Acute lymphangitis is an acute inflammatory process in healthy or anatomically altered lymphatic vessels in either immunocompetent or immunocompromised patients. It generally develops after inoculation of microorganisms into the lymphatic vessels through a skin defect or as a complication of a distal infection.1 It is commonly caused by Streptococcus pyogenes and Staphylococcus aureus; in immunocompromised patients, Gram-negative bacteria; Pasteurella multocida or Spirillum minus after dog, cat or rat bites. Less common culprits are mycobacteria, viruses, fungi, parasites, Rickettsias or non-infectious causes.1 Clinically speaking, acute lymphangitis may be: reticular, tubular, nodular, phlyctenular or necrotising.
We report here a case of tubular acute lymphangitis caused by Rickettsia sibirica mongolitimonae in Valencia, Spain.
This was a 59-year-old man with no relevant medical history who consulted in April 2019 with a four-day history of pre-syncope, general malaise, headache, arthralgia, myalgia and fever of 38.5°C. Three days before the onset of his symptoms, he developed an erythematous papule on his right leg. In the previous 48h it had become enlarged so, suspecting cellulitis, he was started on amoxicillin/clavulanic acid 500mg/8h. Despite the antibiotic, the lesion had worsened, spreading to the knee, and he had developed painful enlarged right inguinal lymph nodes.
He stated that he had not travelled outside Valencia. He had been in the countryside in an area with pigeons, rabbits, cats and dogs.
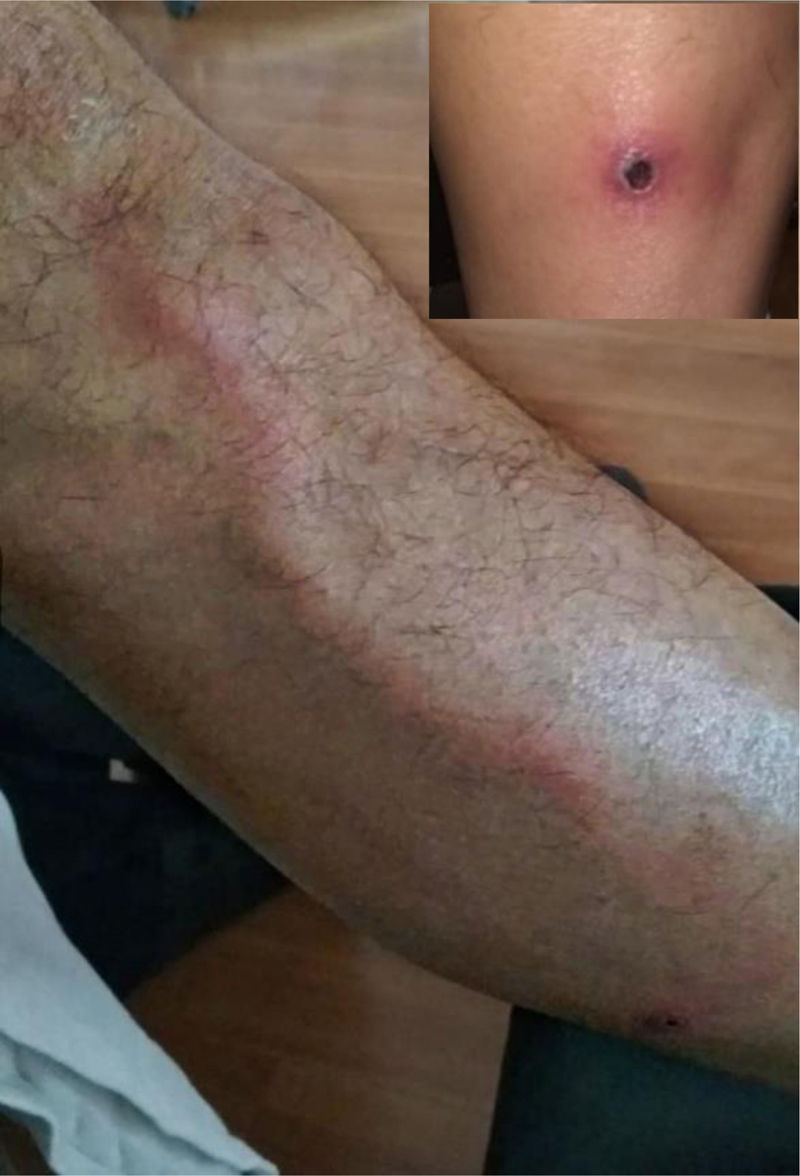
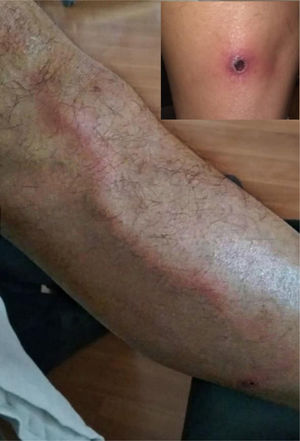
On physical examination, he was found to have a temperature of 37.6°C, the lesions shown in Fig. 1 and left inguinal lymphadenitis. He had no peripheral lesions or rashes. The only blood test finding was CRP 35mg/l. Urinalysis and chest X-ray were normal.
