In this update, antiretroviral therapy (ART) is recommended for all patients infected by type 1 human immunodeficiency virus (HIV-1). The objective of ART is to achieve an undetectable plasma viral load (PVL). Initial ART should comprise 3 drugs, namely, 2 nucleoside reverse transcriptase inhibitors (NRTI), and 1 drug from another family. Four of the recommended regimens, all of which have an integrase strand transfer inhibitor (INSTI) as the third drug, are considered a preferred regimen; a further 6 regimens, which are based on an INSTI, a non-nucleoside reverse transcriptase inhibitor (NNRTI), or a protease inhibitor boosted with cobicistat or ritonavir (PI/COBI, PI/r), are considered alternatives. The reasons and criteria for switching ART are presented both for patients with an undetectable PVL and for patients who experience virological failure, in which case the rescue regimen should include 3 (or at least 2) drugs that are fully active against HIV. The specific criteria for ART in special situations (acute infection, HIV-2 infection, pregnancy) and comorbid conditions (tuberculosis and other opportunistic infections, kidney disease, liver disease, and cancer) are updated.
Se recomienda tratamiento antirretroviral (TAR) a todos los pacientes con infección por VIH-1. El objetivo del TAR es lograr una carga viral plasmática (CVP) indetectable. El TAR inicial debe ser una combinación de 3 fármacos, que incluya 2 inhibidores de la transcriptasa inversa análogos de nucleósidos (ITIAN) y otro de distinta familia. Cuatro de las pautas recomendadas, todas las cuales tienen un inhibidor de la integrasa (INI) como tercer fármaco, se consideran preferentes, y otras 6, basadas en un INI, un inhibidor de la transcriptasa inversa no análogo de nucleósidos (ITINN) o un inhibidor de la proteasa potenciado con cobicistat o ritonavir (IP/COBI, IP/r), como alternativas. Se exponen las causas y los criterios para cambiar el TAR en los pacientes con CVP indetectable así como en los que presentan fracaso virológico, en cuyo caso el TAR de rescate debe incluir 3 (o al menos 2) fármacos plenamente activos frente al VIH. Se actualizan los criterios específicos del TAR en situaciones especiales (infección aguda, infección por VIH-2, embarazo) o comorbilidades (tuberculosis u otras enfermedades oportunistas, enfermedad renal, hepatopatías y neoplasias).
Since 1996, when the arrival of antiretroviral drugs made it possible to build potent combinations, antiretroviral therapy (ART) has led to huge health care benefits (reduced morbidity, mortality and transmission of the human immunodeficiency virus [HIV]). In parallel with these advances, ART has become complicated owing to the high number of drugs and families, as well as the many aspects affecting the appropriate choice of drugs (efficacy, toxicity, resistance, tropism, pharmacologic interactions, use in special situations, and cost-effectiveness).
The complexity and speed with which changes occur necessitate frequent updating of guidelines on ART. For the last 17 years, GESIDA and the National AIDS Plan have jointly edited a consensus document on ART in adults.1 The present document updates previous recommendations in this population.
The objective of this consensus document is to provide health professionals who treat HIV-infected adults with up-to-date knowledge on ART and a series of recommendations based on scientific evidence that can act as guidelines in therapeutic decision making.
Clinical and laboratory evaluation as a guide for ARTClinical evaluationIt is important to take an exhaustive clinical history, including physical and psychological data, treatment, habits, and risk practices. Specific aspects applying to women (e.g., desire to become pregnant and contraception) should be analyzed and a complete physical examination performed.
Recommendation
- •
A clinical history should be taken for all HIV-infected patients. The history should include an evaluation of the patient's drug therapy and comorbid conditions. The patient should also undergo a thorough physical examination, which should be repeated once a year (A-II).
In addition to specific determinations associated with HIV infection and its consequences, other tests should be ordered to take account of previous infections or cardiovascular risk factors.
Recommendation
- •
The initial laboratory workup should include a complete blood count, general biochemistry, and serology testing (Toxoplasma, cytomegalovirus, syphilis, HAV, HBV, and HCV). Viral load, CD4+ T-lymphocyte count, and primary resistance to HIV and HLA-B*5701 should also be determined (A-II).
The number of CD4+ T lymphocytes is the main marker of the risk of progression and onset of non-AIDS events.
Recommendation
- •
The absolute number and percentage of CD4+ T lymphocytes should be determined before initiating ART. Once therapy has started, these determinations should be made periodically to monitor the immune response (A-I).
- •
Determinations can be at longer intervals (up to 12 months) in stable patients with suppressed plasma viral load (PVL) and CD4+ T-lymphocyte counts >300–500cells/μL (C-II).
PVL is a marker of the risk of progression and transmission of HIV.
Recommendations
- •
PVL should be determined before initiation of ART and regularly during treatment (A-II).
- •
PVL is the main parameter for evaluating the virological efficacy of ART and for defining virological failure (A-I).
- •
The objectives of virological suppression (VL <50copies/mL) should be met both in ART-naïve patients and in those who have experienced previous therapeutic failure (A-II).
- •
PVL should be determined using a technique with a quantification limit of at least 50copies/mL. The same technique should always be used (A-II).
- •
If decisions on therapy are to be taken based on PVL, they should be confirmed with a second determination (A-II).
The plasma concentration of antiretroviral drugs is correlated with efficacy and toxicity; therefore, determination of their levels could prove useful in certain situations.
Recommendations
- •
Determination of the plasma concentration of antiretroviral drugs is not recommended for regular monitoring of HIV-infected patients (A-II).
- •
Determination of the plasma concentration of antiretroviral drugs may be indicated in specific clinical situations (e.g., risk of pharmacological interactions, organ transplantation, extreme underweight or overweight, pregnancy, and renal or hepatic insufficiency) and to confirm suspected poor adherence to therapy (B-III).
Viral genome mutations are the consequence of rapid HIV-1 turnover and error-prone reverse transcriptase. The emergence of resistant mutations is associated with virologic failure. Resistance mutations can be either primary or secondary to virologic failure.
Recommendations
- •
Genotyping of reverse transcriptase and protease to detect HIV resistance mutations should be performed in all patients at diagnosis of infection and before initiating ART if this is deferred (A-II).
- •
Assessment of baseline integrase resistance mutations is only recommended when there is a high suspicion of transmission of resistance to integrase strand transfer inhibitors (INSTI) (C-III).
- •
Resistance should be studied by genotyping in all patients in whom virological failure has been confirmed. The study should include integrase resistance mutations if the patient's regimen includes an INSTI (A-I).
The presence of the HLA-B*5701 allele is associated with hypersensitivity reaction to abacavir (ABC), a life-threatening multiorgan clinical syndrome observed during the first 6 weeks of treatment.
Recommendations
- •
HLA-B*5701 should be determined in all patients before initiating an ART regimen containing ABC (A-I).
- •
ABC should not be prescribed if the result of the HLA-B*5701 determination is positive (A-I).
A tropism assay is useful when prescribing maraviroc (MVC)
Recommendation
- •
Viral tropism should be determined before starting therapy with a CCR5 inhibitor (A-I).
The main objectives of ART are to reduce HIV-associated morbidity and mortality, restore and preserve immune function, prevent the harmful effect of viral replication on possible existing comorbid conditions, and prevent transmission of HIV.
When should ART be initiated?Recommendations
- •
ART should be initiated in all HIV-infected patients to prevent disease progression, reduce viral transmission, and limit any harmful effects on possible co-existing comorbid conditions (Table 1).
Table 1.Indications for ART in patients with chronic HIV infection.a
General recommendation ART should be administered to all HIV-infected patientsb (A-I). aIt is important to evaluate when to initiate ART and the drugs that comprise the initial regimen on an individual basis by weighing up the advantages and disadvantages of each of the options.
The patient's disposition and motivation are critical and should be taken into account when deciding when to start therapy.
- •
Initiation of ART should always be evaluated on an individual basis. Both CD4+ T-lymphocyte count and PVL should be determined before initiating ART. Furthermore, the therapeutic regimen should be adapted to lifestyle, comorbid conditions, and possible drug interactions. The risk of poor adherence should also be assessed (A-III).
Recommendation
- •
Initial ART can be a combination of 2 nucleoside reverse transcriptase inhibitors (NRTI) and 1 INSTI, 2 NRTI and 1 non-nucleoside reverse transcriptase inhibitor (NNRTI), or 2 NRTI and 1 boosted protease inhibitor (PI) (A-I). Preferred antiretroviral drugs are set out in Table 2.
