Alagille's syndrome is an infrequent genetic condition with autosomal inheritance and variable expression. The complete form exhibits five clinical signs, chronic intrahepatic cholestasis, characteristic facies, cardiovascular anomalies, posterior embryotoxon, and vertebral defects. If only 3 or 4 of these are present the case is considered as an incomplete form.
The association of Alagille's syndrome with radio-ulnar synostosis is extremely rare. There is only one case described in the indexed literature. A case is presented of Alagille's syndrome with bilateral proximal radio-ulnar synostosis. To the best of our knowledge this is the second reported case of this association.
El síndrome de Alagille es una condición genética infrecuente, con herencia autosómica dominante y expresividad variable. En su forma completa presenta 5 signos clínicos característicos: colestasis intrahepática crónica, una facies característica, anomalías cardiovasculares, embriotoxon posterior y defectos vertebrales. Si solo 3 o 4 de estos están presentes se dice que es una forma incompleta del síndrome.
Es extremadamente infrecuente su asociación con sinostosis radiocubitales, habiendo solo un caso descrito de esta asociación en la literatura indexada. Presentamos un caso de síndrome de Alagille asociado a una sinostosis radiocubital proximal bilateral. Que los autores tengan noticia, es el segundo caso de esta asociación publicado en la literatura.
Alagille's syndrome, also known as arteriohepatic dysplasia, is an infrequent genetic condition with a dominant autosomal inheritance pattern and variable expressivity. In its full form, it presents five characteristics of clinical signs: chronic intrahepatic cholestasis, a characteristic facies, cardiovascular anomalies, posterior embryotoxon and vertebral defects. Cases displaying only 3 or 4 of these signs are said to be incomplete forms of the syndrome.1,2 The diagnosis is usually obtained early, as between 45% and 75% of patients develop cholestasis in the first months of life, along with jaundice and pruritus. They may also present xanthomas in the dorsal aspect of the fingers, groin and other areas. Up to 50% of patients may suffer a delay in growth due to cholestasis. If the hepatic manifestations are very severe and cause cirrhosis and liver failure, they may require a liver transplant. In addition, 90% of patients present cardiopathies, the most frequent being peripheral pulmonary stenosis (67%) and the second most frequent being Fallot's tetralogy (16%). They may also present septal or atrial defects, aortic stenosis and aortic coarctation. Patients may suffer cerebrovascular accidents caused by anomalies of the carotid, basilar and medial cerebral arteries, among others.
Patients may present renal cysts and pancreatic involvement.
Regarding the skeleton, 80% of patients present butterfly vertebrae, usually symmetrical, with no clinical repercussions, although they may exceptionally affect the spine. They may also present a reduced interpeduncular distance in the lumbar spine, spina bifida occulta, hemivertebrae and absence of the twelfth rib. The suboptimal nutritional condition and the multifactorial involvement of the disease may cause osteoporosis and facilitate the onset of fractures.
Therefore, skeletal manifestations are just one of several possible types in Alagille's syndrome and patients require care from various specialists.
The association with bilateral radioulnar synostosis is extremely infrequent, with only 1 such case described in the indexed literature, which does not make any mention about treatment.3 We present a case of Alagille's syndrome associated to bilateral proximal radioulnar synostosis. As far as the authors are aware, this is the second case of this association published in the literature.
Case reportThe patient was a 3-year-old boy who was intervened due to Fallot's tetralogy in 2010 at another centre and diagnosed with Alagille's syndrome through hepatic biopsy following an episode of cholestasis in 2012. The patient presented the characteristic facies of the syndrome, with a small mandible, wide forehead, flattened nose and sunken eyes. The patient was being monitored by the Ophthalmology Service due to ocular problems.
The family consulted our service after the patient showed a reduced range of elbow movement. The patient did not present any relevant history of trauma.
Upon clinical exploration, the median, ulnar and radial nerves were found to be intact. The 2-point discrimination measured with a 2-tip discriminator (North Coast Medical, SF, USA) was found to be within a normal range, and under 6mm in all fingers.
The range of motion of the right elbow was 130° flexion, presenting a loss of extension of −15° and with rotation fixed at 35° pronation. The patient presented a compensatory movement at the level of the wrist that allowed pronation of up to 55° and supination of 20°.
