Arterial vascular injury associated with anterior dislocation of the shoulder is a rare but potentially devastating complication, often seen in the context of high-energy trauma or penetrating injury. It is a medical emergency that can compromise both the viability and functionality of the limb, as well as the patient’s life if it is not identified early and treated properly. However, its diagnosis can be difficult, since it requires a high index of suspicion. The presence of an axillary artery thrombosis after shoulder dislocation resulting from low-energy trauma is extremely rare, even more so with subacute clinical presentation associated with embolism to the radial artery.
La lesión vascular arterial asociada a la luxación anterior de hombro es un complicación rara pero potencialmente devastadora, a menudo en el contexto de traumatismos de alta energía o heridas penetrantes. Se trata de una emergencia médica que puede llegar a comprometer la viabilidad y funcionalidad del miembro, incluso la vida del paciente si no es identificada precozmente y tratada de forma adecuada. Sin embargo, su diagnóstico puede ser difícil, pues precisa un alto índice de sospecha. La presencia de una trombosis de la arteria axilar con una luxación de hombro por un mecanismo de baja energía, es extraordinariamente poco frecuente, especialmente cuando se presenta de forma subaguda con embolismo en la arteria radial.
Although anterior inferior glenohumeral dislocation is one of the most frequent conditions attended in emergency trauma departments, arterial vascular injuries associated with it are infrequent, representing less than 1% of total injuries.1 They usually involve very high energy mechanisms, such as traffic or sports accidents, which cause large displacement of the humeral head and elongation of the axillary artery, and are often described in the context of fractured shoulder or penetrating injuries. Regardless of the mechanism, the resulting injury to the artery wall can trigger vessel thrombosis, aneurysm formation or tear of the artery itself.
Subclavian-axillary thrombosis caused by glenohumeral dislocation is now a medical emergency, due to its associated morbidity and early identification and treatment is essential to ensure the viability of the limb and its full functionality. In the first recorded series2 of axillary artery lesions in chronic shoulder dislocations, half of the patients died, and the rest lost the limb or its functionality. Although treatment of this entity has improved significantly since then, thanks to improved imaging techniques and the development of vascular treatments, subclavian thrombosis remains a potentially serious process, and one that is essential to identify and treat promptly.
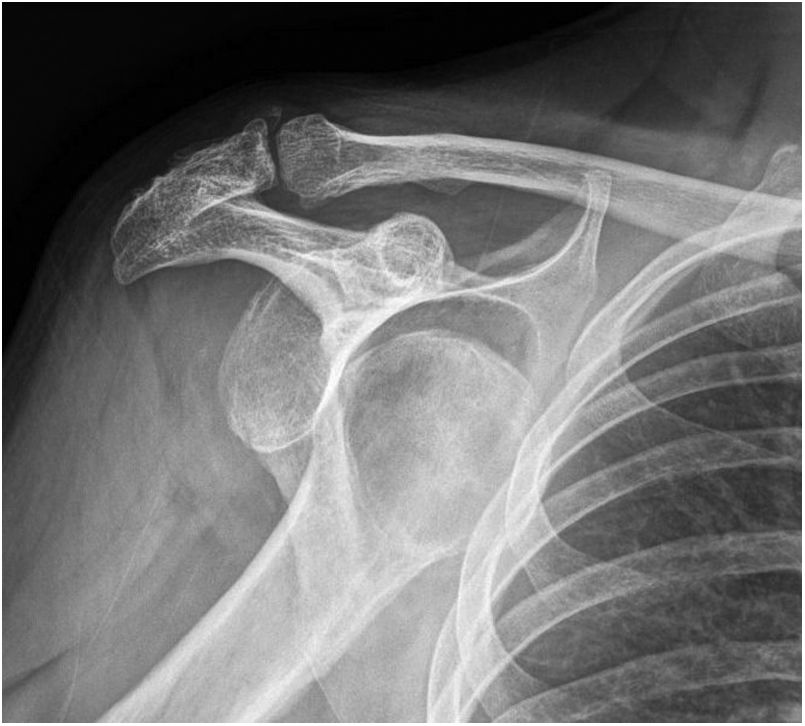
