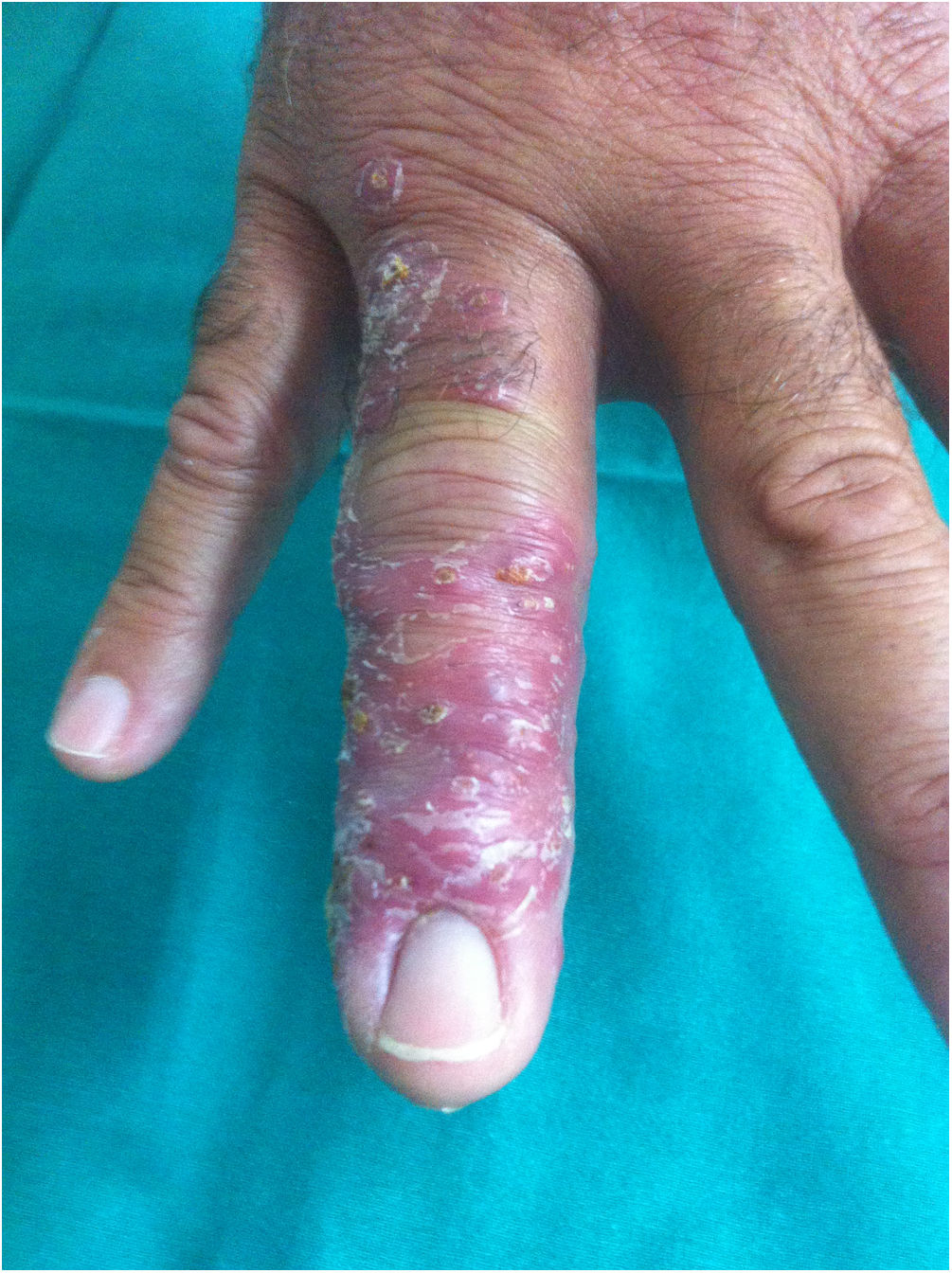
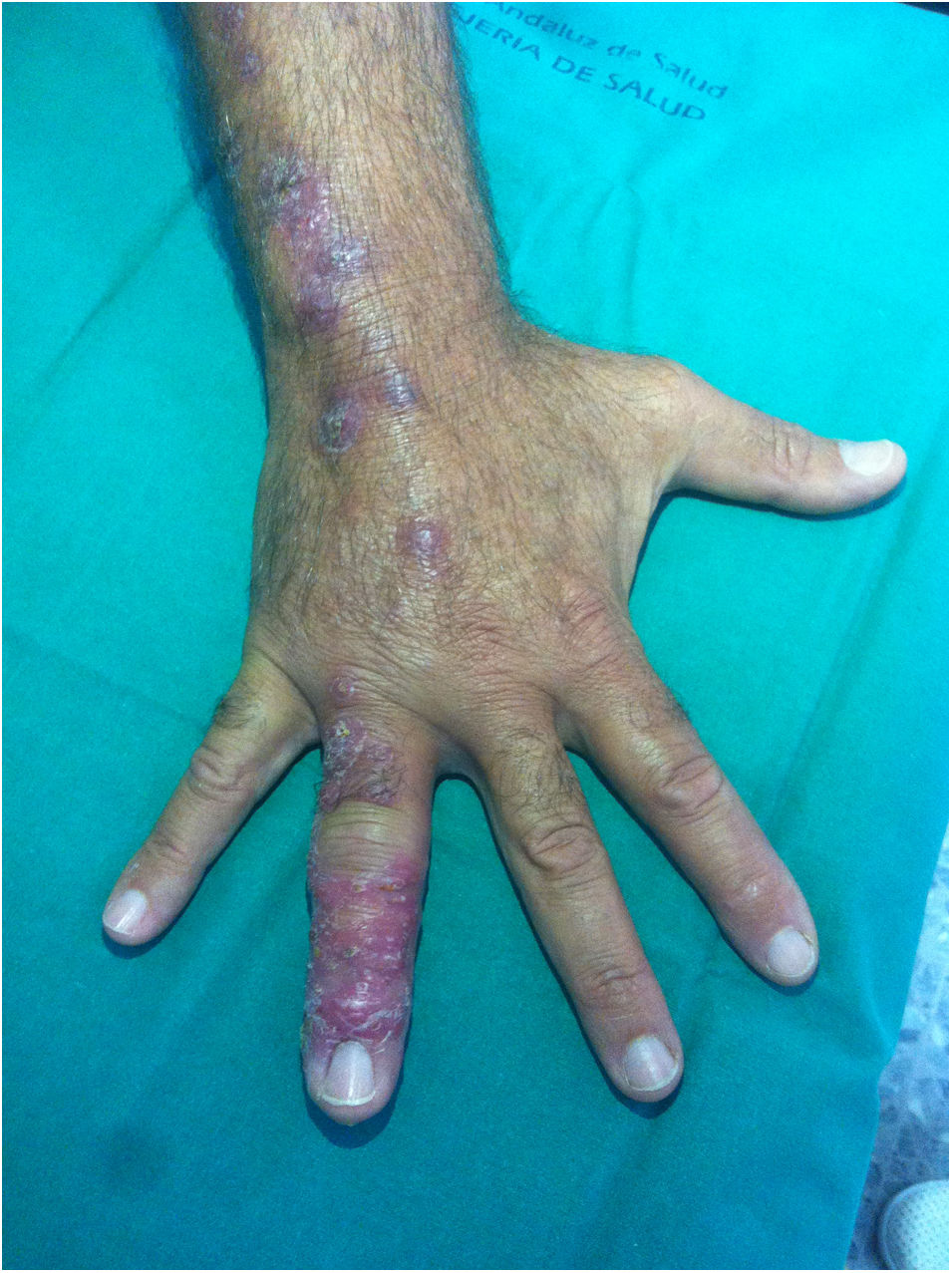
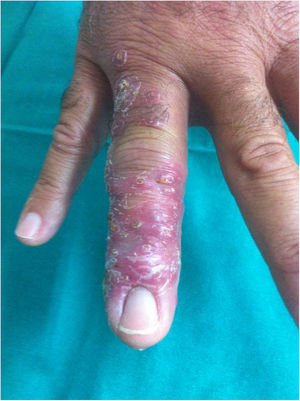
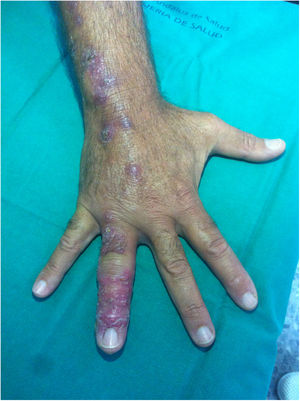
A 52-year-old man was seen due to an eight-week history of nodular skin lesions, which appeared after being pricked with a ‘spike’ at the base of the fourth finger of his right hand while hiking through scrubland. Days later, his finger swelled and painful beaded lesions appeared on the back of his hand, extending proximally to the ipsilateral forearm and arm. Throughout this time, the patient sought medical attention on multiple occasions, both with his GP and at A&E, and was diagnosed with both soft tissue infection and phlebitis. He received local treatments, ciprofloxacin 500 mg/12 h/per os (7 days) and amoxicillin-clavulanic acid 500 mg/125 mg/12 h/per os (7 days), with no improvement. He did not exhibit fever or any other symptoms. From an epidemiological standpoint, he denied handling meat or fish, maintaining aquariums or contact with animals. The physical examination was normal except for the lesions shown in Figs. 1 and 2.
