A 4-year old boy, with history of relevance, presented with bilateral visual impairment, more so in scotopic conditions, and did not improve with optical correction. No significant funduscopic abnormalities were seen, leading to a suspicion of retinal dystrophy. Sequencing of the CACNA1F gene detected the c.3081C > A (p.Tyr1027Ter) mutation, which had occurred de novo in the patient’s mother. This mutation, in the aforementioned clinical context, and with a compatible electronegative pattern, establishes the diagnosis of X-linked type 2 congenital stationary night blindness.
Electrophysiology and genetic testing should be part of the diagnostic protocol for any unexplained loss of vision in children. The description, nomenclature and classification of hereditary retinal dystrophies based on their genotypic and electroretinography characteristics, avoids diagnostic errors due to their usual clinical and phenotypic overlap.
Un varón de 4 años, sin antecedentes relevantes, consulta por disminución de agudeza visual bilateral, más acusada en condiciones escotópicas, que no mejora con corrección óptica. No se aprecian alteraciones funduscópicas significativas, por lo que se sospecha una distrofia retiniana. La secuenciación del gen CACNA1F detecta la mutación c.3081C > A (p.Tyr1027Ter), que se ha producido de novo en la madre del paciente. Esta mutación, en el contexto clínico referido y con un patrón electronegativo compatible, establece el diagnóstico de ceguera nocturna estacionaria congénita tipo 2 ligada al cromosoma X.
La electrofisiología y el estudio genético deben formar parte del protocolo diagnóstico de cualquier pérdida de visión inexplicada en niños. La descripción, nomenclatura y clasificación de las distrofias retinianas hereditarias en base a sus características genotípicas y electrorretinográficas, evita los errores diagnósticos derivados de su habitual superposición clínica y fenotípica.
Congenital stationary night blindness (CSNB) refers to a very rare group of hereditary disorders that begin in childhood and are characterized by alterations in scotopic vision and non-progressive retinal dysfunction. The first patients described with CSNB were the descendants of Jean Nougaret, born in 1637 in the south of France. The spectrum of CSNB is broad and includes variants with different inheritance patterns and different phenotypic expression; however, the