The present study evaluates the impact of vaginal surgery for pelvic organ prolapse (POP) on voiding dysfunction (VD) symptoms and post-void residual (PVR) one year after the intervention.
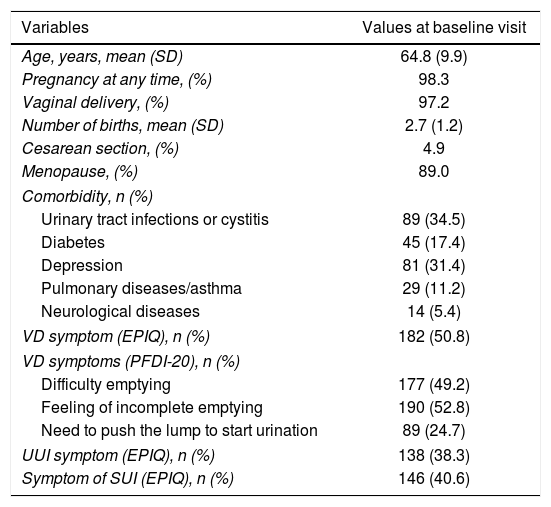
Material and methodsEpidemiological, longitudinal, prospective study. Thirty-nine gynecology units included women with symptomatic POP grade 2 or higher according to the Pelvic Organ Prolapse Quantification (POP-Q) system, who would undergo surgery for vaginal prolapse (CIRPOP-IUE study). Sociodemographic and clinical variables were collected before and after the intervention. At both visits, patients completed the ‘Epidemiology of Prolapse and Incontinence Questionnaire’ (EPIQ) and ‘Pelvic Floor Distress Inventory’ (PFDI-20) questionnaire. PVR volume was measured by bladder catheterization immediately after spontaneous urination.