The range of motion of the left elbow was of 145° flexion, 0° extension and a fixed rotation at 30° pronation. The patient presented a compensatory movement that allowed 60° pronation and 30° supination.
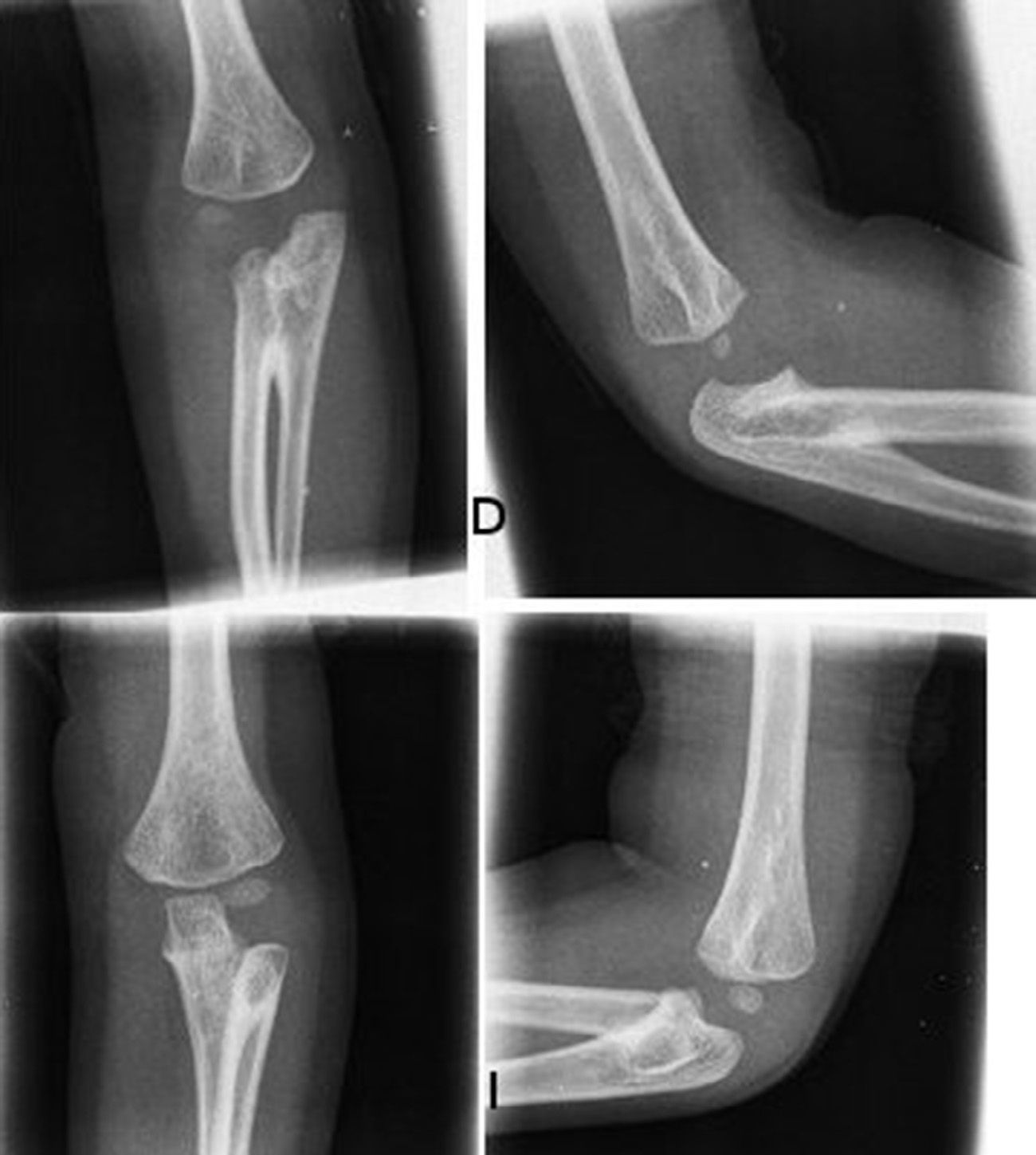