appearance of the fundus is normal in most forms. We present this clinical case with the intention of recalling that electroretinogram (ERG) and gene sequencing are fundamental in the study of diseases such as CSNB which have broad clinical heterogeneity and very low incidence, and which may otherwise lead to significant diagnostic delay or even be labeled as other diseases.1
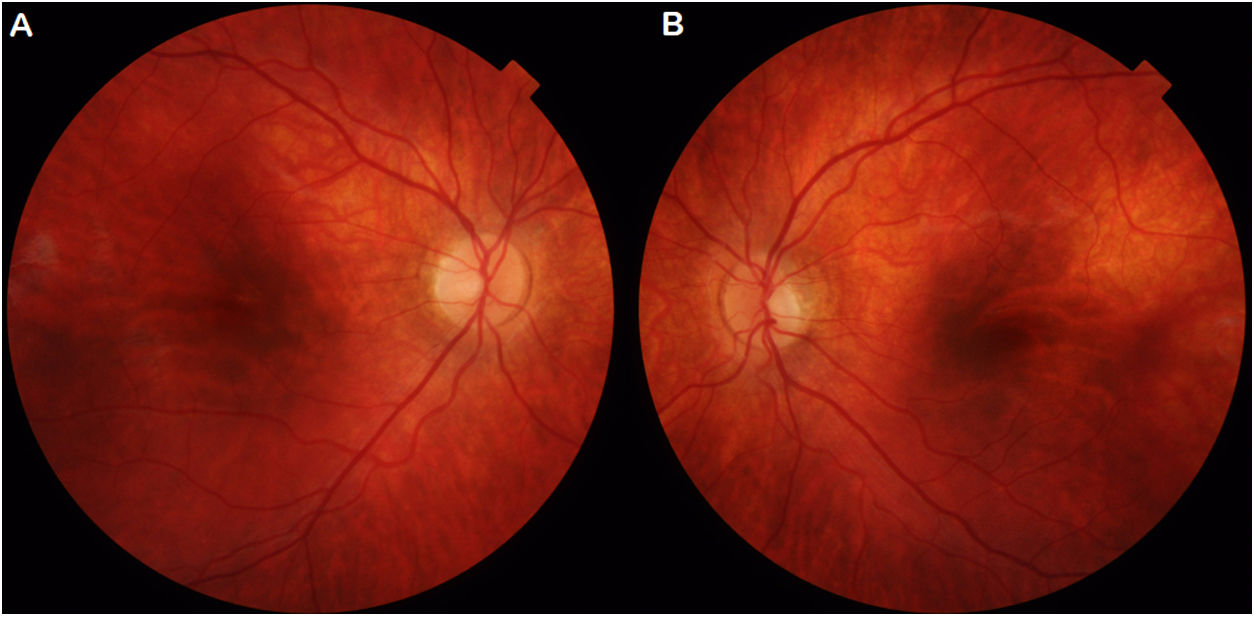
Clinical caseA 4-year-old Caucasian male with no personal or family remarkable history, visited for decreased bilateral visual acuity (VA), more pronounced in scotopic conditions. His parents are healthy and not blood relatives. The patient exhibited deep amblyopia, with VA of 20/100 in the right eye (RE) and 20/200 in the left eye (LE), with suppression of LE in binocularity and no stereoscopic vision. Cycloplegic refraction showed bilateral hypertropic astigmatism of little significance, 120° + 1.00 + 2.00 in the RE and 60° + 1.25 in the LE. Pupil alterations, strabismus, nystagmus and transillumination defects of the iris were not observed. The patient performed the Ishihara test and subsequently the Farnsworth test without confirming the existence of chromatic anomalies in either, despite excellent collaboration. However, the requested visual fields could be assessed. The fundus is slightly hypopigmented at the peripapillary level and in temporary arches, in the absence of other signs of fundoscopic pathology (Fig. 1). Moreover, optical coherence tomography did not reveal any signs of papillary or foveal involvement. Optical correction was prescribed, but the patient hardly experienced improvement in VA so, suspecting retinal dystrophy, electrophysiological tests and genetic study were requested.
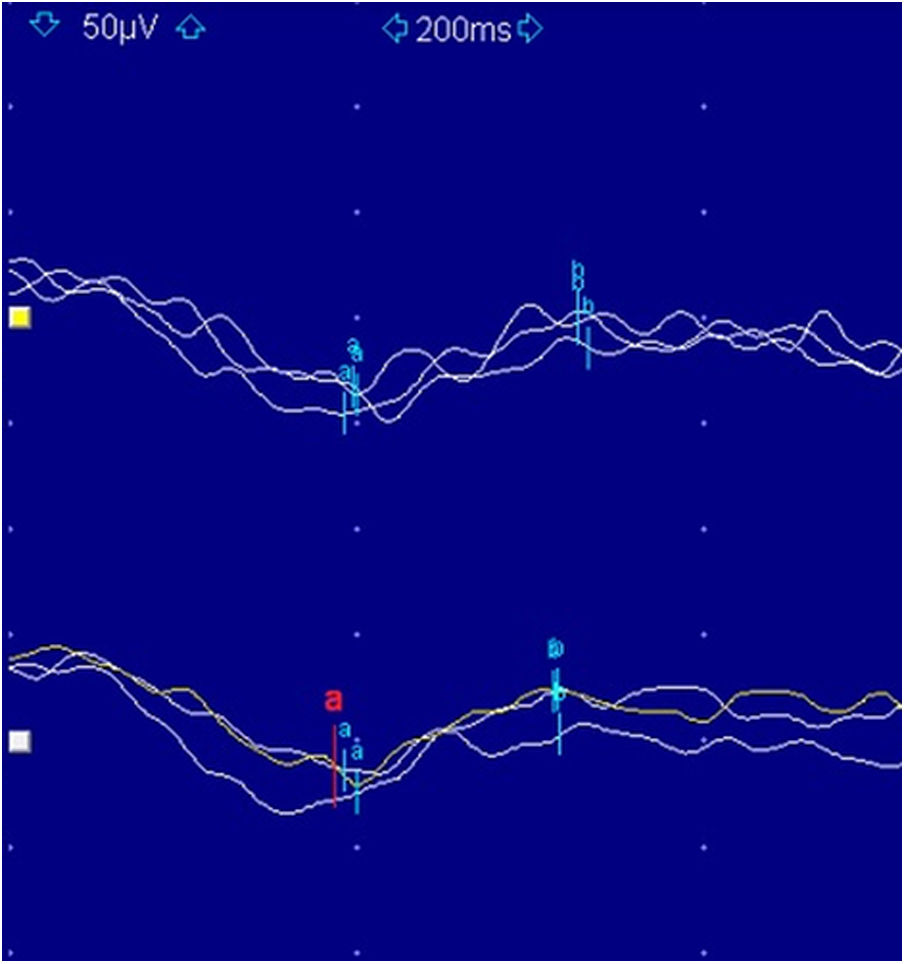
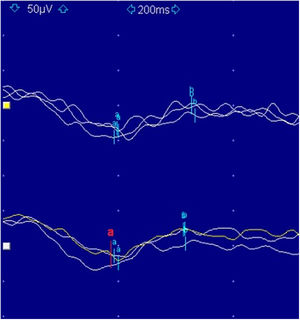
The electrophysiological study comprised visual evoked potential pattern, with normal results, and a flash ERG, with increased latencies and decreased amplitudes in both eyes. These ERG findings suggest a compromise of the peripheral retina; however, its diagnostic value at such a young age is limited due to the inability to discriminate between photopic and scotopic responses. For this reason, at the age of 6, a full-field ERG was performed showing an electronegative pattern (Fig. 2), alteration of photopic and scotopic responses as well as oscillatory potentials.
