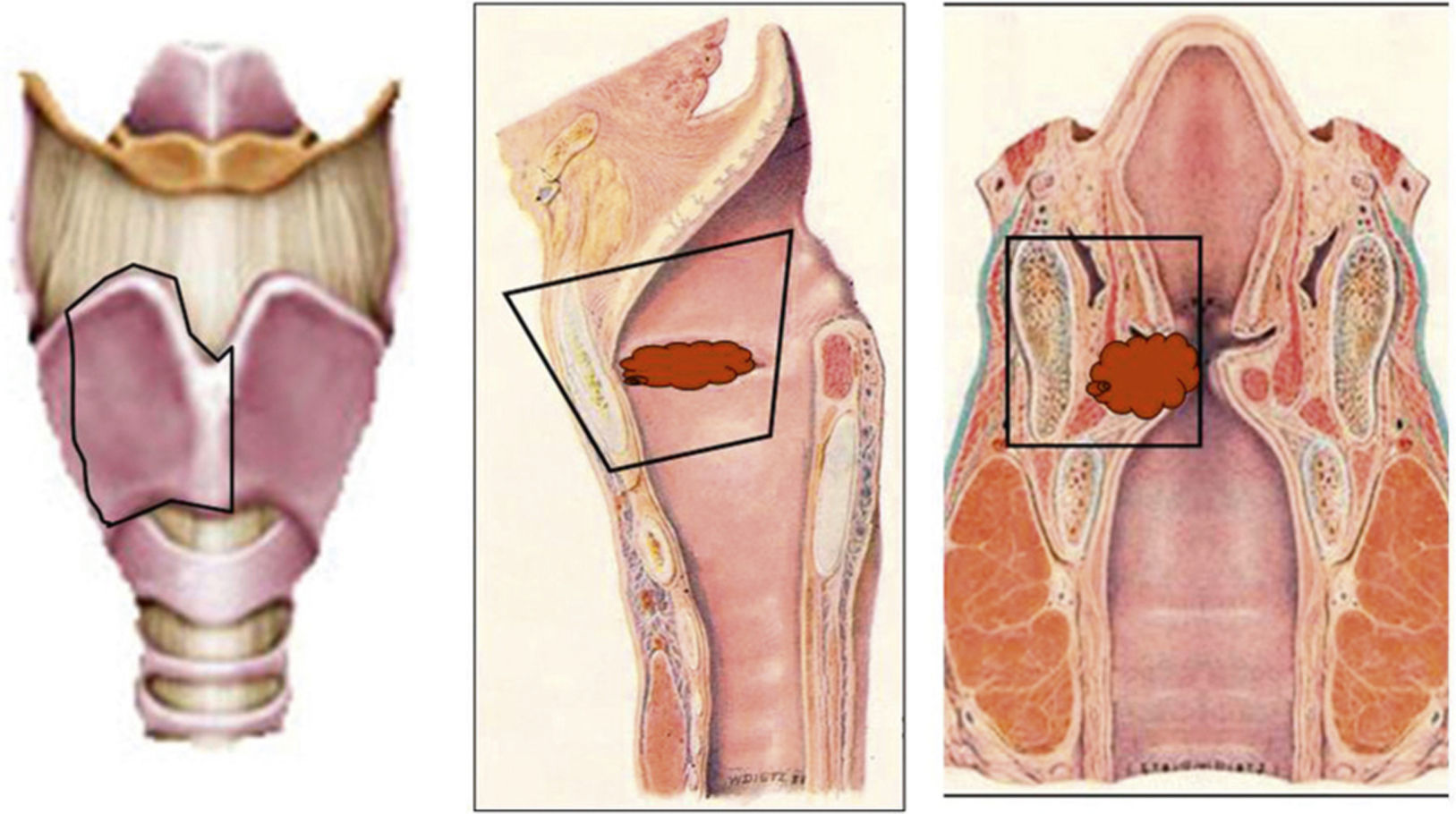
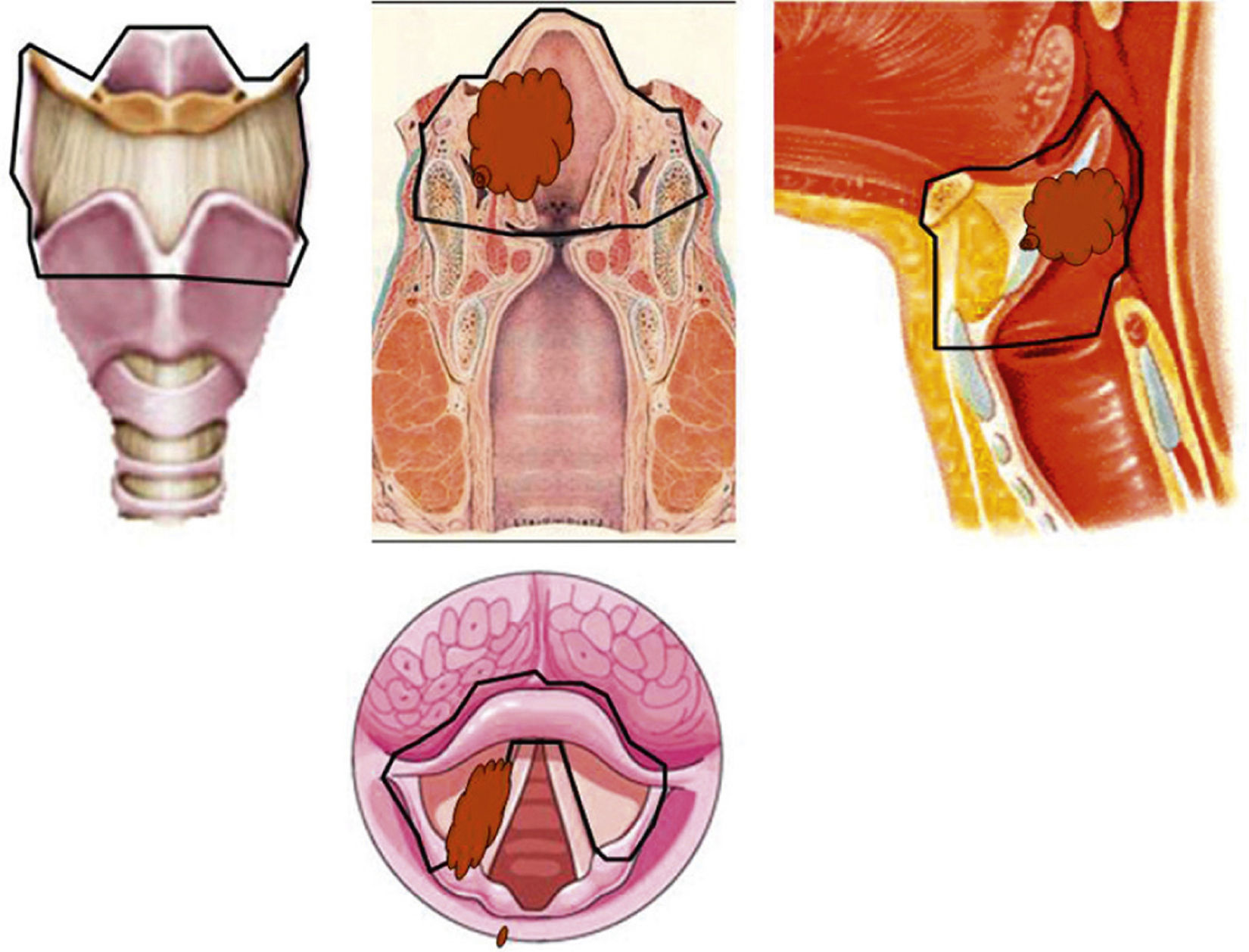
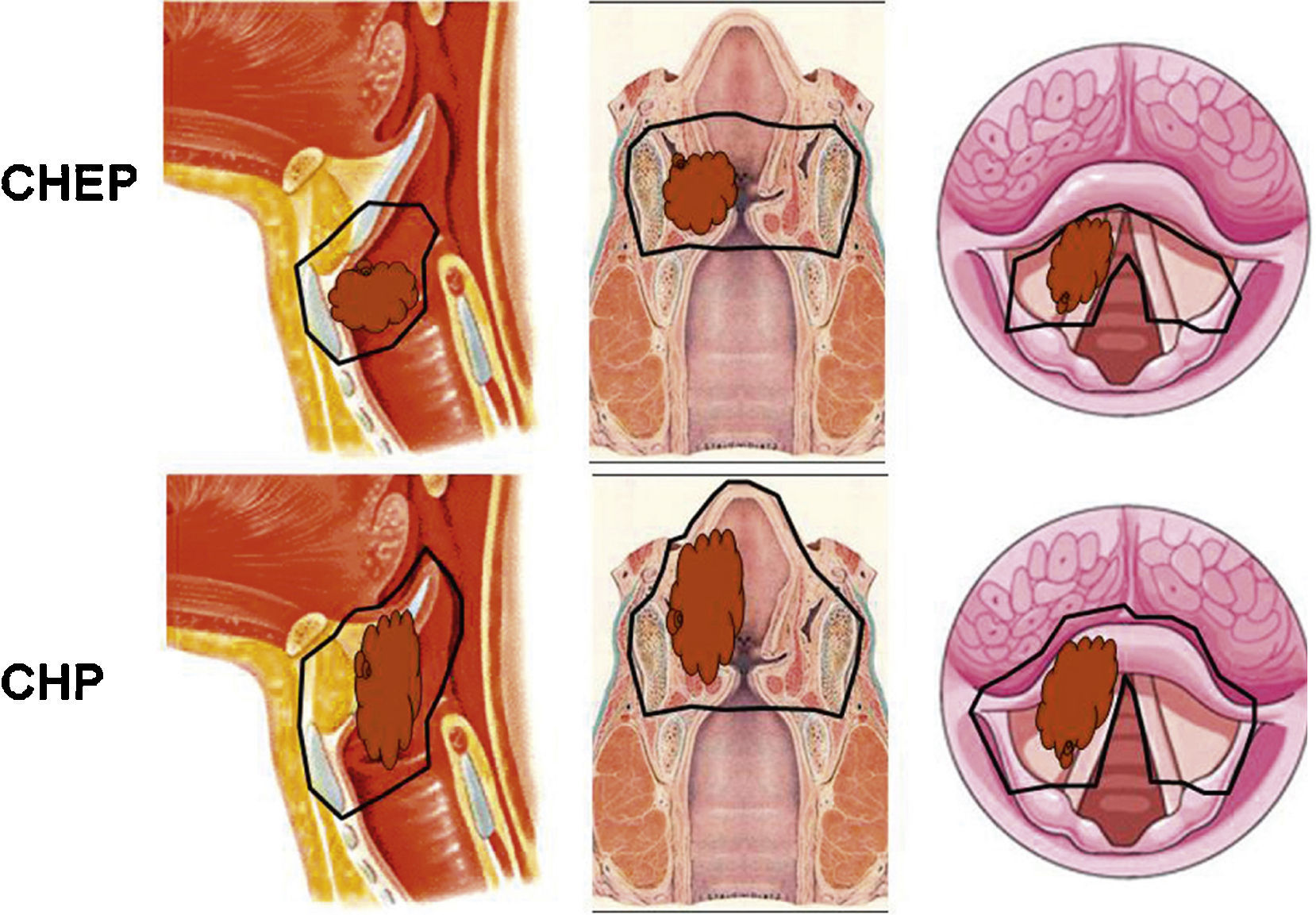
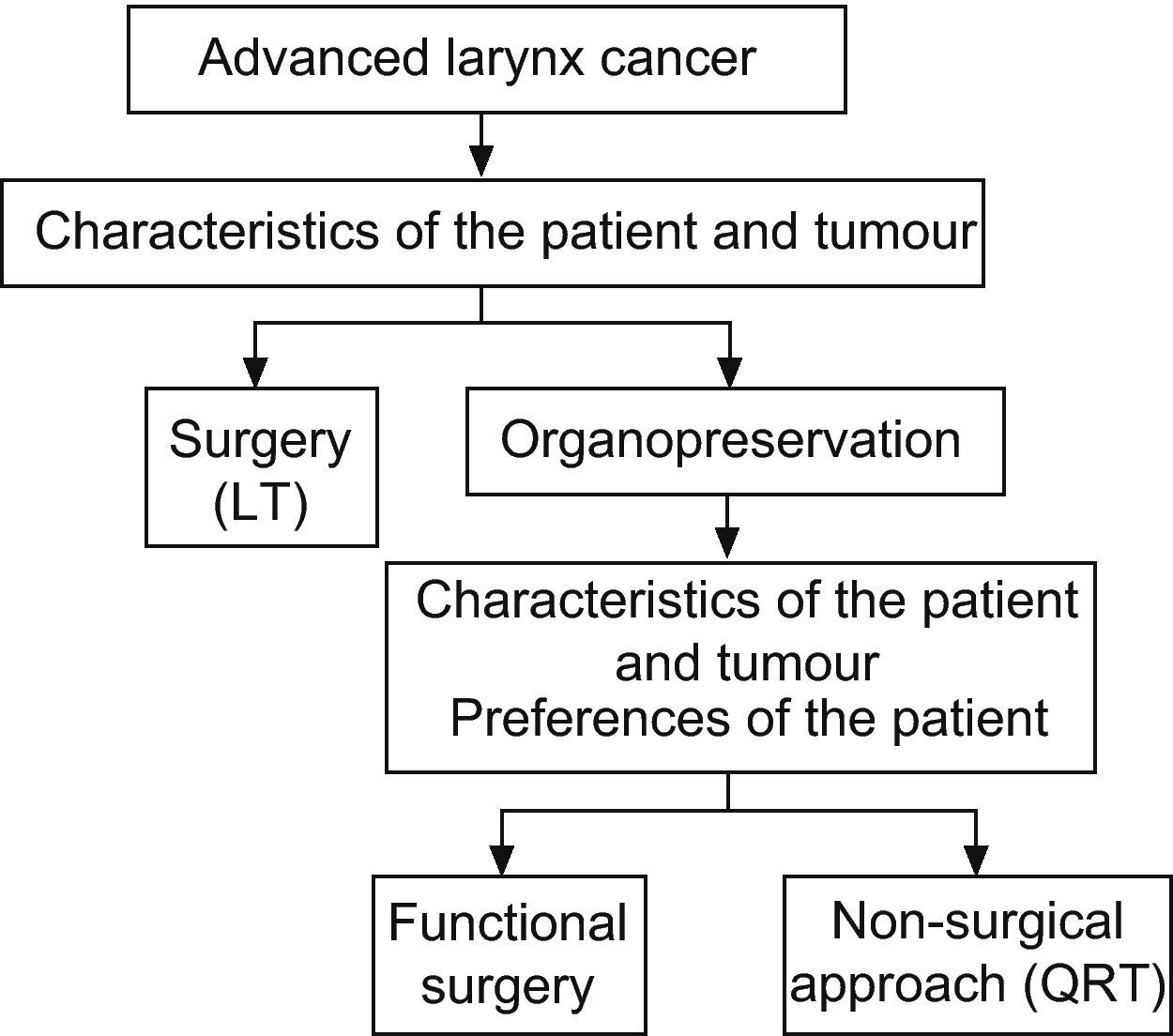
With the current advances and recent organ preservation protocols for intermediate or advanced stage laryngeal cancer, based on chemotherapy, the role of surgery seemed replaced except for surgical rescue of tumours not responding to these treatments, total laryngectomy being the surgical option. This type of non-surgical treatment is offered as a strategy for organ preservation, as opposed to total laryngectomy. However, we believe that there are two organ-preservation strategies, surgical and non-surgical. A wide spectrum of surgical techniques is available and such techniques lead to excellent results, both oncological and functional (speech and