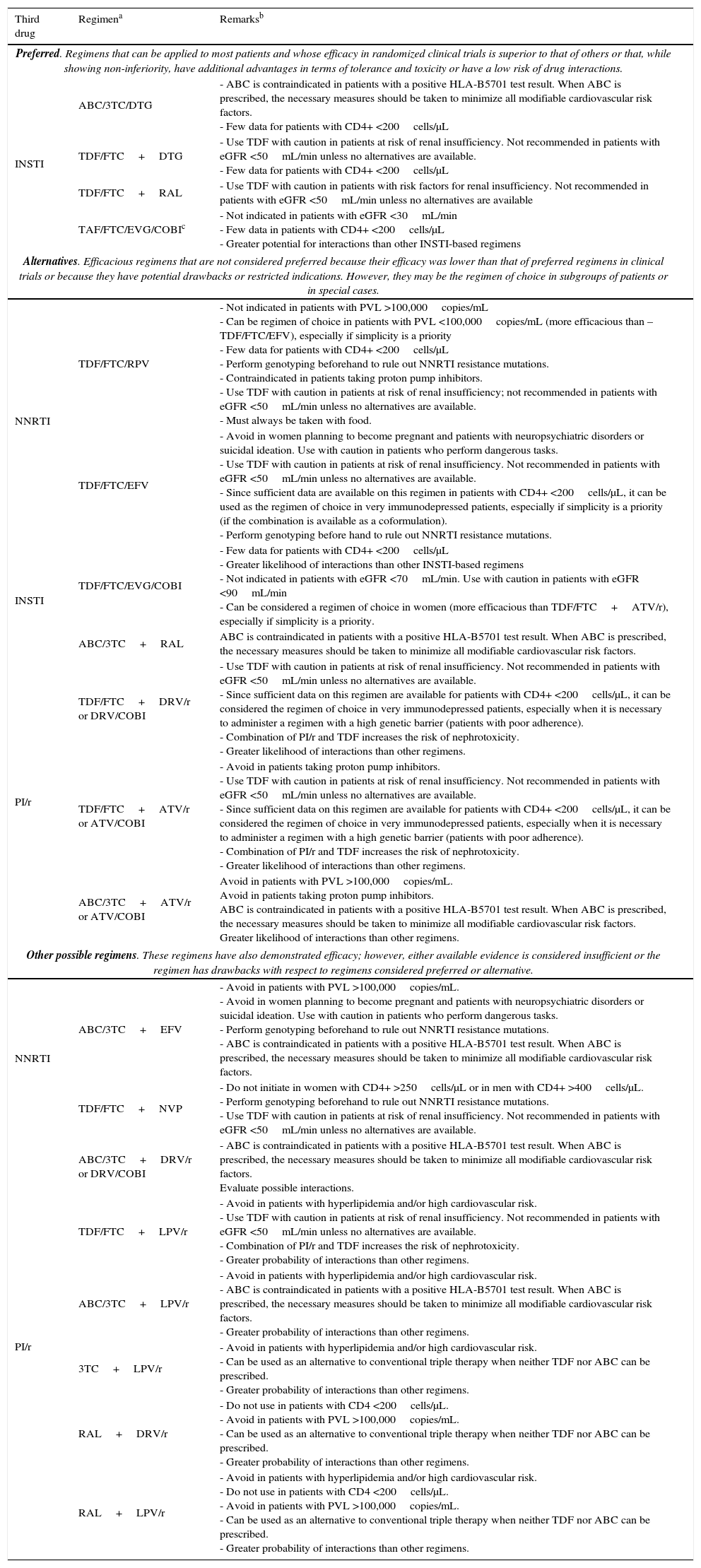
Table 2.Recommended combinations of initial ART.a
Third drug Regimena Remarksb Preferred. Regimens that can be applied to most patients and whose efficacy in randomized clinical trials is superior to that of others or that, while showing non-inferiority, have additional advantages in terms of tolerance and toxicity or have a low risk of drug interactions. INSTI ABC/3TC/DTG - ABC is contraindicated in patients with a positive HLA-B5701 test result. When ABC is prescribed, the necessary measures should be taken to minimize all modifiable cardiovascular risk factors.
- Few data for patients with CD4+ <200cells/μLTDF/FTC+DTG - Use TDF with caution in patients at risk of renal insufficiency. Not recommended in patients with eGFR <50mL/min unless no alternatives are available.
- Few data for patients with CD4+ <200cells/μLTDF/FTC+RAL - Use TDF with caution in patients with risk factors for renal insufficiency. Not recommended in patients with eGFR <50mL/min unless no alternatives are available TAF/FTC/EVG/COBIc - Not indicated in patients with eGFR <30mL/min
- Few data in patients with CD4+ <200cells/μL
- Greater potential for interactions than other INSTI-based regimensAlternatives. Efficacious regimens that are not considered preferred because their efficacy was lower than that of preferred regimens in clinical trials or because they have potential drawbacks or restricted indications. However, they may be the regimen of choice in subgroups of patients or in special cases. NNRTI TDF/FTC/RPV - Not indicated in patients with PVL >100,000copies/mL
- Can be regimen of choice in patients with PVL <100,000copies/mL (more efficacious than – TDF/FTC/EFV), especially if simplicity is a priority
- Few data for patients with CD4+ <200cells/μL
- Perform genotyping beforehand to rule out NNRTI resistance mutations.
- Contraindicated in patients taking proton pump inhibitors.
- Use TDF with caution in patients at risk of renal insufficiency; not recommended in patients with eGFR <50mL/min unless no alternatives are available.
- Must always be taken with food.TDF/FTC/EFV - Avoid in women planning to become pregnant and patients with neuropsychiatric disorders or suicidal ideation. Use with caution in patients who perform dangerous tasks.
- Use TDF with caution in patients at risk of renal insufficiency. Not recommended in patients with eGFR <50mL/min unless no alternatives are available.
- Since sufficient data are available on this regimen in patients with CD4+ <200cells/μL, it can be used as the regimen of choice in very immunodepressed patients, especially if simplicity is a priority (if the combination is available as a coformulation).
- Perform genotyping before hand to rule out NNRTI resistance mutations.INSTI TDF/FTC/EVG/COBI - Few data for patients with CD4+ <200cells/μL
- Greater likelihood of interactions than other INSTI-based regimens
- Not indicated in patients with eGFR <70mL/min. Use with caution in patients with eGFR <90mL/min
- Can be considered a regimen of choice in women (more efficacious than TDF/FTC+ATV/r), especially if simplicity is a priority.ABC/3TC+RAL ABC is contraindicated in patients with a positive HLA-B5701 test result. When ABC is prescribed, the necessary measures should be taken to minimize all modifiable cardiovascular risk factors. PI/r TDF/FTC+DRV/r or DRV/COBI - Use TDF with caution in patients at risk of renal insufficiency. Not recommended in patients with eGFR <50mL/min unless no alternatives are available.
- Since sufficient data on this regimen are available for patients with CD4+ <200cells/μL, it can be considered the regimen of choice in very immunodepressed patients, especially when it is necessary to administer a regimen with a high genetic barrier (patients with poor adherence).
- Combination of PI/r and TDF increases the risk of nephrotoxicity.
- Greater likelihood of interactions than other regimens.TDF/FTC+ATV/r or ATV/COBI - Avoid in patients taking proton pump inhibitors.
- Use TDF with caution in patients at risk of renal insufficiency. Not recommended in patients with eGFR <50mL/min unless no alternatives are available.
- Since sufficient data on this regimen are available for patients with CD4+ <200cells/μL, it can be considered the regimen of choice in very immunodepressed patients, especially when it is necessary to administer a regimen with a high genetic barrier (patients with poor adherence).
- Combination of PI/r and TDF increases the risk of nephrotoxicity.
- Greater likelihood of interactions than other regimens.ABC/3TC+ATV/r or ATV/COBI Avoid in patients with PVL >100,000copies/mL.
Avoid in patients taking proton pump inhibitors.
ABC is contraindicated in patients with a positive HLA-B5701 test result. When ABC is prescribed, the necessary measures should be taken to minimize all modifiable cardiovascular risk factors.
Greater likelihood of interactions than other regimens.Other possible regimens. These regimens have also demonstrated efficacy; however, either available evidence is considered insufficient or the regimen has drawbacks with respect to regimens considered preferred or alternative. NNRTI ABC/3TC+EFV - Avoid in patients with PVL >100,000copies/mL.
- Avoid in women planning to become pregnant and patients with neuropsychiatric disorders or suicidal ideation. Use with caution in patients who perform dangerous tasks.
- Perform genotyping beforehand to rule out NNRTI resistance mutations.