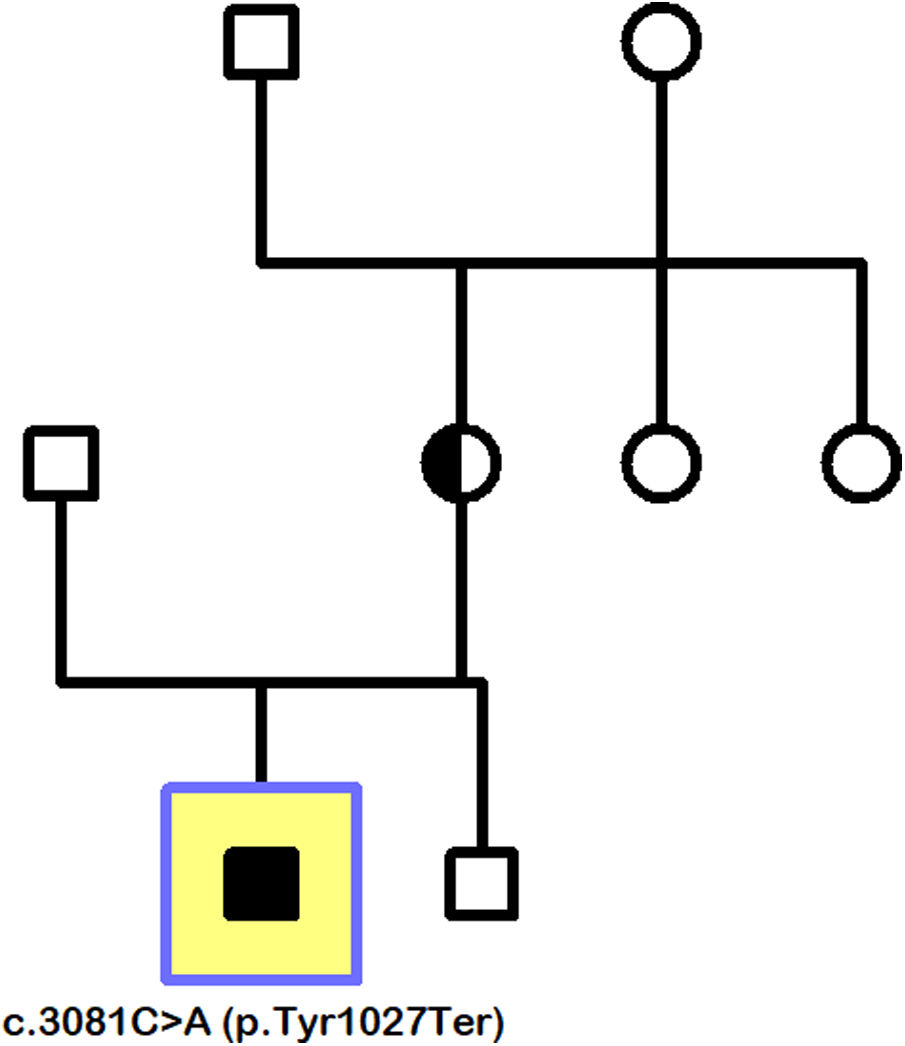
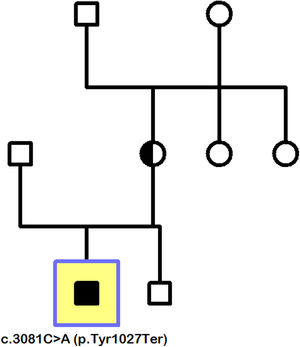
The gene sequencing was focused on cone and rod dystrophies, and evidenced the pathogenic variant c.3081C > A (p.Tyr1027Ter) in the gene CACNA1F located in Xp11.23. The presence of this mutation, together with compatible clinical picture and ERG, established the diagnosis of CSNB type 2 (CSNB2). The family study showed that the patient's mother is a carrier of a de novo truncating mutation, which did not come from the maternal grandparents and was transmitted to the child through recessive inheritance linked to the X chromosome. The patient's younger brother has not inherited the mutation and is therefore unaffected by the disease (Fig. 3).
Family tree (index patient indicated by square). Mother carrier of de novo mutation c.3081C > A (p.Tyr1027Ter), transmitted to her son by X-linked recessive inheritance. Absence of the mutation in the male brother of the index patient, as well as in the maternal grandparents made it unnecessary to extend the study to other members of the family branch.
Currently, at the age of 8, the best corrected VA is 20/30 in the RE (120° + 1.50 + 1.25) and 20/40 in the LE (85° + 1.00), with good binocular fusion and partial stereopsis of 240′'.
DiscussionThe most frequent hereditary pattern in CSNB is the X-linked recessive, with at least 17 genes involved, with more than 360 possible mutations and over 670 alleles affected. These genes encode proteins involved in phototransduction. Sporadic cases of CSNB account for approximately 40%.1
Clinical heterogeneity of the CSNB is significant, with varying degrees of visual deficit and nyctalopia. Most variants of the disease (with the exception of Oguchi's disease and fundus albipunctatus) do not exhibit fundoscopic alterations. VA is highly dependent on the frequent associated refractive errors, especially myopia. Patients with X-linked recessive CSNB are more commonly associated with high myopia and low VA. Some cases are accompanied by nystagmus or strabismus. Nyctalopia is not always symptomatic, probably as a result of an adaptive functional response, which means that on many occasions the impairment of scotopic vision goes unnoticed and this disease is under-diagnosed.1 Microperimetry shows a significant reduction in macular sensitivity in these patients, compared to healthy controls.2 Female carriers are almost always asymptomatic, although they may show evident changes in ERG (absence of oscillatory potentials).3