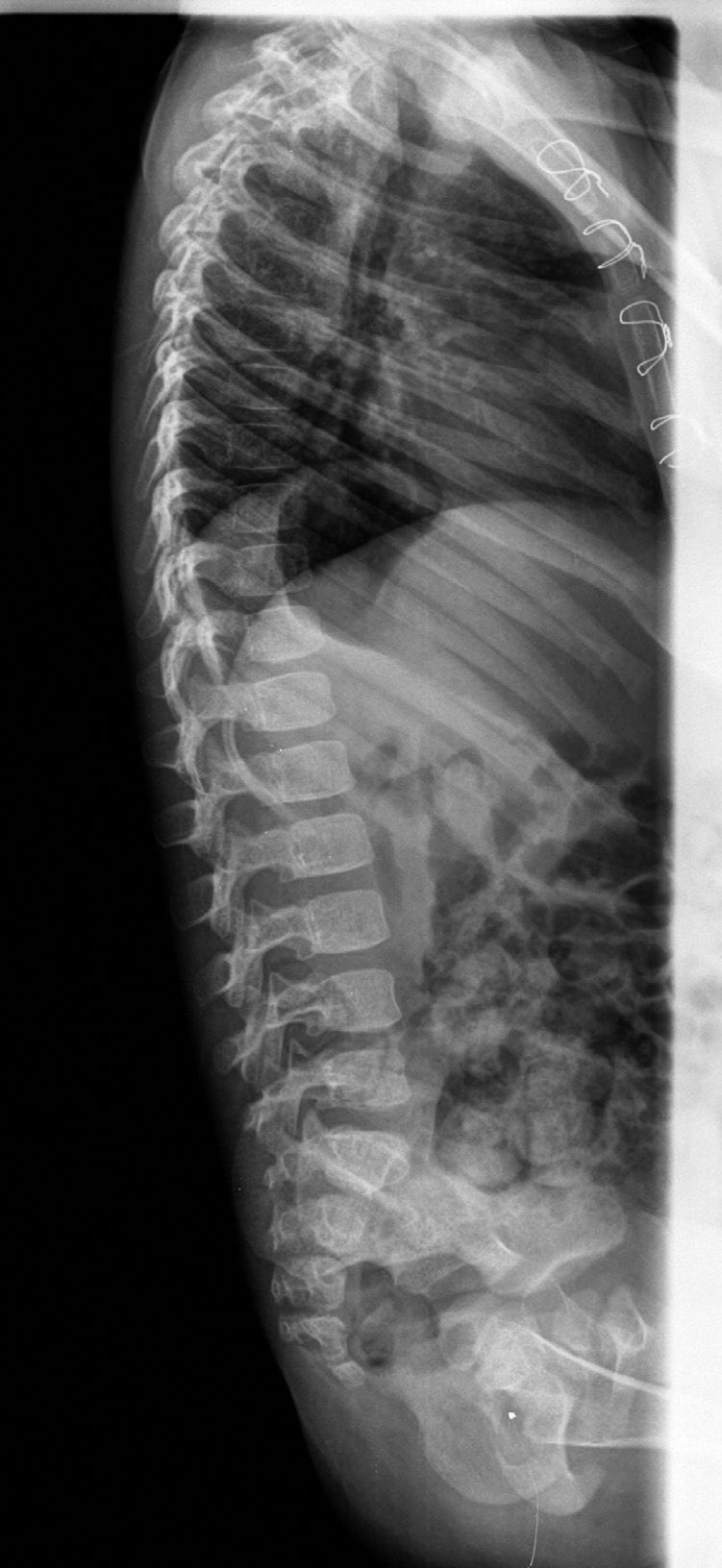
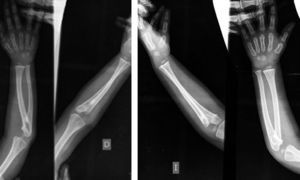
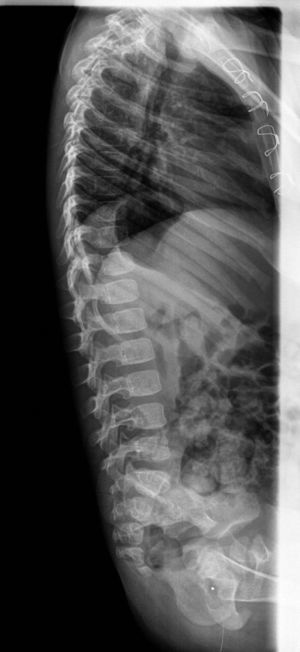
The radiographs of both elbows showed a proximal radioulnar synostosis (Figs. 1 and 2). The radiographs of the spine (Fig. 3) did not reveal any anomalies.
