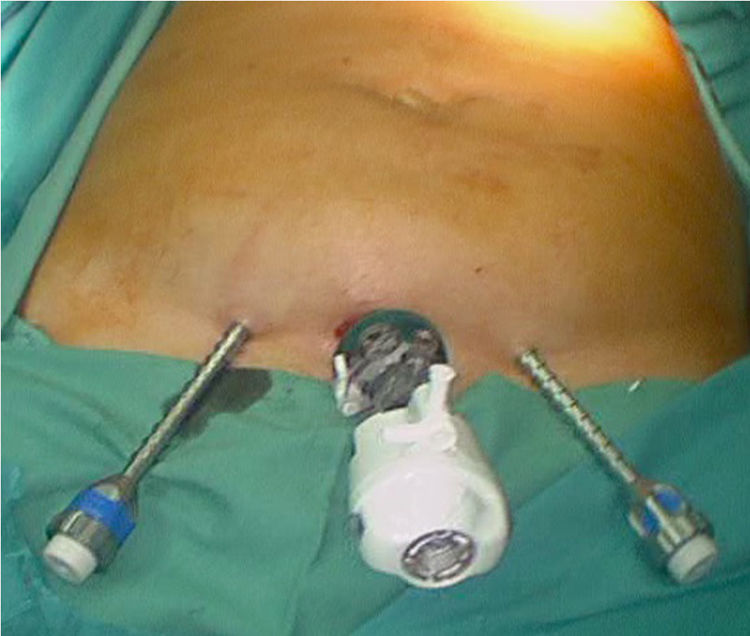
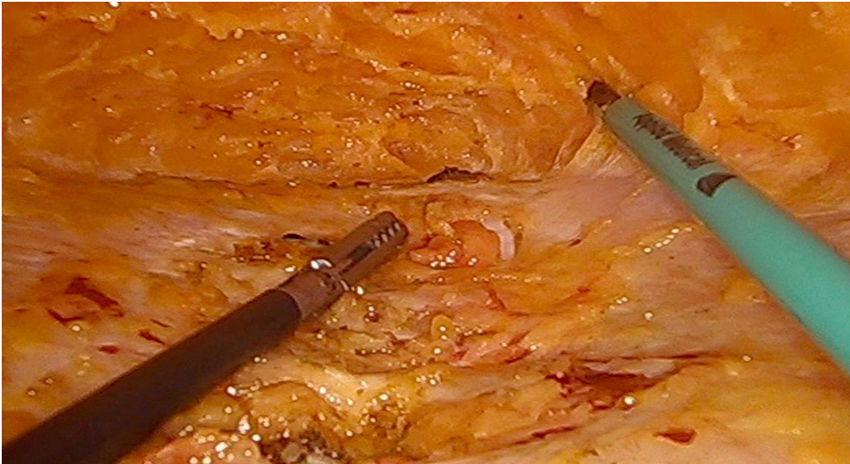
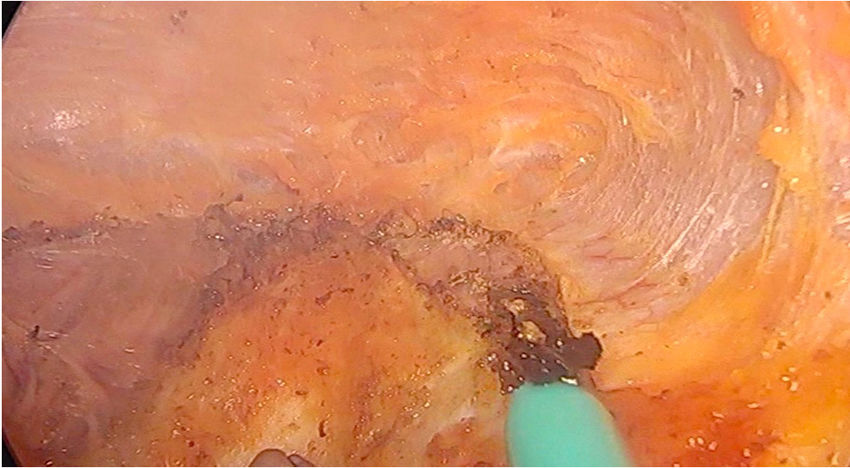
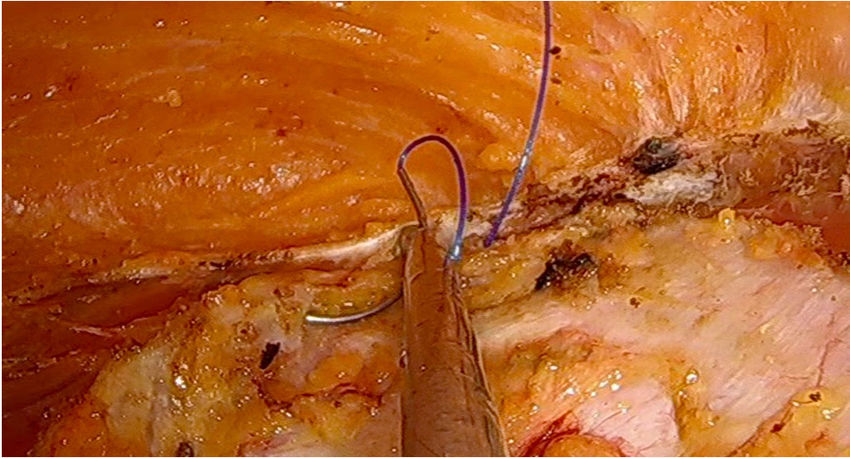
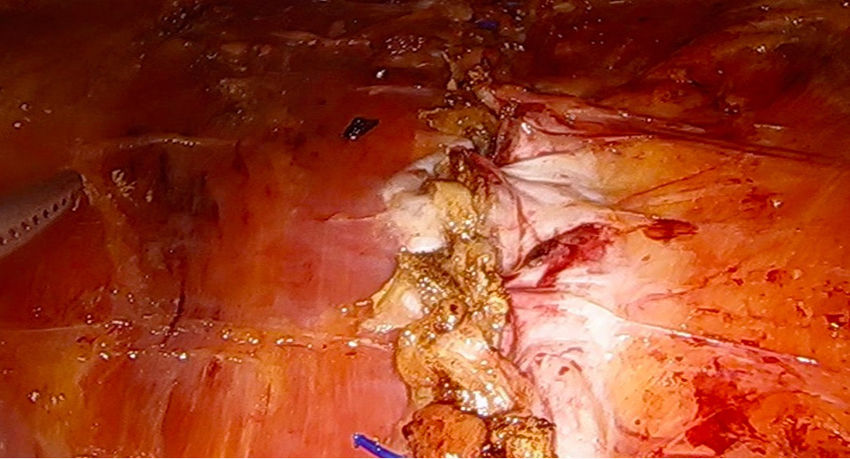
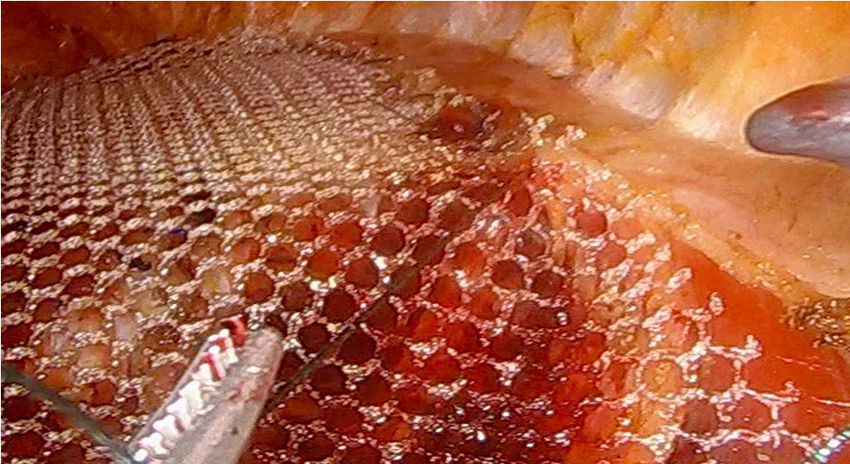
Laparoscopic ventral hernia repair is in full development with the appearance of surgical techniques that try to diminish the disadvantages associated with this procedure. Totally endoscopic subcutaneous ventral hernia surgery with suprapubic access is a new minimally invasive surgical technique that surgically corrects the hernia defect associated or not with diastasis recti, with the advantages of not penetrating the intra-abdominal space and avoiding the prosthesis placement in contact with the viscera, with the consequent complications derived from it (appearance of adhesions or fistulas).
El abordaje mínimamente invasivo de la hernia ventral se encuentra en pleno desarrollo con la aparición de técnicas quirúrgicas que intentan disminuir las críticas asociadas al abordaje laparoscópico tradicional. La cirugía totalmente endoscópica subcutánea de acceso suprapúbico de la hernia ventral es una nueva técnica quirúrgica mínimamente invasiva que corrige quirúrgicamente el defecto herniario asociado o no a diástasis de rectos, con las ventajas de no penetrar en el espacio intraabdominal y evitando la colocación de la prótesis en contacto con las vísceras, con las consiguientes complicaciones derivadas de ello (aparición de adherencias o fístulas).