- ABC is contraindicated in patients with a positive HLA-B5701 test result. When ABC is prescribed, the necessary measures should be taken to minimize all modifiable cardiovascular risk factors.TDF/FTC+NVP - Do not initiate in women with CD4+ >250cells/μL or in men with CD4+ >400cells/μL.
- Perform genotyping beforehand to rule out NNRTI resistance mutations.
- Use TDF with caution in patients at risk of renal insufficiency. Not recommended in patients with eGFR <50mL/min unless no alternatives are available.PI/r ABC/3TC+DRV/r or DRV/COBI - ABC is contraindicated in patients with a positive HLA-B5701 test result. When ABC is prescribed, the necessary measures should be taken to minimize all modifiable cardiovascular risk factors.
Evaluate possible interactions.TDF/FTC+LPV/r - Avoid in patients with hyperlipidemia and/or high cardiovascular risk.
- Use TDF with caution in patients at risk of renal insufficiency. Not recommended in patients with eGFR <50mL/min unless no alternatives are available.
- Combination of PI/r and TDF increases the risk of nephrotoxicity.
- Greater probability of interactions than other regimens.ABC/3TC+LPV/r - Avoid in patients with hyperlipidemia and/or high cardiovascular risk.
- ABC is contraindicated in patients with a positive HLA-B5701 test result. When ABC is prescribed, the necessary measures should be taken to minimize all modifiable cardiovascular risk factors.
- Greater probability of interactions than other regimens.3TC+LPV/r - Avoid in patients with hyperlipidemia and/or high cardiovascular risk.
- Can be used as an alternative to conventional triple therapy when neither TDF nor ABC can be prescribed.
- Greater probability of interactions than other regimens.RAL+DRV/r - Do not use in patients with CD4 <200cells/μL.
- Avoid in patients with PVL >100,000copies/mL.
- Can be used as an alternative to conventional triple therapy when neither TDF nor ABC can be prescribed.
- Greater probability of interactions than other regimens.RAL+LPV/r - Avoid in patients with hyperlipidemia and/or high cardiovascular risk.
- Do not use in patients with CD4 <200cells/μL.
- Avoid in patients with PVL >100,000copies/mL.
- Can be used as an alternative to conventional triple therapy when neither TDF nor ABC can be prescribed.
- Greater probability of interactions than other regimens.aWhen available, fixed-dose combinations should be used. There are no data showing that FTC and 3TC can be considered therapeutically equivalent; therefore, use of one or other drug in the regimens selected essentially depends on experience of use in combination with other drugs in the regimen.
The clinical trials on which the evidence for each regimen is based are referenced in the text.
In drugs from the same family and with the same level of recommendation, the order reflects the preference of the expert panel.
bThe remarks reflect aspects that should be taken into consideration when choosing the regimen; they do not aim to be an exhaustive guide to the precautions to be taken when receiving these drugs. Please see the main text and the appropriate Summary of Product Characteristics for more information.
Cost and pricing of the therapeutic regimens are addressed elsewhere in these guidelines. The cost-effectiveness of the regimens is analyzed formally in an article published simultaneously with the guidelines.
The NRTI combinations of choice are considered to be those comprising tenofovir/emtricitabine (TDF/FTC) and those comprising abacavir/lamivudine (ABC/3TC), which should be administered as co-formulated preparations.
Recommendations
- •
The NRTI combinations of choice for initial regimens are TDF/FTC and ABC/3TC (AI).
- •
Co-formulated preparations are recommended (A-II).
- •
TDF/FTC should be used with caution in patients with renal insufficiency (A-II).
- •
ABC/3TC should be used with caution in patients with a high PVL (>100,000copies/mL) when combined with an NNRTI or a PI/r other than LPV/r (A-II).
Recommendations
- •
The combination efavirenz (EFV)/TDF/FTC is considered an alternative option (A-I).
- •
The combination EFV+ABC/3TC should be avoided in patients with a PVL >100,000copies/mL (B-I).
- •
EFV is contraindicated during the first trimester of pregnancy. Other options are recommended in women who do not use effective contraception. Similarly, EFV should be avoided in patients with neuropsychiatric disorders or a history of suicidal ideation and in patients who perform dangerous tasks if they present symptoms of somnolence, dizziness, and/or difficulty concentrating (A-III).
- •
Nevirapine (NVP) is contraindicated in women with CD4+ T-lymphocyte counts >250cells/μL and in men with >400cells/μL (A-II).
- •
Rilpivirine (RPV) should not be administered to patients with a PVL >100,000copies/mL (A-II).
- •
The combination RPV/TDF/FTC can be considered a preferred regimen in patients with a PVL <100,000copies/mL (A-I).
Recommendations
- •
The recommended PI-based regimens are DRV/r or DRV/COBI QD+TDF/FTC and ATV/r or ATV/COBI QD+TDF/FTC (A-I). The combination of ATV/r or ATV/COBI+ABC/3TC is also recommended, although it should be avoided in patients with a PVL >100,000copies/mL (A-I).
- •
Other PI-based regimens include LPV/r (BID or QD)+TDF/FTC or ABC/3TC (B-I). The combination DRV/r (or DRV/COBI)+ABC/3TC can also be used, although it has not been formally assessed in a clinical trial (B-III).
- •
ATV and DRV can be boosted interchangeably with ritonavir (RTV) 100mg or COBI 150mg (B-II).
- •
LPV/r+3TC, LPV/r+RAL, and DRV/r+RAL can be used as an alternative to conventional triple therapy when it is not possible to use TDF or ABC (B-I). NRTI-sparing double regimens (DRV/r or LPV/r+RAL) should not be used as initial treatment in patients with advanced disease (CD4+ T-lymphocyte counts <200cells/μL and/or a PVL >100,000copies/mL) (A-I).
Recommendations
- •
Dolutegravir (DTG) combined with TDF/FTC or coformulated with ABC/3TC, raltegravir (RAL) combined with TDF/FTC, and elvitegravir (EVG) coformulated with COBI/TAF/FTC are considered preferred regimens for initial treatment (A-I).
- •
The combination EVG/COBI/tenofovir alafenamide (TAF)/FTC is preferred over EVG/COBI/TDF/FTC owing to its better tolerability profile and the possibility of administering it with estimated glomerular filtration rate (eGFR) >30mL/min (A-I).
- •
The combination EVG/COBI/TDF/FTC can be used as initial ART, although it should not be used in patients with an estimated glomerular filtration rate <70mL/min) (A-I).
- •
In women, EVG/COBI/TDF/FTC is considered a preferred regimen (A-I).
- •
The combination of RAL with ABC/3TC is considered an alternative in initial treatment because less evidence is available (A-I).
PVL is considered undetectable at <50copies/mL. Most clinical trials on switching ART included patients who have maintained virological suppression at this level for at least 6 months.
There are several reasons for changing an efficacious ART regimen (e.g., tolerance, toxicity, comorbid conditions, drug interactions, and reducing the pill burden or number of daily doses). However, efficacious ART always has the common and priority objective of maintaining an undetectable PVL. Efficacious ART can be switched in 2 ways: proactively, which is recommended when attempting to prevent a severe or incurable adverse event, and reactively, which is mandatory in the case of an adverse effect.
After switching ART in this context, maintenance of virological suppression and performance of relevant laboratory tests should be evaluated within 3–6 weeks.
Virological considerations when switching efficacious ARTRecommendation
- •
Switching from a regimen containing 2 NRTI+PI/r to one containing 2 NRTI+1 NNRTI, 1 INSTI or unboosted ATV is only possible if the antiviral activity of the 2 NRTI and third drug can be guaranteed (A-I). Without forgetting that the main objective is to maintain virological suppression, the physician should carry out a meticulous evaluation of the toxicity profile, interactions, dietary restrictions, and anti-HBV activity (where necessary) of the new regimen.
(a) NRTI
Switching stavudine (d4T) or zidovudine (ZDV) for TDF or ABC
Recommendation
- •
Proactive switch from d4T or ZDV to TDF or ABC in order to prevent or try to reverse lipoatrophy associated with thymidine analogs (A-I).
Switching from ABC/3TC to TDF/FTC
Recommendation
- •
The association between ABC and increased incidence of cardiovascular events is open to debate. This committee cannot make a recommendation on the strength of evidence for switching from ABC/3TC to TDF/FTC.
Switching from TDF to ABC
Recommendation
- •
The switch from TDF to ABC is a valid option in patients with osteopenia or osteoporosis associated with TDF, as long as the results of HLA-B*5701 testing are negative (A-II).
