A properly immunised 7-year-old male with no prior history of note came to the emergency department due to swelling and right palpebral erythema. His signs and symptoms had started 72h earlier with a pustular lesion on his upper eyelid. He came in as his inflammatory signs had worsened despite treatment with oral amoxicillin–clavulanic acid. He reported no history of a bite or sting and no history of cutaneous herpes.
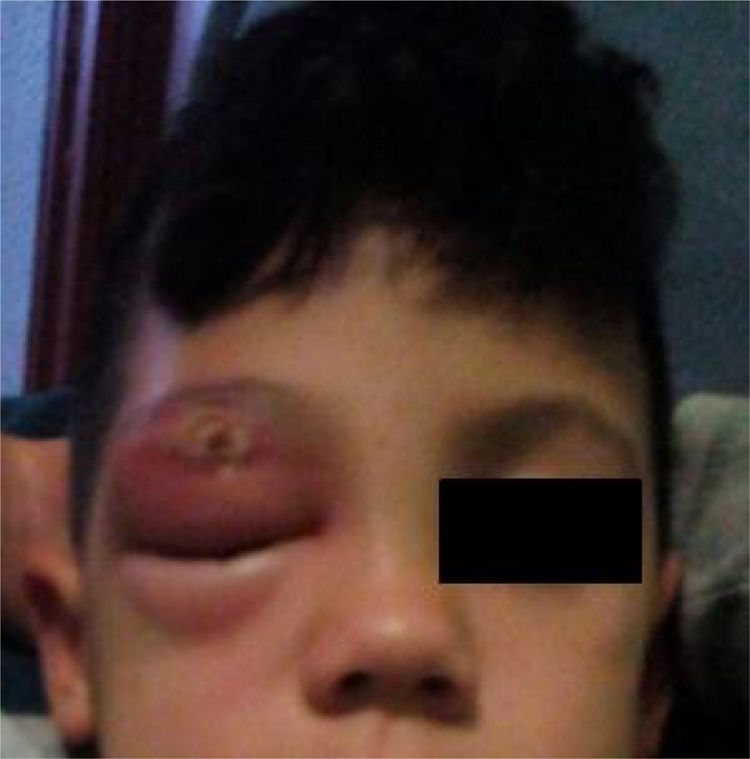
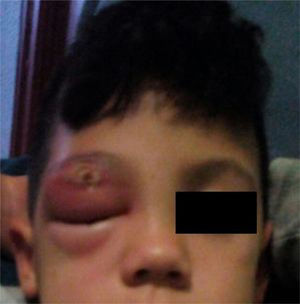
A physical examination revealed that he was afebrile with right palpebral swelling that made it difficult for him to open his eye and a crusty lesion on his upper eyelid (Fig. 1). Painful right submandibular lymphadenopathy measuring 2cm×2cm was palpated. Apart from these findings, the examination was normal. Blood testing revealed leukocytes 15,700mm–3 (neutrophils 10,000mm–3) and C-reactive protein 3mg/dl. Blood was drawn for culture. Purulent content was drained from the wound for culture as well. With a diagnosis of preseptal cellulitis, the patient was admitted with intravenous amoxicillin–clavulanic acid, and his wounds were dressed and drained. He showed a great deal of improvement following 3 days of hospitalisation and was sent home to continue on oral antibiotic therapy.
