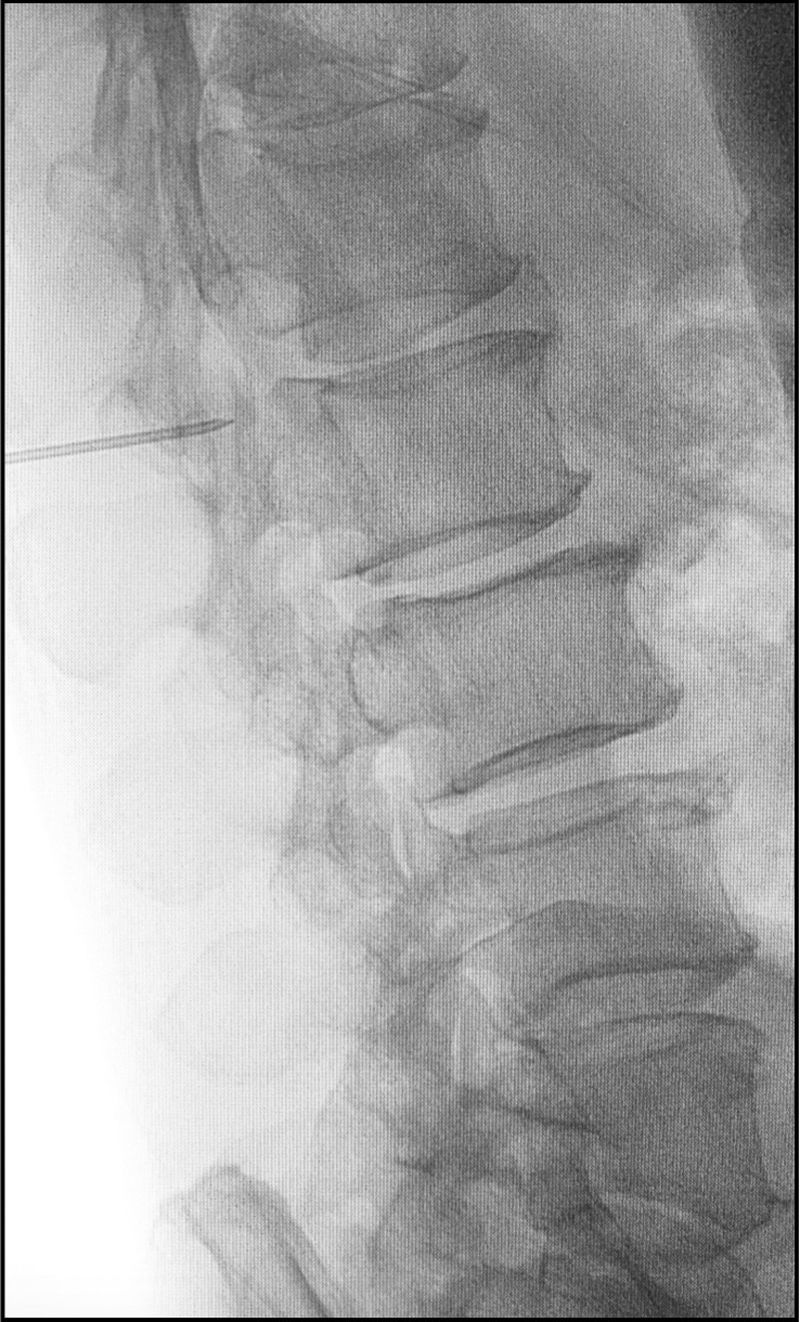
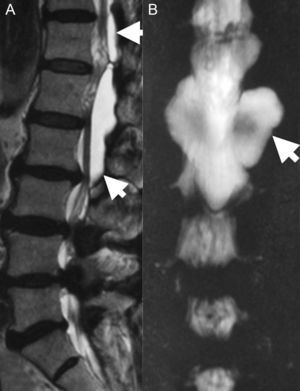
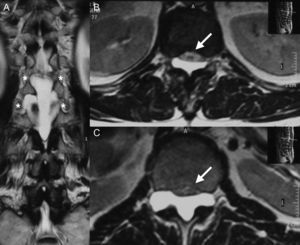
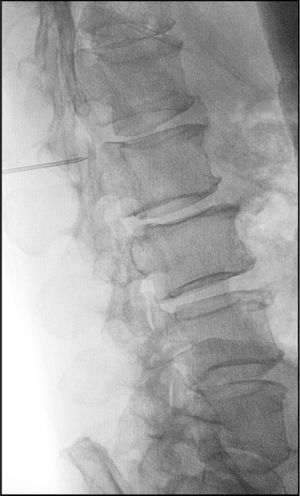
Clinical caseA 67-year-old male with a history of type 2 diabetes mellitus and lower back pain irradiating to both legs, predominantly the right, neurogenic claudication of both legs and weakness in both feet for 15 months. Physical examination revealed hypoesthesia in the right L5 dermatome, increased myotatic reflexes in both legs with Babinski sign and 4/5 power in the psoas and quadriceps bilaterally. Central and lateral stenosis of the spinal canal could be seen on magnetic resonance imaging at lumbar level from L3-L4, L4-L5, as well as the presence of a cystic lesion with regular limits, from T12 to L2. The lesion was hypointense in T1-weighting and hyperintense in T2-weighting, characteristically homogeneous with the cerebrospinal fluid; no contrast enhancement was observed on the MRI (Fig. 1). The compression of the conus medullaris and the dural sac was notable in T12-L1 and L1-L2 respectively and bilateral foraminal stenosis (Fig. 2), at the same levels due to expansion of the cyst. Given these signs, we decided to perform an evacuatory lumbar puncture targeting the spinal extradural cyst in space L1-L2 guided by fluoroscopy (Fig. 3), in order to decompress the nerve elements on which the cyst had an expansive effect. After the procedure, the patient's myelopathic syndrome improved, he had normal osteotendinous reflexes in both legs, and there were no bilateral Babinski reflexes. However, the patient continued to have neurogenic claudication and radicular pain in both legs, therefore one month after the evacuatory puncture a minimally invasive approach with microscope and tubular retractor system was undertaken through the midline for segments L3-L4 and L4-L5, and the narrow lumbar canal was decompressed. This achieved complete improvement of his symptoms.
