Elbow instability is a difficult to diagnose condition in certain cases, and could lead to some problems that limit daily functioning, such as joint blocks, bumps, projections, muscle weakness, and persistent pain.
A case is presented of a patient with a clinical picture of epicondylitis, with a previous history of a fall on the affected arm. As there was no improvement after performing conventional non-aggressive treatment, surgery was performed on the affected tendon. The outcome of this was persistent pain and clinical instability of the elbow that ended up requiring surgery to reconstruct the ligament over the external complex. In the follow-up 6 months after the operation, the clinical instability had disappeared, but there was still external discomfort and a 30° extension deficit.
When faced with a picture of epicondylitis with a previous injury that does not respond to conventional therapies, it is important to take into account the possibility of an underlying elbow instability, ruling this out with a correct physical examination and, where necessary, with the appropriate complementary tests.
La inestabilidad de codo es una enfermedad de diagnóstico difícil en determinados casos, y puede conllevar unos problemas limitantes para la funcionalidad diaria como los bloqueos articulares, los resaltes, la debilidad muscular y el dolor persistente.
Presentamos el caso de un paciente con clínica de epicondilitis con antecedente previo de una caída sobre el brazo afecto. Tras efectuar los tratamientos convencionales no agresivos y no obtener mejoría, se realiza cirugía sobre la afectación tendinosa. El caso evoluciona hacia la persistencia del dolor, y a una clínica de inestabilidad articular que acaba por precisar cirugía reconstructiva ligamentaria sobre el complejo externo. En el control a los 6 meses de la última intervención ha desaparecido la clínica de inestabilidad, pero aún persisten las molestias en cara externa y un déficit a la extensión de 30°.
Es importante tener en consideración ante un cuadro de epicondilitis con traumatismo previo, rebelde a los tratamientos conservadores, la posibilidad de que haya una inestabilidad de codo subyacente, descartándola con una correcta exploración física y con pruebas complementarias si se precisan.
The elbow is a complex joint and its stability depends on a large number of bony, muscular and ligamentous structures.
Thus, the humeral-ulnar joint, anterior portion of the medial humeral-ulnar ligament and ulnar external collateral ligament or ulnar lateral collateral ligament (ULCL) are considered as primary stabilizers of the elbow in varus/valgus.1–5 The secondary stabilizers include the radial head, the insertion of the flexor/extensor musculature and the joint capsule.
The most common pattern within elbow instabilities is posteroexternal instability,1,2,4 frequently caused by a lesion of the ulnar external collateral ligament. The diagnosis depends on a correct physical examination (varus/valgus with extension and flexion at 30°, lateral pivot shift) and the results of the complementary imaging tests (Rx, CT and MRI).
Additionally, elbow instability includes acute and chronic conditions. In the first case, early diagnosis (important for a correct treatment of this disease) is often difficult except in situations associating an episode of elbow dislocation or fracture (otherwise, they normally go unnoticed). It should be suspected in cases of falls with a combination of axial compression and external rotation of the elbow, by far the most frequent mechanism.1,2,4,5 Chronic cases have a worse prognosis and are often associated with acute and inadequately treated trauma or with surgical sequelae in that region.1,4
We present the case of a patient with an initial diagnosis of epicondylitis, who evolved toward posterolateral elbow instability after treatment.