Clinical caseAn active (mechanic), dyslipidaemic, 55-year-old male, with 2 previous episodes of traumatic anterior dislocation of the right shoulder, not associated with fracture (the first 11 months and the second 4 months previously), for which he was in the process of rehabilitation. During physiotherapist-assisted exercises he suffered a third dislocation episode with a hyperabduction manoeuvre of the arm. The patient was assessed in the emergency department. Showing typical epaulet sign shoulder deformity and functional powerlessness to mobilise the affected arm, neurological examination was non-pathological, and pulses were present at all levels of the limb. After an unremarkable clinical examination and conventional radiographic study, which confirmed an anteroinferior shoulder dislocation (Fig. 1), the dislocation was simply reduced using a Milch manoeuvre after subacromial infiltration of local anaesthetic, with an interval of less than one hour from dislocation of the shoulder to its reduction, since the dislocation occurred in the hospital’s own gym. After the reduction the clinical and radiographic examination was satisfactory, and the patient was discharged with his arm antalgically immobilised with a sling. After 10 days, the patient attended their health centre reporting paraesthesia in the fingers of the immobilised arm, with preserved motor function and distal pulses intact. This was categorised as a sensitive condition associated with the immobilisation. Two days later, the patient went back to their health centre due to coldness and marked pallor in his right hand and hypoaesthesia in his fingers, with absence of radial and ulnar pulses, combined with haematoma on the inner face of the elbow to the level of the medial epicondyle.
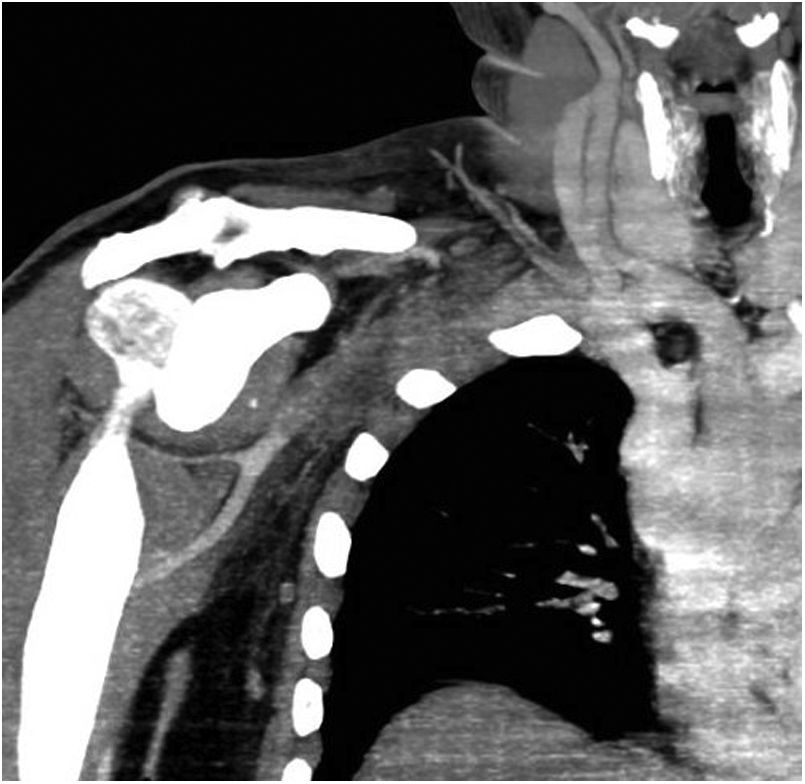
Given the suspicion of vascular involvement, the patient was referred to the hospital’s emergency department. An arterial Doppler ultrasound was performed on the upper limbs to detect absence of arterial flow at the radial and ulnar levels. Both were occupied by thrombogenic material up to the humeral bifurcation, and a permeable humeral artery with monophasic arterial flow was observed, suggesting stenosis or proximal occlusion. On completing the study with CT angiography, the suspicion was confirmed of arterial thrombosis from the middle third of the right subclavian artery to the proximal humeral artery, where it was repermeabilised, associating perivascular inflammatory changes in the thoracic outlet attributable to the different previous episodes of glenohumeral dislocation (Fig. 2). In the distal region of the limb the complete occupation of the ulnar and radial arteries was confirmed as a possible embolisation of the proximal thrombosis.
