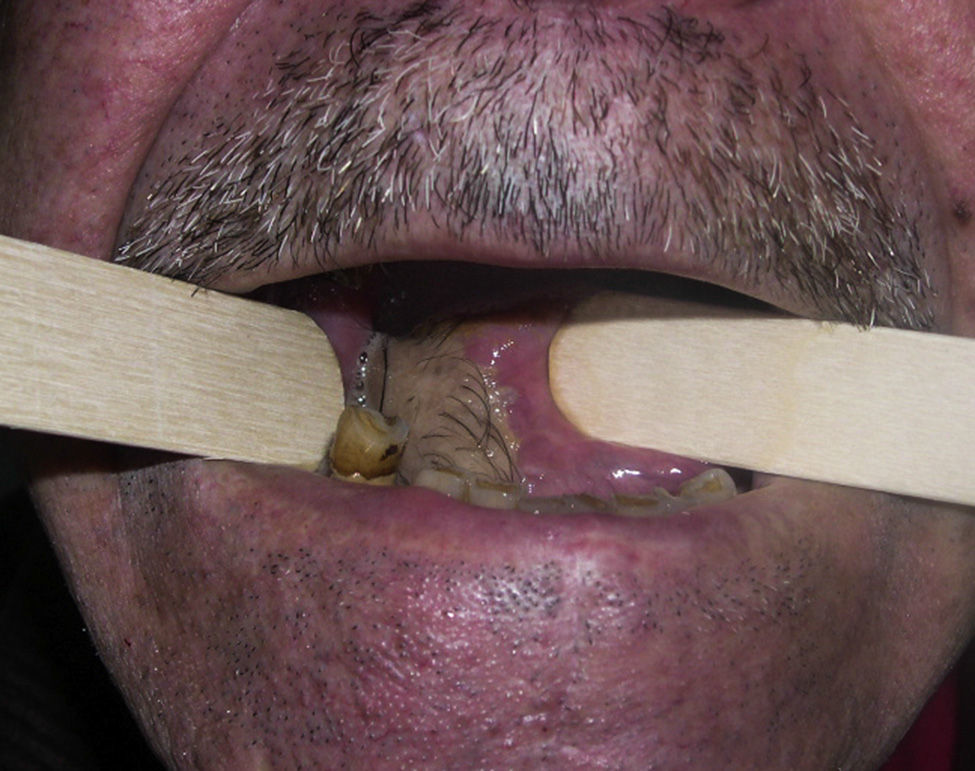
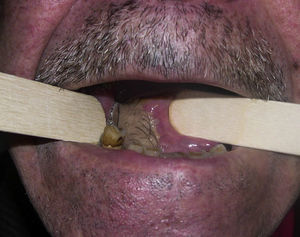
Radial graft is one of the optimal treatments for reconstruction after tongue cancer, but it is not free of side effects. Hypertrichosis over the graft, causing an intraoral paratrichosis, might downgrade the quality of life and even require further interventions.
Clinical caseThe case is presented of a 58 year-old man, who developed hypertrichosis after surgery for tongue carcinoma.
DiscussionThe therapeutic options, from choosing a graft from less hairy areas to laser depilation or de-epithelisation of the graft are discussed.
ConclusionsIntraoral paratrichosis is a serious complication that can produce dysphagia, nauseas, and vomiting, and can evolve into mal nutrition and produce an important decrease in life quality of patients.
El injerto radial es uno de los tratamientos de elección para la reconstrucción tras el cáncer de lengua, pero no está libre de problemas posteriores. La hipertricosis sobre el injerto provocó una paratricosis intraoral que puede disminuir la calidad de vida del sujeto, y hacer que requiera nuevas reintervenciones.
Caso clínicoPresentamos el caso de un varón de 58 años que tras cirugía por carcinoma de la base de la lengua presenta paratricosis sobre el injerto radial.
DiscusiónSe discuten las distintas opciones terapéuticas que abarcan desde la elección de colgajos procedentes de regiones anatómicas con menor densidad capilar, hasta el uso de técnicas de depilación láser o la desepitelización del colgajo.
ConclusionesLa paratricosis intraoral es una complicación importante que puede condicionar disfagia, náuseas y vómitos, con la subsecuente desnutrición que disminuye considerablemente la calidad de vida del paciente.
Reconstructive surgery after intraoral neoplasias is a true challenge for a surgeon. Radial graft is one of the optimal treatments, but it is not free of side effects. In the case we present here, a hypertrichosis over the graft, causing an intraoral paratrichosis, might downgrade the quality of life and even require further interventions.
Clinical caseThe patient is a 58-year-old man with a personal history of alcoholism and smoker of 40 cigars daily for around 35 years. He came for a consultation because of a 3-day evolution odynophagy and dysphonia. During exploration, he presented hyperaemic oropharynx with right submaxilar adenopathy of around 3cm diameter, unpainful, hard and undisplaceable. Due to clinical persistence, despite the treatment, he was referred to the service of Otolaryngology, which undertook a biopsy of the adenopathy, the result showing epidermoid tongue carcinoma T3N1Mx.
After this diagnosis, surgical treatment was performed with extirpation, functional cervical dissection and reconstruction with microvascularized radial flap, with no radiotherapy.
The patient was on a diet prescribed by a nutritionist, gave up his toxic habits and followed symptomatic treatment of mucositis.
A good functional recovery was achieved in speech and swallowing; tongue sensitivity was recovered at 6 months. As a consequence, paratrichosis was left on the flap, which affected the quality of life of the patient (Fig. 1). To palliate this problem, he was shaved, since he showed dysphagia to solid and liquid intake.
The persistence of previous clinical data led to laser treatment. Good results were obtained and the patient manifests minimal discomfort and can perform the different oro-buccal functions without inconvenience.
DiscussionDuring surgery of the oral cavity carcinoma, tongue reconstruction is the key factor for functional recovery. In the oral cavity, it is particularly important that the reconstruction method keeps the 3 main functions: speech, mastication and deglutition. One of the most used reconstructive techniques is the radial free flap.1
Intraoral paratrichosis is described as a relatively common complication after these techniques, even though the numbers are very small; Chaine et al.2 described only one case among 25.
This complication does not only cause discomfort and decrease the patient's quality of life, but also sometimes causes nausea and vomiting, directly affecting the nutritional state. The natural evolution of this complication is the decrease of capillary growth over time; however, when this does not occur, laser depilation is the correct thing to do. The use of different sources of energy was described in the literature.3,4 A last resort is the option to perform a de-epithelisation of the flap2 to avoid this complication. The group Sieg et al.5 recommend the use of flap of the forearm's ulnar region, since this is usually a less hairy area.
ConclusionIntraoral paratrichosis is a relatively common complication that should not be neglected in reconstructive buccal surgery. It is not only an aesthetic problem but also causes great discomfort, deterioration of the quality of life, and can influence deglutition and malnutrition problems. The treatment of this ailment includes the use of grafts with lower capillary density, such as the forearm's ulnar region, up to laser treatment or even reintervention to de-epithelialise the flap.
Conflict of interestThe authors declare that there are no conflicts of interest.
Please cite this article as: Segura-Sampedro JJ, Sampedro-Abascal C, Parra-López L, Muñoz-Rodríguez JC. Paratricosis en cavidad oral tras autoinjerto. Cir Cir. 2015;83:309–311.