To review the treatment of hidradenitis suppurativa and the role of etanercept in terms of efficacy and safety.
MethodsDescriptive, cross-sectional and retrospective study. Patients diagnosed with hidradenitis suppurativa who were treated with etanercept (indication not on its Summary of Product Characteristics) until June 2009 were included in the study. The study variables were: age, sex, treatments before and after etanercept, response, adverse effects, duration and reason for stopping treatment.
ResultsAntibiotics, contraceptives, corticosteroids, isotretinoin or oral sulfones were used as the first-line treatment. When patients no longer responded to these treatments, the use of etanercept was requested. It was well tolerated but it only led to an initial improvement. It was, therefore, suspended. The options employed included the following: corticosteroids, antibiotics, isotretinoin, contraceptives, immunosuppressive drugs and antiandrogens. Patients who were treated with adalimumab and infliximab as an alternative treatment found that their lesions flared up. Surgery was considered as a last option. At present, the majority of patients are undergoing maintenance therapy with oral treatments.
ConclusionsThe treatment of hidradenitis suppurativa is based on antibiotics, corticosteroids or contraceptives. These are able to control the disease temporarily. Etanercept is well tolerated but it only results in an initial improvement. Similar results have been found with infliximab and adalimumab. The affected areas can be controlled with surgery. Therefore, the role of TNF inhibitors in the treatment of hidradenitis suppurativa is controversial.
Revisión del tratamiento de la hidradenitis supurativa y papel de etanercept en términos de eficacia y seguridad.
MétodosEstudio descriptivo transversal retrospectivo. Se incluyeron pacientes diagnosticados de hidradenitis supurativa tratados con etanercept (indicación fuera de ficha técnica) hasta junio de 2009. Las variables estudiadas fueron: edad, sexo, tratamientos anteriores y posteriores a etanercept, respuesta, efectos adversos, duración y motivo de suspensión.
ResultadosComo primera línea de tratamiento se emplearon antibióticos, anticonceptivos, corticoides, isotretinoína o sulfonas orales. Ante la falta de respuesta mantenida se solicitó el uso de etanercept. Fue bien tolerado, pero únicamente permitió obtener una mejoría inicial, por lo que fue suspendido. Las siguientes opciones que se emplearon incluyeron corticoides, antibióticos, isotretinoína, anticonceptivos, inmunosupresores y antiandrógenos. Los pacientes tratados con adalimumab e infliximab como alternativa presentaron reactivación de las lesiones. Como última opción se plantea el tratamiento quirúrgico. Actualmente, la mayoría de los pacientes están en terapia de mantenimiento con tratamientos orales.
ConclusionesEl tratamiento de la hidradenitis supurativa se basa en antibióticos, corticoides o anticonceptivos con los que se obtiene un control transitorio de la enfermedad. El etanercept es bien tolerado, pero su eficacia se limita a una mejoría inicial. Se han obtenido resultados similares con infliximab y adalimumab. La cirugía permite obtener un control en la zona intervenida. Por tanto, el papel de los anti-TNF en el tratamiento de la hidradenitis supurativa es controvertido.
Hidradenitis suppurativa (HS) is a chronic and recurrent inflammatory disorder of the apocrine sweat glands characterised by the presence of deep and painful follicular nodules, papules, pustules and abscesses, located mainly in the armpits, groin and perianal region.1,2 The disease course is variable, and lesions frequently progress to fibrosis, suppuration, deformation and hypertrophy.3
The prevalence of HS is around 1%–4%.1,4 It affects more women than men, with a ratio of 3:1, and generally occurs between puberty and 40 years with a mean age-of-onset of 23 years.4
The aetiology and pathogenesis of HS are unknown. It is believed that the disease develops after occlusion of the hair follicle as a result of a defect in the maturation of these cells that prevents the shedding of follicular epithelium. The occlusive folliculitis triggers an inflammatory reaction resulting in tissue destruction and epithelial damage. The situation is frequently aggravated by bacterial infections.1
Treatment of HS is complex, as there are no specific treatments for this disease, and those currently employed are ineffective in most cases.2,5 Antibiotics, corticosteroids, immunosuppressants, retinoids, topical antiseptics and anti-androgens are the main treatments for the early stages of the disease.4 Moreover, therapeutic efficacy is limited as the disease progresses, necessitating the use of alternatives.4
However, tumour necrosis factor alpha (TNF) inhibitors have appeared as an alternative for patients with moderate to severe HS,6 although there is still no conclusive data on the effectiveness of these drugs in HS.7–9
In this study we focused on the role of etanercept, a TNF inhibitor, with approved indications for the treatment of autoimmune diseases.10 Several studies have shown efficacy in the treatment of HS.11–14 Others, however, show a limited role for etanercept in the treatment of this disease.5,15 Therefore, our aim was to study the effectiveness of etanercept for treatment of HS in 6 patients treated at the Hospital Costa del Sol (Marbella).
MethodsIt was a retrospective cross-sectional study in a level 2 hospital. The territorial scope of the hospital is the Costa del Sol health district comprising 358433 inhabitants (according to the census of 1 January 2008).