The full-field ERG functionally classifies the CSNB in 2 groups. The Riggs type is very unusual and corresponds almost exclusively to the autosomal dominant forms, in which an alteration in the scotopic responses (exaggerated wave b in the absence of wave a) is observed, with normal photopic responses, suggesting an intrinsic defect of the rods.1 The Schubert-Bornschein type appears to be associated with autosomal recessive or X-linked forms of inheritance and is much more frequent. This second group is characterized by an electronegative pattern (selective loss of wave b with preservation of wave a), with mixed alteration of photopic and scotopic responses, which gives rise to a post-transductional anomaly, without directly affecting the function of cones or rods.4
Miyake's team has studied the mechanisms of phototransduction at the CSNB with Schubert-Bornschein-type ERG and has described 2 pathways of synaptic dysfunction between photoreceptors and bipolar cells, stating that they should not be considered as variants of the same disease but rather as independent clinical entities with different genetic mutations, etiopathogenic mechanisms and electroretinal patterns.5 The terms used in international nomenclature are type 1 (CSNB1) or complete forms (cCSNB) and type 2 (CSNB2) or incomplete forms (icCSNB).1
The most common mutation in the CSNB1 or cCSNB affects the NYX gene, which encodes nictalopine. It is characterized by a post-synaptic dysfunction that corresponds with a negative ERG in scotropic conditions, with normal or slightly subnormal photopic function. CSNB1 is often associated with elevated myopia, nystagmus and symptomatic nictalopia.1,5
CSNB2 or icCSNB is associated with different genetic mutations, the most frequent being that of the CACNA1F gene, present in approximately 55% of X-linked CSNB cases and located on the short arm of the X chromosome (Xp11.23), encoding a transmembrane protein from a calcium channel (Cav1.4) that regulates glutamate release in phototransduction.6 The phenotypic expression of the CSNB2 is more heterogeneous, with inconstant nictalopia (54% do not report quality of life alterations), variable refractive errors from myopia to hypermetropia, photophobia, sensitivity to light, and sometimes