The complete blood count and clinical chemistry, including transaminases and coagulation, revealed no abnormal findings. Syphilis, HBV, HCV and HIV serology tests were negative. The plain X-ray of the patient’s chest and right hand revealed no abnormalities. With a diagnosis of nodular lymphangitis secondary to sporotrichosis, two punch skin biopsies were performed, which were processed for microbiological and histological study.
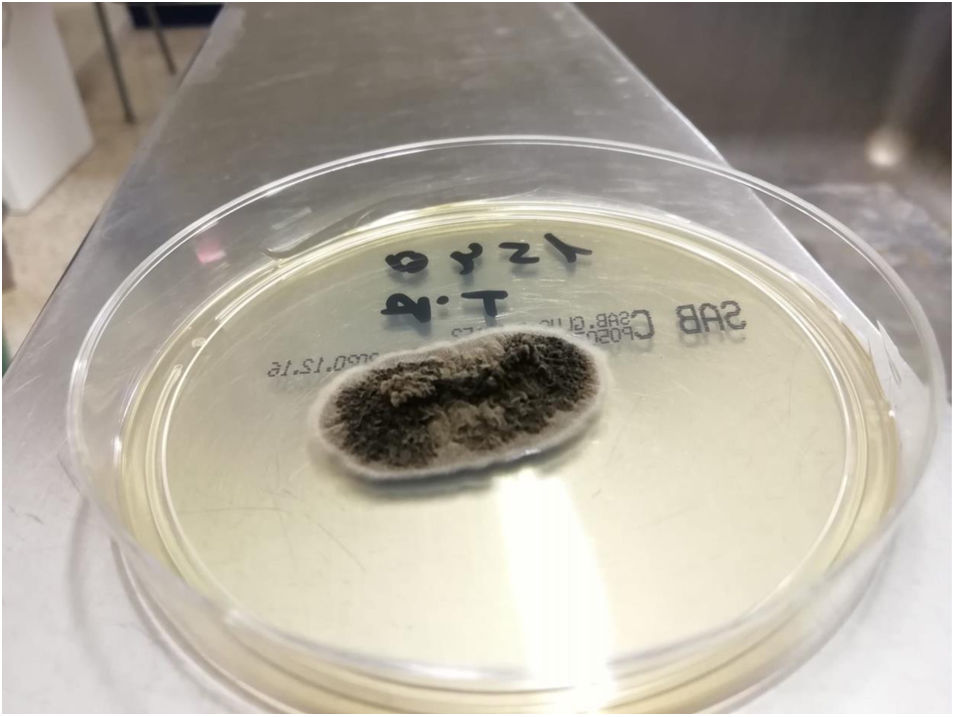
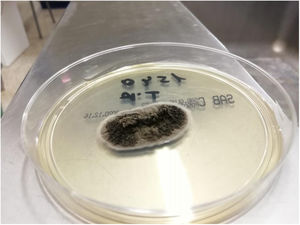
Clinical courseEmpirical treatment with itraconazole 200 mg/day/per os was started. The fungal culture isolated Sporothrix schenckii (Fig. 3). Auramine staining and mycobacterial culture were negative. The histological study identified a dense mixed inflammatory infiltrate in the superficial and reticular dermis with necrosis. PAS staining was negative and no microorganisms were found in the infiltrate. Three months after starting treatment, the patient's lesions had completely resolved. He completed the six-month regimen with no evidence of clinical or blood toxicity.
Final considerationsSporotrichosis is a subacute or chronic granulomatous fungal infection caused by fungi of the species Sporothrix schenckii. These fungi are thermally dimorphic, expressing their filamentous form in nature at temperatures below 37 °C and their yeast-like form in the tissue and at temperatures of 37 °C1. They are found all over the world in soil, plants, decomposing