Since its first description in china in January 2020, COVID-19 pandemia outbreak has affected health organization and conventional care in all settings as wards, intensive care and surgery. Hip fracture patients usually are older and have a lot of comorbidities. This type of patients benefit from early surgery. However, surgery in COVID-19 patients with active infection is associate with bad outcomes and mortality. We present three patients with COVID infection undergoing hip fracture surgery. Surgery was performed tree weeks after admission. Despite have risk factor (old age, arterial hypertension, elevated inflammatory parameters) the outcome was good and were discharged from hospital without events.
La pandemia COVID-19 y su diseminación desde la descripción de los primeros casos en China en enero de 2020, ha condicionado la organización sanitaria y la asistencia convencional, tanto en sala de hospitalización como en unidades de cuidados intensivos (UCI), o consultas y actividad quirúrgica. Los pacientes con fractura de cadera, habitualmente ancianos y pluripatológicos, se benefician de una intervención precoz, sin embargo, la cirugía en presencia de infección SARS-CoV-2 activa, parece condicionar una morbimortalidad elevada. Presentamos 3 casos de pacientes ancianos con COVID-19 y fractura de cadera, intervenidos tras 3 semanas de evolución y con presencia de PCR positiva. A pesar de factores pronósticos de gravedad (edad, hipertensión arterial y marcadores de inflamación elevados) el postoperatorio fue el habitual y fueron dados de alta del hospital.
Since mid-April 2020, more than 2.4 million cases of COVID-19 (infection caused by coronavirus 2 and associated with severe acute respiratory syndrome, SARS-CoV-2) have been reported.1
Although people of any age are at risk of infection and serious disease, the probability of very serious COVID infection and death is higher in people over 65 years of age, while a mortality rate of 75% has been described in patients aged over 80 years admitted to the ICU.2 The incidence of hip fracture in the elderly and the benefits of early surgery are known; however, surgery in patients with COVID-19 appears to be associated with high morbidity and mortality.3 We present 3 cases of elderly patients with hip fracture and COVID infection in whom surgery was successful.
Case reportsCase 1An 88-year-old woman with a body mass index (BMI) of 22, and a history of hypertension, stage IIIb chronic renal failure, obesity, dyslipidaemia, hyperuricaemia, osteoporosis, depressive syndrome, and cognitive dysfunction. She had previously undergone surgery for hip and knee arthroplasty. Her background treatment consisted of olmesartan, amlodipine, hydrochlorothiazide, carvedilol, furosemide, escitalopram and paracetamol. She had an allergy to ibuprofen.
After falling at home, she was diagnosed with a Rorabeck IIa supracondylar periprosthetic femoral fracture above a total knee prosthesis. The patient reported contact with household members who presented symptoms of fever and cough. Nasopharyngeal swab polymerase chain reaction (PCR) testing for SARS-COV-2 infection performed in our hospital was positive. She was admitted to the COVID ward and managed conservatively with orthopaedic treatment. The patient presented a dry cough with no dyspnoea or work of breathing, and was afebrile. Arterial O2 saturation (SatO2) was good without the need for oxygen therapy, and chest radiological showed no signs of SARS-COV-2 infection. Oral treatment with hydroxychloroquine 400mg/12h/1 day and 200mg/every 12h/5 days was started, as per the hospital protocol. On the third day after admission, she presented arterial hypotension and acute anaemia, which responded well to fluid therapy and red blood cell (RBC) transfusion; a concomitant urinary infection was treated with ceftriaxone. Labs are shown in Table 1. Given the good evolution of the patient, surgery was scheduled for day 18 after admission, even though the PCR was still positive. Spinal anaesthesia was performed at the L3–L4 level with a simple puncture, administering 10mg of 0.5% isobaric bupivacaine. Haemodynamic and respiratory patterns remained stable throughout surgery. The patient required transfusion of 2 units RBC and small boluses of phenylephrine up to a total dose of 0.6mg. Immediate postoperative care was performed in the operating room for 2h, after which she was transferred to the ward. Subsequent evolution was uneventful, and 7 days later the patient was discharged to a nursing home.