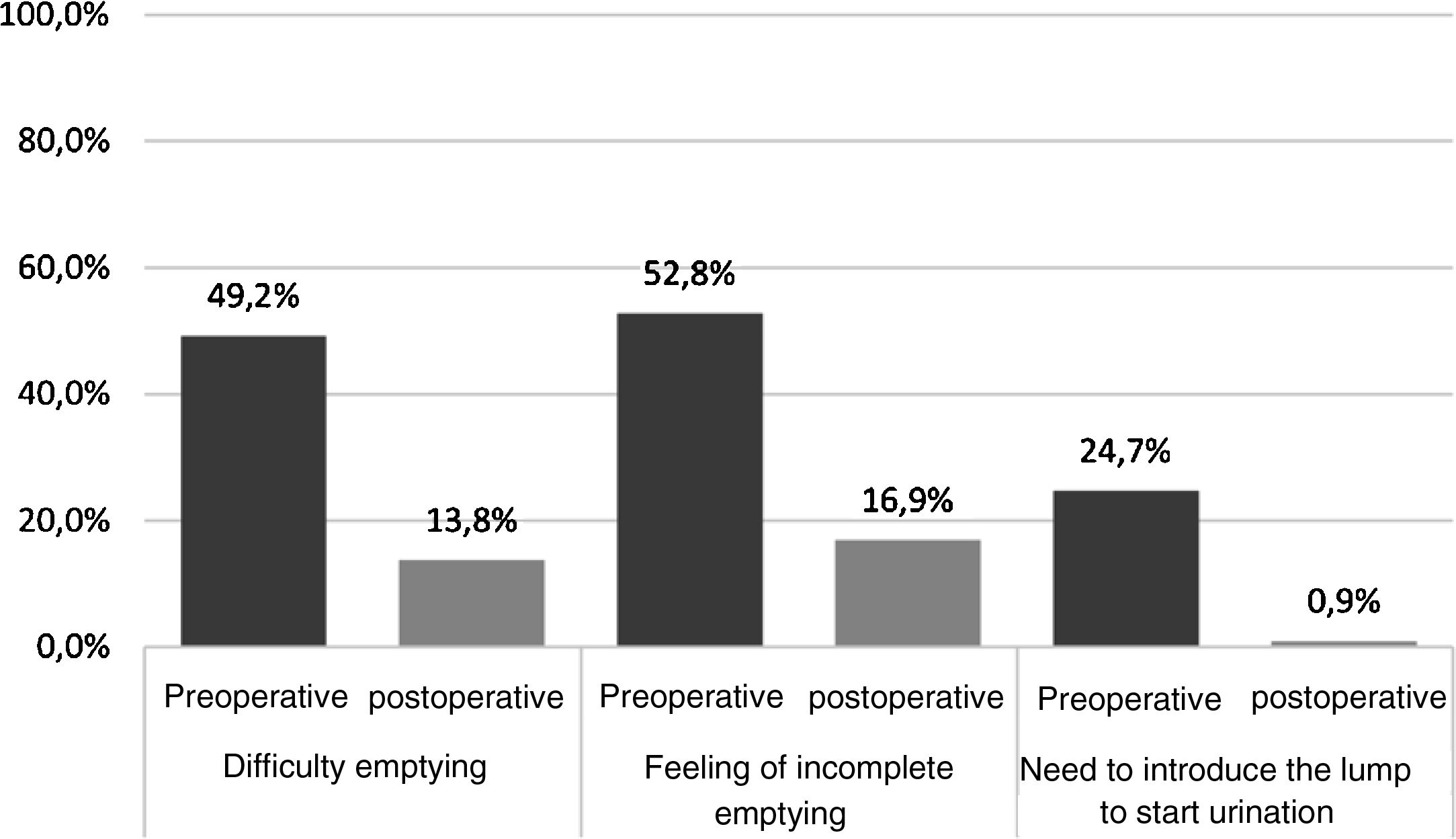
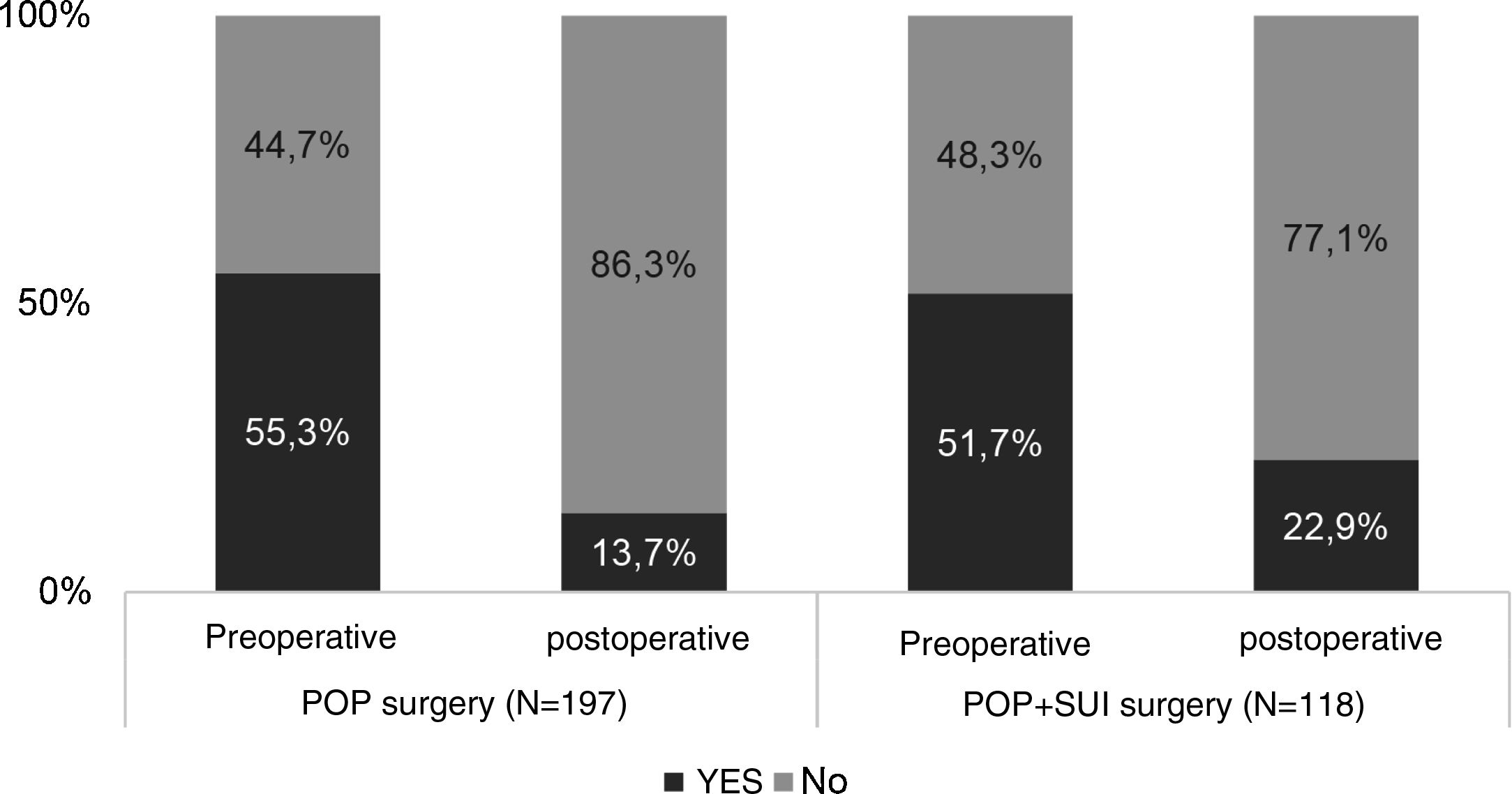
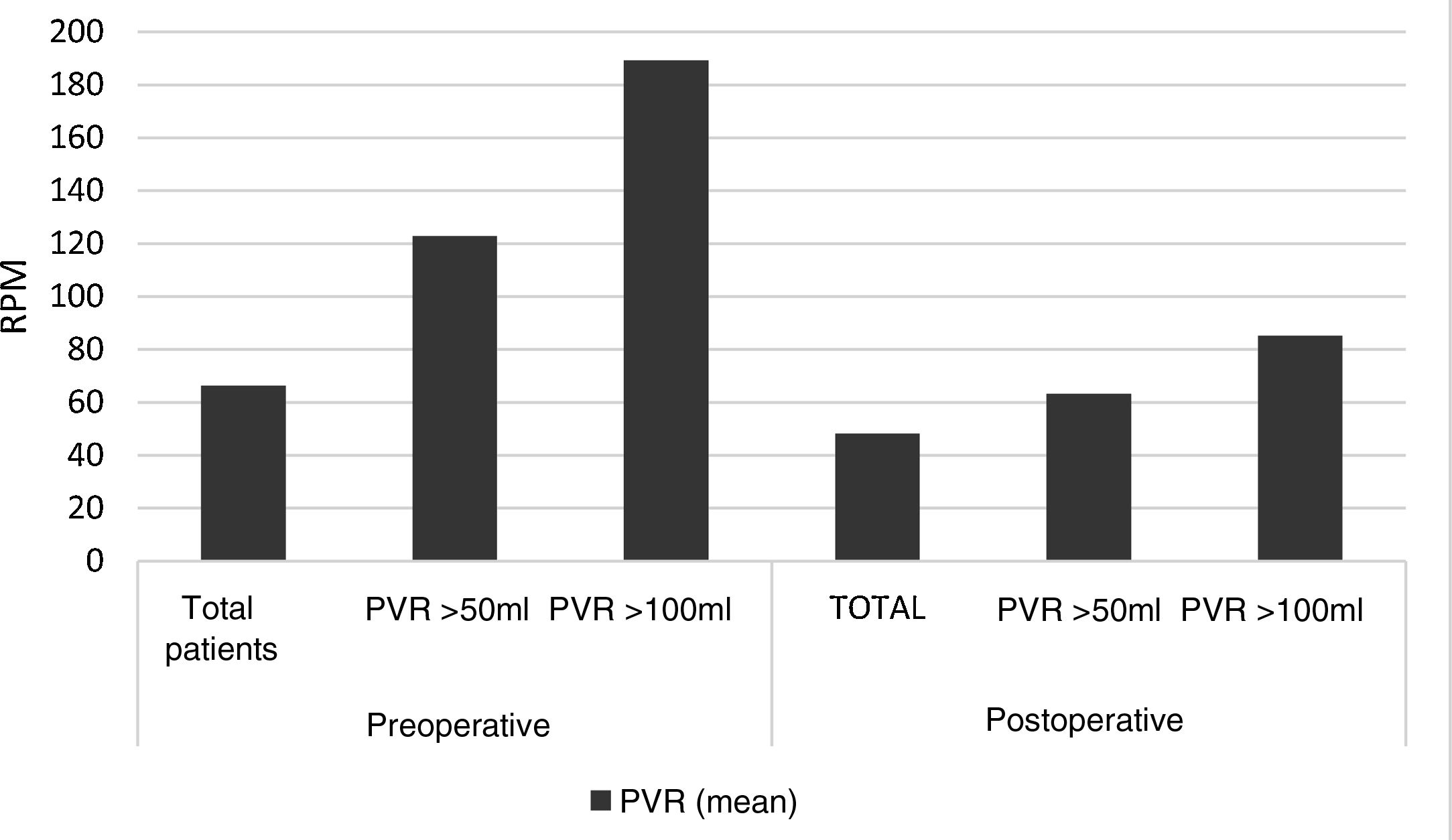
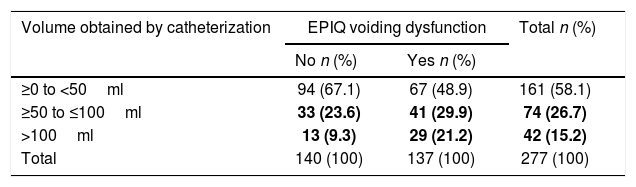
ResultsVD symptoms were present in 50% cases before the intervention. PVR was measured in 277 women of which 116 (41.87%) were >50ml and 42/277 (15.2%) were >100ml. Objective and subjective reduction in VD symptoms was observed one year after the intervention. Mean PVR volume was reduced with statistical significance, from a mean (SD) of 66.4 (68.9)ml to 48.3 (51.3)ml. The number of patients who reported difficulty in emptying and sensation of incomplete emptying on the EPIQ and PFDI-20 questionnaires also decreased.
ConclusionsIn general, improved voiding functions were observed in the CIRPOP-IUE study through a decrease in specific VD symptoms and a reduction in mean PVR volume.