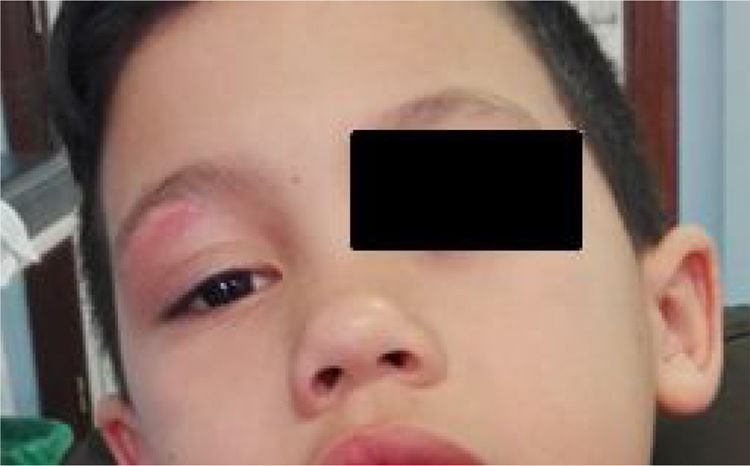
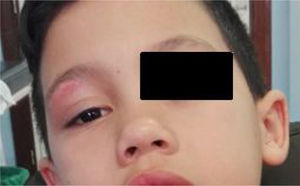
Clinical courseWhen assessed 4 days after discharge, the patient showed slight right palpebral swelling and erythema with resolution of the central lesion (Fig. 2) and disappearance of his submandibular lymphadenopathy. The culture of the exudate from the wound on blood agar and chocolate agar plates showed limited colonies of a bacterium with a chalk-white colour and a damp scent on the third day of incubation in a 37°C oven. These colonies corresponded to branched Gram-positive bacilli on Gram staining. Using MALDI-TOF® mass spectrometry, the colonies were identified as Nocardia spp. (score 1900). In view of this, the patient's treatment was switched to oral trimethoprim-sulfamethoxazole (SXT). The isolate was ultimately identified as Nocardia brasiliensis by means of complete sequencing of the 16S rRNA gene with a concordance of >99.6% with the reference sequence deposited in GenBank (CP003876, Nocardia brasiliensis ATCC-700358). An antibiogram was prepared by the agar diffusion method with E-test® concentration gradient strips (bioMérieux) with a dilution of inoculum adjusted to the 0.5 McFarland turbidity pattern and incubation at 37°C 48–72h. Resistance was interpreted according to CLSI criteria. The bacterium was sensitive to SXT, amoxicillin–clavulanic acid, ceftriaxone, imipenem, tobramycin, amikacin, clarithromycin, linezolid and minocycline and resistant only to ciprofloxacin. In follow-up at 12 weeks the patient's lesions were seen to have resolved completely with no recurrences. A basic immunology study and an NADPH activity study were ordered and their results were normal.
CommentsPrimary cutaneous nocardiosis is an uncommon disease caused by species belonging to the genus Nocardia spp. These are partially acid and alcohol fast Gram-positive bacilli and strict aerobes with a tendency towards branching. They are saprophytes that are ubiquitous in the environment, being found in land, water and organic decomposition material.1 They are transmitted through inhalation or direct inoculation into the skin and have an incubation period of less than 2 weeks.2,3
There are 2 forms of presentation: systemic disseminated and primary cutaneous. The latter accounts for 5–7% of cases; Nocardia brasiliensis is the main species involved. It affects immunocompetent children and adults and is preferentially located in the limbs, neck and face. Cutaneous nocardiosis presents in 3 clinical stages: localised skin disease, characterised by papular/crusty lesions with a tendency to ulcerate; lymphocutaneous syndrome secondary to spread to or primary infection of the lymph nodes with the potential to abscess; and the chronic form with progression to mycetomas.2,3
Often, the onset of symptoms is preceded by 2 weeks by trauma and infection through contaminated wounds or infection through insect bites.2,4,5
The diagnosis is made using Gram and culture techniques, since Nocardia spp. has a characteristic microscopy, and most species grow in typical culture media within 48–72h, with the exception of some slow-growing species. Identification on a species level is done using mass spectrometry (MALDI-TOF®) or sequencing of the 16S rRNA gene.1,2 Our case was definitively identified as Nocardia brasiliensis using the latter technique; an initial attempt achieved identification only on a genus level.
Today, SXT is the treatment of choice; surgical debridement of the lesion is also needed.6,7 As this infection tends to recur, prolonged antibiotic regimens for one month to 4 months and clinical check-ups for up to a year after antibiotic therapy is suspended are suggested.8–10
Ours was a case of cutaneous nocardiosis in an immunocompetent paediatric patient. Despite its rarity, it is important to consider this aetiology in cases of clustered papules with a tendency to abscess and accompanying lymphadenopathy with a poor response to typical antibiotic therapy and in cases in which there is a history of a contaminated wound. Proper diagnosis and treatment requires sampling for culture.
We would like to thank Dr Pablo Rojo, Dr Fernando Chaves and the Microbiology Department at Hospital Universitario 12 de Octubre in Madrid, Spain.
Please cite this article as: Llanos Alonso N, Epalza Ibarrondo C, Carretero Vicario O, Prieto Tato LM. Niño de 7 años con celulitis preseptal de evolución tórpida. Enferm Infecc Microbiol Clin. 2018;36:662-663.