Subtotal petrosectomy is the complete exenteration of all air cell tracts of the temporal bone. The isthmus of the Eustachian tube is obliterated and the external auditory canal is closed. The aim of this study was to describe the use of this technique in the management of certain cases of chronic otitis media.
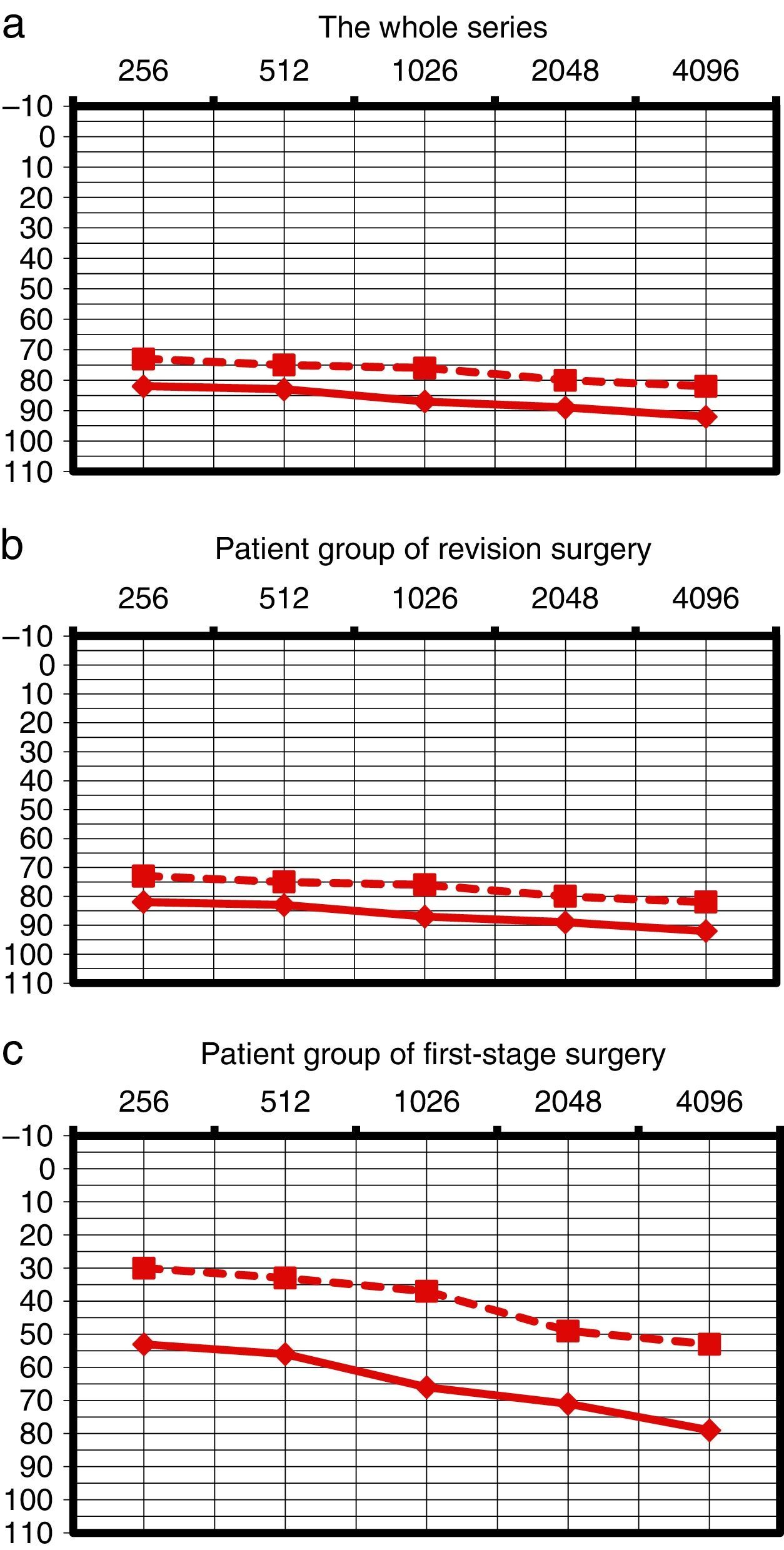
Materials and methodsWe conducted a retrospective revision of the patients treated in our institution with this technique for chronic otitis media in a 5-year period (2008–2012). All charts were reviewed and data from the otomicroscopy, audiometry, radiology, surgical findings, postoperative complications and follow-up (including diffusion magnetic resonance imaging, MRI) of a minimum of 24 months were collected.
ResultsIn this period petrosectomy was performed on 28 patients for chronic otitis media. We treated 13 cases as primary cases, while 15 cases were secondary (patients that had already undergone another procedure in that ear). Fifteen cases had no serviceable hearing. Only 1 case had an immediate postoperative complication (infection); during the posterior follow-up, 2 cases had to be reoperated for diffusion restriction in the mastoid area revealed in the MRI 2 years after surgery.
ConclusionsA subtotal petrosectomy is rarely performed for the treatment of chronic otitis media. However, it is a technique that we have to keep in mind for the treatment of certain cases where there is recurrence and deep hearing loss, as well as in cases with good cochlear reserve if the disease coexists with other complications.
La petrosectomía subtotal consiste en la eliminación completa de todas las celdas neumáticas del hueso temporal. La Trompa de Eustaquio se oblitera y el conducto auditivo externo se cierra. El objetivo de este estudio es describir el uso de esta técnica en el manejo de determinados casos de otitis media crónica.
Material y MétodoSe realiza un estudio retrospectivo de los pacientes intervenidos en nuestro hospital de petrosectomía subtotal para el tratamiento de otitis medias crónicas en un período de 5 años (2008–2012). Se recogieron datos de su historia clínica, exploración otomicroscópica, audiometría, radiología, hallazgos quirúrgicos, complicaciones postquirúrgicas y seguimiento posterior (incluyendo Resonancia magnética con difusión) con un mínimo de 24 meses de seguimiento.
ResultadosEn este período se realizaron 28 petrosectomías para el tratamiento de otitis medias crónicas. 15 casos fueron secundarias, es decir, el oído ya había sido intervenido con anterioridad y en 13 casos se trató de una actitud primaria. 15 de estos casos no tenían una audición útil. El postoperatorio inmediato transcurrió sin incidencias en todos los casos salvo en uno en el que ocurrió una infección. A largo plazo, debieron reintervenirse dos casos por mostrar la Resonancia restricción en la difusión a los dos años de la cirugía.
ConclusionesLa necesidad del empleo de la petrosectomía subtotal en el tratamiento de las otitis medias crónicas es rara pero deberemos tenerlo en cuenta en aquellos casos recurrentes en los que exista una hipoacusia severa a profunda así como en casos con buena reserva coclear si coexiste una complicación añadida.