(A) T2-weighted coronal section magnetic resonance image showing the foraminal extension of the cyst (asterisk) in T12-L1 and L1-L2. (B) T2-weighted axial section magnetic resonance image of level T12 showing ventral displacement of the conus medullaris (arrow) caused by the cyst. (C) T2-weighted axial section magnetic resonance image of level L1 showing compression of the cauda equina (arrow) caused by the cyst.
Spinal extradural arachnoid cysts are rare lesions of the spine and represent 1% of the expansive spinal lesions.6 They present more frequently in young male adults (male to female ratio of 2:1),7 and males are predominantly affected during the second decade of life.8 The associated causes are spinal trauma, surgery, arachnoiditis and neural tube defects.9 Various hypotheses have been proposed to explain why spinal arachnoid cysts form: (1) proliferation or loculation of arachnoid trabeculae in the septum posticum; (2) a fault in the expansion of the arachnoid trabecula; and (3) the formation of arachnoid diverticuli in weak areas of the spinal dura mater.1,5
Another aetiological explanation is that the condition is genetic; through the identification of heterozygotic mutations that result in loss of FOXC2 gene function (forkhead box C2 genes) in patients with familial spinal extradural arachnoid cysts. However, sporadic cysts are associated with mutations that cause loss of function of the HOXD4 gene (U homebox D4 family genes).10 Subsequently the active secretion of liquid through the cyst walls, passive osmosis of water and hydrostatic pressure of cerebrospinal fluid are possible mechanisms for the expansion of cystic volume.6 The usual location of extradural cysts inside the spinal canal is the posterior aspect of the dural sac; however, they can be found anywhere inside it.1 Symptoms can be intermittent and also exacerbated by Valsalva manoeuvres or changes in position.11 Remissions and fluctuations of symptoms have been reported in 30% of patients as a consequence of changes of pressure in the spinal canal secondary to changes in the hydrostatic pressure of the cerebral spinal fluid.1,7 Doita et al.12 used cinematic magnetic resonance to study the pathomechanism of fluctuating symptoms during Valsalva manoeuvres in patients with these cysts and concluded that changes in pressure in the extradural space and in the arachnoid cyst might cause symptoms of intermittent compression of the spinal cord. Symptoms that are often asymmetric included weakness, numbness, neuropathic pain, myelopathy and incontinence, and spastic or flaccid paraparesis.13 Very rarely, the cyst can be accompanied by herniation of the spinal cord inside it, and syringomyelia.14 Histopathologically, these cysts comprise layers of fibrocollagenous tissue with disseminated meningothelial cells.1 Magnetic resonance imaging has high sensitivity and specificity in diagnosing lesions that contain cerebrospinal fluid.1,3,15 The differential diagnoses include: Tarlov or perineural cyst, ganglion cyst, synovial cyst, meningeal diverticula next to the nerve roots, meningocele, dermoid cyst and neuroma with cystic changes.16 Nabors et al.17 classified them into 3 categories in 1988. Type I: extradural cyst without nerve tissue; Type IA: extradural meningeal or extradural spinal arachnoid cyst; Type IB: sacral meningocele; Type II: extradural cyst containing nerve tissue, Tarlov or perineural cyst; Type III: spinal cyst. The management can vary according to the patient's symptoms.18 There are many surgical options reported in the literature: bone decompression, subtotal or total resection of the cyst, drainage and marsupialisation of the cyst.19 In asymptomatic patients, conservative management with subsequent clinical observation is recommended.18 The cornerstone of management in patients with moderate to severe neurological deterioration is complete removal of the cyst followed by obliteration of the pedicle and complete repair of the dural defect, in order to prevent the valve mechanism and recurrence of the cyst.20 However, the site of communication of the cyst between the extradural and subarachnoid space is not always found during surgery.21 Some other authors such as Kunz et al.22 conclude that patients with mild symptoms could be treated conservatively, while patients with moderate to severe neurological deficit might benefit from surgical treatment.
ConclusionsAlthough spinal extradural arachnoid cysts are rare, surgeons should always suspect them as a diagnosis, especially in patients that present homogeneous cystic lesions with cerebrospinal fluid on T1 and T2-weighted magnetic resonance. The medical literature describes various ways of treating these lesions, and the objective of all of them is decompression of the nerve elements. More evidence is needed to standardise a management option in patients with no neurological symptoms and those with mild neurological symptoms.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that they have followed the protocols of their work center on the publication of patient data.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Conflict of interestThe authors have no conflict of interests to declare.
Please cite this article as: Quillo-Olvera J, Quillo-Reséndiz J, Gutiérrez-Partida C-F, Rodríguez-García M. Quiste aracnoideo extradural espinal: reporte de un caso y revisión de la literatura. Cir Cir. 2017;85:544–548.