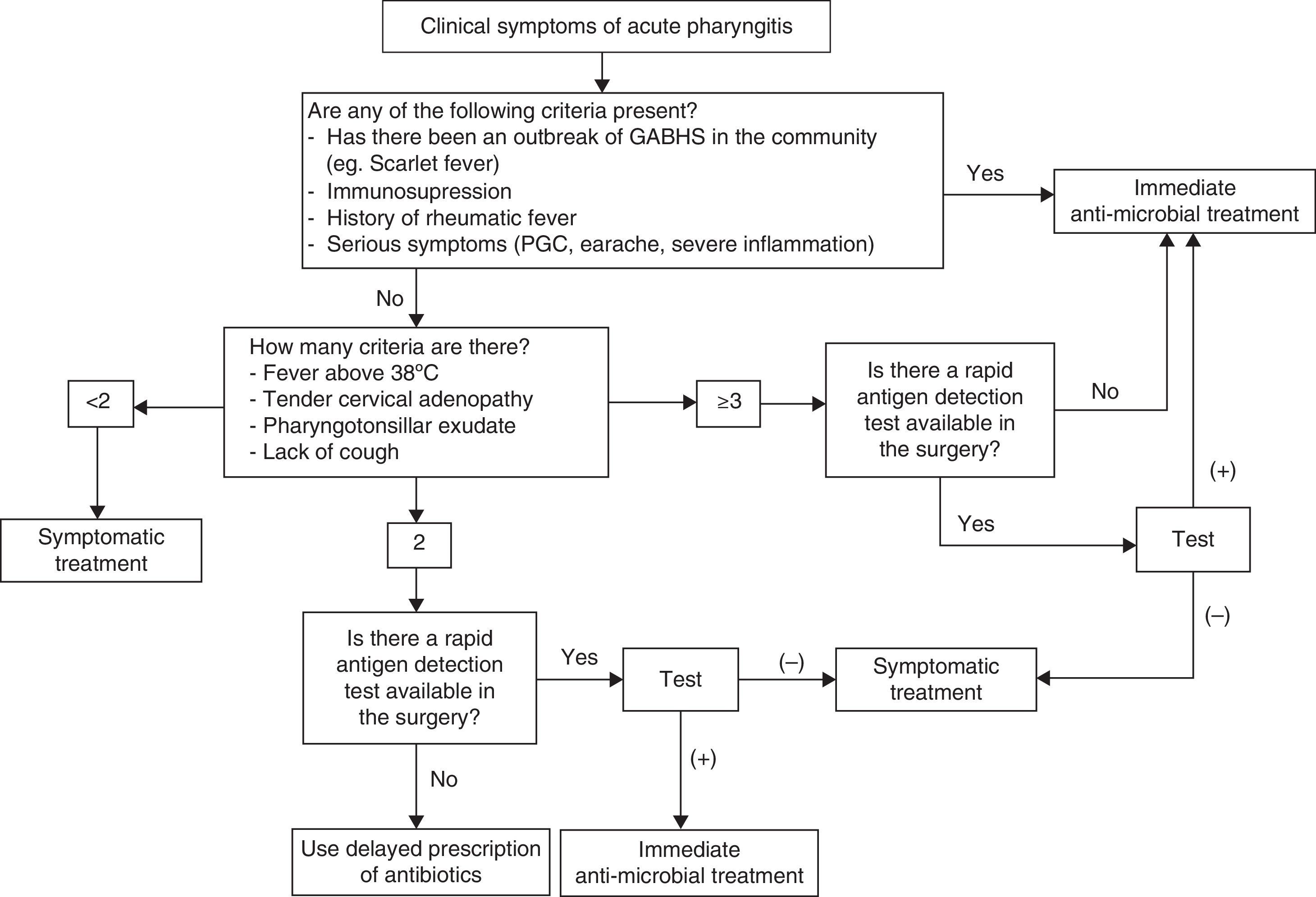
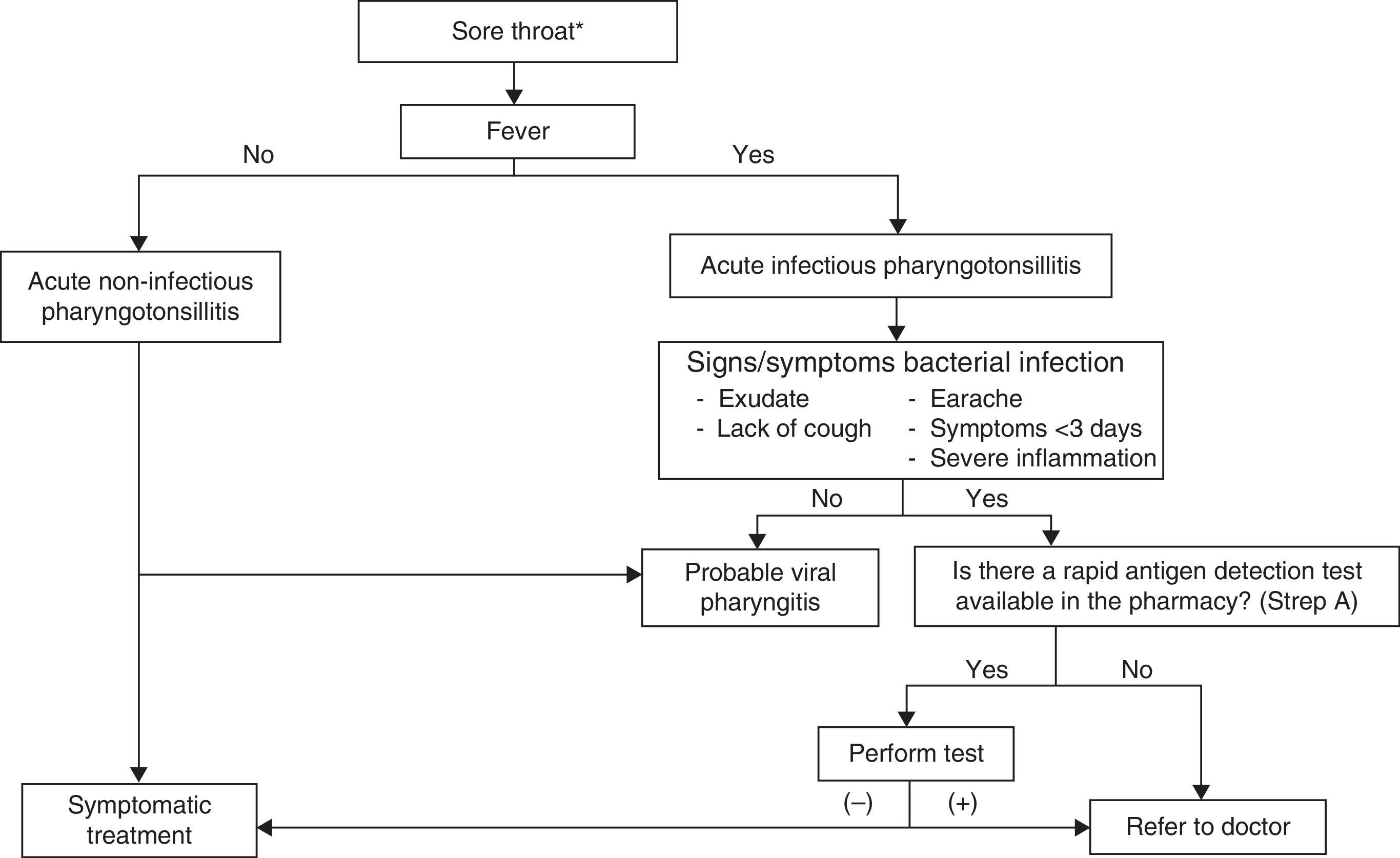
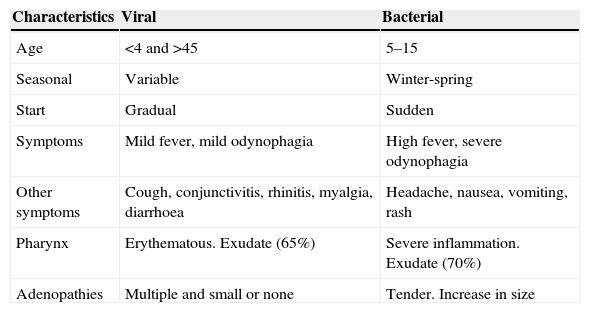
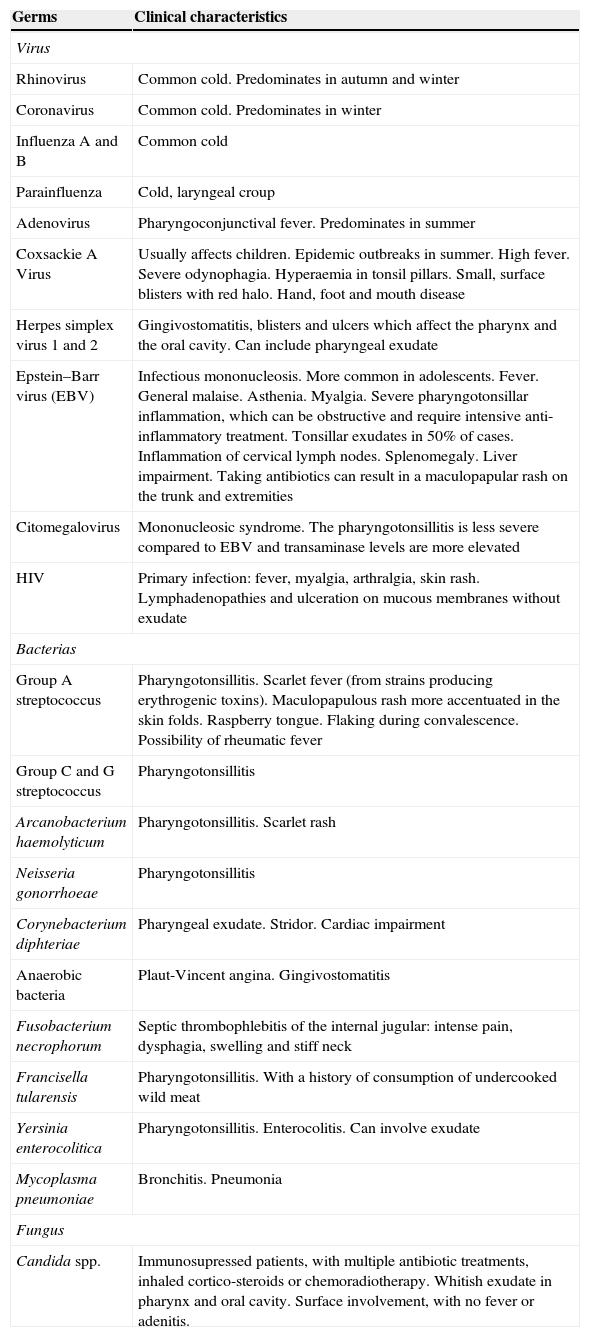
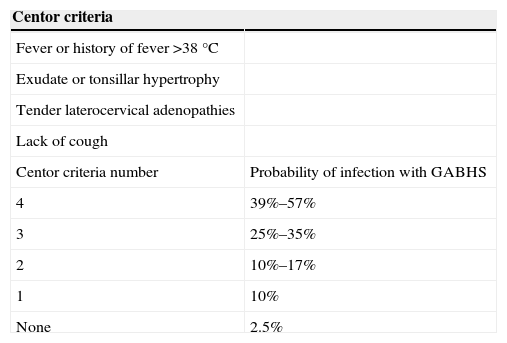
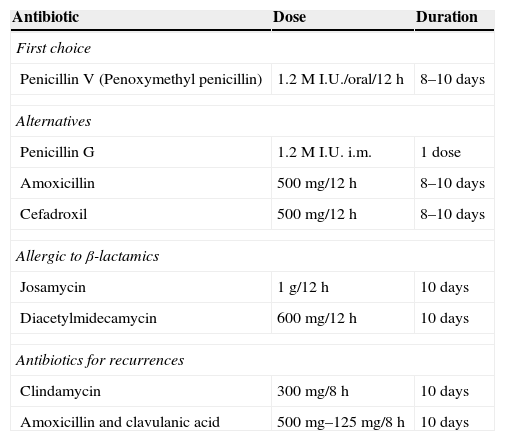
Acute pharyngitis in adults is one of the most common infectious diseases seen in general practitioners’ consultations. Viral aetiology is the most common. Among bacterial causes, the main agent is Streptococcus pyogenes or group A β-haemolytic streptococcus (GABHS), which causes 5%–30% of the episodes. In the diagnostic process, clinical assessment scales can help clinicians to better predict suspected bacterial aetiology by selecting patients who should undergo a rapid antigen detection test. If these techniques are not performed, an overdiagnosis of streptococcal pharyngitis often occurs, resulting in unnecessary prescriptions