The presence of atopy is considered as a risk factor for severe respiratory symptoms in children. The objective of this study was to examine the effect of atopy on the course of disease in children hospitalised with viral pneumonia.
MethodsChildren between the ages of 1 and 6 years hospitalised due to viral pneumonia between the years of 2013 and 2016 were included to this multicentre study. Patients were classified into two groups as mild–moderate and severe according to the course of pneumonia. Presence of atopy was evaluated with skin prick tests. Groups were compared to evaluate the risk factors associated with severe viral pneumonia.
ResultsA total of 280 patients from nine centres were included in the study. Of these patients, 163 (58.2%) were male. Respiratory syncytial virus (29.7%), Influenza A (20.5%), rhinovirus (18.9%), adenovirus (10%), human metapneumovirus (8%), parainfluenza (5.2%), coronavirus (6%), and bocavirus (1.6%) were isolated from respiratory samples. Eighty-five (30.4%) children had severe pneumonia. Atopic sensitisation was found in 21.4% of the patients. Ever wheezing (RR: 1.6, 95% CI: 1.1–2.4), parental asthma (RR: 1.5, 95% CI: 1.1–2.2), other allergic diseases in the family (RR: 1.8, 95% CI: 1.2–2.9) and environmental tobacco smoke (RR: 1.6, 95% CI: 1.1–3.5) were more common in the severe pneumonia group.
ConclusionsWhen patients with mild–moderate pneumonia were compared to patients with severe pneumonia, frequency of atopy was not different between the two groups. However, parental asthma, ever wheezing and environmental tobacco smoke exposure are risk factors for severe viral pneumonia in children.
Interaction between asthma and viral infections has been known for a very long time. Attention has been drawn in many studies to decreased antiviral response in patients with asthma.1 Epithelium damage, disrupted epithelium repair mechanisms, inflammation and insufficient immune response that occur in asthma cause these patients to become more sensitive to airway irritants as well as viral infections.2 Atopy, which refers to the genetic tendency to develop allergic diseases such as allergic rhinitis, asthma and atopic dermatitis and viral infections, disrupts the integrity of the epithelium barrier by way of synergic effect on the respiratory tract. This damage on the respiratory epithelium causes the onset of inflammation, thus triggering wheezing episodes and asthma.1,3–5 Inflammation in the respiratory tract due to atopy in addition to the disruption of the epithelial barrier integrity places these patients under risks of severe viral lower respiratory tract infections.
Atopic children are more at risk for severe pneumonia during pandemic influenza epidemics.6–8 Also, the first Rhinovirus (RV) infection in patients with asthma is generally in the form of lower respiratory tract infection and it is more severe and lasts longer.5,9 It was put forth in a prospective cohort study that the risk of hospitalisation due to severe Respiratory syncytial virus (RSV) infection is greater in atopic children in comparison with the control group.10 It is also reported that asthma and atopic dermatitis increase the risk of pneumococcal infections.11 Recent studies show that atopic sensitisation emerges prior to respiratory tract infections. Both viral illness and allergic sensitisation/exposure increase risks of severe respiratory tract diseases that require hospitalisation.12 The objective of this study was to examine the effects of the presence of atopy on the course of disease in children hospitalised with viral pneumonia. We hypothesised that atopic children are at increased risk for severe pneumonia with viral infections.
Materials and methodAll children between the ages of 1 and 6 years hospitalised with a viral pneumonia between 01/11/2013 and 01/01/2016 were included in this multicentre prospective study. Cases with chronic disease including asthma, gastroesophageal reflux, tracheomalacia, tuberculosis, congenital heart disease, cystic fibrosis, primary ciliary dyskinesia, vascular ring, bronchopulmonary dysplasia, or immune deficiency were excluded from the study. Presenting symptoms of the patients, laboratory findings, radiological findings and duration of hospitalisation were recorded.
AtopyAtopy is defined as positive skin prick tests (SPT) to one or more allergens.
Virus detection and identificationVirus detection and identification were carried out in the nasopharyngeal aspirates example via real-time reverse transcription polymerase chain reaction (RT-PCR) method (Fast Track Diagnostics Luxembourg S.‘a.r.I).
