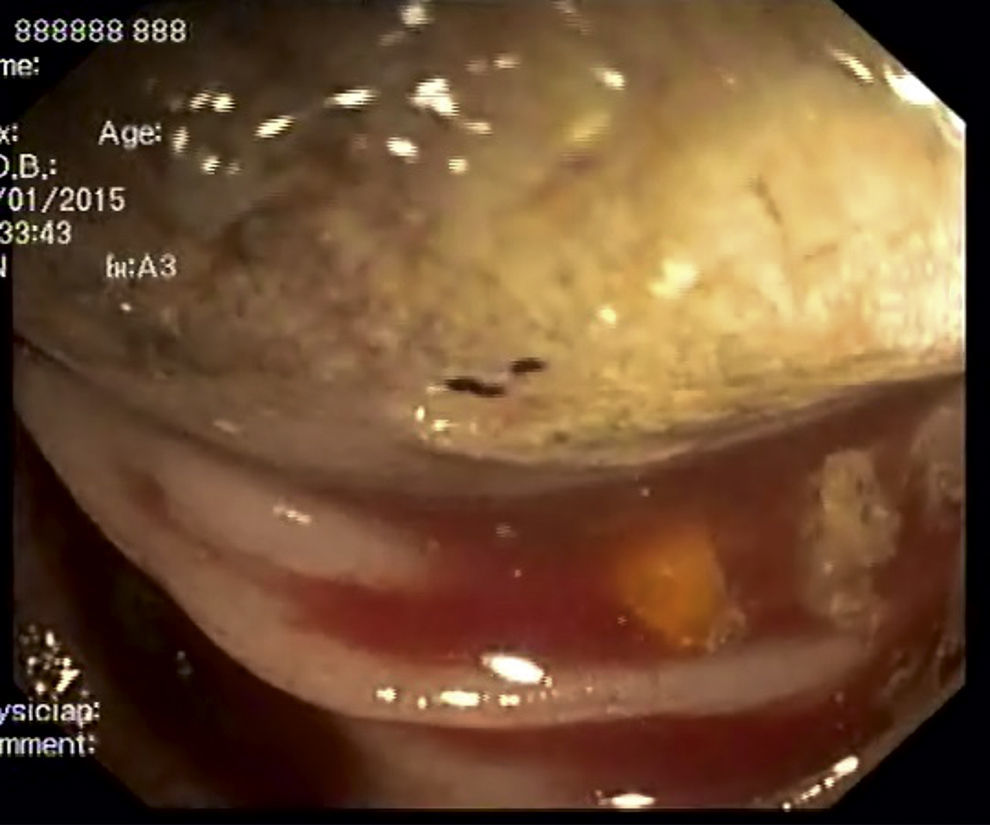
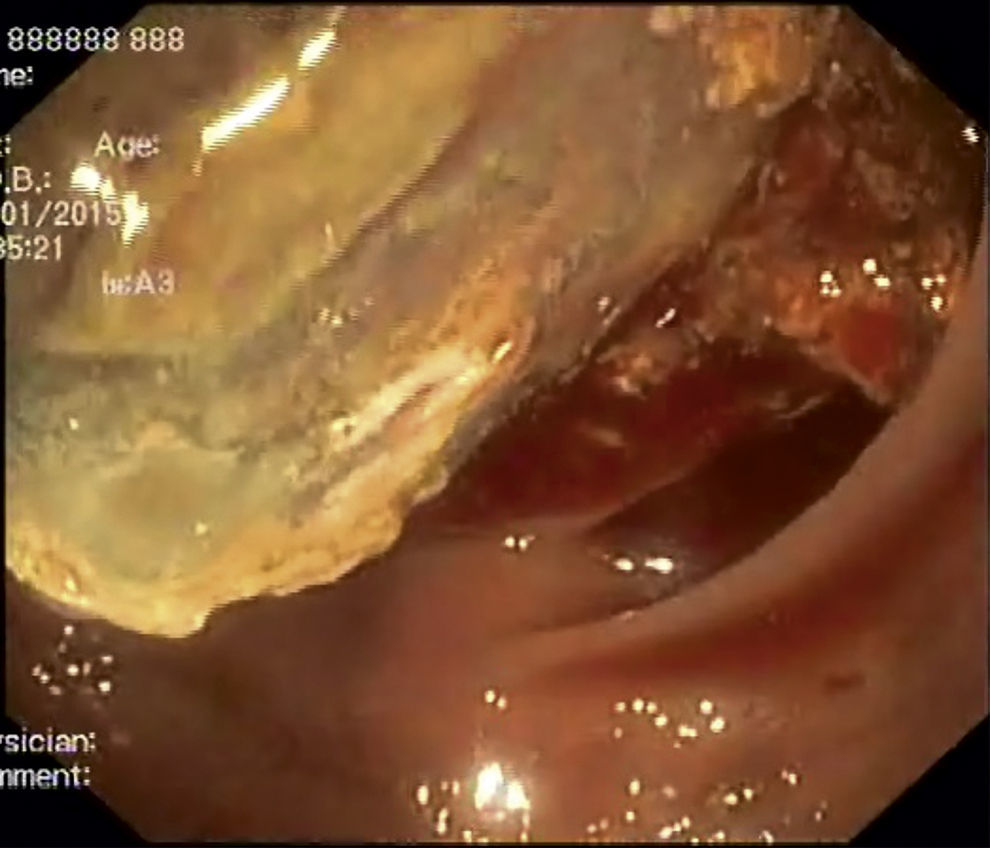
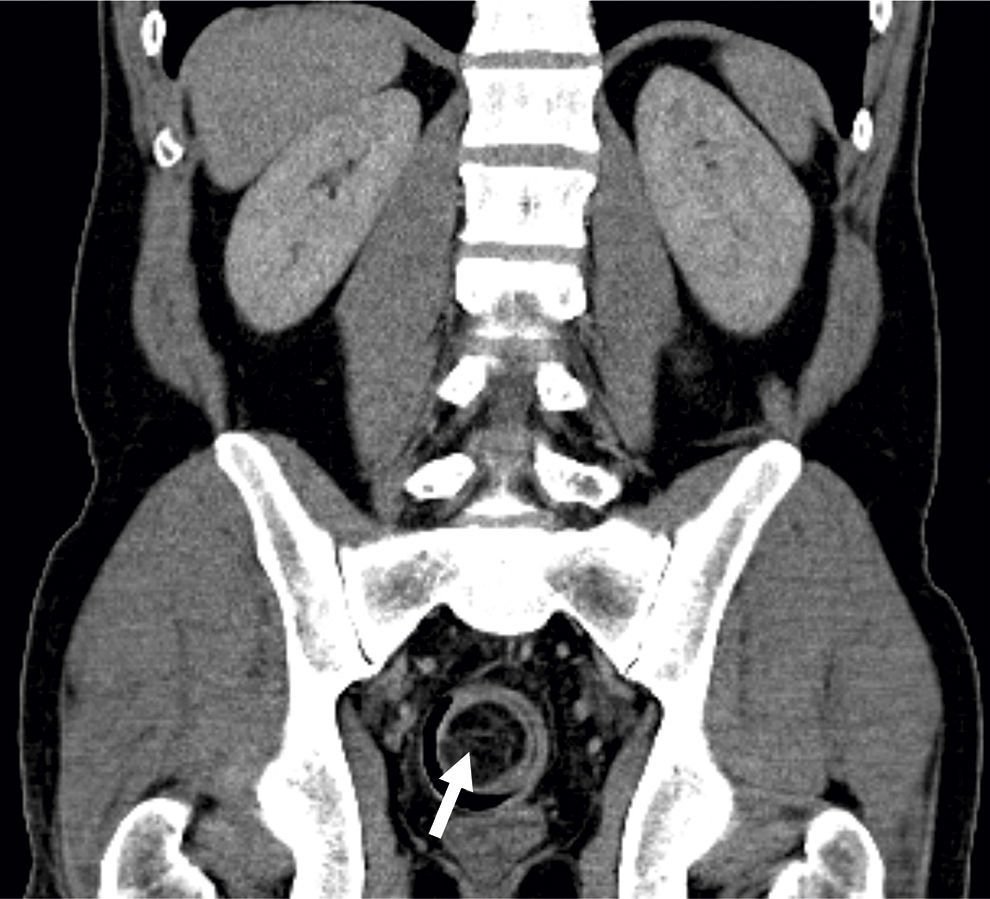
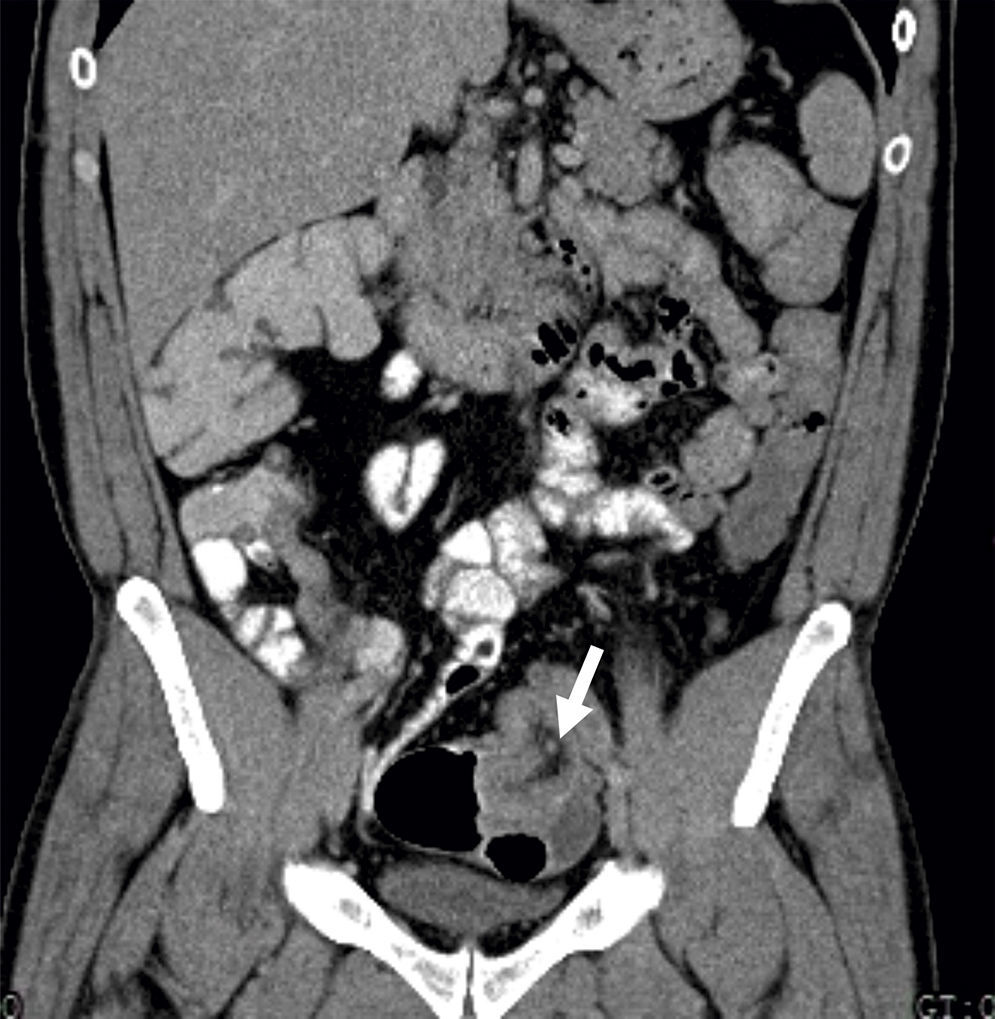
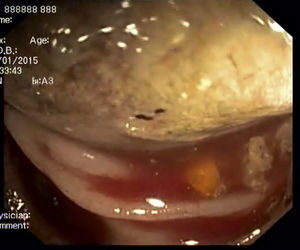
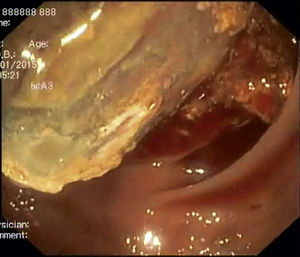
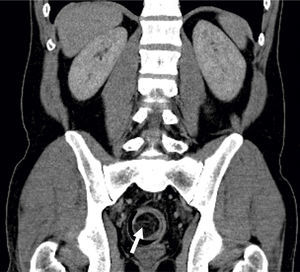
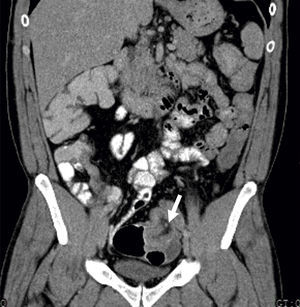
A 41-year-old man, was admitted in the emergency department due to repeated lower abdominal pain, constipation and hematochezia with one month of evolution. His past medical history was irrelevant. The physical examination and laboratory data were normal. The patient denied anorexia, weight loss and fever. A colonoscopy revealed an extensive mass with a regular mucosal surface with ischemia and ulceration at the distal top (Figs. 1 and 2), in the descending colon. This lesion occupied more than 2/3 of the circumference and conditioned lumen stenosis. Biopsies revealed inflammatory changes. An abdominal and pelvic computed tomography (CT) showed colocolic intussusception (Fig. 