(b) NNRTI
Switching from EFV/TDF/FTC to RPV/TDF/FTC
Recommendation
- •
In patients with adverse central nervous system (CNS) effects caused by EFV/TDF/FTC, the switch to RPV/TDF/FTC is one of the options that can improve the symptoms associated with EFV (A-II). There are no data in favor of recommending a proactive switch in patients who do not have CNS symptoms or data comparing this switch with a switch to other antiretroviral drugs that do not cause CNS effects.
Switching from EFV to etravirine (ETV)
Recommendation
- •
In patients with CNS adverse effects caused by EFV, the switch to ETV can lead to an improvement in EFV-associated neuropsychological symptoms (A-II). There are no data to recommend a proactive switch in patients who do not have CNS symptoms or data comparing this switch with a switch to other antiretroviral drugs that do not cause CNS effects.
Switching from EFV to NVP
Recommendation
- •
In patients with CNS adverse effects caused by EFV, switching to NVP could improve EFV-associated neuropsychological symptoms (A-II). There are no data to recommend a proactive switch in patients who do not have CNS symptoms or data comparing this switch with a switch to other antiretroviral drugs that do not cause CNS effects. Switching is also an option in patients with high LDL cholesterol induced by EFV (A-II).
Switching from EFV or NVP+2 NRTI to EFV/TDF/FTC
Recommendation
- •
Switching to EFV/TDF/FTC is an option in patients taking ART with EFV and NVP who wish to reduce their pill burden (A-II).
Switching from ATV/r+ABC/3TC to unboosted ATV+ABC/3TC
Recommendation
- •
In patients taking ATV/r+ABC/3TC, switching to ATV+ABC/3TC is a simplification option when attempting to avoid RTV, owing to hyperbilirubinemia, dyslipidemia, diarrhea, or the risk of interactions with RTV (A-I).
Switching from ATV/r+TDF/FTC to unboosted ATV+ABC/3TC
Recommendation
- •
In patients taking ATV/r+TDF/FTC, switching to ATV+ABC/3TC is an option in those cases where both TDF and RTV have to be avoided (A-II).
(a) Switching from NRTI to INSTI
Switching from TDF to RAL
Recommendation
- •
Switching from TDF to RAL in patients who are also taking a PI/r is also an option in patients with reduced bone mineral density (A-II).
(b) Switching from NNRTI to INSTI
Switching from EFV to RAL
Recommendation
- •
Switching from EFV to RAL is an option in patients with CNS adverse events caused by EFV (A-II). There are no data to recommend a proactive change in patients with no CNS symptoms or data comparing this switch with a switch to other antiretroviral drugs that do not cause CNS effects.
- •
Switching from EFV to RAL is a valid option in patients with dyslipidemia caused by EFV (A-I).
Switching from TDF/FTC+EFV or NVP to TDF/FTC/COBI/EVG
Recommendation
- •
Switching from TDF/FTC+EFV or NVP to coformulated TDF/FTC/COB/EVG is virologically safe. This change is an option for patients who wish to simplify their current regimen and can improve CNS symptoms caused by EFV (A-I). There are no data to recommend a proactive change in patients who do not have CNS symptoms. Similarly, there are no data comparing this switch with switches to other drugs that do not cause CNS symptoms.
(c) Switching from fusion inhibitors to INSTI
Switching from enfuvirtide (ENF) to RAL
Recommendation
- •
Switching from ENF to RAL is a safe option that obviates parenteral administration of ENF (A-I).
(d) Switching from a PI to an NNRTI
Switching from a PI/r to EFV/TDF/FTC
Recommendation
- •
Switching to EFV/TDF/FTC is an option in patients who are taking ART with PI/r. This approach makes it possible to reduce the daily pill burden, although patients may experience EFV-induced CNS adverse effects (B-I).
Switching from PI/r to NVP
Recommendation
- •
Switching from a PI to NVP could be an option in patients taking a PI/r in order to avoid the adverse effects of RTV (B-III).
Switching from PI/r to RPV/TDF/FTC
Recommendation
- •
Switching from an ART regimen comprising 2 NRTI and 1 PI/r to the co-formulation RPV/TDF/FTC is a valid option in patients with gastrointestinal disorders or dyslipidemia. It also enables the daily pill burden to be reduced (A-I).
(e) Switching from PI/r to INSTI
Switching from PI/r to RAL
Recommendation
- •
Switching to RAL+2 active NRTI is a valid option for patients with dyslipidemia taking ART with NRTI+1 PI/r (B-I).
Switching from PI/r to TDF/FTC/COBI/EVG
Recommendation
- •
Switching from TDF/FTC+ATV/r or DRV/r or LPV/r to TDF/FTC/COBI/EVG is virologically better than the previous options. This switch is an option for patients who wish to simplify their current regimen and can improve RTV-associated digestive symptoms in some patients (A-I).
(f) Switching to TAF/FTC/COBI/EVG from TDF-containing regimens
Recommendation
- •
Switching from TDF/FTC/COBI/EVG, TDF/FTC/EFV, or TDF/FTC-ATV/r to TAF/FTC/COBI/EVG is virologically safe in patients whose virus remains sensitive to all the components in the regimen. This change is also associated with improved bone mineral density and kidney function. The switch is even feasible in patients with mild or moderate kidney failure (A-I).
(g) Switching to ABC/3TC/DTG from regimens containing 2 NRTI and PI, NNRTI, or INSTI
Recommendation
- •
Switching to ABC/3TC/DTG from regimens containing 2 NRTI and PI, NNRTI, or INSTI is virologically safe. This switch is an option in patients who wish to simplify their current regimen.
Switching 2 NRTI and ATV/r or LPV/r to 3TC+ATV/r or 3TC+LPV/r
Recommendation
- •
Switching from 2 NRTI+ATV/r or LPV/r to dual therapy with 3TC+ATV/r or 3TC+LPV/r is an option if the clinician wishes to avoid or prevent the adverse effects caused by NRTI. This option requires the patient to fulfill the following criteria: (1) No chronic hepatitis B; (2) PVL <50copies/mL for at least 6 months; and (3) No mutations in the protease gene or previous virological failure to PI/r or 3TC (A-I).
Recommendation
- •
Monotherapy with DRV/r once daily or LPV/r twice daily is a valid option for preventing adverse effects caused by NRTI if the patient fulfills the following criteria: (1) No chronic hepatitis B; (2) PVL <50copies/mL for at least 6 months; (3) No mutations in the protease gene and no previous virological failure with PI (B-I).
1. Definitions
Virological failure. Two confirmed determinations of PVL >50copies/mL 24 weeks after initiating ART.
Transient rebound of low-level viremia (“blips”). Isolated and transient increase in PVL (50–200copies/mL) after virological suppression.
Immunological failure. Inability to reach an adequate CD4+ T-lymphocyte count despite maintaining a PVL <50copies/mL.2. Determinants of virological failure
The determinants of virological failure can be patient-dependent (adherence), drug-dependent (dosing errors, potency, genetic barrier, inadequate plasma concentrations, drug or food interactions), and HIV-dependent (pre-existing resistance mutations to any of the drugs in the current ART regimen).3. Objective of ART after virological failure
The objective of ART is to achieve maintained viral suppression. Therefore, a new regimen should be started with 3 or at least 2 active antiretroviral drugs. Rescue ART should not be delayed in order to prevent the accumulation of resistance mutations, increased PVL, and impairment of the immune system.4. Strategies for improving the success of rescue ART regimens
The measures to be taken when prescribing rescue ART are as follows: facilitating adherence, determining resistance mutations and viral tropism, reviewing previous therapy, and occasional monitoring of plasma concentrations of antiretroviral drugs.5. Clinical scenarios in virological failure
5.1. Virological failure with low viral loads
- (a)
PVL between 50 and 200copies/mL. It is generally not recommended to modify ART, although some studies have demonstrated selection of new resistance mutations and an association between bacterial translocation and systemic inflammation.
- (b)
PVL between 200 and 1000copies/mL. This level is associated with selection of resistance mutations. Resistance testing should be performed and a rescue regimen designed bearing in mind resistance mutations, previous virological failure, problems with adherence, toxicity, the risk of interactions, and ease of administration of antiretroviral therapy. Intensification of ART by adding a single active drug is contraindicated in these situations.
5.2. Early virological failure
Early virological failure occurs after the first line of ART. Selection of resistance mutations and second-line regimens differs according to the initial ART regimen applied.
- (a)
Virological failure to 2 NRTI+NNRTI: The most common resistance mutations after virological failure with EFV or NVP are K103N, L100I, and Y181C. K103N alone maintains sensitivity to RPV and ETV. Virological failure with RPV leads more frequently to selection of E138K and/or Y181C, which generate resistance to all the NNRTI. Virological failure to NNRTI may be accompanied by resistance mutations to NRTI, especially that caused by M184V and, albeit less frequently, K65R.