Skin prick testPresence of atopy was evaluated by skin prick tests (SPT). All participants had SPTs for Dermatophagoides pteronyssinus, Dermatophagoides farinae, Alternaria alternata, cat, grass mix (Phleum pratense, Poa pratensis, Dactylis glomerata, Lolium perenne, Festuca pratensis, and Avena eliator), tree mix (Betula verrucosa, Alnus glutinosa, and Coryllus avellena), Olea europea, Blatella germanica, histamine, and negative controls. Standardised core allergen extracts and controls were provided by ALK-Abello, Horsholm, Denmark. The tests were administered using prick test device on the volar surface of both forearms and recorded after 15min and considered as positive if the mean wheal diameter was 3mm larger compared to the negative control. Positive SPT was defined as a wheal ≥3mm to one or more allergens. SPT of patients who had received corticosteroid therapy were performed four weeks after hospital discharge. On the other hand, SPT were performed after completion of pneumonia treatment in patients who had not received steroids.
Severity of viral pneumoniaPatients were classified into two groups as mild–moderate and severe according to the course of pneumonia. The patients were considered to have severe pneumonia if at least one of the following criteria was present5:
SpO2<90% (in ambient air)
2nd or 3rd stage intensive care or mechanical ventilation support requirement
Development of atelectasis or effusion
Impaired consciousness (tendency to sleep, lethargy, confusion, unresponsiveness to painful stimulant)
Excessive dehydration
Apnoea
All risk factors that may cause a severe viral pneumonia course were examined. These risk factors included gender, body mass index (BMI), education status of the family, whether or not influenza vaccination had been given, environmental tobacco smoke exposure (ETS), presence of atopic disease in the patient, presence of atopic disease in the family, causative agent, type of allergen, and the presence of pets.
Statistical analysisData analysis was carried out via SPSS 22.0 (IBM statistics for Windows version 22, IBM Corparation, Armonk, New York, United States) and Medcalc 14 (Acacialaan 22, B-8400 Ostend, Belgium) software. Shapiro–Wilk test was used to examine whether the data fit normal distribution or not and the variance homogeneity of the data was examined via Levene test. Independent-Samples T test together with Bootstrap results was used to compare two independent groups, Mann–Whitney U test was used with Monte Carlo simulation technique. Pearson Chi-Square and Fisher Exact tests were tested via Monte Carlo Simulation technique for the comparison of categorical data. Relative risk values were calculated in order to examine the ratio between developing a disease in those with a risk factor and those that do not. Logistic regression test was used to calculate the odds-ratio for quantitative explanatory variables with statistically significant binary (diotome) response variables. Quantitative data were expressed in the tables as mean±sd (standard deviation), median±IQR (Interquartile Range) and as median Range (Maximum–Minimum) values. Categorical data were expressed as n (number) and percentages (%). Data were examined at a confidence level of 95% and a p value of less than 0.05 was accepted as statistically significant.
Ethical approvalApproval was taken from Izmir Dr. Behçet Uz Child Disease and Padiatric Surgery Training and Research Hospital Non-Pharmacologic Clinical Studies Ethical Council (no. 2013/54).
ResultsA total of 280 patients from different geographical regions of Turkey were included in the study. A total of 31 patients whose medical records were missing could not be included in the study. There were 163 (58.2%) males with an average age of 32.9±21.08 (min 11–max 72) months and BMI of 16.4 (min 10.8–max 29.5). The average duration of hospitalisation was 9.2±7.90 (min 1–max 60) days. Viral agents included RSV (29.7%), Influenza A (20.5%), rhinovirus (18.9%), adenovirus (10%), human metapneumovirus (hMPV) (8%), parainfluenza (5.2%), coronavirus (6%), and bocavirus (1.6%).