El presente trabajo evalúa el impacto de la cirugía vaginal del prolapso de órganos pélvicos (POP) en los síntomas de disfunción de vaciado (DV) y en el residuo posmiccional (RPM) un año después de la intervención.
Material y métodosEstudio epidemiológico, longitudinal y prospectivo. Un total de 39 unidades de ginecología incluyeron mujeres con POP sintomático de grado 2 o superior según la clasificación Pelvic Organ Prolapse Quantification (POP-Q) que iban a ser sometidas a cirugía del prolapso por vía vaginal (estudio CIRPOP-IUE). Se recogieron variables sociodemográficas y clínicas antes y después de la intervención. En ambas visitas, las pacientes cumplimentaron los cuestionarios Epidemiology of Prolapse and Incontinence Questionnaire (EPIQ) y Pelvic Floor Distress Inventory (PFDI-20). El RPM se midió por sondaje vesical inmediatamente después de una micción espontánea.
ResultadosEl 50% de las mujeres refirieron síntomas de DV antes de la intervención. El RPM se midió en 277 mujeres de las cuales en 116 (41,87%) fue >50ml y en 42/277 (15,2%) fue >100ml. Un año tras la intervención, se observó una reducción objetiva y subjetiva de los síntomas de DV. El RPM medio se redujo de forma estadísticamente significativa, pasando de una media (DE) de 66,4 (68,9)ml a 48,3 (51,3)ml. También disminuyó el número de pacientes que reportaron dificultad de vaciado y sensación de vaciado incompleto en los cuestionarios EPIQ y PFDI-20.
ConclusionesEn general, se observó una mejora de la función miccional tanto a través de la disminución de los síntomas específicos de DV como de la reducción del volumen medio del RPM.