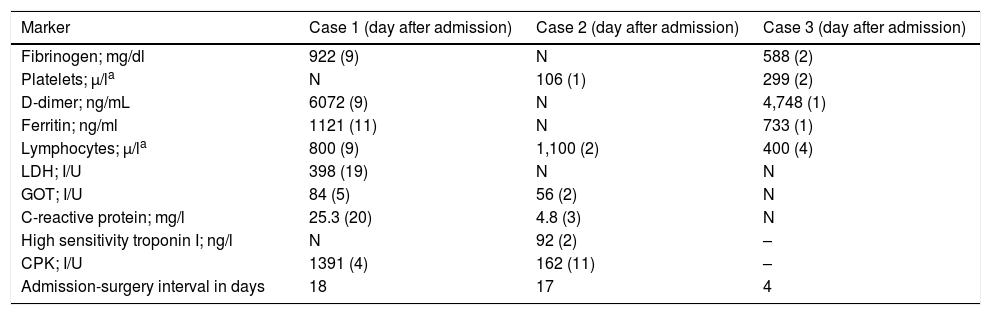
Maximum or minimum lab markers of poor prognosis and day of onset after admission.
| Marker | Case 1 (day after admission) | Case 2 (day after admission) | Case 3 (day after admission) |
|---|---|---|---|
| Fibrinogen; mg/dl | 922 (9) | N | 588 (2) |
| Platelets; μ/la | N | 106 (1) | 299 (2) |
| D-dimer; ng/mL | 6072 (9) | N | 4,748 (1) |
| Ferritin; ng/ml | 1121 (11) | N | 733 (1) |
| Lymphocytes; μ/la | 800 (9) | 1,100 (2) | 400 (4) |
| LDH; I/U | 398 (19) | N | N |
| GOT; I/U | 84 (5) | 56 (2) | N |
| C-reactive protein; mg/l | 25.3 (20) | 4.8 (3) | N |
| High sensitivity troponin I; ng/l | N | 92 (2) | – |
| CPK; I/U | 1391 (4) | 162 (11) | – |
| Admission-surgery interval in days | 18 | 17 | 4 |
CPK: creatine phosphokinase; GOT: glutamic oxaloacetic transaminase; LDH: lactate dehydrogenase; N: no data.
A 93-year-old woman with a BMI of 39.5 and a history of arterial hypertension, obesity, ischaemic stroke 3 years prior, bronchial asthma, duodenal ulcer, severe spondylarthrosis with L4 vertebral compression, and chronic renal failure. She was under treatment with acetylsalicylic acid, transcutaneous fentanyl, bromazepam, omeprazole, inhaled bronchodilators (salbutamol, budesonide, ipratropium), furosemide, metamizole, and desvenlafaxine. She was admitted to the emergency room after suffering an accidental fall and reported pain and functional impairment in lower limbs. The radiological study revealed a basicervical fracture of the right hip. Screening for SARS-CoV-2 with nasopharyngeal swab PCR was positive, and the patient was transferred to the COVID ward. On admission, she received conservative treatment for the fracture, hydroxychloroquine for 5 days and ceftriaxone for 8 days. Both respiratory and hemodynamical parameters remained stable, except for acute anaemia that required transfusion of 1 unit RBC. Labs are shown in Table 1. On day 17 of admission, we decided to go ahead with surgery, despite persistence of positive PCR. Spinal anaesthesia was performed with 9mg of isobaric bupivacaine at the level of L2–L3. Puncture in the lateral decubitus position was difficult due to spondylarthrosis and scoliosis. During surgery, she presented arterial hypotension, which was treated with fluid replacement and transfusion of 1 unit RBC. Postoperative care was performed in the operating room for 95min, after which she was transferred to the ward. During her hospital stay she presented a urinary infection which resolved after antibiotic treatment (ciprofloxacin). After 8 days of evolution, she is awaiting discharge home.
Case 3A 91-year-old male patient with a BMI of 30 and a history of hypertension, dyslipidaemia, heart failure, cognitive impairment, Parkinson's disease and anxiety-depressive syndrome, receiving chronic lorazepam, risperidone, sertraline, levodopa, carbidopa, entacapone and furosemide. He was admitted to the emergency room after presenting intense pain in the left hip for 2 days, denying accidental fall or trauma. The radiological study revealed a subcapital fracture of the left hip. Screening for SARS-CoV-2 with nasopharyngeal swab PCR was positive, and the patient was transferred to the COVID ward. After admission, the chest radiographic study showed bilateral parenchymal infiltrates, but he remained asymptomatic. He was treated with hydroxychloroquine and ceftriaxone. A report was subsequently obtained from his nursing home showing PCR positive for SARS-CoV-2 15 days before hospital admission. Surgery was scheduled 5 days after admission, and was performed under spinal anaesthesia at the level of L3–L4 with 11mg of 0.5% isobaric bupivacaine. The procedure was uneventful. Immediate postoperative care was performed in the operating room for 60min, requiring transfusion of 1 unit RCB. He was later transferred to the ward. Seven days later, he was discharged to a nursing home. Labs are shown in Table 1.