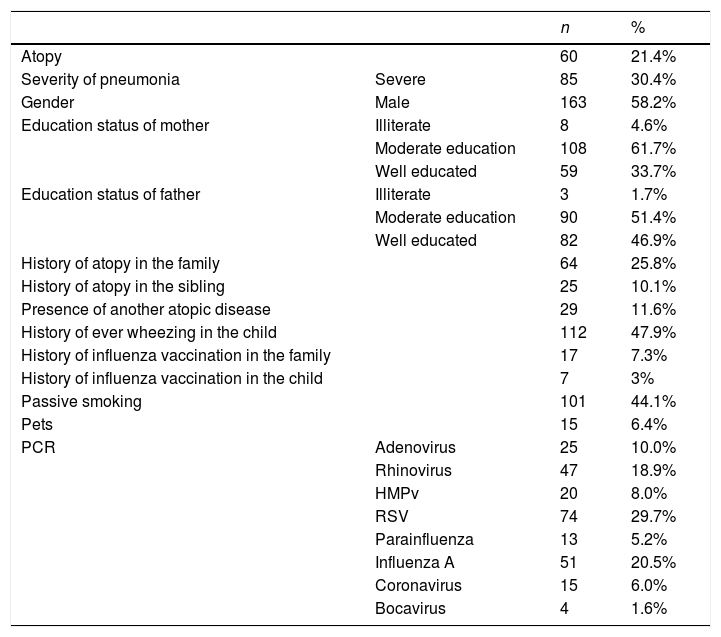
When the history of atopy in the family was questioned, 16% had parental asthma, 6.9% had family history of allergic rhinitis, 3.6% eczema and 6.0% food/drug allergy in the family. Forty-eight percent of the patients had ever wheezing, 5.2% had allergic rhinitis, 2% had eczema and 5.2% had food/drug allergy. Environmental tobacco smoke exposure was present in 44.1% of the patients. When the family education status was evaluated 33.7% mothers had high-school education and 46.9% of the fathers had high-school education. Three percent of the patients had received influenza vaccine and 6.4% had pets in their homes (Table 1).
Demographic and clinical findings of patients.
| n | % | ||
|---|---|---|---|
| Atopy | 60 | 21.4% | |
| Severity of pneumonia | Severe | 85 | 30.4% |
| Gender | Male | 163 | 58.2% |
| Education status of mother | Illiterate | 8 | 4.6% |
| Moderate education | 108 | 61.7% | |
| Well educated | 59 | 33.7% | |
| Education status of father | Illiterate | 3 | 1.7% |
| Moderate education | 90 | 51.4% | |
| Well educated | 82 | 46.9% | |
| History of atopy in the family | 64 | 25.8% | |
| History of atopy in the sibling | 25 | 10.1% | |
| Presence of another atopic disease | 29 | 11.6% | |
| History of ever wheezing in the child | 112 | 47.9% | |
| History of influenza vaccination in the family | 17 | 7.3% | |
| History of influenza vaccination in the child | 7 | 3% | |
| Passive smoking | 101 | 44.1% | |
| Pets | 15 | 6.4% | |
| PCR | Adenovirus | 25 | 10.0% |
| Rhinovirus | 47 | 18.9% | |
| HMPv | 20 | 8.0% | |
| RSV | 74 | 29.7% | |
| Parainfluenza | 13 | 5.2% | |
| Influenza A | 51 | 20.5% | |
| Coronavirus | 15 | 6.0% | |
| Bocavirus | 4 | 1.6% |
| Mean±SD | Median (min–max) | ||
|---|---|---|---|
| Age | 32.9±21.08 | 24 (72–11) | |
| BMI | 16.8±2.51 | 16.4 (29.5–10.8) | |
| Duration of Hospitalisation (day) | 9.2±7.90 | 7 (60–1) | |
| Fever | 37.4±0.96 | 37 (39.9–36) | |
| HR | 119.8±23.56 | 114.5 (186–60) | |
| RR | 34.9±10.83 | 32 (70–12) | |
| SaO2 | 95.1±4.32 | 96 (100–72) | |
| Haemoglobin | 11.4±1.37 | 11.3 (16–7.6) | |
| Leucocyte | 12,050.6±4997.40 | 11,200 (31,280–11.9) | |
| Lymphocyte | 37.5±19.97 | 34.5 (85–2) | |
| Monocyte | 7.3±7.18 | 6.695 (79–0) | |
| Neutrophil | 52.7±22.47 | 54.3 (94.3–0) | |
| Eosinophil | 1.7±2.32 | 0.7 (13.8–0) | |
| Basophile | 0.4±0.40 | 0.3 (2.26–0) | |
| Thrombocyte | 373,482.3±123,195.68 | 366,000 (1,006,000–385) |
SD: standard deviation, max: maximum, min: minimum. PCR: polymerase chain reaction, BMI: body mass index, HR: heart beats per minute, RR: respiratory rate per minute, SaO2: oxygen saturation.
