Carpal coalitions are relatively frequent between bones in the same carpal row. Coalitions between bones of different rows, however, are very uncommon. We present a case of bilateral intercarpal coalition between the trapezium and scaphoid as an incidental finding, confirming its hereditary origin since a parent has the same bilateral coalition.
Las coaliciones carpianas son relativamente frecuentes entre huesos de la misma hilera del carpo. Son mucho más infrecuentes las coaliciones entre huesos de diferente hilera. Presentamos un caso de coalición intercarpiana entre trapecio y escafoides bilateral como hallazgo casual, confirmando su origen hereditario ya que uno de los progenitores presenta la misma coalición.
Carpal coalitions are caused by synostosis or synchondrosis of 2 or more carpal bones.1 Their incidence in the adult population varies from 0.1% to 9%.2 The few references to this condition show that complete coalitions are more common between the semilunate and pyramidal bones (SP)2 and the capitate and hamate bones.3
Coalitions between the scaphoid and trapezium bones (ST) are very rare. The majority of series contain one or no cases, and when they do contain one, they are often associated with hereditary syndromes or other coalitions.4
We present the case of a patient with asymptomatic bilateral hereditary ST diagnosed following fracture of the distal radius.
Clinical caseA 17 year-old man (patient A) with a history of asthma visited the Emergency Department of our hospital to evaluate a distal radius fracture caused by a chance fall 2 weeks beforehand.
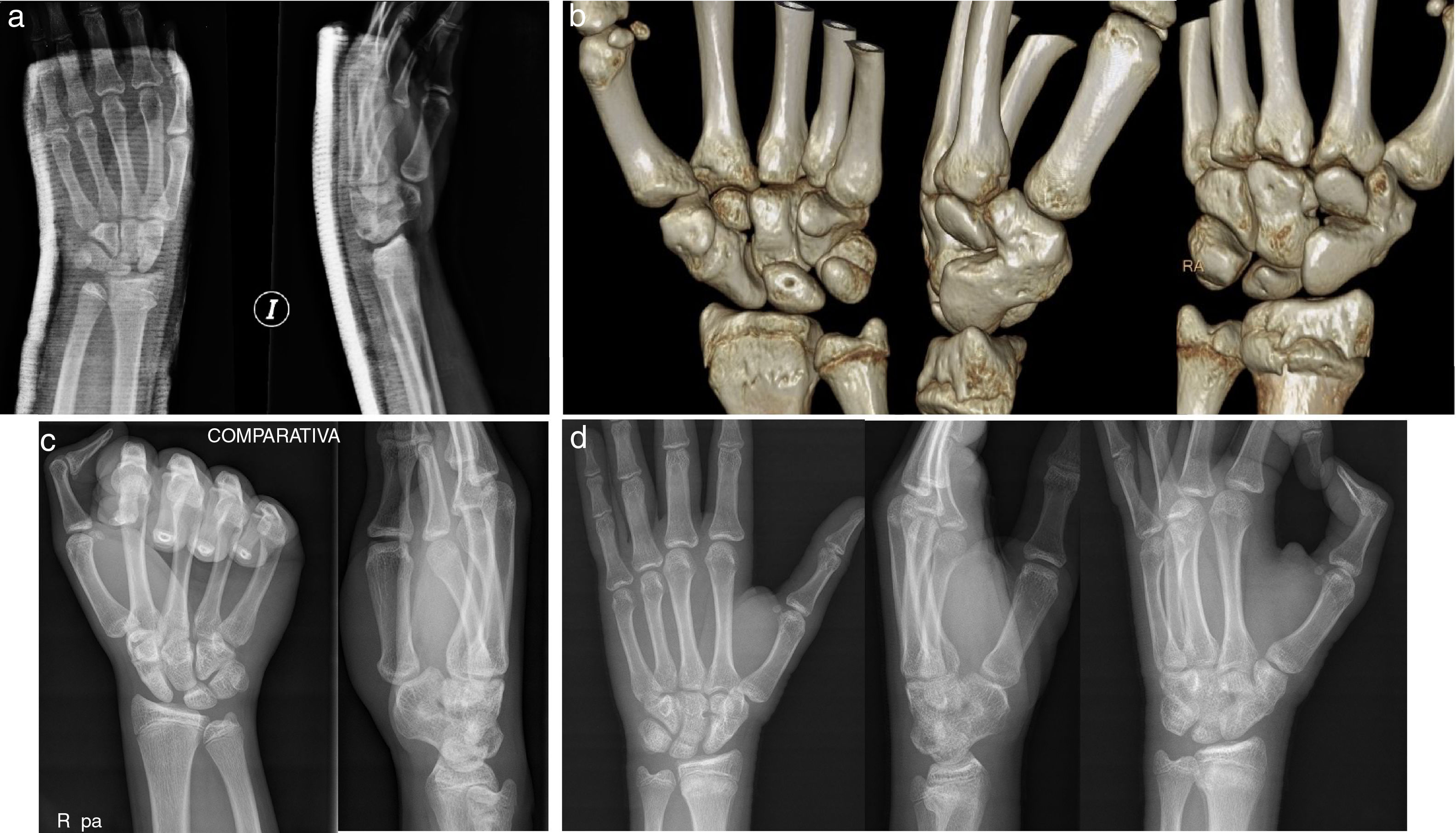
The first X-ray images showed a 12° dorsal angle and an 18° radial inclination (Fig. 1a) of the distal end of the radius. Open physes were observed, as well as an increase in the scapholunate space. Given the time that had passed since the fracture, computed tomographic imaging was used to evaluate the existence of a fracture callus prior to attempting the closed reduction of the same (Fig. 1b). The report confirmed the diagnosis of type II epiphysiolysis according to Salter's classification. No signs of consolidation were detected and a 3mm scapholunate space was found, together with a dorsal angle of 11° and a 17° radial inclination and extension of the semilunate bone respecting the scaphoid. No liquid was found in the joint and no other findings are mentioned. An attempt at closed reduction of the fracture was made on the basis of this information, without achieving any clear improvement in radiological measurements. The possibility of surgery was then raised, together with a fluoroscopic test to evaluate the scapholunate space.
