Oncological outcomes of radical prostatectomy (RP) in patients progressing on active surveillance (AS) are debated. We compared outcomes of AS eligible patients undergoing RP immediately after diagnosis with those doing so after delay or disease progression on AS.
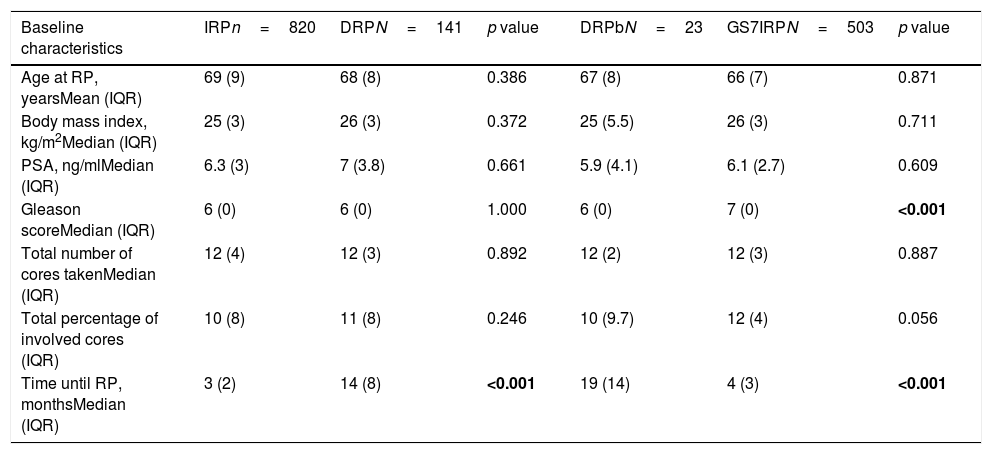
MethodsBetween 2000 and 2014, 961 patients were AS eligible as per EAU criteria. RP within 6 months of diagnosis (IRP) or beyond (DRP), RP without AS (DRPa) and AS patients progressing to RP (DRPb) were compared. Baseline PSA, clinical and biopsy characteristics were noted. Oncological outcomes included adverse pathology in RP specimen and biochemical recurrence (BCR). Matched pair analysis was done between DRPb and GS7 patients undergoing immediate RP (GS7IRP).
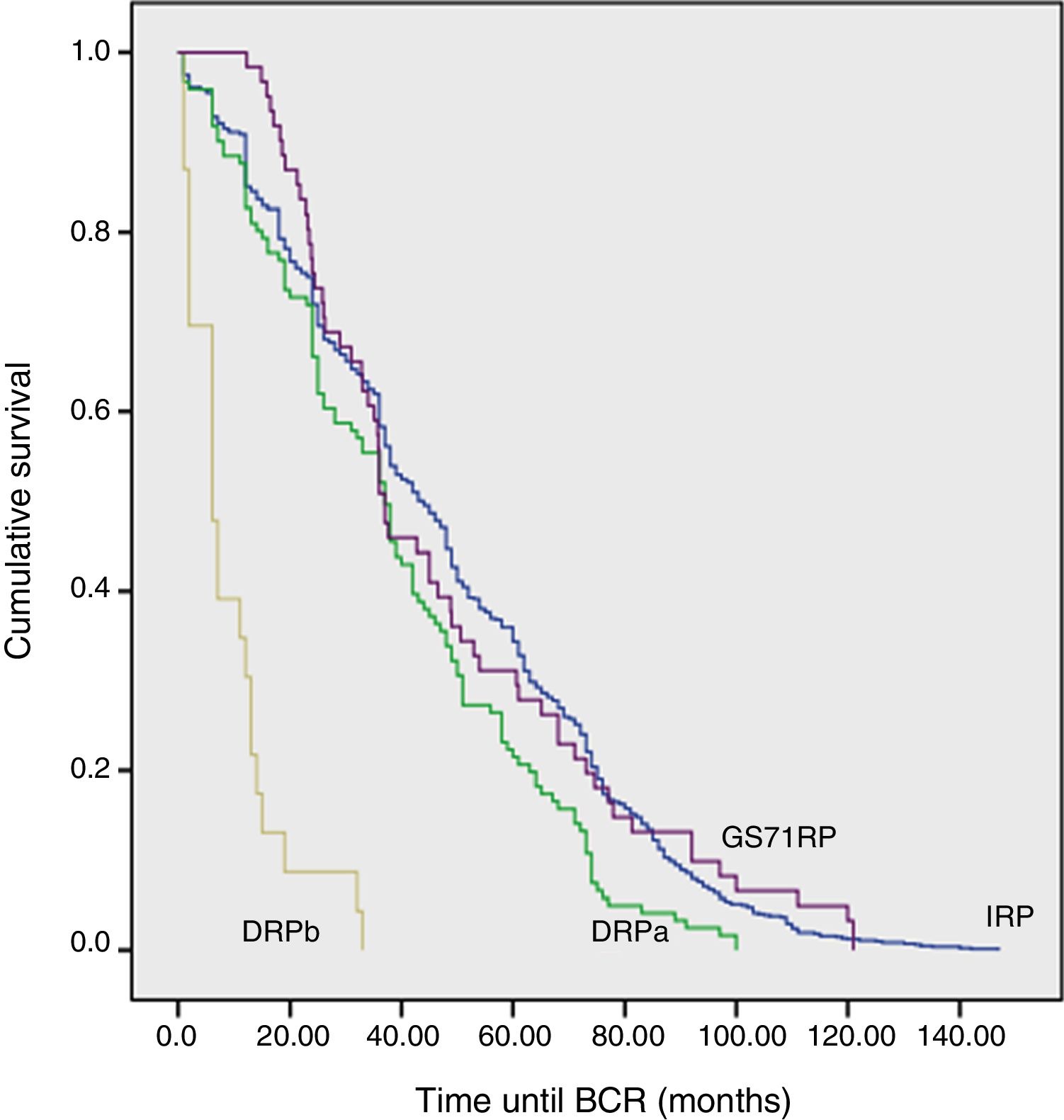
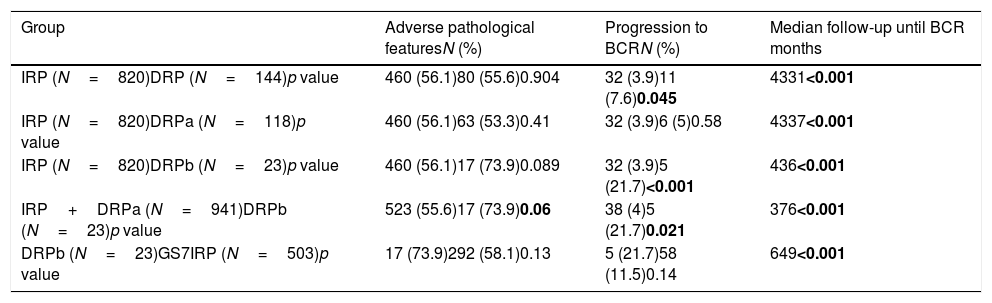
ResultsIRP, DRP, DRPa and DRPb had 820 (85%), 141 (15%), 118 (12.24%) and 23 (2.7%) patients respectively. IRP, DRPa and DRPb underwent RP at a median of 3, 9 and 19 months after diagnosis respectively. Baseline characteristics were comparable. DRP vs. IRP had earlier median time (31 vs. 43 months; p<0.001) and higher rate of progression to BCR (7.6 vs. 3.9%; p=0.045). DRPb showed higher BCR (19 vs. 5%; p=0.021) with earlier median time to BCR, compared to IRP and DRPa (p=0.038). There was no difference in adverse pathology and BCR rates, but time to BCR was significantly lesser in DRPb (49 vs. 6 months; p<0.001), compared to GS7IRP.
ConclusionsPatients progressing on AS had worst oncological outcomes. RP for GS7 progression and matched pair of GS7 patients had similar outcomes. Worse oncological outcomes in AS progressors cannot be explained by a mere delay in RP.