Atopy was found in 60 (21.4%) patients; most frequent sensitisations were mite (11.4%), grass/pollen mixture (7.1%) and Alternaria (5%). Atopy was more frequent in patients with influenza (29.2%) and rhinovirus (25%) infections (p=0.196) but no statistically significant difference was found. Atopic patients were older compared to non-atopic patients with viral pneumonia (p=0.001).
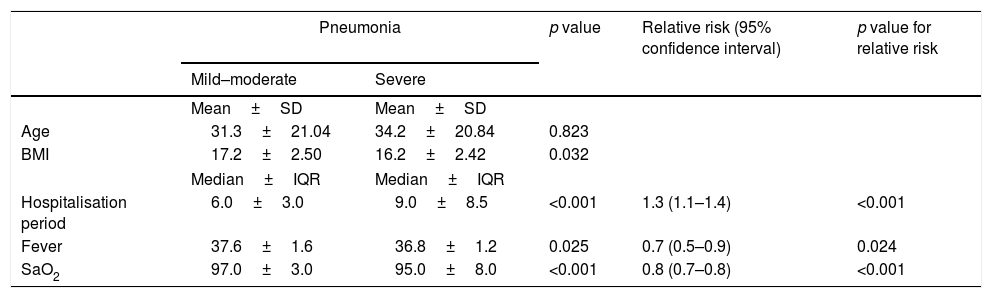
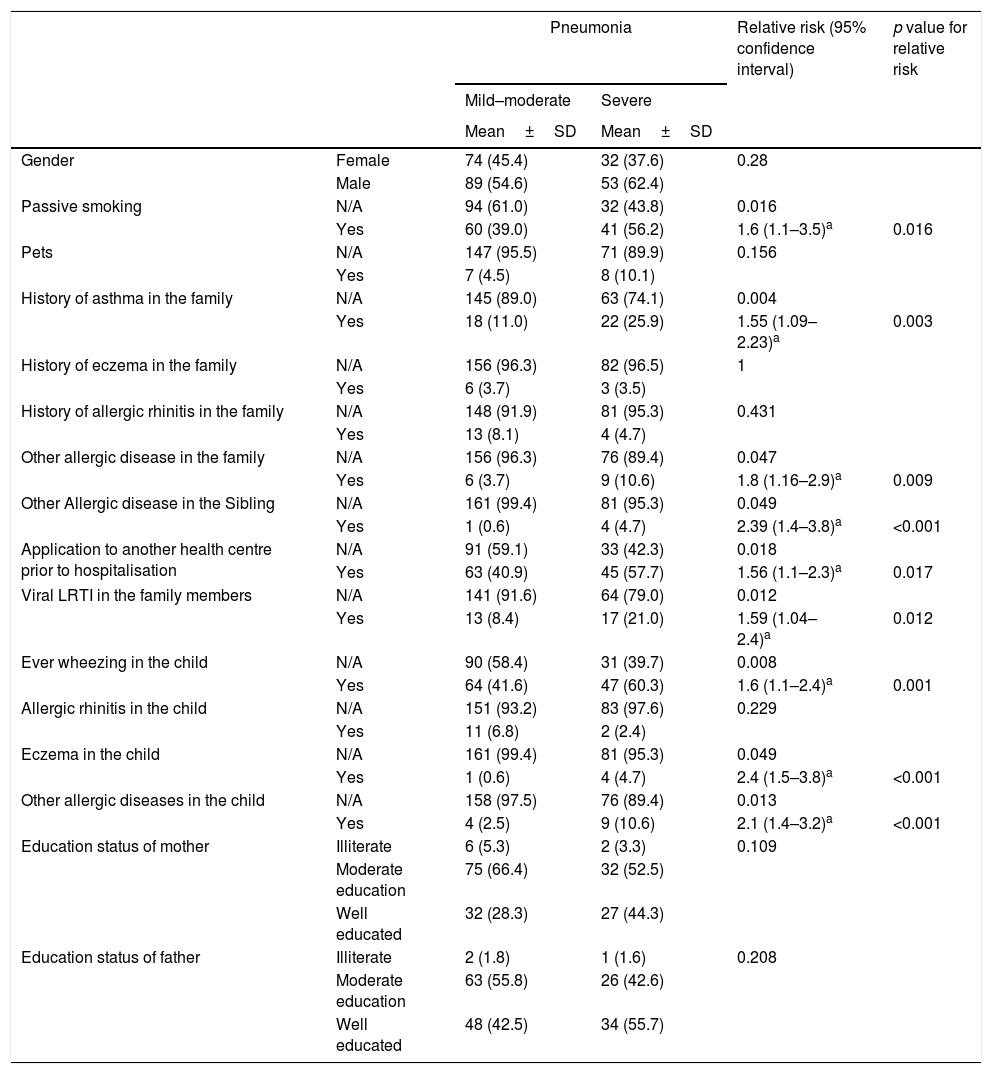
One hundred and ninety-five patients (69.6%) had mild–moderate, 85 (30.4%) had severe pneumonia. When compared to patients with mild or moderate pneumonia, patients with severe pneumonia were found to carry a significantly greater relative risk (RR) in terms of ever wheezing (RR: 1.6, 95% CI: 1.1–2.4), parental asthma (RR: 1.5, 95% CI:1.09–2.23), other allergic diseases in the family (RR: 1.8, 95% CI: 1.16–2.9) and ETS (RR: 1.6, 95% CI: 1.1–3.5) respectively. The education status of the parents, existence of pets, whether the patient or the family members had had influenza vaccination during this year or in the past were not associated with the severity of pneumonia (Tables 2a and 2b).
Distribution of risk factors according to the course of the disease.
| Pneumonia | p value | Relative risk (95% confidence interval) | p value for relative risk | ||
|---|---|---|---|---|---|
| Mild–moderate | Severe | ||||
| Mean±SD | Mean±SD | ||||
| Age | 31.3±21.04 | 34.2±20.84 | 0.823 | ||
| BMI | 17.2±2.50 | 16.2±2.42 | 0.032 | ||
| Median±IQR | Median±IQR | ||||
| Hospitalisation period | 6.0±3.0 | 9.0±8.5 | <0.001 | 1.3 (1.1–1.4) | <0.001 |
| Fever | 37.6±1.6 | 36.8±1.2 | 0.025 | 0.7 (0.5–0.9) | 0.024 |
| SaO2 | 97.0±3.0 | 95.0±8.0 | <0.001 | 0.8 (0.7–0.8) | <0.001 |
Independent T test (Bootstrap) – Mann Whitney U test (Monte Carlo).
SD: standard deviation; IQR: interquartile range; BMI: body mass index; HR: heart beats per minute; RR: respiratory rate per minute; SaO2: oxygen saturation.
Distribution of risk factors according to the course of the disease.