Once the diagnosis was confirmed, anticoagulant treatment adjusted to the patient’s weight was initiated and he was urgently referred to the referral hospital with a vascular surgery department. On his arrival at the referral hospital, the vascular surgery department observed acute ischaemia of the right upper limb, with absence of pulses at all levels, combined with mild paraesthesia and coldness and pallor of the hand compared to the contralateral limb, without impaired sensation or mobility, classified as acute grade I (viable) ischemia and treated conservatively with anticoagulant therapy. Fifteen days after the initial symptoms, the patient was reassessed, and clear clinical improvement was observed. The humeral pulse had recovered weakly, and the paraesthesia and signs of coldness and pallor had disappeared. As the only residual symptom, the patient reported claudication of the limb on exercise. A new arterial echo-Doppler was performed, where partial repermeabilisation of the subclavian- axillary axis was observed. It was decided, therefore, to continue anticoagulant therapy for 2 months, and subsequently to continue therapy with simple antiaggregation and vascular rehabilitation exercises.
DiscussionAnteroinferior glenohumeral dislocation is a clinical entity in its own right within the pathology of trauma due to its frequency, mechanism of injury, clinical presentation, reduction manoeuvres and potential associated complications. The anatomical proximity of the axillary neurovascular structures to the biomechanical axis of movement of the humeral head during dislocation places them at potential risk of injury.
Although there are many anatomical variations, classically the axillary artery, continuation of the subclavian artery, begins at the outer edge of the major round muscle. Using the pectoralis minor muscle as the reference we can distinguish 3 segments; the first segment of the axillary artery is located between the first rib and the upper edge of the pectoralis major muscle and gives rise to only one branch, the upper thoracic artery. The second part of the axillary artery is located in depth to the pectoralis minor muscle, and gives rise to 2 branches, the thoracoacromial and the lateral thoracic, both of which are often collateral in origin. The third part of the axillary artery runs distal to the pectoralis minor muscle, and gives rise to 3 branches: the subscapular, the anterior humeral circumflex and the posterior humeral circumflex. This last segment, located discreetly in front of the lower rim of the glenoid fossa, is considered to be particularly vulnerable to the stretching and elongation of tissues, which causes shoulder dislocation, especially at the exit of the subscapular branch of the axillary artery.
Three mechanisms have been proposed to explain axillary artery injury after anterior shoulder dislocation. The theory of Adovasio3 is the most widely accepted, according to which the axillary artery would be anatomically fixed between the circumflex and subscapular arteries, with limited mobility with the normal extension and abduction movements of the shoulder. This has been demonstrated experimentally in cadavers.4 Hyperabduction of the arm, together with direct compression by the dislocated humeral head would cause elongation of the axillary artery and disruption at the level of the exit of the subscapular artery. Brown5 suggested that the lateral edge of the pectoralis minor muscle could act as a fulcrum on which the axillary artery would be twisted. The brachial plexus, which surrounds the artery, could also exert a string effect. The last mechanism proposed by Jardon6 would involve fixation of the axillary artery to the pericapsular scar tissue resulting from previous recurrent instability.
Up to 75% of patients with axillary artery injury following previous shoulder dislocation are males over the age of 75,7 with dyslipidaemia and a certain degree of atheromatosis that would cause loss of vascular flexibility, with thrombosis and pseudoaneurysm being more common in these patients. A second group of patients is identified, younger, with a previous history of recurrent glenohumeral instability that would result in a scar bed to which the vascular structures would adhere, such that after shoulder dislocation, a vascular injury would occur, of the thrombosis and arterial transection type in particular. Dislocation of the shoulder represents a blunt trauma to the axillary artery, and whether the artery is elongated or compressed, its inner layer may tear as it loses elasticity with age, while the adventitious layer remains intact. A partial subadventitial tear would lead to the creation of an intimal flap and sub-intimal haematoma that would eventually obstruct flow and cause thrombosis.
Axillary artery injuries can be classified as acute or delayed. Acute lesions include partial or total disruption of the artery, resulting in bleeding and thrombosis, and are the result of compression or laceration by bone fragments, expansive haematomas or arterial spasms. Delayed injuries include false aneurysms, arteriovenous fistulas, thrombosis and thromboembolism.