decreased VA in photopic conditions.7 CSNB2 determines a defect at the presynaptic level, and an ERG with a decreased amplitude of wave b is observed in both scotopic and photopic conditions.8 The photopic response is much more affected than in CSNB1, and therefore CSNB2 must be differentiated by ERG from pure cone dystrophies, in which a normal scothopic response usually exists.1
The mutation of the CACNA1F gene is associated not only with CSNB2, but also with the development of two other ocular pathologies, i.e., X-linked rod and cone dystrophy type 3 and Åland Islands eye disease or Forssius-Eriksson syndrome. The influence of genetic or environmental modifiers may be responsible for their different phenotypic expression.9 Normal colour vision, the absence of nystagmus and foveal hypoplasia and the compatible pattern of ERG support the diagnosis of CSNB2 in this case. The pathogenic significance of the c.3081C > A (p.Tyr1027Ter) mutation in CSNB2 seems not to have been previously described in the literature, or at least, has not been found in our literature search.
Electrophysiology and genetic study should be part of the diagnostic protocol for any unexplained vision loss in children. This clinical case perfectly illustrates the challenge that diseases such as CSNB2 can pose. The presence of a de novo mutation further complicated the tracing of possible family cases in the anamnesis. ERG and gene sequencing have been essential to confirm the involvement of scotopic vision and to rule out other hereditary retinal dystrophies with similar phenotypic characteristics, but of a progressive nature and worse prognosis, such as juvenile X-linked retinoschisis or Leber's congenital amaurosis. It is therefore recommended that the description, nomenclature and classification of this type of disease should always be based on its genotypic and electroretinographic characteristics, thus avoiding diagnostic errors derived from frequent clinical and phenotypic overlap.1,5,10
Conflict of interestNo conflict of interest was declared by the authors.
Please cite this article as: Galindo-Bocero J, Macías-Franco S, García-González N, Valles-Antuña C, Hernando Acero I, Rozas-Reyes P. Diagnóstico de un caso de ceguera nocturna estacionaria congénita tipo 2 ligada al cromosoma X mediante electrorretinografía y secuenciación del gen CACNA1F. Arch Soc Esp Oftalmol. 2020;95:607–610.