Pharyngocutaneous fistula is the most frequent complication after total laryngectomy. Its incidence varies between 9%–25% in post primary total laryngectomy patients, to 14%–57% in salvage laryngectomy post radiotherapy or post chemotherapy+radiotherapy. The pectoralis major myofascial flap (PMMF) is postulated as a useful tool to decrease the incidence of this complication.
Materials and methodRetrospective analysis of a group of patients treated by salvage laryngectomy, associated or not with pharyngeal closure reinforcement with PMMF.
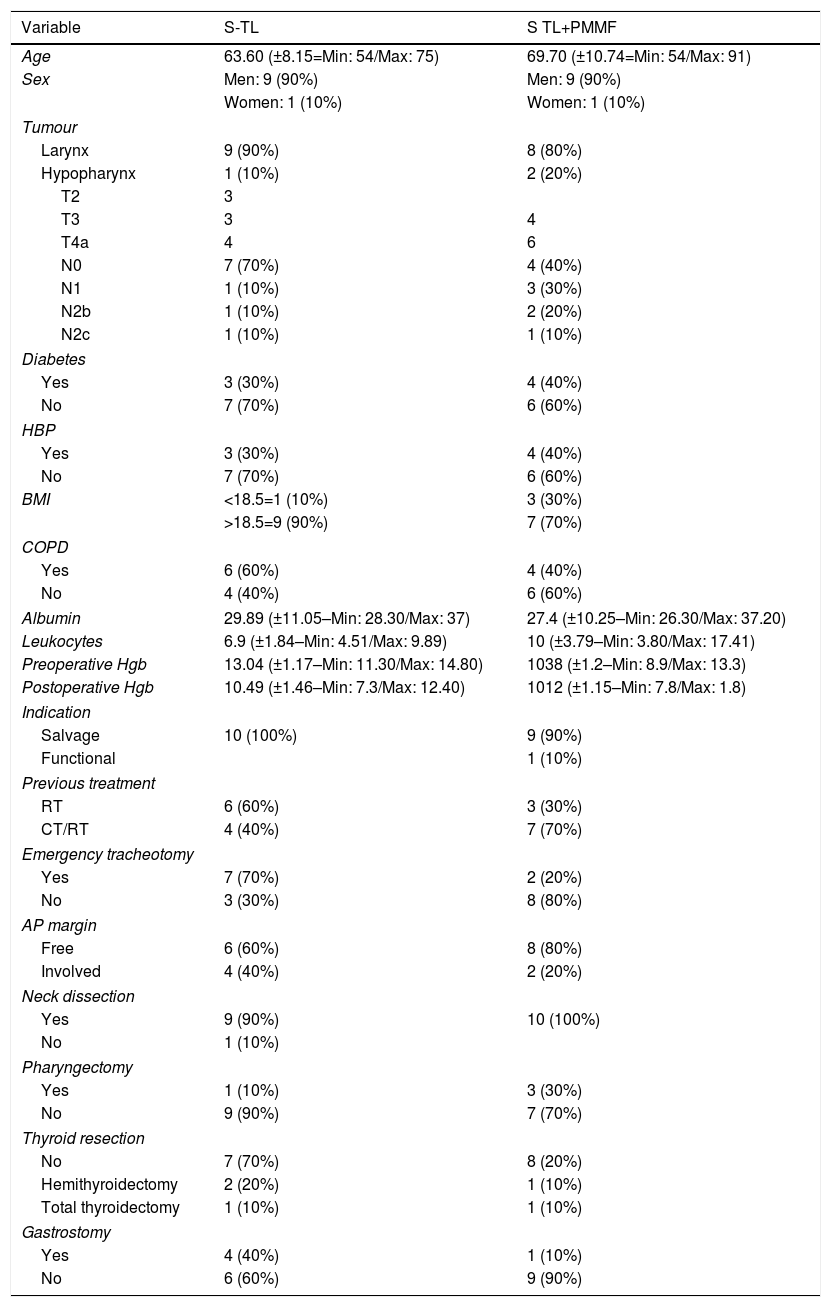
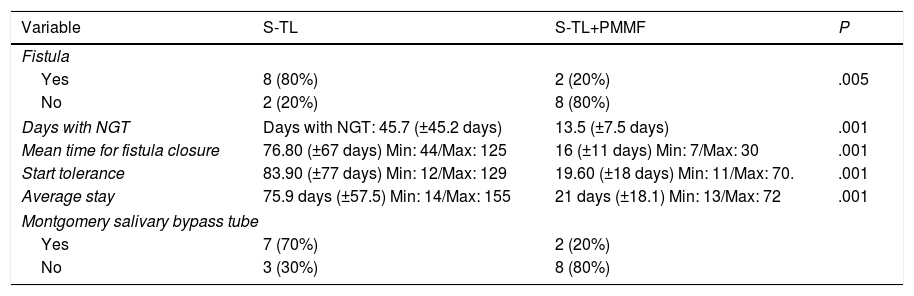
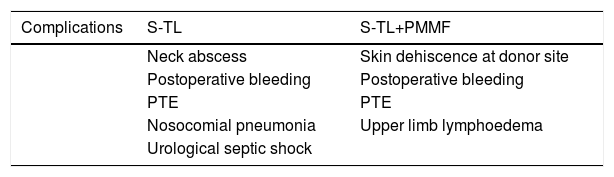
ResultsTwenty patients were included, 18 males (90%) and 2 females (10%), in 10 of whom the PMMF was used. The average age was 66.65 years. Seventeen (85%) had a laryngeal tumour and 3 (15%) had a hypopharyngeal tumour. Eight (80%) patients in the non-PMMF group had postoperative fistula, whereas only 2 (20%) patients in the PMMF group had a fistula during the postoperative period (P=.005). The mean time for fistula closure was significantly shorter in the cases where PMMF flap was used (16±11 days vs. 76.8±67 days, P=.001), as was hospital stay (19.6±18 days vs. 83.9±77 days, P=.001).
ConclusionThe use of PMMF in our series is associated with a lower rate of post salvage laryngectomy fistulas in patients treated primarily by organ preservation protocol for laryngeal/hypopharyngeal cancer. In turn, it promotes local healing by decreasing the mean duration of fistula closure and the mean hospital stay.