After reviewing the tomographic images during preoperative planning a coalition was detected between the scaphoid and trapezium bones. Taking this finding into account it was decided to take a comparative X-ray image (Fig. 1c) of the contralateral wrist, which showed the same findings: ST coalition with an increase in the scapholunate space and semilunate bone in extension. The patient was completely asymptomatic in the contralateral wrist and had no symptoms prior to the fall.
Given these findings and the lack of improvement in radiological parameters after reduction, the decision was taken to apply orthopaedic treatment of the fracture, removing the plaster cast after 5 weeks (Fig. 1d).
ResultsAfter removing the plaster cast the patient had an immediate range of movement of 60° dorsal flexion, 40° volar flexion and complete pronosupination. The patient had no pain in the site of the fracture and the external appearance of the wrist was very similar to that of the contralateral one, with no visible deformity.
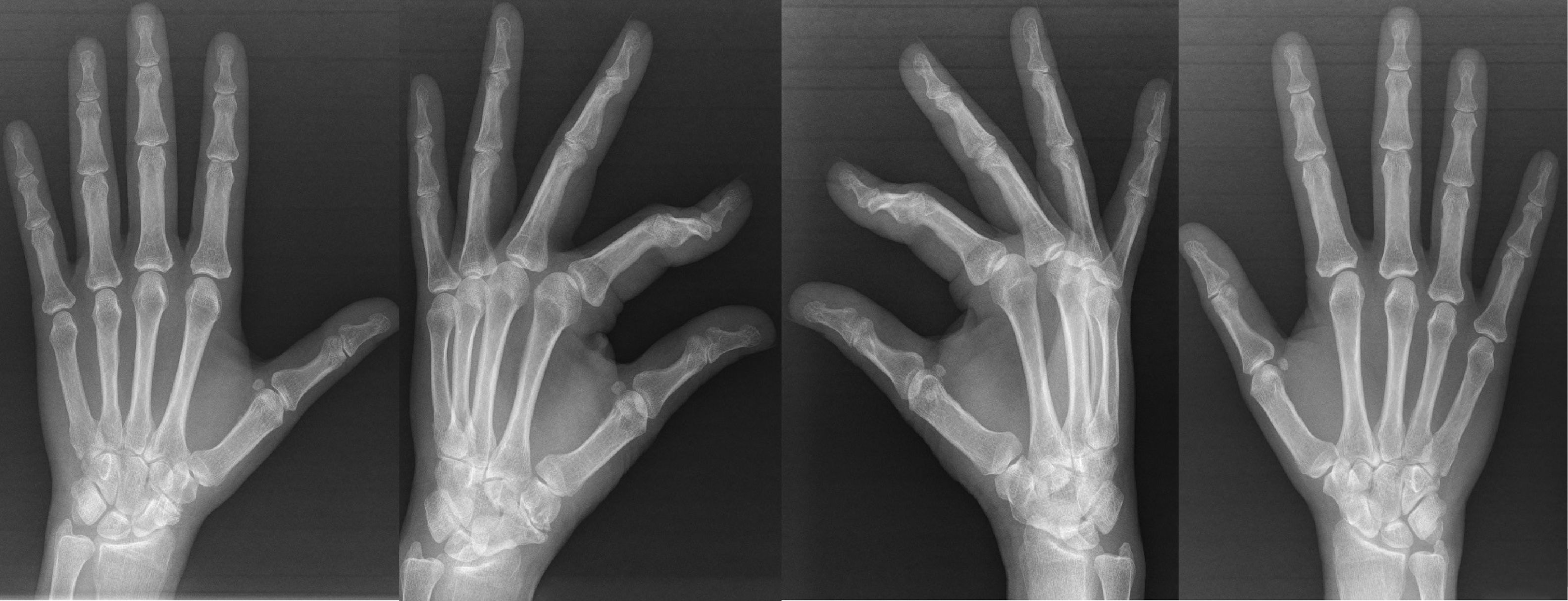
Taking into account the possibility that this is a hereditary coalition the decision was taken to take X-ray images of both hands of the patient's parents. In the case of the mother (patient B) the same type of coalition was found in different degrees. On the right side it was a synchondriosis and on the left side it consisted of a synostosis without an increased scapholunate space (Fig. 2). The patient was clinically asymptomatic.
