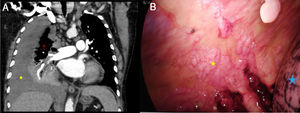
A 70-year-old man with a history of paroxysmal atrial fibrillation and COVID-19 pneumonia who required admission to the ICU for 30 days. One month later, he presented dyspnoea and orthopnoea. A lung CT (Fig. 1A) showed a predominantly right bilateral pleural effusion. Surgical evacuation was decided, given the volume of perfusion. The patient entered the operating room with severe dyspnoea and 88% oxygen saturation. General anaesthesia was performed with a 37Fr double lumen tube. The patient's blood oxygen fell during selective blockade of the right lung, but improved when the haemothorax was drained. After evacuation, multiple pleural implants forming clusters and a necrotic implant in the posterior parietal pleura were observed (Fig. 1B). This suggests that the patient had an undiagnosed tumour that had progressed rapidly during bilateral COVID-19 pneumonia.
(A) Coronal CT of pulmonary arteries showing right pleural effusion (yellow star) causing compressive atelectasis of the underlying lung (red arrow). (B) Video thoracoscopy image (VATS) showing parietal pleural tissue with implants forming clusters (yellow star) and lung (blue star). Colour images are only shown in the online version of the article.
Please cite this article as: López Herrero R, Álvarez Fuente E, Sánchez Quirós B, Román García P. Hemotórax masivo tras neumonía bilateral por COVID-19. Rev Esp Anestesiol Reanim. 2021;68:552.