| Pneumonia | Relative risk (95% confidence interval) | p value for relative risk | |||
|---|---|---|---|---|---|
| Mild–moderate | Severe | ||||
| Mean±SD | Mean±SD | ||||
| Gender | Female | 74 (45.4) | 32 (37.6) | 0.28 | |
| Male | 89 (54.6) | 53 (62.4) | |||
| Passive smoking | N/A | 94 (61.0) | 32 (43.8) | 0.016 | |
| Yes | 60 (39.0) | 41 (56.2) | 1.6 (1.1–3.5)a | 0.016 | |
| Pets | N/A | 147 (95.5) | 71 (89.9) | 0.156 | |
| Yes | 7 (4.5) | 8 (10.1) | |||
| History of asthma in the family | N/A | 145 (89.0) | 63 (74.1) | 0.004 | |
| Yes | 18 (11.0) | 22 (25.9) | 1.55 (1.09–2.23)a | 0.003 | |
| History of eczema in the family | N/A | 156 (96.3) | 82 (96.5) | 1 | |
| Yes | 6 (3.7) | 3 (3.5) | |||
| History of allergic rhinitis in the family | N/A | 148 (91.9) | 81 (95.3) | 0.431 | |
| Yes | 13 (8.1) | 4 (4.7) | |||
| Other allergic disease in the family | N/A | 156 (96.3) | 76 (89.4) | 0.047 | |
| Yes | 6 (3.7) | 9 (10.6) | 1.8 (1.16–2.9)a | 0.009 | |
| Other Allergic disease in the Sibling | N/A | 161 (99.4) | 81 (95.3) | 0.049 | |
| Yes | 1 (0.6) | 4 (4.7) | 2.39 (1.4–3.8)a | <0.001 | |
| Application to another health centre prior to hospitalisation | N/A | 91 (59.1) | 33 (42.3) | 0.018 | |
| Yes | 63 (40.9) | 45 (57.7) | 1.56 (1.1–2.3)a | 0.017 | |
| Viral LRTI in the family members | N/A | 141 (91.6) | 64 (79.0) | 0.012 | |
| Yes | 13 (8.4) | 17 (21.0) | 1.59 (1.04–2.4)a | 0.012 | |
| Ever wheezing in the child | N/A | 90 (58.4) | 31 (39.7) | 0.008 | |
| Yes | 64 (41.6) | 47 (60.3) | 1.6 (1.1–2.4)a | 0.001 | |
| Allergic rhinitis in the child | N/A | 151 (93.2) | 83 (97.6) | 0.229 | |
| Yes | 11 (6.8) | 2 (2.4) | |||
| Eczema in the child | N/A | 161 (99.4) | 81 (95.3) | 0.049 | |
| Yes | 1 (0.6) | 4 (4.7) | 2.4 (1.5–3.8)a | <0.001 | |
| Other allergic diseases in the child | N/A | 158 (97.5) | 76 (89.4) | 0.013 | |
| Yes | 4 (2.5) | 9 (10.6) | 2.1 (1.4–3.2)a | <0.001 | |
| Education status of mother | Illiterate | 6 (5.3) | 2 (3.3) | 0.109 | |
| Moderate education | 75 (66.4) | 32 (52.5) | |||
| Well educated | 32 (28.3) | 27 (44.3) | |||
| Education status of father | Illiterate | 2 (1.8) | 1 (1.6) | 0.208 | |
| Moderate education | 63 (55.8) | 26 (42.6) | |||
| Well educated | 48 (42.5) | 34 (55.7) | |||
Pearson Chi Square Test (Monte Carlo) – Fisher Exact (Exact).
PCR: polymerase chain reaction, HMPv: human metapneumovirus, RSV: respiratory syncytial virus. LRTI: lower respiratory tract infection.
Not surprisingly, patients with severe pneumonia had longer duration of hospitalisation (p<0.001) and their body mass indexes were lower (p=0.032). Children with severe pneumonia had lower number of lymphocytes (p<0.001) and eosinophils (p=0.003), and higher number of neutrophils (p<0.001) compared to mild to moderate group.
Atopy was detected in 17.6% of children with severe pneumonia and 16.4% in mild–moderate pneumonia (p=0.736). Even though no statistically significant difference was found in terms of atopy in the group with severe pneumonia, ever wheezing (p=0.008) and parental asthma (p=0.004) were observed more frequently in children with severe pneumonia (Table 2b).
DiscussionIn this study, there was no effect of atopic sensitisation on the severity of viral pneumonia in children. However, history of allergic diseases such as ever wheezing, atopic dermatitis and food/drug allergy were associated with severe pneumonia.