- (b)
Virological failure to 2 NRTI+PI/r: The probability of resistance to PI is very low. PI/r protect against resistance to NRTI, which is uncommon. The only mutation involved is M184V.
- (c)
Virological failure to 2 NNRTI+INSTI: Virological failure to RAL or EVG leads to cross-resistance between both drugs. The mutations involved are T66K, E92Q, Q148H/K/R, and N155H. In this setting resistance to NRTI is frequent. Clinical trials involving naïve patients have shown that DTG has a high genetic barrier, with the result that resistance mutations are exceptionally detected in the integrase gene or reverse transcriptase gene after virological failure to DTG.
It is generally recommended to use a PI/r with 2 antiretroviral drugs, preferably NRTI, that conserve their antiviral activity. DRV/r is the most efficacious PI/r of all the rescue lines analyzed.
In patients whose first NNRTI-based ART regimen (ie, one based on NVP or EFV) fails, a dual regimen with LPV/r+RAL is not inferior to LPV/r+2 or 3 NRTI (SECOND LINE study). Joint therapy with boosted PI+RAL could be an option in patients who require an NRTI-sparing regimen.
5.3. Advanced virological failure
Advanced rescue therapy is a rescue regimen that is administered when virological failure has occurred with at least 2 ART lines. A regimen comprising 3 or at least 2 active antiretroviral drugs can be designed by combining drugs from different families. In this setting, DRV/r is superior to other PI/r and should be included in most rescue regimens. DTG at 50mg BID is efficacious in most patients with resistance to RAL and EVG.
5.4. Virological failure in patients with no therapeutic options
In patients with no therapeutic options, it is impossible to design an ART regimen with a minimum of 2 fully active antiretroviral drugs. Most patients continue to have relatively stable CD4+ T-lymphocyte counts. ART should not be suspended. The ART regimen should be non-suppressive and easy to take, with minimum toxicity. It should also be able to reduce viral replicative capacity and not generate resistance mutations. Furthermore, the patient should be referred to a specialized center with experience in treating this population and where access to new antiretroviral drugs is provided through clinical trials or expanded-access studies.
Recommendations (switching ART because of virological failure)
- •
The objective of rescue ART is to achieve a PVL <50copies/mL (A-II).
- •
Switching ART because of virological failure should be performed early to avoid accumulation of mutations and to facilitate the response to the new treatment (A-III).
- •
The new ART regimen should contain 3 totally active antiretroviral drugs. If this is not possible, 2 fully active drugs should be combined with other drugs that maintain partial virological activity, especially in the case of advanced rescue in patients with limited therapeutic options (A-I). Regimens with only 2 active antiretroviral drugs based on a boosted PI may be a reasonable option in patients who have experienced a non-advanced failure when it is not possible to use NRTI or construct a simple regimen with 3 active drugs (A-I).
- •
Resistance and viral tropisms should be assessed in order to design the best alternative regimen. The test should be performed while the patient is receiving the failed treatment or as soon as possible after suspension of the failed treatment. If the results of previous genotyping tests are available, all the resistance mutations detected should be evaluated (A-I).
- •
The causes of virological failure – poor adherence, drug or food interactions, previous therapy, and previous toxicity – should be analyzed. The new regimen should be comfortable and well tolerated (A-III).
- •
In patients who have experienced virological failure, DRV/r is the PI/r that has proven most efficacious in all the rescue lines. When major resistance mutations are present, the recommended dose is 600/100mg BID (A-I).
- •
DTG is the INSTI of choice in patients who experience virological failure who are INSTI-naïve (A-I). In the case of previous failure to RAL or EVG, the dose of DTG should be 50mg BID, accompanied by optimized background therapy (A-II).
- •
The use of tipranavir/ritonavir (TPV/r), ENF, or thymidine analogs is restricted to patients with no other therapeutic options (A-III).
- •
In patients with low-grade virological failure (PVL detectable but ≤200copies/mL), genotyping can be performed with a 2–3mL plasma sample (A-II). If genotyping does not reveal resistance mutations, an ART regimen with a high barrier to resistance should be maintained. In patients with a PVL >200copies/mL, genotyping should be performed. The choice of the new ART regimen should be based on both resistance mutations and previous ART. ART should not be intensified with a single drug (A-III).
- •
ART should not be suspended in patients with advanced virological failure and no therapeutic options (A-II). In this situation, the approach should involve antiretroviral drugs that reduce viral replicative capacity and do not lead to resistance mutations that might compromise future treatments (A-III).
- •
In patients with no therapeutic options, it is important to monitor the CD4+ count and PVL and to consult with clinicians and virologists specialized in resistance and rescue therapy who are involved in restricted access programs (B-III).
Adherence to ART is the patient's ability to become suitably involved in the choice, initiation, and completion of his/her treatment in order to achieve an undetectable PVL.
Recommendations
- •
Before initiating ART, the patient should be prepared and factors likely to limit adherence should be identified and corrected (A-III).
- •
Once ART has been initiated, a first check-up should be made after 2–4 weeks to verify adherence and correct adherence problems if necessary (A-III).
- •
Adherence should be monitored and reinforced at visits to the doctor (A-III).
- •
Adherence should be monitored by a multidisciplinary team including a doctor, nursing staff, specialists in psychological support, and a hospital pharmacist (A-III).
- •
In the case of patients whose adherence is irregular, it is preferable to use regimens based on boosted PI in order to prevent the development of resistance (A-III).
- •
Using fixed dose combinations of antiretroviral drugs simplifies ART and thus facilitates continued adherence. The use of whole regimens in a single tablet is the most efficient strategy for preventing selective poor adherence (A-II).
Tolerability depends on drug-related factors (number and size of tablets, administration requirements, and number and intensity of immediate side effects) and patient-related factors (age, sex, weight, clinical situation, and expectations from treatment).
(a) Immediate adverse effects
The immediate adverse effects are well defined. In some cases, these can be anticipated and are usually easy to control. Adverse effects are usually gastrointestinal, cutaneous, or neuropsychological.
Recommendations
- •
Avoid the use of antiretroviral drugs whose immediate adverse effects are similar to clinical manifestations or laboratory abnormalities that are already present in a specific patient (A-II). HLA-B*5701 testing is mandatory before prescribing ABC, since it has a negative predictive value of almost 100% for the risk of hypersensitivity reaction to this drug (A-I).
- •
The patient should be informed about the correct way to take an ART regimen and the possibility of immediate adverse events. In any case, the patient should be told how to deal with specific adverse events and always be able to contact the doctor directly. Mild immediate adverse events can be treated symptomatically by evaluating the patient's progress and tolerability. If the adverse effect is very intense or long-lasting or cannot be tolerated by the patient, the potential culprit antiretroviral drug(s) should be switched (A-I).
(b) Late adverse effects
Late adverse effects are worse and more difficult to prevent and control. They exacerbate the symptoms of chronic diseases associated with aging and affect the functioning of organs and systems. In general, the absolute risk of late adverse effects of currently recommended antiretroviral drugs is very small.
Recommendations
- •
ART should be tailored by evaluating the risk or presence of chronic diseases in such a way that the regimen selected does not contain antiretroviral drugs that can favor the onset or progression of these diseases (A-II).
- •
Withdrawal of some of the antiretroviral drugs involved in late adverse effects can improve – albeit partially – the underlying clinical abnormality, although it is not known whether such a modification can alter the natural history of the specific chronic disease or survival. Antiretroviral drugs contribute collaterally to the risk or progression of specific chronic diseases, although other factors are generally considered to be more important. Priority should be given to interventions to address these factors (A-II).
Interactions between antiretroviral drugs or between antiretroviral drugs and other agents, food, herbal products, and recreational drugs could have significant clinical consequences.
Recommendations
- •
All medications, natural products, and alternative medicines taken by the patient should be recorded in the clinical history in order to evaluate potential interactions (A-III).
- •
Contraindications should be taken into account and the corresponding dose adjustments made where necessary (A-I).
- •
Plasma levels should be monitored when prescribing 2 or more drugs with potential pharmacokinetic interactions in order to avoid toxicity or lack of efficacy (A-II).
In more than 50% of cases, acute HIV infection is characterized by self-limiting acute febrile syndrome similar to influenza or infectious mononucleosis. Acute infection (first 30 days) should not be confused with recent infection (patients diagnosed during the previous 6 months).
Recommendations
- •
ART should be recommended in all patients with acute HIV infection, regardless of the symptoms, their severity, or their duration (A-II) and should be started as soon as possible to obtain the maximum benefit.
