A 60-year-old man with a history of deep vein thrombosis (DVT) a few months earlier had received treatment with low molecular weight heparin, which was then suspended. He had no known drug allergies or any other medical or surgical history of note.
Six days earlier, he was admitted to a different hospital owing to acute fever, asthenia and dry cough. He was diagnosed with COVID-19 and bilateral pneumonia, confirmed by polymerase chain reaction (PCR) on a nasopharyngeal sample and compatible chest X-ray. Treatment was started with lopinavir/ritonavir plus hydroxychloroquine. The patient responded favourably and was discharged 48 h after admission to complete treatment on an outpatient basis.
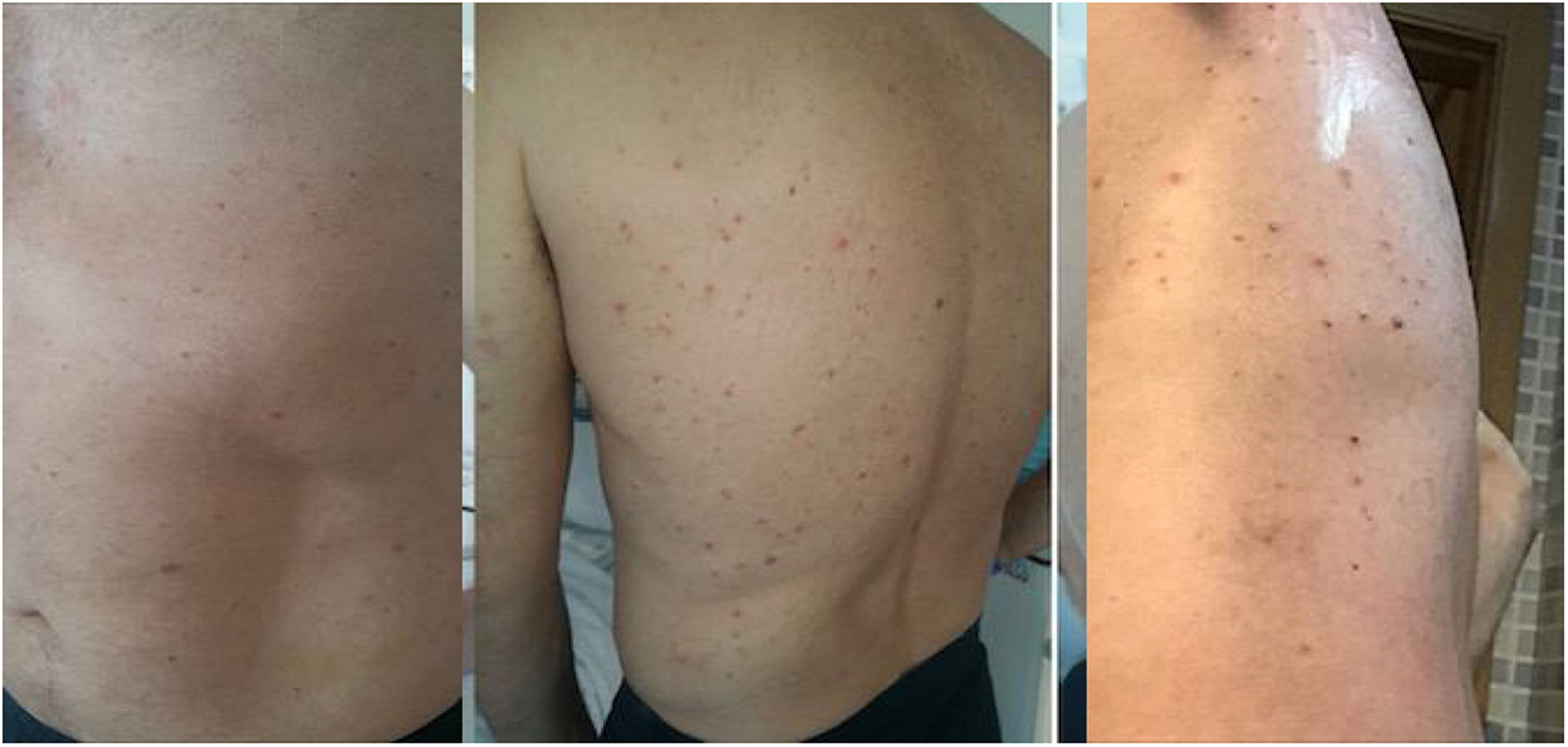
The day prior to his admission to our department, he developed a slightly pruriginous erythematous vesicular rash limited to his trunk (Figs. 1A–C). After he was assessed by Dermatology, he underwent a skin biopsy and was diagnosed with probable chickenpox, admitted to the Infectious Diseases ward and treated with intravenous acyclovir.
The patient did not recall having had chickenpox as a child. He presented neither fever nor respiratory signs or symptoms. A chest X-ray showed no evidence of pneumonia.
Clinical procedureDuring the patient’s admission, the results for the skin biopsy were received, in which an inflammatory pattern was reported. Varicella-zoster virus (VZV) serology yielded a negative result for IgM and a positive result for IgG. In addition, PCR for VZV in the biopsy sample was negative.
Given these results, acyclovir was discontinued. PCR for SARS-CoV-2 in the skin biopsy sample was ordered. This was also negative.
During his stay, the patient completed the treatment with lopinavir/ritonavir plus hydroxychloroquine that had been previously started. He remained afebrile with no respiratory signs or symptoms. The chest X-ray taken was normal and the rash resolved within a few days.
Closing remarksThe most common clinical symptoms of COVID-19 are fever, cough and dyspnoea. However, various parts of the body may also be affected, such as the heart, kidneys, central nervous system and skin.
At the start of the pandemic, there was little data in the literature on skin involvement. In a series by Guan et al.,1 published in the New England Journal of Medicine (NEJM) on 28 February, it only occurred in two patients out of a total of 1,099 patients, corresponding to a rate of 0.2%. A subsequent article by Recalcati.2 from Ospedale Alessandro Manzoni [Alessandro Manzoni Hospital] in northern Italy reported the data analysed in a series of 88 patients where 18 patients (20.4%) presented skin involvement: 14 had an erythematous rash, three had urticaria and one had a varicelliform rash. Galván et al.3 published a prospective, multicentre study with 375 patients in which they classified skin manifestations according to five patterns (maculopapular [the most common: 47%], pseudo-chillblain, vesicular, urticarial and livedo-necrotic) and established a relationship between disease severity and each of the five patterns, as well as a relationship between the pattern and the clinical course of the disease. These patterns were confirmed in subsequent publications.4–6
Our patient had a slightly pruriginous rash with a varicelliform appearance affecting the trunk, in the context of SARS-CoV-2 infection. He was diagnosed with probable chickenpox, admitted to the Infectious Diseases ward and started on treatment with intravenous acyclovir.
His rash developed in the acute phase of the infection, a few days after the onset of the viral symptoms.
His clinical course was favourable. He remained afebrile with no respiratory signs or symptoms. The chest X-ray taken did not show pneumonia. His skin lesions resolved within a few days.
FundingThe authors declare that they received no funding to conduct this study.
Please cite this article as: Goikoetxea Agirre AJ, Ibarrola Hierro M, Nieto Arana J, del Alamo Martínez de Lagos M. Lesiones eritematovesiculosas cutáneas. Enferm Infecc Microbiol Clin. 2021;39:153–154.