3), in the terminal portion of the descending colon, caused by a lipomatosus mass with 7cm×4cm larger diameter (Fig. 4). The patient underwent a segmental colon resection by laparoscopy. The histological examination of the surgical specimen revealed a partially necrotic submucosal lipoma.
The authors describe this case due to its rarity. Colonic lipoma is a very rare benign tumor, however it is the second most common benign tumor of the colon with an incidence between 0.2 and 4%.1 In 90% of these cases the origin of the lipoma is confined to the submucosal layer.2 It is more frequently found in the right colon by colonoscopy. These lesions are usually asymptomatic and do not require specific treatment. Lipomas larger than 4cm, are considered giant and are symptomatic in 75% of cases.3 Symptoms are usually abdominal pain, bleeding, colonic obstruction and intussusception. The intussusception is a rare complication that requires a differential diagnosis with a malignant lesion. Literature describes that lipomas larger than 2cm should be removed due to colonic intussusception risk.4
The treatment for symptomatic lipomas has typically included surgical resection, but the use of minimally invasive techniques such as endoscopic therapy is increasing.4 Thus, various endoscopic procedures, including snare resection, endoscopic submucosal dissection, unroofing, endoloop technique and a combination of the last two, the “grasp-to-retract, ligate, unroof, and let-go” technique have been introduced recently for safe resection4.4,5 In this case, the patient underwent a surgical resection because he presented with an acute colonic obstruction from intussusception.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that no patient data appear in this article.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
AuthorshipFilipa Ávila did the writing of the manuscript. All authors were responsible for the revision of its contents.
Conflicts of interestThe authors have no conflicts of interest to declare.