vegetables and several species of animal, particularly cats1,2. The infection is predominantly acquired by cutaneous inoculation with the contaminated medium, or following bites or scratches by infected cats, while infection by inhalation is rare1,2. The clinical perspective takes into consideration the cutaneous, lymphocutaneous, osteoarticular, pulmonary and disseminated forms, with lymphocutaneous sporotrichosis (lymphangitic form) being the classic and most common infection1–3. Differential diagnosis with other nodular lymphangitis-causing infections is therefore warranted: Nocardia brasiliensis infection, Mycobacterium marinum infection, Leishmania brasiliensis infection and tularaemia4–7. The epidemiological context, incubation period and certain clinical characteristics are key to a successful differential diagnosis4–7. A traumatic wound while gardening, caused by splinters or contaminated with earth or soil, should lead clinicians to suspect sporotrichosis or nocardiosis, while an injury in contact with water should point to M. marinum infection7. For hunters who develop a painful ulcer with regional lymphadenopathy and systemic symptoms days after contact with infected animals, tularaemia should be considered5,6. Purulent exudate is typical of nocardiosis5,7. A definitive diagnosis is made by isolating and identifying the causative microorganism in aspirate culture or tissue biopsy2,8. If Sporothrix schenckii is suspected, its isolation in Sabouraud agar incubated at 25 °C is recommended. Growth of the filamentous form should be observed in 5–7 days. Thermal dimorphism, with the conversion of the fungus into its yeast form, is required for definitive identification. This is achieved in enrichment cultures such as brain heart infusion (BHI) agar or blood agar incubated at 37 °C2,8. The treatment of choice for cutaneous forms and nodular lymphangitis caused by sporotrichosis consists of itraconazole 200 mg/day/per os, to be maintained for 2–4 weeks after lesion resolution, typically for a total of 3–6 months9. In conclusion, several infectious agents must be considered in the aetiology of nodular lymphangitis in order to clinically diagnose the infection. Early and precise culture-based microbiological diagnosis could prevent the incorrect use of antimicrobials and disease progression.
Please cite this article as: Rodríguez-Gómez FJ, Pérez Cáceres JA, Martínez-Marcos FJ, Merino Muñoz D. Lesiones en mano y brazo de curso tórpido tras herida punzante en un varón aficionado al senderismo. Enferm Infecc Microbiol Clin. 2021;39:516–517.