Se debaten los resultados oncológicos de la prostatectomía radical (PR) en pacientes que progresan en vigilancia activa (VA). Comparamos los resultados de los pacientes elegibles para VA sometidos a PR inmediatamente después del diagnóstico con aquellos que lo hacían después de un retraso o progresión de la enfermedad en VA.
MétodosEntre 2000 y 2014, 961 pacientes fueron elegibles para VA según los criterios de la EAU. Se comparó la PR a los 6 meses del diagnóstico (PRI) o más allá (PRT), PR sin VA (PRTa) y pacientes en VA que progresan a PR (PRTb). Se registró PSA inicial, características clínicas y de biopsia. Los resultados oncológicos incluyeron patología adversa (PA) en la muestra de PR y recurrencia bioquímica (RBQ). Se realizó un análisis de pares emparejados entre los pacientes con PRTb y GS7 sometidos a PR inmediata (GS7PRI).
ResultadosPRI, PRT, PRTa y PRTb tuvieron 820 (85%), 141 (15%), 118 (12,24%) y 23 (2,7%) pacientes respectivamente. PRI, PRTa y PRTb se sometieron a PR a una mediana de 3, 9 y 19 meses después del diagnóstico, respectivamente. Las características basales fueron comparables. PRT vs. PRI tuvieron una mediana de tiempo más temprana (31 vs. 43 meses; p<0,001) y una mayor tasa de progresión a RBQ (7,6 vs. 3,9%; p=0,045). PRTb mostró RBQ más alta (19 frente a 5%; p=0,021) con una mediana de tiempo más temprana a RBQ, en comparación con PRI y PRTa (p=0,038). No hubo diferencias en las tasas de PA y RBQ, pero el tiempo hasta RBQ fue significativamente menor en PRTb (49 frente a 6 meses; p<0,001), en comparación con GS7PRI.
ConclusionesLos pacientes que progresaron en VA tuvieron los peores resultados oncológicos. PR para progresión de GS7 y par coincidente de pacientes con GS7 tuvieron resultados similares. Peores resultados oncológicos en los progresores de VA no pueden explicarse por una mera demora en PR.