- •
ART should generally be offered to all recently infected patients (B-II).
- •
ART should be initiated when acute HIV infection is detected during pregnancy (A-I).
- •
If ART is to be initiated, it should be done so with the same preferential regimens used to treat chronic HIV infection (A-I) (Table 2). A regimen comprising 2 NRTI and an INSTI could reduce PVL more rapidly during the first 4–8 weeks than PI or NNRTI and, thus, make it easier to reduce transmission of HIV (A-I). The combination of DTG or RAL+2 NRTI (preferably TDF/FTC) would also have the advantage of reaching higher concentrations in genital tract secretions (B-III).
- •
Testing for resistance and viral tropism should always be performed at diagnosis of acute or recent infection, irrespective of whether ART is to be initiated (A-II).
- •
If the results of resistance testing are not available, it is preferable to begin with a regimen based on a PI/r until the results become available (A-II).
- •
If is ART is initiated, it should be administered indefinitely (A-I).
The genomic organization of HIV-2 is similar to that of HIV-1, except for certain structural differences that can significantly affect its pathogenicity and its sensitivity to antiretroviral drugs.
Recommendations
- •
The general principles of ART in patients infected by HIV-2 should be the same as those of HIV-1 infection (A-III).
- •
The preferred regimen for initial ART in these patients is the combination of 2 NRTI and 1 boosted PI or an INSTI (A-III).
- •
The use of NNRTI, MVC, or ENF is not indicated for the treatment of HIV-2 infection (A-I).
A specific GESIDA document and documents from other scientific societies on women and pregnancy are available. The most important recommendations are summarized below.
Recommendations
- •
All pregnant women must undergo HIV serology testing (A-I). If the result is negative, testing must be repeated during the third trimester (A-II).
- •
Pre-pregnancy counseling must form part of health care for HIV-infected women of childbearing age and should include a recommendation for ART so that the woman can become pregnant with an undetectable PVL (A-II).
- •
ART is indicated in all pregnant women, irrespective of CD4+ T-lymphocyte count and PVL, in order to ensure that PVL remains undetectable (A-I).
- •
The choice of specific antiretroviral drugs should be based on resistance studies, drug safety, and ease of adherence. If there are no resistance mutations, the regimen of choice is ZDV or TDF or ABC+3TC or FTC+LPV/r or ATV/r (A-I); if resistance mutations are detected, patients can receive any of the “preferential” and “alternative” antiretroviral drugs after a personalized evaluation (A-III).
- •
Intrapartum intravenous administration of ZDV is only indicated in women whose PVL is >1000copies/mL or unknown at the time of delivery, irrespective of any previous ART received (A-I).
- •
Elective cesarean delivery is indicated at week 38 in women with a pre-labor PVL of >1000copies/mL (A-II).
- •
Mothers cannot breastfeed. Adapted formula food must be used (A-I).
- (a)
Initial ART in patients with opportunistic infections other than tuberculosis
Recommendations
- •
In most opportunistic infections (except tuberculosis and cryptococcal meningitis), ART should be started as soon as possible (preferably within the first 15 days after starting treatment for the infection) (A-II).
- •
Patients with Pneumocystis jiroveci pneumonia who are not receiving ART, should start ART during the 2 weeks following the diagnosis of Pneumocystis jiroveci pneumonia (A-I).
- •
In patients with cryptococcal meningitis, initiation of ART should be deferred for 5 weeks because of the greater risk of death associated with early initiation (especially in patients with <5cells/μL in CSF or increased intracranial pressure) (A-I).
- •
- (b)
ART and tuberculosis
Treatment of tuberculosis in HIV-infected adults was the subject of a consensus document from GESIDA/Secretariat of the National AIDS Plan, which is available for consultation.
Optimal timing of ART
Recommendations
- •
ART should always be started during treatment of tuberculosis, irrespective of the CD4+ T-lymphocyte count, since it reduces the risk of death (A-I).
- •
The optimal time for initiating ART depends on the CD4+ T-lymphocyte count. If the CD4+ T-lymphocyte count is <50cells/μL, ART should be started as soon as possible, after verifying tolerance to anti-tuberculosis treatment, but not later than the first 2 weeks (A-I). If the CD4+ T-lymphocyte count is >50cells/μL, initiation of ART can be delayed until the intense phase of anti-tuberculosis treatment has been completed (8 weeks). This approach reduces the risk of adverse effects and the development of immune reconstitution inflammatory syndrome (IRIS) without compromising survival (A-I).
ART regimens
Drug interactions constitute the main difficulty when attempting to treat tuberculosis and HIV infection simultaneously.
Recommendations
- •
Choice of NRTI: No significant interactions or evidence of toxicity have been found between antituberculosis drugs and NRTI. Therefore, ABC, TDF, 3TC, and FTC can be used in these patients with no added risks (A-I).
- •
Choice of the third drug. Since most experience and the best results have been obtained with EFV, this is the antiretroviral drug of choice (A-I). The dose of EFV is standard for all patients (600mg/d), irrespective of body weight and with no need to increase to 800mg/d (A-I).
- •
Alternative third drugs. Based on experience or sufficient evidence, the alternative regimens that can be recommended include NVP at habitual doses (A-II) and RAL at 800mg/12h (A-II), although 400mg/12h has proven to be efficacious, as has MVC at 600mg/12h (A-III). Despite the absence of clinical data, the results of pharmacokinetic studies show that DTG can be administered with rifampicin at 50mg/12h (A-III).
- •
Drugs that cannot be used. The other NNRTI (RPV and ETV), PI (whether boosted or not with RTV or COBI), and EVG should not be co-administered with rifampicin. In the exceptional case of a PI being the only option for ART, rifampicin should be replaced by rifabutin and the corresponding adjustment in drug doses should be made (A-II).
Immune reconstitution inflammatory syndrome (IRIS)
IRIS is a frequent complication, especially in patients with a very low CD4+ T-lymphocyte count and when ART is initiated very early with respect to anti-tuberculosis treatment.
Recommendations
- •
If the patient develops IRIS, neither ART nor anti-tuberculosis medication should be interrupted (A-III).
- •
The symptoms of IRIS can by managed by adding non-steroidal anti-inflammatory drugs in mild to moderate cases (A-III) or corticosteroids in moderate to severe forms (A-II).
- •
- (c)
Renal insufficiency
For a complete overview of the diagnosis, prevention, and treatment of renal disorders in HIV-infected patients, please consult the ad hoc consensus document drafted by GESIDA, the SEN, and the SEQC.
Recommendations
- •
It is necessary to adjust the dose of NRTI, except for ABC (A-II).
- •
No dose adjustment is required for NNRTI, PI, ENF, RAL, or DTG (A-II).
- •
The dose of MVC should be adjusted if it is used in combination with potent CYP3A4 inhibitors such as PI (except TPV/r), ketoconazole, itraconazole, clarithromycin, and telithromycin (A-II).
- •
Co-formulations of antiretroviral drugs are not advised in patients with significant renal insufficiency. The co-formulation TDF/FTC/COBI/EVG should not be used in patients with an eGFR <70mL/min. The co-formulations TDF/FTC/EFV, TDF/FTC/RPV, and ABC/FTC/DTG should not be used in patients with eGFR <50mL/min. The co-formulation TAF/FTC/COBI/EVG should not be used in patients with eGFR <30mL/min. In these cases, antiretroviral drugs should be administered separately and the appropriate adjustments made (B-III).
- •
In patients with renal insufficiency (any stage), kidney function should be closely monitored and nephrotoxic drugs avoided (A-III).
- •
In patients with advanced chronic renal insufficiency, the dose should be adjusted according to the recommendations of the summary of product characteristics, taking into account possible drug interactions, which are more common and more dangerous in this situation (A-II). In the absence of contraindications, the combination of ABC+3TC (adjusted for eGFR) with an NNRTI or a non-boosted INSTI (DTG or RAL) or DRV/r can be used (A-III).
- •
- (d)
Liver disease (HCV, HBV, cirrhosis)
Initiation of ART
Recommendations
- •
Patients co-infected with HCV should initiate ART irrespective of their CD4+ T lymphocyte count (A-I).
- •
In patients who require treatment for hepatitis C, it is generally preferable to initiate ART before starting treatment for HCV infection (A-III).
- •
Patients co-infected with HBV for whom treatment of HBV infection is indicated should initiate ART containing TDF and FTC or 3TC (A-I).
Choice of antiretroviral drugs
The choice of antiretroviral drugs must be made taking into account potential liver toxicity, presence of cirrhosis, HBV co-infection, and the need for simultaneous treatment of HCV.