swallowing). The aim of this paper is to present options for organ-preserving surgery for laryngeal cancer. A review of surgical techniques available for functional preservation in cancer of the larynx at intermediate or advanced stage is presented. In addition to the classic approaches, such as vertical partial laryngectomy and horizontal or supraglottic laryngectomy, options for conservative laryngeal surgery have improved significantly over the past two decades. Minimally invasive surgery, transoral laser surgery, and supracricoid partial laryngectomy have become important laryngeal preservation approaches for patients with laryngeal cancer. Surgery must define its role in the multidisciplinary treatment of advanced cancers of the larynx, which at present often favours (chemo)radiotherapy protocols.
Con los actuales avances y los últimos protocolos de preservación de órgano para el cáncer de laringe en estadio intermedio o avanzado, basados en la quimioradioterapia, el papel de la cirugía parecía relevado únicamente al rescate quirúrgico de los tumores que no respondían a estos tratamientos, siendo la opción quirúrgica la laringectomía total. Este tipo de tratamientos no quirúrgicos, se ofrecen como estrategias de preservación de órgano, en contraposición a la laringectomía total. Sin embargo, nosotros consideramos que hay dos estrategias de preservación de órgano, no quirúrgica y quirúrgica. Un amplio espectro de técnicas quirúrgicas están disponibles y dan lugar a unos excelentes resultados tanto oncológicos como funcionales (habla y deglución). El objetivo de este artículo es presentar las opciones para la cirugía de conservación de órgano para el cáncer de laringe. Se realiza una revisión de las técnicas quirúrgicas disponibles para la preservación funcional en los carcinomas de laringe en estadio intermedio o avanzado. Además de los abordajes clásicos, como la laringectomía parcial vertical y la laringectomía supraglótica u horizontal, las opciones para la cirugía con-servadora laríngea han mejorado significativamente en las últimas dos décadas. La cirugía mínimamente invasiva y la cirugía transoral laser, y la laringectomía parcial supracricoidea se han convertido en importantes abordajes de conservación laríngea para los pacientes con cáncer de laringe. La cirugía debe definir su papel en el tratamiento multidisciplinario de los cánceres avanzados de laringe, que actualmente favorece a menudo a los protocolos de (quimio) radioterapia.