DiscussionThe SARS-CoV-2 pandemic has compelled hospitals to re-organise their units and services, establishing 2 hospitals within each centre, one for COVID patients and one for non-COVID patients, each in a different location, with different pathways and different healthcare organization from emergency admission to hospital discharge.1,2 This has had a major impact on surgery: many scheduled interventions have been postponed or cancelled, and only emergency procedures are performed. This has also greatly affected the care protocol for hip fracture in elderly patients. Given the comorbidities and frailty commonly associated with this type of patient, guidelines recommend performing surgery within 72h of admission, unless the injury has been caused by or occurs concomitantly with another condition.3–5 Prompt surgery has significantly improved outcomes in terms of both postoperative complications (atelectasis, pneumonia, pressure ulcers, pulmonary embolism, urinary infections, delirium, etc.) and mortality.
COVID-19 infection appears to progress through 3 stages: an initial stage of viral replication in the upper airway lasting around 7–8 days in which it is more frequent to find positive PCR tests; a second inflammatory stage (with cytokine storm) with varying degrees of pulmonary involvement (from asymptomatic cases with no radiological manifestations to bilateral interstitial pneumonias and ARDS), and a third recovery phase with or without sequelae.6 We now know that many patients, particularly children and young people, remain asymptomatic, while patients older than 65 years present more severe forms of the disease, with mortality approaching 90% in patients older than 80 years who require mechanical ventilation for respiratory failure. There appears to be evidence that a history of disease (diabetes, ischaemic heart disease, peripheral vascular disease, arterial hypertension, obesity) is a risk factor for severe forms linked to phenomena of vasculitis and thrombosis.7,8 We present 3 reports of patients with positive nasopharyngeal swab PCR in whom postoperative evolution after hip fracture surgery was uneventful. In all cases, clinicians had to decide between performing surgery as soon as possible and risking development of pneumonia, or delaying surgery until symptoms had improved (ideally with a negative PCR) and risking postoperative complications. In the first 2 cases, surgery was performed after the patients had been hospitalised for more than 15 days and PCR was still positive. During this time the patients did not develop respiratory symptoms and were treated with hydroxychloroquine and 3rd generation cephalosporin, but no antiviral treatment. However, they did present elevated acute phase reactants (ferritin, CRP, lymphopenia, and D-dimer), which are inflammatory and prognostic markers of COVID-19.9 In the first case, D-dimer and ferritin values were high, with significant lymphopenia on day10 of admission; nevertheless, the patient showed no clinical or radiological data of respiratory disease. The third case is even more interesting, since they patient presented a picture of pneumonia on admission, but remaining asymptomatic with normal blood gas levels. As the patient had tested positive 15 days previously, surgery was performed 5 days after admission (about 20 days after the first positive PCR), despite maintaining elevated acute phase reactants and significant lymphopenia. Although spinal anaesthesia has not been shown to be superior to general anaesthesia in terms of mortality, it does seem to improve morbidity, and is the technique of choice in COVID-19 patients because it does not involve aerolsolsation.10–12
In conclusion, we present 3 cases of patients with hip fracture and SARS-CoV-2 in whom surgery was performed despite the absence of negative PCR. All 3 patients made a full recovery. Although early surgery benefits these patients, it is usually best to wait at least 3 weeks due to reduce the risk of mortality that appears to be associated with surgery in the inflammatory phase of the disease. However, in hospitalised patients with positive PCR, we can only estimate when the infection occurred and the stage of evolution of the disease. It seems advisable to initially take a conservative approach, wait for symptomatic improvement, and undertake surgery with a certain safety margin, even though this involves delaying the procedure and increasing the risk of morbidity and mortality for other causes.
Please cite this article as: Rabanal LLevot JM, Moreno Suarez FM, Merodio Gómez A, Solar Herrera A, Tejón Pérez G. Fractura de cadera en el anciano e infección por COVID-19. Descripción de 3 casos. Rev Esp Anestesiol Reanim. 2021;68:99–102.