Recommendations
- •
Any antiretroviral drug can be used in patients with chronic liver disease and normal liver function, including patients with cirrhosis (Child–Pugh, class A) (A-I), although it seems reasonable to avoid dideoxynucleoside drugs (A-III).
- •
In patients with hepatocellular insufficiency, unboosted INSTI do not require dose adjustments and are the drugs of choice (A-I). Boosted PI have a greater therapeutic margin than NNRTI (A-II).
- •
With the exception of sofosbuvir, currently used DAA (simeprevir, daclatasvir, ledipasvir, paritaprevir, ombitasvir, and dasabuvir) present significant pharmacokinetic interactions with antiretroviral drugs that may require doses to be adjusted or coadministration to be contraindicated (A-I).
- •
An updated pharmacologic interaction software package should be used before prescribing a DAA-containing regimen in a patient on ART.
- •
- (e)
Cancer
Please refer to the relevant GESIDA documents for complete information on cancer in HIV-infected patients.
Recommendations
- •
ART is an essential component of the treatment of HIV-infected patients with Kaposi sarcoma or non-Hodgkin lymphoma (A-II).
- •
Patients with other types of cancer who are not receiving ART should initiate therapy as soon as possible (A-II).
- •
Given its pharmacological characteristics, excellent tolerance, and minimal interactions, RAL should be the antiretroviral drug of choice, where possible, in patients receiving chemotherapy (A-III). DTG can be considered in cases of resistance to RAL (C-III).
- •
ART is expensive, and in a setting where resources are limited, budgets must be managed appropriately. There are major differences in cost between the various combinations used for initial ART. A pharmaco-economic evaluation must take into account not only the cost of ART, but also its efficiency. Therefore, together with the present consensus document, GESIDA has published a pharmaco-economic study in which the cost-effectiveness of the recommended preferred and alternative regimens is evaluated. Please consult the relevant document.
Recommendation
- •
Cost-effectiveness criteria should be taken into account when deciding on initial ART (A-III).
This consensus document was drafted without grant aid or other funding, whether collective or individual, from any private institutions. The conflicts of interest not associated with this document declared by the Members of the Editorial Board are set out below.
Koldo Aguirrebengoa has acted as a consultant for AbbVie, Gilead Sciences, and Janssen. He has participated in clinical studies and trials carried out by AbbVie, Merck Sharp & Dohme, Gilead, Janssen, and ViiV Healthcare and has received payment for talks from AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare.
Antonio Antela has received payment for participating in consultancy meetings, acting as a researcher in clinical trials, and speaking at meetings or symposia from AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, and ViiV Healthcare.
José R. Arribas has acted as a consultant for AbbVie Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, Tobira, and ViiV Healthcare. He has received grant support for clinical research from Janssen, Merck Sharp & Dohme, and Gilead and payment for talks from AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare.
Victor Asensi has acted as a consultant for AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, and ViiV Healthcare and has received payment for talks from AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare. He has also received research grants from Janssen.
Juan Berenguer has acted as a consultant for AbbVie, Bristol-Myers Squibb, Gilead, Janssen, Janssen Therapeutics, Merck, and ViiV Health care. He has received clinical research grant support from Bristol-Myers Squibb, Merck Sharp & Dohme, and ViiV Health care and payment for talks from AbbVie, Bristol-Myers Squibb, Gilead, Janssen, Merck Sharp & Dohme, and ViiV Health care.
José R. Blanco has acted as a consultant for AbbVie, Boehringer-Ingelheim, Bristol-Myers Squibb, Gilead Sciences, GlaxoSmithKline, Janssen, Merck, and ViiV Healthcare. He has received payment for talks from AbbVie, Boehringer-Ingelheim, Bristol-Myers Squibb, Gilead Sciences, GlaxoSmithKline, Janssen, Merck Sharp & Dohme, and ViiV Healthcare and for preparation of training presentations for Gilead Sciences and Bristol-Myers Squibb.
Vicente Boix has acted as a consultant for AbbVie, Bristol-Myers Squibb, Boehringer Ingelheim, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare and has received payments for talks from AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare.
José Luis Casado has acted as a consultant for AbbVie and ViiV Healthcare. He has received payment for talks from AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare and has received clinical research grants from Janssen, Gilead Sciences, and ViiV Healthcare.
Bonaventura Clotet has acted as a consultant, participated in clinical trials, and given paid talks for BMS, AbbVie, Gilead, Janssen, Merck Sharp & Dohme, and ViiV Healthcare.
Manuel Crespo has acted as a consultant for AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare and has received clinical research grants from Gilead Sciences and ViiV Healthcare. He has received payment for talks from AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare and for developing training presentations from Bristol-Myers Squibb, Gilead Sciences, and ViiV Healthcare.
Pere Domingo has acted as a consultant for AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, and ViiV Healthcare. He has received clinical research grant support from AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, and ViiV Healthcare and payment for talks from AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, and ViiV Healthcare.
Carlos Dueñas has acted as a consultant for Gilead Sciences and Janssen. He has received payment for talks from AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare.
Vicente Estrada has acted as a consultant for AbbVie, Gilead Sciences, and Janssen. He has received clinical research grant support from AbbVie, Boehringer Ingelheim, Gilead Sciences, and Janssen and payment for talks from AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare.
Federico García has acted as a consultant for and received payment for talks from Gilead Sciences, ViiV Healthcare, AbbVie, and Roche Diagnostics.
José M. Gatell has acted as a consultant for AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, GlaxoSmithKline, Merck Sharp & Dohme, and ViiV Healthcare. He has received clinical research grant support from AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, GlaxoSmithKline, Merck Sharp & Dohme, and ViiV Healthcare and payment for talks from AbbVie, Bristol-Myers Squibb, Gilead Sciences, GlaxoSmithKline, Merck Sharp & Dohme, ViiV Healthcare.
Juan Luis Gómez Sirvent has acted as a consultant for AbbVie, Boehringer Ingelheim, and Bristol-Myers Squibb. He has also participated in clinical trials and studies sponsored by AbbVie, Boehringer Ingelheim, Gilead Sciences, Janssen, and ViiV Healthcare and has received payment for talks from AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare.
Juan González García has acted as a consultant for Abbott Laboratories, AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck, and ViiV Healthcare and has received payment for talks from Abbott Laboratories, AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare.
Félix Gutiérrez has acted as a consultant for Bristol-Myers Squibb, Gilead Sciences, GlaxoSmithKline, Merck Sharp & Dohme, and ViiV Healthcare and has received payment for talks and preparation of training materials from Bristol-Myers Squibb, Gilead Sciences, GlaxoSmithKline, Merck Sharp & Dohme, and ViiV Healthcare.
José Antonio Iribarren has acted as a consultant for AbbVie and Janssen and has received clinical research grant support from AbbVie, Bristol-Myers Squibb, Gobierno Vasco, FIPSE, and FISS. He has also received financial support to attend scientific meetings from AbbVie, Gilead, Janssen, and ViiV and has participated in training activities, talks, and symposia sponsored by AbbVie, Bristol-Myers Squibb, Gilead, Merck Sharp & Dohme, Novartis Janssen, Pfizer, and ViiV.
Hernando Knobel has acted as a consultant for AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare and has received payment for talks from AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare. He has also received payment for developing training presentations from AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare.
Josep M. Llibre has acted as a consultant for Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare and has received payment for providing training from Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare.
José López Aldeguer has acted as a consultant for AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, and ViiV Healthcare. He has received clinical research grant support from Bristol-Myers Squibb and ViiV Healthcare and has received payment for talks from AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare.
Juan E. Losa has acted as a consultant for AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare and has received payment for talks from AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare.
Fernando Lozano has acted as a consultant for AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck-Sharp & Dohme, and ViiV Healthcare and has received payment for training sessions from AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck-Sharp & Dohme, and ViiV Healthcare.
Josep Mallolas has acted as a consultant for AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, GlaxoSmithKline, Merck Sharp & Dohme, and ViiV Healthcare and has received research grants from AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, GlaxoSmithKline, Merck Sharp & Dohme, and ViiV Healthcare. He has also received payment for talks from AbbVie, Bristol-Myers Squibb, Gilead Sciences, GlaxoSmithKline, Merck Sharp & Dohme, and ViiV Healthcare.
Ana Mariño has received grant aid for attendance at conferences and meetings from AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, and ViiV Healthcare.