Diagnosis of a vascular complication after shoulder dislocation is based on clinical suspicion and physical examination and confirmed by the relevant vascular imaging tests. Due to the subtle symptoms of this type of injury, a high level of clinical suspicion is required to identify the vascular arterial injury early, establish the appropriate treatment and prevent complications. The anamnesis must be directed so as to determine the mechanism of injury, especially if the patient is conscious, a possible history of recurrent shoulder injury or arteriosclerosis which could act as predisposing factors. The classical signs of acute arterial ischaemia, with absence of pulse, pallor, pain, paraesthesia or even paralysis are usually absent even in the case of severe axillary artery injury due to the presence of a profuse collateral network around the shoulder. As a result, a patient with a totally thrombosed or even totally disrupted axillary artery may present with a viable limb or a distal pulse. Even so, palpation of the distal pulses, both before and after reduction of the shoulder dislocation, is the simplest physical examination measure for suspected vascular injury. The absence of a pulse or the presence of a weak or significantly decreased radial or ulnar pulse relative to the contralateral limb in a shoulder dislocation is indicative of vascular injury. The pulse can be restored by simply reducing the dislocated shoulder, and it is extremely important that the reduction manoeuvre is as early and smooth as possible, as it can magnify established vascular damage. Absence of a pulse on clinical examination in an anterior shoulder dislocation may be due to acute arterial collapse due to the compressive effect of the humeral head, especially if the degree of displacement is significant, reflex vasospasm secondary to arterial damage, or in the worst case, arterial transection. In these cases, reduction of the dislocation is an emergency, rapidly restoring the pulse in the event of vasospasm or vascular collapse, but absence of pulse persisting in the case of arterial transection. Even with complete restoration of the pulse after reduction, a vascular imaging study should always be requested. However, due to the presence of profuse collateral glenohumeral peri-capsular circulation, there may a pulse and adequate perfusion and capillarity in the fingers, but this does not rule out vascular injury. In other words, the absence of a pulse may indicate vascular injury, but its presence does not rule it out. The presence of a weak or asymmetric arterial pulse with respect to the contralateral limb should never be attributed to vasospasm, and a vascular imaging study should be performed.8
Probably the most useful symptom to identify inadequate distal circulation is the presence of paraesthesia,9 since injury to the axillary artery can be associated with injury to the brachial plexus in up to 60% of cases, due to the close anatomical relationship between the two, while vascular injury determines the viability of the limb in the short term. In cases of slowly progressive ischaemia, paraesthesia, lividity of the fingers, peripheral coldness or weak radial pulse can be the only symptoms present. Other less frequent signs include the appearance of an expansive axillary haematoma, which may be pulsating in the case of a pseudoaneurysm or a decreasing haematoma that may appear in the anterosuperior region of the ipsilateral hemithorax. The appearance of this haematoma, although rare, is highly indicative of possible injury to the axillary artery. The triad of axillary haematoma, absent or weak arterial pulse and dysaesthesia in the context of shoulder dislocation should always alert the specialist to a possible associated arterial injury.9
With regard to imaging tests, vascular Doppler ultrasound is a very useful tool for the diagnosis of vascular lesions, and in most cases is sufficient for diagnosis. However Doppler vascular ultrasound is an operator-dependent technique that can under-diagnose the extent of vascular involvement. Therefore, it must be supplemented with CT angiography, which enables accurate identification not only of the exact location of the thrombus, but also its extent and collateral circulation, providing useful information for decision making.
Although endovascular surgery techniques have improved significantly,10 open surgery remains the treatment of choice.
ConclusionThere are few cases described in the literature of axillary arterial thrombosis due to shoulder dislocation secondary to a low energy mechanism and without a context of fracture, which also present insidiously due to distal thromboembolisation. A knowledge of this pathological process is of utmost importance for its early and accurate diagnosis, in order to treat it urgently to ensure the viability and functionality of the limb.
Level of evidenceLevel of evidence iv.
Please cite this article as: Pellicer-Garcia V, Bargay-Juan P. Trombosis arterial subclavioaxilar y embolización distal tras luxación glenohumeral anterior traumática. Rev Esp Cir Ortop Traumatol. 2020;64:130–133.