Patients were selected through the pharmacy department's outpatient dispensing program. A search was made for etanercept prescriptions assigned to the dermatology service up to June 2009 for use in unapproved indications by the Agencia Española de Medicamentos y Productos Sanitarios (Spanish Agency of Medicines and Health Products). The diagnosis of these patients was confirmed from the medical records, and 6 patients who received etanercept for the treatment of HS were identified.
The variables recorded were age, sex, previous surgical and pharmacological treatments and those following the use of etanercept, doses of etanercept, therapeutic response, time to response assessment, adverse effects, treatment period, and reasons for suspension.
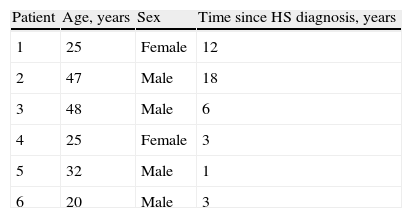
ResultsThere were 6 patients treated and followed up for HS in the dermatology department of the Hospital Costa del Sol, Marbella (Table 1).
Etanercept was not used as a first-line treatment in any of the patients. It was used as a second-line treatment in 1 patient, as a third-line treatment in 3 patients, a fifth-line treatment in 1 patient, and a sixth-line treatment in 1 patient.
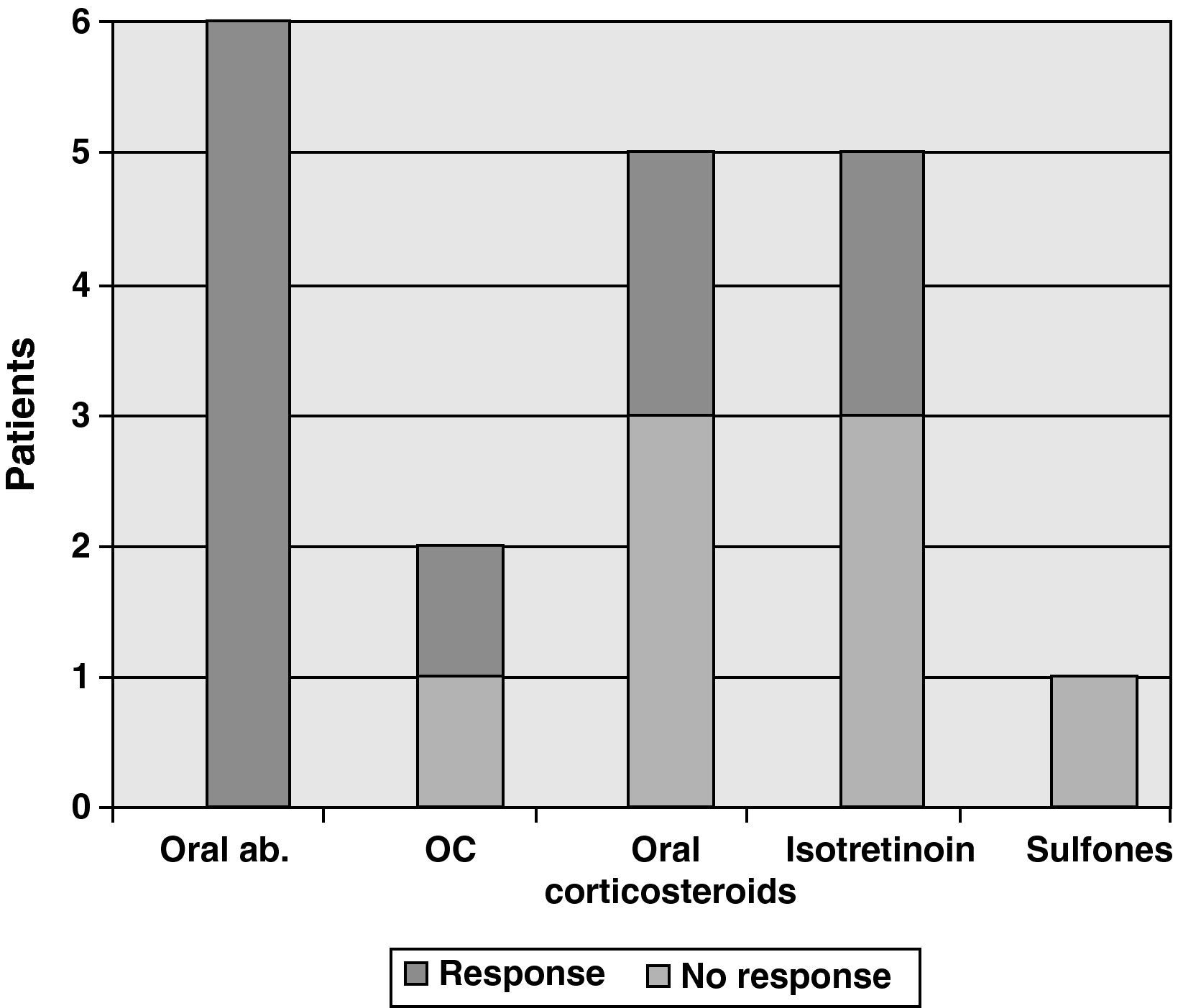
The first-line treatments included antibiotics, steroids, contraceptives, isotretinoin and oral sulfones. None of the patients could control the disease and prevent new lesions with these conventional drugs. However, some improvement was made in the treatment of exacerbations and they led to an initial transient improvement in some cases. Fig. 1 has a list of patients, previous treatments to etanercept and response, which is defined as acute infection control in the case of oral antibiotics and initial improvement in the rest of the treatments.