José M. Miró has acted as a consultant for AbbVie, Bristol-Myers Squibb, Gilead Sciences, Merck Sharp & Dohme, Novartis, and Sanofi and has received clinical research grant support from Cubist, Gilead, ViiV, Novartis, Merck Sharp & Dohme, Fondo de Investigaciones Sanitarias (FIS) del Instituto de Salud Carlos III (Madrid), Fundación para la Investigación y Prevención del Sida en España (FIPSE, Madrid), Ministerio de Sanidad, Servicios Sociales e Igualdad (MSSSI, Madrid), National Institutes of Health (NIH, Bethesda, Maryland, USA), and NEAT. He has also received payment for talks from AbbVie, Bristol-Myers Squibb, Gilead Sciences, Merck Sharp & Dohme, Novartis, and ViiV Healthcare.
Santiago Moreno has acted as a consultant for AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and Roche and has received clinical research grant support from AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and Roche. He has also received payment for talks from AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and Roche.
Rosario Palacios has acted as a consultant for Bristol-Myers Squibb, Gilead Sciences, and Janssen and has received payment for talks from Bristol-Myers Squibb, Merck Sharp & Dohme, Janssen, Gilead Sciences, and ViiV-Healthcare.
José A. Pérez Molina has acted as a consultant for Bristol-Myers Squibb, Gilead Sciences, Merck Sharp & Dohme, and ViiV Healthcare and has received payment for talks from Bristol-Myers Squibb, Merck Sharp & Dohme, and ViiV Healthcare.
Juan A. Pineda declares that he has received payment for consultancy services from AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, GlaxoSmithKline, Janssen, and Merck Sharp & Dohme and research grants from Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, GlaxoSmithKline, Janssen, Merck Sharp & Dohme, Roche Pharma, and ViiV Healthcare. He has also received payment for talks from Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, GlaxoSmithKline, Janssen, Merck Sharp & Dohme, Roche Pharma, and ViiV Healthcare.
Rosa Polo declares that she has not received any grant aid or subsidies associated with this document. In the past, she has received payment for preparation of training presentations for Gilead Sciences, Janssen, and Merck Sharp & Dohme.
Federico Pulido has acted as a consultant for AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare and has received payment for talks from Abbott Laboratories, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare.
Esteban Ribera has acted as a consultant for and received support for research and training on HIV infection from AbbVie, Bristol-Myers Squibb, Ferrer International, Gilead, GlaxoSmithKline, Janssen, Merck Sharp & Dohme, Pfizer, Roche Farma, Schering Plough, and ViiV.
Antonio Rivero has acted as a consultant for AbbVie, Bristol-Myers Squibb, Gilead Sciences, Merck Sharp & Dohme, and ViiV Healthcare. He has received clinical research grant support from AbbVie, Bristol-Myers Squibb, Gilead Sciences, Merck Sharp & Dohme, and ViiV Healthcare and payment for talks from AbbVie, Bristol-Myers Squibb, Gilead Sciences, Merck Sharp & Dohme, and ViiV Healthcare.
Rafael Rubio has acted as a consultant for AbbVie, Bristol-Myers Squibb, Gilead Sciences, and Janssen and has received payment for talks from AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, Roche, and ViiV Healthcare.
José Sanz Moreno has participated in clinical trials sponsored by Bristol-Myers Squibb, and ViiV Healthcare. He has received payment for consultancy work and preparing training presentations for AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, and ViiV Healthcare.
Jesús Sanz Sanz has acted as a consultant for AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, ViiV Healthcare, and Boehringer Ingelheim. He has received payment for talks from AbbVie, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp & Dohme, ViiV Healthcare, and Boehringer Ingelheim and for preparing training presentations from ViiV Healthcare.
María Jesús Téllez has acted as a consultant for AbbVie, Bristol-Myers Squibb, Gilead Sciences, and Janssen and has received payment for talks from Gilead Sciences and Janssen.
Javier de la Torre has acted as a consultant for Bristol-Myers Squibb, Gilead Sciences, GlaxoSmithKline, Janssen, Merck Sharp & Dohme, and ViiV Healthcare and has received payment for talks from AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, GlaxoSmithKline, Janssen, Merck Sharp & Dohme, and ViiV Healthcare.
Montserrat Tuset has received clinical research grant support from Bristol-Myers Squibb, Gilead Sciences, Merck Sharp & Dohme, and Janssen and payment for talks from Janssen, Merck Sharp & Dohme, Gilead Sciences, and ViiV Healthcare.
The Board of GESIDA and the National AIDS Plan acknowledge the contributions and opinions of Pablo Bachiller, Belén Box, Esther Cabrero, Santiago Cenoz, Inmaculada Clotet, Manuel Cotarelo, Adrià Curran, Pedro Ferrer, Marcela González, Raquel González, Beatriz Hernández-Novoa, Francisco Ledesma, José Emilio Martin Herrero, Nuria Sánchez, Óscar Rincón, Felipe Rodríguez Alcántara, Óscar Serrano, José Verdejo y Eugenia Vispo.
Antonio Rivero1, Rosa Polo2, José López Aldeguer3, Fernando Lozano4, Antonio Antela5, Koldo Aguirrebengoa6, José Ramón Arribas7, Victor Asensi8, Juan Berenguer9, José Ramón Blanco10, Vicente Boix11, José Luis Casado12, Bonaventura Clotet13, Manuel Crespo14, Pere Domingo15, Carlos Dueñas16, Vicente Estrada17, Federico García18, José María Gatell19, Juan Luis Gómez-Sirvent20, Juan González-García21, Félix Gutiérrez22, José Antonio Iribarren23, Hernando Knobel24, Josep María Llibre25, Juan Emilio Losa26, Josep Mallolas27, Ana Mariño28, José M. Miró29, Santiago Moreno30, Rosario Palacios31, Juan Antonio Pineda32, Federico Pulido33, Esteban Ribera34, Rafael Rubio35, José Sanz Moreno36, Jesús Sanz Sanz37, María Jesús Téllez38, Javier de la Torre39, Montserrat Tuset40, José A. Pérez Molina41.
1Hospital Universitario Reina Sofía/IMIBIC, Córdoba; 2Secretaría del Plan Nacional sobre el Sida, Ministerio de Sanidad, Servicios Sociales e Igualdad;3Hospital Universitario La Fe, IIS La Fe, Valencia; 4Hospital Universitario Virgen de Valme, Sevilla, e-mail ID: fernandolozano@telefonica.net; 5Hospital Clínico Universitario, Santiago de Compostela. 6Hospital Universitario de Cruces, Bilbao; 7Hospital Universitario La Paz-IdiPAZ, Madrid; 8Hospital Universitario Central de Asturias, Oviedo. 9Hospital General Universitario Gregorio Marañón, Madrid 10Hospital San Pedro-CIBIR, Logroño; 11Hospital General Universitario, Alicante; 12Hospital Ramón y Cajal-IRYCIS, Madrid; 13Hospital Germans Trias i Pujol, Badalona; 14Hospital Vall d’Hebron, Barcelona; 15Hospitals Universitaris Arnau de Vilanova i Santa Maria-IRB, Lleida; 16Hospital Universitario, Burgos. 17Hospital Clínico San Carlos, Madrid; 18Complejo Hospitalario Universitario, Granada; 19Hospital Clínic-IDIBAPS, Universidad de Barcelona, Barcelona; 20Hospital Universitario de Canarias, Santa Cruz de Tenerife. 21Hospital Universitario La Paz-IdiPAZ, Madrid; 22Hospital General Universitario de Elche, Universidad Miguel Hernández, Alicante; 23Hospital Universitario Donostia, San Sebastián; 24Hospital del Mar, Barcelona; 25Hospital Germans Trias i Pujol, Badalona; 26Hospital de Alcorcón, Fundación Alcorcón, Madrid; 27Hospital Clínic-IDIBAPS, Universidad de Barcelona, Barcelona; 28Hospital Arquitecto Marcide, Ferrol; 29Hospital Clínic-IDIBAPS, Universidad de Barcelona, Barcelona; 30Hospital Ramón y Cajal-IRYCIS, Madrid; 31Hospital Universitario Virgen de la Victoria, Málaga; 32Hospital Universitario Virgen de Valme, Sevilla; 33Hospital Doce de Octubre, Madrid; 34Hospital Vall d’Hebron, Barcelona; 35Hospital Doce de Octubre, Madrid; 36Hospital Universitario Príncipe de Asturias, Alcalá de Henares, Madrid. 37Hospital Universitario de la Princesa, Madrid; 38Hospital Clínico San Carlos, Madrid; 39Hospital Costa del Sol, Marbella; 40Hospital Clínic-IDIBAPS, Universidad de Barcelona, Barcelona; 41Hospital Ramón y Cajal-IRYCIS, Madrid.