The set of symptoms relating to disorders of the balance system are common in the general population. However, there are few studies quantifying the frequency of onset of the various vestibular disorders that present in specialist otoneurology units in the Spanish population. The aim of this study is to establish the epidemiology of vestibular disorders, their form of presentation, and the expected care burden in a specialist otoneurology clinic.
Material and methodsA retrospective, descriptive, observational study of patients referred to the otoneurology unit of a third level hospital between 1/1/2015 and 31/12/2015.
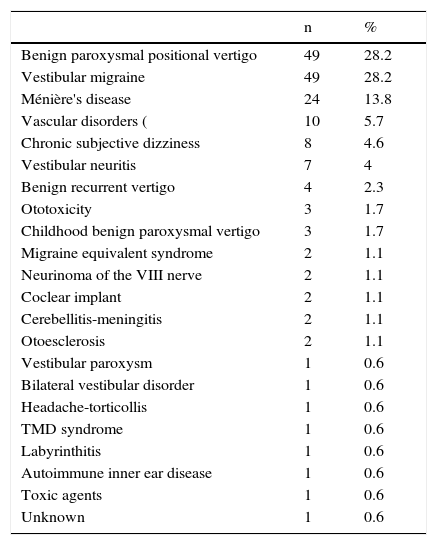
ResultsOne hundred and seventy-four patients were assessed (121 women and 53 men) with a mean age of 53±17 years. Forty-three individuals per 100,000 inhabitants were assessed over the study period. The patients were referred in the majority from external ENT (36.8%) and primary care (28.7%) clinics. The most frequent reason for consultation was dizziness (40.2%) followed by vertigo (31%). The most frequent diagnoses were benign paroxysmal positional vertigo (28.2%) and vestibular migraine (28.2%) –defined (59%) or probable (41%)–, followed by Ménière's disease (13.8%), vascular disorders (5.7%), chronic subjective dizziness (4.6%) and vestibular neuritis (4%).
ConclusionsThe availability of precise information on the prevalence and impact of vestibular disorders is important to enable the health services to plan an appropriate response to the expected care demand in the community. Benign paroxysmal positional vertigo and vestibular migraine are the most commonly diagnosed disorders in otoneurology clinics. Systematic terminology is essential for the comparison of results.
El conjunto de síntomas relacionados con los trastornos del sistema de equilibrio son comunes en la población general. Sin embargo, hay pocos estudios que cuantifiquen la frecuencia de inicio de los diversos trastornos vestibulares que se presentan en unidades especializadas de otoneurología. El objetivo de este estudio es establecer la epidemiología de los trastornos vestibulares,La forma de presentación y la carga de atención esperada en una clínica especialista en otoneurología.
Material y métodosEstudio descriptivo observacional retrospectivo sobre los pacientes remitidos a la consulta de Otoneurología de un centro hospitalario de tercer nivel entre el 1/1/2015 y el 31/12/2015.
ResultadosFueron valorados 174 pacientes (121 mujeres y 53 hombres) con una media de edad de 53±17 años. Durante el periodo de estudio se valoraron 43 individuos por cada 100.000 habitantes. Los pacientes fueron remitidos en su mayoría desde consultas externas de Otorrinolaringología (36,8%) y desde Atención Primaria (28,7%). El motivo de consulta más frecuente fue inestabilidad (40,2%), seguido de vértigo (31%). Los diagnósticos más frecuentes fueron vértigo posicional paroxístico benigno (28,2%) y migraña vestibular (28,2%) –definida (59%) o probable (41%)–, seguidos de enfermedad de Ménière (13.8%), trastornos de origen vascular (5.7%), mareo subjetivo crónico (4,6%) y neuritis vestibular (4%).
ConclusionesDisponer de información precisa acerca de la prevalencia e impacto de los trastornos vestibulares es importante para la correcta planificación de los servicios sanitarios con el objetivo de responder satisfactoriamente a la demanda asistencial esperada en la comunidad. El trastorno más frecuentemente diagnosticado en una consulta de Otoneurología es el vértigo posicional paroxístico benigno y la migraña vestibular. Para la comparación de resultados es indispensable la utilización de terminología sistemática.