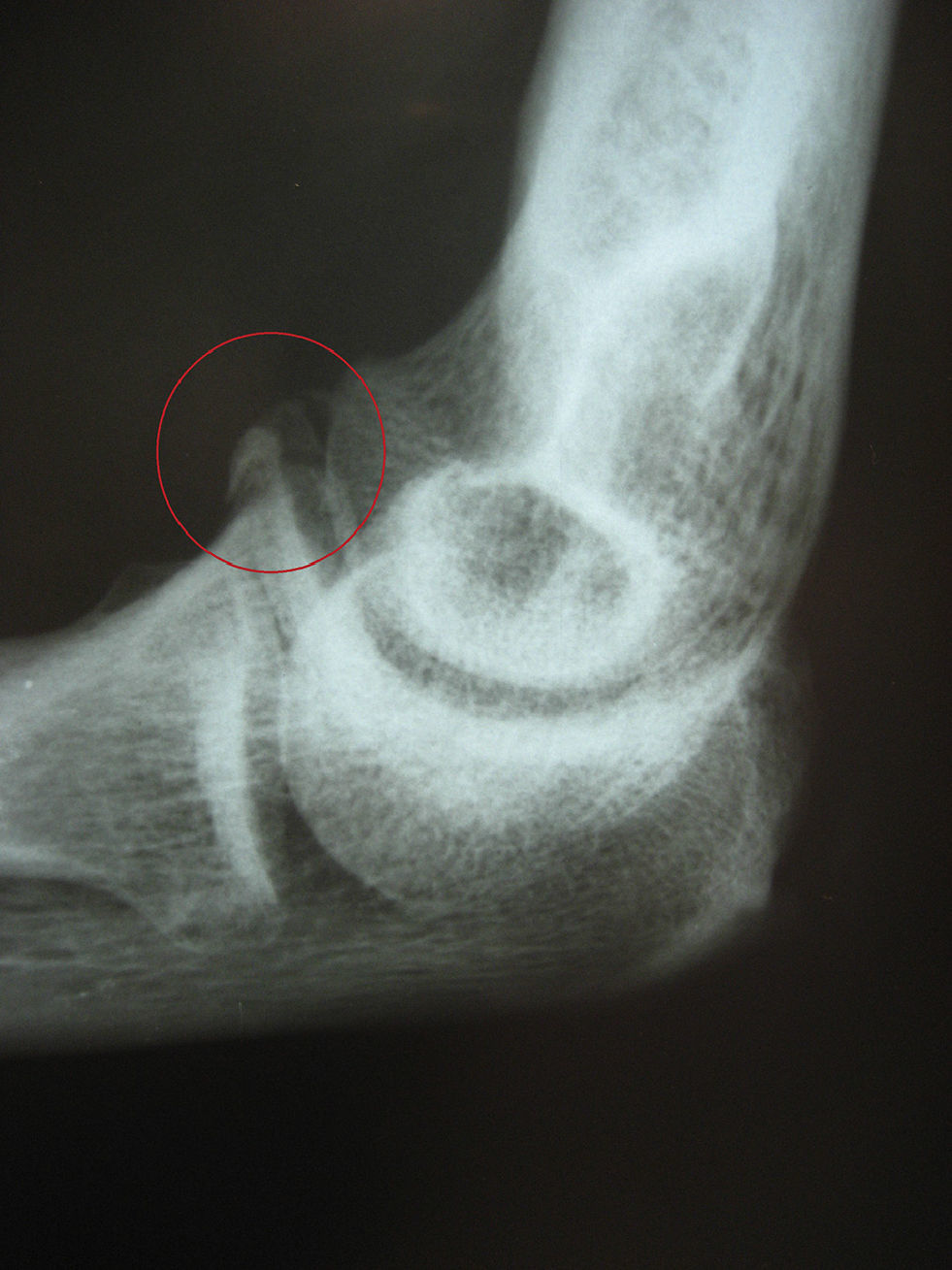
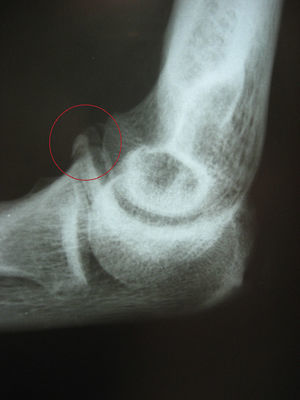
Case reportThe patient was a right-handed, 40-year-old male office worker. The initial symptoms began as pain on the lateral side of the left elbow with positive epicondyle maneuvers. The relevant history included an accidental fall on the affected hand 4 months earlier, with a diagnosis of grade I coronoid fracture (Fig. 1) which required immobilization and rehabilitation.
The tendon inflammation was treated with rehabilitation. The patient received 2 injections of anesthetic and corticosteroid agents in the painful area and, subsequently, 2 sessions of shock waves which partially improved the symptoms. Due to the persistence of symptoms, an MRI study was conducted which revealed a consolidated coronoid fracture, as well as signs of epicondylitis and rarefied image on the proximal insertion of the humeral-ulnar lateral ligament, which did not show a fracture clearly. Clinically, the patient did not report blocking or feeling of collapse, and the varus was stable upon exploration. Thus, surgery was performed at 7 months from the onset of the epicondylar pain. The procedure consisted of a proximal disinsertion of the extensor muscles, epicondylar decortication with perforations on the area and atensional reinsertion of the disinserted musculature, and immobilization for 3 weeks with a brachiopalmar cast and subsequent restart of rehabilitation.