DiscussionCarpal coalitions are relatively common entities, and in the bibliography their incidence is said to vary from 0.1% to 9%, and they are more frequent in individuals of black races.1–4 They may be associated with syndromes such as multiple congenital arthrogryposis, foetal alcohol syndrome or Turner's syndrome,1,2 among others. In these cases coalitions may occur between more than 2 carpal bones. Cases associated with other bone malformations have been described, such as Madelung's disease or proximal radiocubital synostosis, although in the majority of cases it occurs without any association to other complaints.
The most widely accepted aetiology for the origin of the abnormality is a fault in differentiation during weeks 4–8 of pregnancy,1,2 giving rise to incomplete separation of the cartilaginous precursors. Most authors agree that the term “fusion” should be abolished from the attempt to explain the origin of this complaint, given that it may only be used in acquired cases. In the case we present, an X-ray image taken 3 years before the trauma shows 2 differentiated ossification nuclei for the scaphoid and trapezium which subsequently fused, giving rise to this ST coalition. Other possible etiologies are trauma, inflammatory arthropathies and even the metaplastic conversion of mesoderm derivatives, as in the case of coalition between the pyramidal and pisiform bones. All of these causes are less frequent in this type of anatomical abnormality.2
Carpal coalitions were described for the first time by Sandifort in 1779.1 There are not many references in the bibliography to this entity. The longest series published to date is the one by DeFazio et al.,2 with a total of 103 cases in 85 individuals, 18 of which are bilateral. The most frequent coalition is SP, with 92 cases, while only 2 were between the scaphoid and trapezium, neither of which was bilateral. Van Hoorns et al.3 described a total of 98 cases, 85 between the capitate and hamate bones; none of the coalitions described in this study were of the ST, as occurred in our clinical case. Delaney and Estar1 mention a total of 36 cases in which the most frequent coalition was the SP, with no case of ST coalition.
Coalition between the scaphoid and trapezium is of the intercarpal type, given that it occurs between bones in both rows of carpal bones. This is far less common than coalition between bones in the same row. We only found 2 other references, apart from those cited, to this type of coalition in the bibliography: the first of these refers to a unilateral case;5 the second describes a bilateral case6 with increased scapholunate space. In this second case the mother was also affected, with the same bilateral coalition but without increased scapholunate space. This agrees with data that show intercarpal fusion is genetically transmissible, dominant autosomic Mendelian inheritance unlinked to sex having been proven.7
The most widely used classification of carpal coalitions in the bibliography is the one described by DeVilliers Minnaar8 for the SP coalition, and this has been extended to cover other types. This classification divides them into 4 types, depending on the type of fusion between the bones and other associated carpal abnormalities. Although this classification has been widely used, it is not easy to apply because of the difficulty in detecting the degree of ossification and associated alterations. Due to these problems other classifications have been created, such as the one by Sing et al.,9 which is very descriptive but contains many subtypes, making it hard to use. Lastly, the classification described by Burnett10 divides coalitions into bony and non-bony, making it simpler to use in clinical practice. According to this classification, patient B has a bilateral ST carpal coalition of two different types. Her right hand has a non-bone coalition that is detectable in oblique projection due to the irregular margin separating both bones, with the chief differentiating diagnosis of arthrosis at this level. Her left hand has a bone coalition with clear continuity between both bones. There is no other published case in the bibliography of bilateral ST coalition in different degrees in the same patient.
To conclude, it is essential to underline the importance of taking comparative X-ray images when we detect rare findings in a unilateral X-ray image or when, as in this case, a distance is detected between the semilunate and scaphoid bones which seems abnormal. Performing studies of this type helps us to reach a correct diagnosis and therefore select the most suitable treatment for our patients.
Level of evidenceLevel of evidence v.
Please cite this article as: García-Lamas L, Porras-Moreno MÁ, Jiménez-Díaz V. Coalición carpiana escafotrapezoidea hereditaria. A propósito de un caso. Rev Esp Cir Ortop Traumatol. 2018;62:467–470.