La fístula faringocutánea es la más frecuente de las complicaciones poslaringectomía total. Su incidencia varía entre un 9-25% en pacientes poslaringectomía total primaria, hasta un 14-57% en laringectomía de rescate posradioterapia o posquimioterapia+radioterapia. El colgajo de músculo pectoral mayor miofascial (PMMF) se postula como una herramienta útil para disminuir la incidencia de esta complicación.
Material y métodoAnálisis retrospectivo de pacientes tratados mediante laringectomía total de rescate, asociada o no a refuerzo de sutura faríngea con colgajo de PMMF.
ResultadosVeinte pacientes fueron incluidos, 18 hombres (90%) y 2 mujeres (10%), en 10 de los cuales se utilizó colgajo de PMMF. La edad promedio fue de 66,65 años. Diecisiete (85%) presentaron un tumor laríngeo y 3 (15%) un tumor de hipofaringe. Ocho (80%) pacientes del grupo sin PMMF presentaron fístula en el postoperatorio, mientras que tan solo 2 (20%) pacientes del grupo de PMMF presentaron fístula durante el postoperatorio (p=0,005). El tiempo promedio para el cierre de la fístula fue significativamente menor en los casos en que se empleó el PMMF (16±11 vs 76,8±67 días, p=0,001), así como la estancia hospitalaria (19,6±18 vs 83,9±77 días, p 0,001).
ConclusiónEl uso del PMMF se asocia a una menor tasa de fístulas poslaringectomía total de rescate en pacientes tratados de forma primaria mediante protocolo de conservación de órgano por cáncer de laringe/hipofaringe, y favorece la cicatrización local disminuyendo el tiempo promedio de cierre de fístulas y la estancia media hospitalaria.