Natural and acquired immunity of the airway is insufficient in asthma.13,14 Airway epithelium is a chemical, physical, and immunological barrier.15 In addition to holding the cells together, the airway epithelium tight junction regions act as a protective barrier that prevents harmful molecules and infectious agents from entering the tissue, by preventing their passage from the intracellular gaps between the molecules and ions.16–19 It has been shown that patients with asthma are more sensitive to allergens and environmental irritants due to defects in the epithelium barrier.20 Children generally face house allergens more during the first years of their lives. The risk of developing asthma increases as a result of this sensitivity to allergens.21,22 It has been shown in studies that the exposure of lung epithelium to allergens with proteolytic activity such as house-dust mite, pollen, mould and fungi causes an increase in epithelium permeability by separating the tight junction regions between the epithelium cells.23 All respiratory tract viruses enter from the airway epithelium, replicate in the airway epithelium thus damaging both ciliated and non-ciliated respiratory tract epithelium cells. As a result, they cause necrosis, ciliostasis, loss of cilia and decrease in mucociliary clearance in the airway epithelium.24,25 Both atopy and viral infections cause loss of integrity in the epithelium barrier, which has a vital importance due to its synergic effect on the respiratory tract.1,4
Forty-two percent of children who were hospitalised in intensive care units during the 2009–2010 pandemic influenza epidemic had asthma/atopic sensitisation, and H1N1-related severe respiratory tract infections were more common in atopic children in comparison with non-atopic children.6 In another study carried out during the same year, of the 33 children who had an asthma attack during the pandemic influenza epidemic, 66.7% had had an asthma attack before but had not received a protective treatment for asthma, whereas 31.8% had their first asthma attack. Severe asthma attack, pneumonia and atelectasis develop more easily in atopic patients.8 However, no such difference has been determined in seasonal influenza.6,8 In our study the presence of atopy by a skin prick test was not a risk factor for severe viral pneumonia. However, we showed that ever wheezing and parental asthma, which are related with atopic structure, were associated with severe of pneumonia.
When volunteers are subject to in vivo RV inoculation, those with asthma have more severe symptoms in comparison with the controls.26 Experimental RV studies show that allergic sensitisation and exposure to allergens are related with increase in the severity of RV related lower respiratory tract infections and asthma exacerbations.1 Ducharme, FM et al.27 showed that almost in two-thirds of patients, predominantly pre-schoolers (those aged six years or older), viruses have been detected in their nasopharyngeal secretions, mainly RV and RSV. In our study, influenza (29.2%) and RV (25%) pneumonias were more frequent in atopic children, which supports the previous findings.
Effects of pollutants such as cigarettes are generally neglected in the existence of allergens and viruses.28 When a comparison was made between children hospitalised for community acquired pneumonia, duration of hospitalisation of children with two or more smoking family members in the house was longer, and that their intensive-care needs were greater.29 Previous studies reported that ETS for Gambian and Alaskan children and smoking of the mother for Finnish children are related with invasive pneumococcal disease.30–32 Jroundi et al.33 showed that smoking in the house was associated with a worse prognosis in children with pneumonia. As expected, ETS was a significant risk factor for severe pneumonia from our study. Jung et al.11 reported that other allergic diseases such as asthma and atopic dermatitis also increase the risk of pneumococcal infections. We also showed that the risk of severe pneumonia increased by 2.4 times (p<0.001) for those who had a history of eczema.