The appearance of the eschar raised the suspicion of rickettsiosis and he was started on treatment with oral doxycycline 100mg/12h for five days. Within 48h his temperature had returned to normal and the rest of the symptoms and lesions gradually disappeared.
For the aetiological diagnosis, serological chemiluminescence immunoassay (CLIA) (Vircell, Granada, Spain) was performed for Rickettsia conorii, C. burnetti and B. burgdorferi, which were negative. A sample of exudate was obtained from the eschar, and Real-Time PCR (Fast Track Diagnostic, Luxembourg) detected Rickettsia spp DNA. Definitive species identification was obtained by molecular sequencing of a 525bp fragment of the ompA gene, which confirmed the presence of Rickettsia sibirica mongolitimonae (99.7% similarity with sequences deposited in GenBank®).2 The serology was repeated at six weeks using CLIA and indirect immunofluorescence (IIF) (Vircell, Granada, Spain): IgG and IgM were positive against Rickettsia conorii, with evidence of cross reactions between R. sibirica and R. conorii.3
Acute tubular, trunk- or branch-like lymphangitis affects the main superficial branches of the lymphatic vessels. An erythematous plaque appears and an indurated, erythematous, warm, palpable and painful sinuous tubular cord develops (Fig. 1), extending proximally to the regional lymph nodes (lymphadenitis). It is usually accompanied by systemic symptoms: chills, fever, general malaise, headache, arthralgia, myalgia and nausea and/or vomiting. Laboratory tests may show leucocytosis, increased inflammatory parameters, and positive blood cultures.1 It generally responds to empirical oral antibiotics. Infants and small children may require hospital admission in the case of significant systemic involvement or antibiotic resistance. Further exploratory tests are not usually necessary, unless there is a lack of response or atypical aetiology is suspected.1
The presence of lymphangitis, fever and an inoculation eschar should make us suspect lymphangitis-associated rickettsiosis (LAR)4 and start treatment with doxycycline. LAR do not have a specific clinical-aetiological correlation, and can be caused by different species of Rickettsiae.5,6 One of these is R. sibirica mongolitimonae, which is involved in less than half of the published cases of LAR.6,7 This is a rare type of rickettsiosis,8 which causes lymphangitis in approximately 35% of cases.9 It tends to be transmitted in spring and summer by tick bites of the genera Rhipicephalus and Hyalommas.5 We confirmed a case of lymphangitis due to R. sibirica mongolitimonae by PCR analysis of the eschar sample. This technique allows the definitive diagnosis of rickettsiosis with precision, speed and high sensitivity and specificity.10 Serology requires 2–3 weeks for seroconversion and shows cross-reactions, as in our case. The existence of cross reactions means that R. sibirica mongolitimonae is probably underdiagnosed, not only as a cause of LAR, but also of other types of rickettsiosis, as the microbiological diagnosis is based mainly on serology, and in many cases it is only performed against R. conorii.
Please cite this article as: Miguélez Ferreiro S, Navalpotro Rodríguez D. Linfangitis aguda tubular por Rickettsia sibirica mongolitimonae. Enferm Infecc Microbiol Clin. 2020;38:506–507.