of antibiotics, most of which are broad spectrum. Consequently, management algorithms that include the use of predictive clinical rules and rapid tests have been set up. The aim of the treatment is speeding up symptom resolution, reducing the contagious time span and preventing local suppurative and non-suppurative complications. Penicillin and amoxicillin are the antibiotics of choice for the treatment of pharyngitis. The association of amoxicillin and clavulanate is not indicated as the initial treatment of acute infection. Neither are macrolides indicated as first-line therapy; they should be reserved for patients allergic to penicillin. The appropriate diagnosis of bacterial pharyngitis and proper use of antibiotics based on the scientific evidence available are crucial. Using management algorithms can be helpful in identifying and screening the cases that do not require antibiotic therapy.
La faringoamigdalitis aguda (FAA) en el adulto es una de las enfermedades infecciosas más comunes en la consulta del médico de familia. La etiología más frecuente es viral. Dentro de la etiología bacteriana, el principal agente responsable es Streptococcus pyogenes o estreptococo β-hemolítico del grupo A (EBHGA), causante del 5-30% de los casos. En el manejo diagnóstico, las escalas de valoración clínica para predecir la posible etiología bacteriana, son una buena ayuda para seleccionar a qué pacientes se deben practicar las técnicas de detección rápida de antígeno estreptocócico. Es conocido que, en general, sin estas técnicas se tiende al sobrediagnóstico de FAA estreptocócica, con la consiguiente prescripción innecesaria de antibióticos, muchas veces de amplio espectro. Así, con el manejo de las escalas y la técnica de diagnóstico rápido, elaboramos los algoritmos de manejo de la FAA. Los objetivos del tratamiento son acelerar la resolución de los síntomas, reducir el tiempo de contagio y prevenir las complicaciones supurativas locales y no supurativas. Los antibióticos de elección para el tratamiento de la FAA estreptocócica son penicilina y amoxicilina. La asociación de amoxicilina y clavulánico no está indicada en el tratamiento inicial en la infección aguda. Los macrólidos tampoco son un tratamiento de primera elección; su uso debe reservarse para pacientes con alergia a la penicilina. Es importante en nuestro país adecuar tanto el diagnóstico de la FAA bacteriana y la prescripción de antibióticos a la evidencia científica disponible. La implantación de protocolos de actuación en las farmacias comunitarias puede ser de utilidad para identificar y cribar los casos que no requieran tratamiento antibiótico.