Even simple nutritional changes may have effects on prevention of virus-induced disease.1 Lower body mass index (BMI) for our cases with severe pneumonia indicate the importance of nutritional support in virus-related pneumonia. Lazzerini et al.34 showed that pneumonia related fatality rates increase in cases with malnutrition. A study by Jroundi et al.33 supported these findings showing that prognosis is worse in children with weight-for-age Z score <1SD. Ahanchian et al.13 pointed out that nutritional support will decrease the recurrence of lower respiratory tract infections in children. Jroundi et al.33 studied 689 children with pneumonia and showed that cyanosis, paleness, prematurity and passive smoking were risk factors for worse prognosis, while ever wheezing or asthma story were not. Jackson et al.35 reported that low birth weight, lack of exclusive breastfeeding, crowding – more than seven persons per household, exposure to indoor air pollution, incomplete immunisation, undernutrition – weight-for-age less than two standard deviations and HIV infection were risk factors for severe pneumonia in children aged five years and below. A direct relationship could not be shown between the presence of atopy and severe pneumonia in our study, however the presence of ever wheezing, allergic disease story and parental asthma were associated with worse pneumonia. Camara et al.36 carried out a study on children aged under 12 and reported that atopy history in the family for children under the age of two and the inhalant allergen sensitivity for children above the age of two were risk factors for viral respiratory tract infections. These findings are in accordance with our study. Kusel et al.37 evaluated children aged six months, two, five and ten years old who had severe viral respiratory tract infections with regard to atopy. While the rate of atopy was not increased at two years of age, it increased by 2.56 between the ages of 2–5 and by 17.14 times at the age of ten. This relationship was observed in cases who had severe RSV infection at an early age.
The average age of children with atopy was greater in comparison with the ages of those without atopy in our study (p=0.001). Perhaps, different results may be obtained when in vitro methods such as sIgE are used instead of SPT to detect the presence of atopy at early ages. One of the limitations of our study was that atopic status has not been monitored at periodic intervals.
Hyvärinen et al.38 examined the effects of severe bronchiolitis and pneumonia during the infantile period on teenage asthma reporting that repeated wheezing, atopic dermatitis and elevated blood eosinophils were early asthma-predictive factors. It was also observed in our study that repeated wheezing and accompanying story of allergic disease were related with severe pneumonia.
The relation between persistent respiratory problems and socioeconomic status has been remarked in many studies.39,40 However, as the families in general did not want to say their actual level of income, we could not evaluate the economic status directly. We tried to indirectly evaluate according to their educational level. We can say that the socioeconomic level of the patients’ parents is generally middle class. The education status of the parents was not associated with both the severity of pneumonia and atopy.
By determining the risk factors for severe pneumonia, it will be possible to use various treatment modalities on these children at early ages and thus prevent the development of severe pneumonia. Persistent wheezing and asthma development at later ages will thus be prevented by preventing severe pneumonia at an early age. In our study, even though the presence of atopy was not a risk factor for severe pneumonia, history of atopy in patients who had severe lower respiratory tract infections may indicate that the disease may follow a severe course in atopic patients. Decreasing exposure to allergens in addition to decreasing ETS may also decrease the risk of severe lower respiratory tract infection.
Ethical disclosuresConfidentiality of dataThe authors declare that they have followed the protocols of their work centre on the publication of patient data and that all the patients included in the study have received sufficient information and have given their informed consent in writing to participate in that study.
Right to privacy and informed consentThe authors have obtained the informed consent of the patients and/or subjects mentioned in the article. The author for correspondence is in possession of this document.
Protection of human subjects and animals in researchThe authors declare that the procedures followed were in accordance with the regulations of the responsible Clinical Research Ethics Committee and in accordance with those of the World Medical Association and the Helsinki Declaration.
Funding sourceNo external funding was secured for this study.
Contributors’ statement pageSemiha Bahçeci Erdem: literature search, study design, data collection, data analysis, manuscript preparation/editing, final manuscript approval.
Demet Can: literature search, study design, data collection, data analysis, manuscript preparation/editing, final manuscript approval.
Saniye Girit: literature search, study design, data collection, manuscript preparation/editing, final manuscript approval.
Ferhat Catal: literature search, data collection, manuscript preparation/editing.
Velat Sen: literature search, manuscript preparation/editing, data collection
Sevgi Pekcan: literature search, data collection, manuscript preparation/editing.
Hasan Yüksel: literature search, data collection, manuscript preparation/editing.
Ayşen Bingöl: literature search, manuscript preparation/editing, data collection.
İlknur Bostancı: literature search, manuscript preparation/editing, data collection.
Duygu Erge: literature search, manuscript preparation/editing, data collection.
Refika Ersu: literature search, study design, data collection, manuscript preparation/editing, final manuscript approval.
Financial disclosureThe authors have no financial relationships relevant to this article to disclose.
Conflict of interestThe authors have no conflicts of interest to disclose.