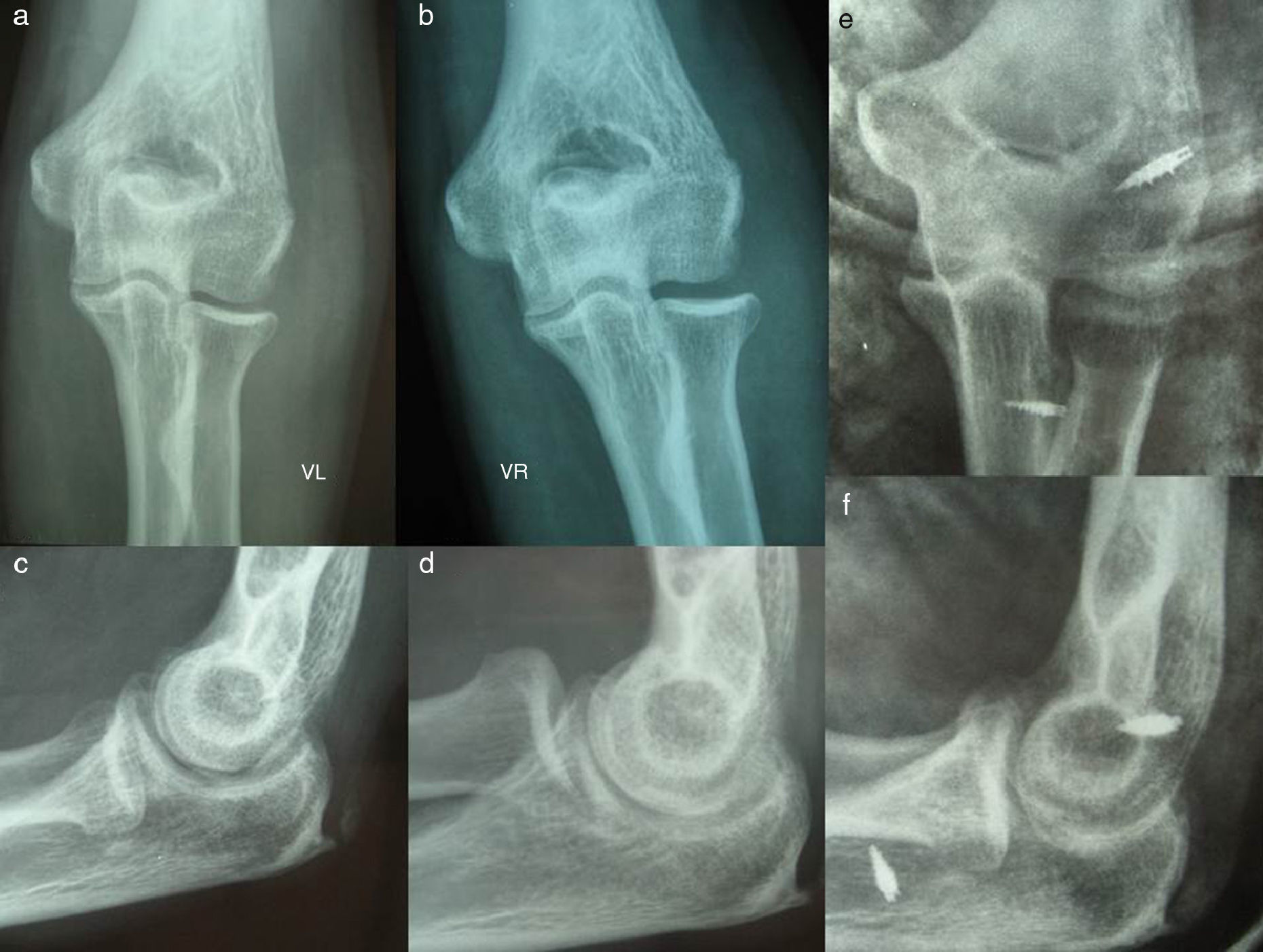
The symptoms evolved toward a persistence of pain, as well as the onset of clicks, painful and unstable varus, evident projection on the radial head during pronosupination and positive pivot shift maneuver (Fig. 2a–d).