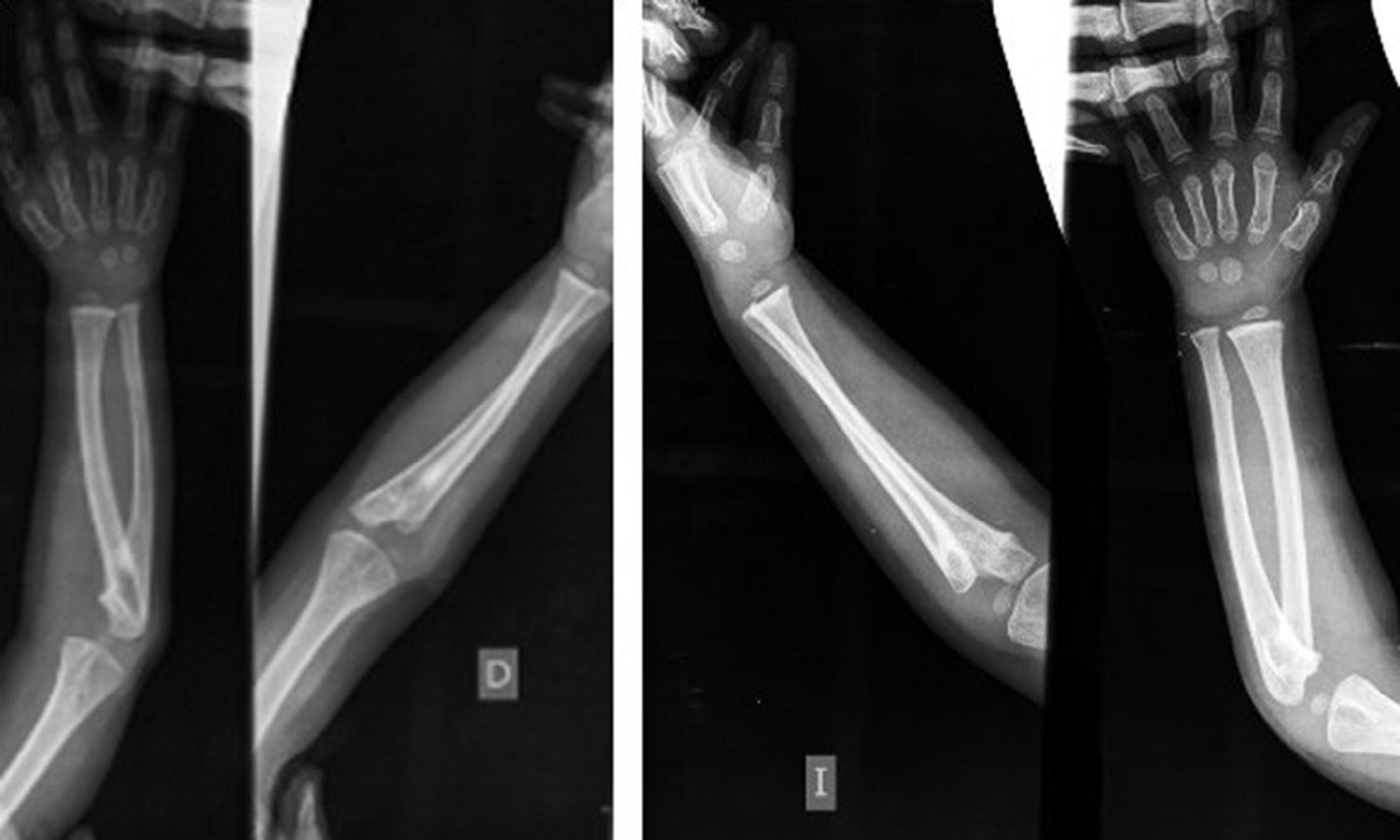
The patient did not report any kind of pain in the range of movement of the elbow or the wrist and was able to grasp objects and manipulate them for games and everyday activities (Fig. 4).