In the absence of sustained response to previous alternatives, treatment with a modulating factor of the inflammatory response was suggested. Etanercept was administered at a starting dose of 100mg/week subcutaneously. In 2 patients, the dose was reduced to 50mg/week after an initial improvement assessed at 16 and 20 weeks, respectively. One of these 2 patients, after a week with a dose of 50mg/week, presented with an exacerbation of the disease and returned to the initial dose of 100mg/week.
An initial improvement was seen in 4 patients, with new lesions appearing in a time ranging between 3 and 8 months. The other 2 patients experienced no improvement whatsoever, and so were considered as non-responders.
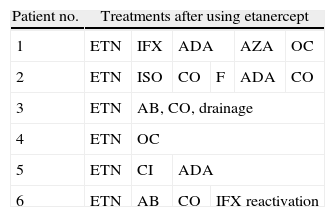
The treatments used subsequently to etanercept, except for the current treatment, are shown in Table 2.
Treatments After Using Etanercept.
| Patient no. | Treatments after using etanercept | |||||
| 1 | ETN | IFX | ADA | AZA | OC | |
| 2 | ETN | ISO | CO | F | ADA | CO |
| 3 | ETN | AB, CO, drainage | ||||
| 4 | ETN | OC | ||||
| 5 | ETN | CI | ADA | |||
| 6 | ETN | AB | CO | IFX reactivation | ||
AB: oral antibiotics; ADA: adalimumab; AZA: azathioprine; CI: corticosteroid infiltration; CO: oral corticosteroids; ETN: etanercept; F: finasteride; IFX: infliximab; ISO: isotretinoin; OC: oral contraceptives.
Currently, 4 patients are receiving the treatment they had before starting etanercept, 3 of them without lesions, and 1 with suppurative lesions.
Other TNF inhibitors, adalimumab and infliximab were also administered to 4 of the 6 patients, with all cases having presented inflammatory activity in the lesions.
Adverse reactions related to the medication were seen in 2 patients. The 1st patient presented sulfone-related anaemia, gastritis due to azathioprine and angio-oedema, tachycardia and joint pain associated with treatment with infliximab. The 2nd patient presented mastitis and presyncope episodes associated with the use of adalimumab.
Additionally, 66% of the patients received surgical treatment. Of these, 50% did so before treatment with etanercept. The surgery was not effective in 25% of the cases, while improvement was observed in the treated area in 75%. Of patients who did not receive surgical treatment, 33% are waiting to be operated upon.
DiscussionThe results obtained show that there is no effective therapy for the treatment of HS. All patients followed a similar treatment with similar results.
As a first-line treatment, the use of antibiotics, contraceptives, steroids, isotretinoin and/or oral sulfones showed some initial transient improvement in the lesions. No case achieved adequate control or could prevent the occurrence of new lesions. Oral antibiotics are effective in the treatment of acute infection.
Etanercept was used for the treatment of HS after at least one other treatment option had been used. It was well tolerated, but only yielded an initial improvement in the lesions, which prompted the discontinuation of the treatment after a variable period that depended on the patient.
After treatment failure, subsequent treatments were administered according to each patient. Some of the cases were treated with other TNF inhibitors, like infliximab and adalimumab, with a similar response to that obtained with etanercept.
Currently, most patients are receiving the treatment they had prior to the use of etanercept: antibiotics, steroids or oral contraceptives.
Surgery is an alternative in patients with HS who gain no control of their disease with drug therapy. However, the efficacy of this procedure is restricted to the treated area.
In view of these results and those reported in the literature, the role of etanercept in the treatment of HS is controversial. Authors such as Trent et al.6 and Cusack et al.14 demonstrate the efficacy of etanercept in patients with HS. Other authors have shown limited efficacy in treatment with etanercept. Lee et al.5 conclude their study stating that there is minimum clinically significant evidence for the efficacy of etanercept. In the study by Pelekanou et al.,11 there was a lack of response in 1/3 of the patients (n=10), and all those who had an initial response required retreating. Giamarellos et al.12 obtained a good response in the initial control of the disease in a phase II open trial on the safety and efficacy of etanercept in HS, and mentioned the need to develop controlled trials to determine the efficacy of etanercept in HS.
A limitation of the study was the lack of use of indices to objectively appraise the response to treatment, which made it very difficult to expand the sample size with results from other hospitals.
Conflict of InterestThe authors affirm they have no conflicts of interest.
Please cite this article as: López-Martín C, et al. Respuesta parcial de etanercept en el tratamiento de la hidradenitis supurativa. Farm Hosp. 2011;35(4):189.e1–189.e4.