The symptoms led to a diagnosis of posterolateral instability. For this reason, at 5 months from the initial surgery, a capsular-muscular retensing of the epicondyle was performed by transosseous sutures, reconstruction of the ULCL on the retightened tissue by allograft of tibialis anterior from the tissue bank (anchored to the epicondyle with a harpoon and at the level of the ulnar crest), and stitches attaching the plasty to adjacent tissue to prevent its projection (Fig. 2e and f).
ResultsThe elbow was immobilized for 2 months with a splint at 90° flexion–extension and neutral pronosupination, and rehabilitation treatment was started from that date. Passive and active assisted mobilizations were the first steps, followed by active movement against gravity after the third month of the ligament reconstruction.
At the end of the follow-up period 6 months after the last intervention (at 4 months of the start of the rehabilitation treatment), no signs of instability were observed during the exploration, with persistent discomfort in the external side and an extension deficit of 30° with 120° flexion and pronosupination of 60° and 70°, respectively. The Mayo Elbow Performance Score was of 75 points (considered as a good result).
DiscussionThe condition of posterolateral elbow instability was first described in 1991 by O’Driscoll.1,5 It usually has a traumatic origin, except in a context of generalized hyperlassitude, and is clinically manifested as locking, clicking, projection, persistent pain and recurrent dislocation.
The literature contains several reports mentioning the relationship in the differential diagnosis between epicondylitis and lateral elbow instability. Thus, cases of epicondylitis with a previous history of trauma (however slight) and with persistent pain despite nonaggressive treatment, should always lead to suspicion of possible posterolateral elbow instability.1,6–8 This is very important because, as described by Dzugan et al, patients in treatment due to chronic epicondylitis who suffer acute injuries of the ULCL require early repair of both lesions in order to obtain satisfactory results.8
Likewise, steroid injections and even the usual surgery on the epicondyle tendons can damage the lateral collateral ligament sufficiently to cause instability of the joint.1,2,5–7 Even Kalainov and Cohen,6 in their review of 3 cases of posterolateral rotational instability in relation to lateral epicondylitis, advocated performing a pivot shift test systematically after completing any tendon release conducted in the epicondylar region.
In the present case, the origin of the elbow ligament failure was the previous injury, 4 months before the onset of epicondylar pain symptoms. In all likelihood, there was an initial involvement of elbow stability (grade I fracture of the coronoid on the initial Rx and rarefied image at the level of the external ligament on the MRI obtained 4 months later). Since elbow stability was maintained by the secondary stabilizers, the musculature became overloaded and caused painful symptoms compatible with epicondylitis. The surgery performed at that level (including musculotendinous disinsertion) unbalanced the symptoms and exposed the underlying initial instability.
We believe that a thorough physical examination (including a pivot shift test) and the use of MRI in cases of recalcitrant epicondylitis are necessary and essential to establish a correct differential diagnosis,7,8 especially in cases in which there is a history of previous trauma. MRI images of lesions on the ulnar coronoid apophysis and the lateral collateral ligament itself (as in the case presented) should lead us to suspect a possible instability, and obviate epicondylar tendon release as the only surgical option, making it necessary to add a surgical procedure on the ligamentous lesion.8
The treatment of choice1,4,5,9 in cases of chronic posterolateral instability is based on an open reconstruction of the affected ligament using allografts, with anchorage on the epicondyle seeking the humeral isometric point and on the lateral part of the ulnar (crista supinator). Arthroscopic techniques may be a possible alternative option in the future.1,10 The results reported by Antuña and O’Driscoll1 with this open technique were good, with stiffness (especially due to a lack of extension) and recurrence of instability (20%) being the most frequent complications.
Level of evidenceLevel of evidence v.
Ethical responsibilitiesProtection of people and animalsThe authors declare that this investigation did not require experiments on humans or animals.
Confidentiality of dataThe authors declare that they have followed the protocols of their workplace on the publication of patient data and that all patients included in the study received sufficient information and gave their written informed consent to participate in the study.
Right to privacy and informed consentThe authors declare that this work does not reflect any patient data.
Please cite this article as: Llop-Corbacho A, Romero-Ruiz J, Denia-Alarcón N. Inestabilidad externa de codo tras el tratamiento quirúrgico de la epicondilitis. A propósito de un caso. Rev Esp Cir Ortop Traumatol. 2014;58:242–245.