The case was explained to the family and, since the patient seemed to be well adapted to the limitation in forearm rotation, the decision was to continue observation, ruling out surgery.
DiscussionProximal radioulnar synostosis is an infrequent anomaly caused by the lack of separation between the radius and ulna before birth, which normally takes place at the end of the first trimester. It can be associated to hypoplasia of the thumb, carpal coalition, symphalangism and clubfoot. The most frequently associated syndromes are Apert syndrome, arthrogryposis, alcoholic fetopathy and Klinefelter syndrome.4
We were only able to find one case in the literature of Alagille's syndrome associated to proximal radioulnar synostosis. The article did not mention any treatment, instead focusing on the accompanying radiographic findings.3 According to James and Bednar,4 a conservative approach is the most common in the treatment of congenital proximal radioulnar synostosis, as patients often display a considerable compensatory movement at the level of the wrist, which may allow patients to suffer a very small functional deficit.
The indication for surgery is controversial. Cleary and Omer5 indicated surgical interventions very rarely, based more on a functional deficit that on the position of the hand. Simmons and Southmayd6 believed that surgery was indicated when there was more than 60° fixed pronation. Ogino and Hikino7 analysed 40 cases of proximal radioulnar synostosis (15 of them bilateral). Of these, 12 patients did not present any deficit for everyday activities and did not require treatment. The mean deformity in pronation among this group was 21.2°. A further 22 patients presented some level of limitation for everyday activities and required surgical treatment. The mean deformity in pronation among this group was of 60.7°. The authors described the presence of a compensatory wrist movement in patients with congenital radioulnar synostosis. This movement, which was present in nearly all cases, enabled a mean range of movement between 75.6° pronation and 11.3° supination. The authors recognised that there are multiple cultural reasons to indicate surgical treatment or not, since the eating utensils used in western cultures require a smaller supination movement than is necessary in oriental cultures.
In summary, surgery is indicated in cases of bilateral hyperpronation that do not allow affected children to carry out everyday activities. Children who maintain a correct compensatory movement and do not report difficulties for everyday activities do not normally require treatment.
There are two main surgical options. The first is to carry out a derotating osteotomy in at least one of the forearms, so that one of the hands will not present an extreme pronation. Green and Mital8 were the first to describe this technique, concluding that the best position in bilateral cases was 30–45° pronation in the dominant side and 20–30° supination in the non-dominant. The most frequent complications are a loss of rotation and neurovascular complications, such as Volkmann ischaemic contracture and radial paresis. Multiple variations have been described in order to minimise these complications, including the use of Ilizarov fixators for progressive distraction with osteotomies at two levels.9
The other option is to carry out a resection of the synostosis and interposition of a free adipofascial flap, like a lateral arm flap or a free inguinal flap. This procedure was initially described by Kanaya and Ibaraki,10 who employed it on 7 patients, opening the synostosis and interposing a lateral adipofascial arm flap between the ulna and radius. None of their patients presented recurrence of the synostosis in 4 years of monitoring. They reported a mean supination of 26° and a mean pronation of 45°. Kao et al.11 described the use of a free adipofascial inguinal flap, interposed after resecting the synostosis in an isolated clinical case report. The patient was a 12-year-old girl who suffered bilateral radioulnar synostosis, with a fixed pronation of 90° in the left forearm and 70° in the right. The authors operated on the left forearm and obtained a supination of 70° and a pronation of 50°, after a monitoring period of 28 months.
In summary, we present a case of Alagille's syndrome suffering significant multisystemic involvement and associated to bilateral proximal radioulnar synostosis which did not produce a considerable functional deficit. The authors believe that, under these circumstances, the best approach is a conservative one.
Conflict of interestsThe authors have no conflict of interests to declare.
Please cite this article as: Couceiro J, Gómez B, Sanmartín M. Síndrome de Alagille asociado a sinostosis radiocubital proximal: caso clínico y revisión de la literatura. Rev Esp Cir Ortop Traumatol. 2015;60:81–85.