To determine whether the number and percentage of positive biopsy cores identify a Gleason 3+4 prostate cancer (PC) subgroup of similar biologic behavior to Gleason 3+3.
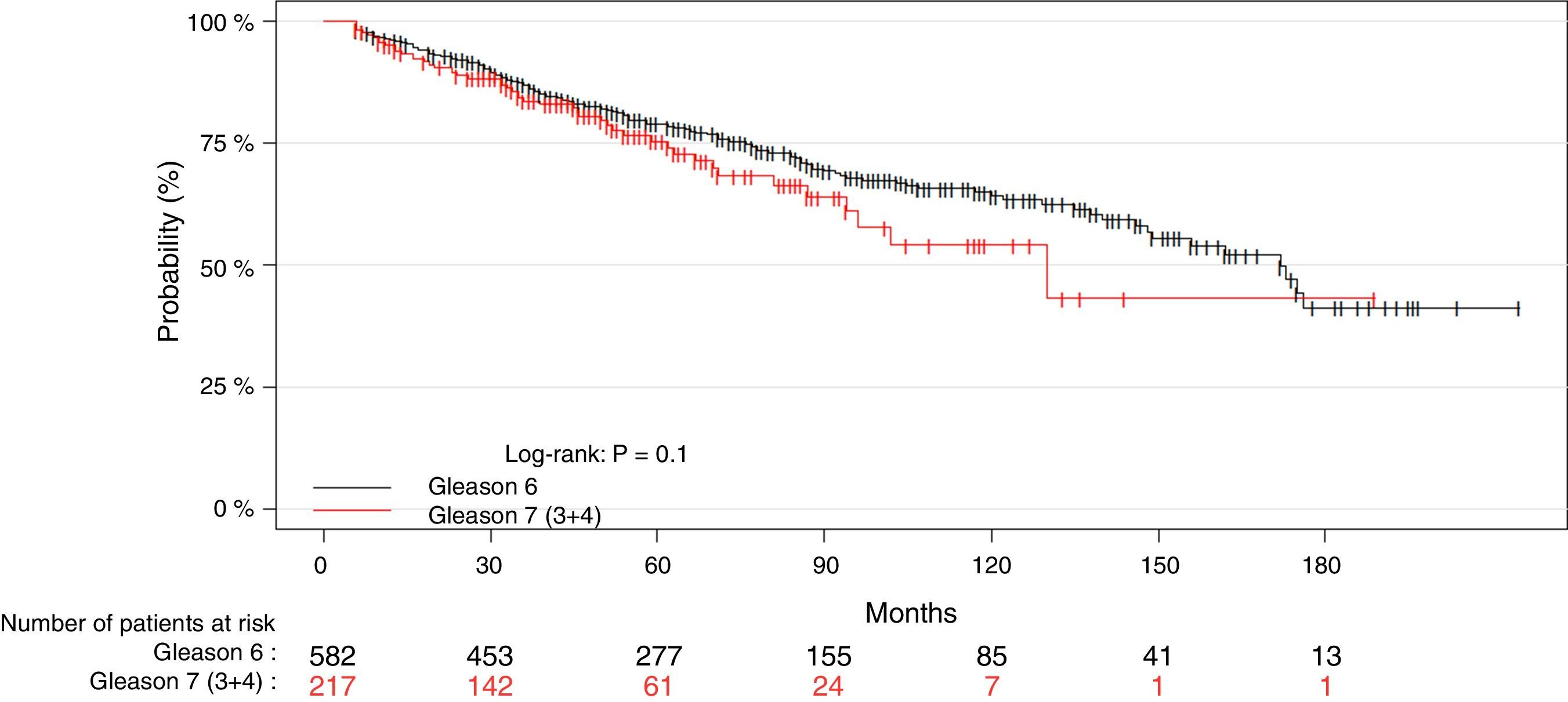
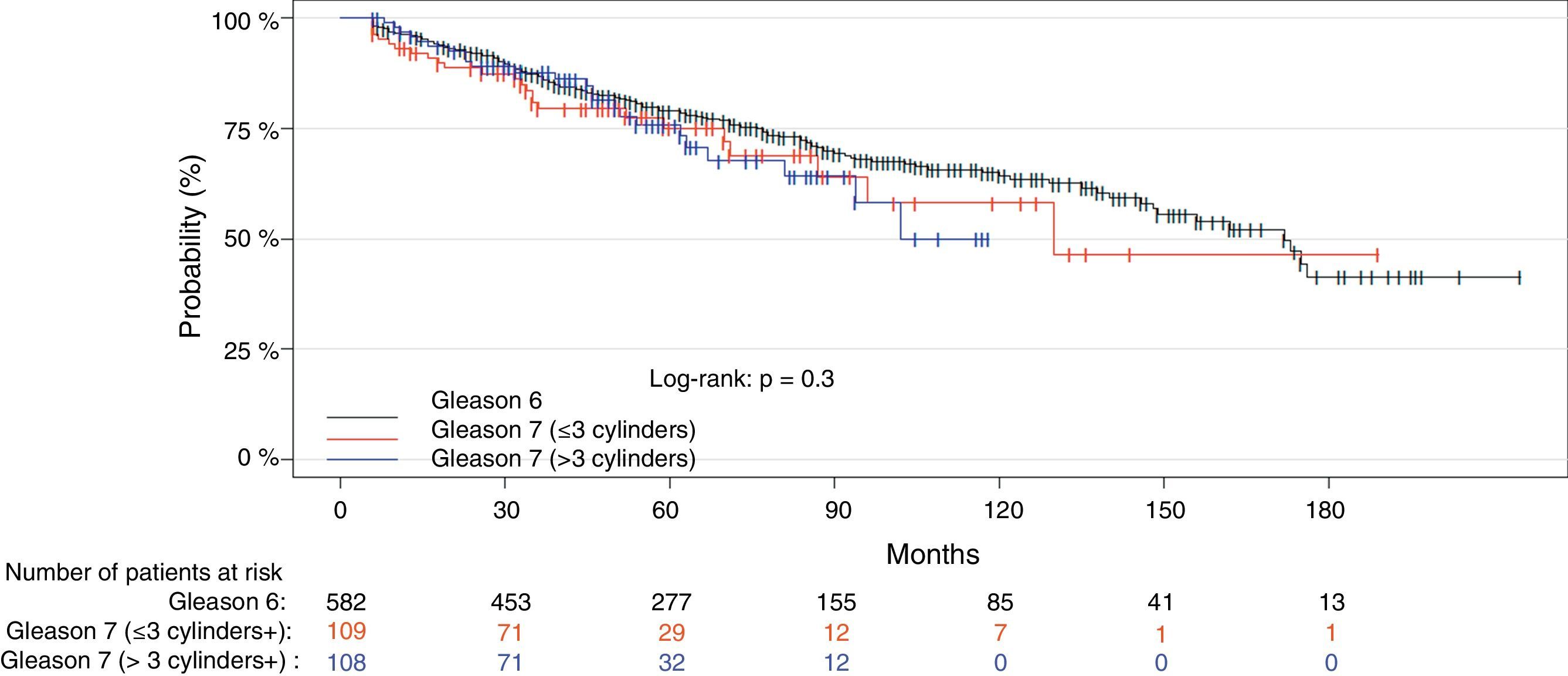
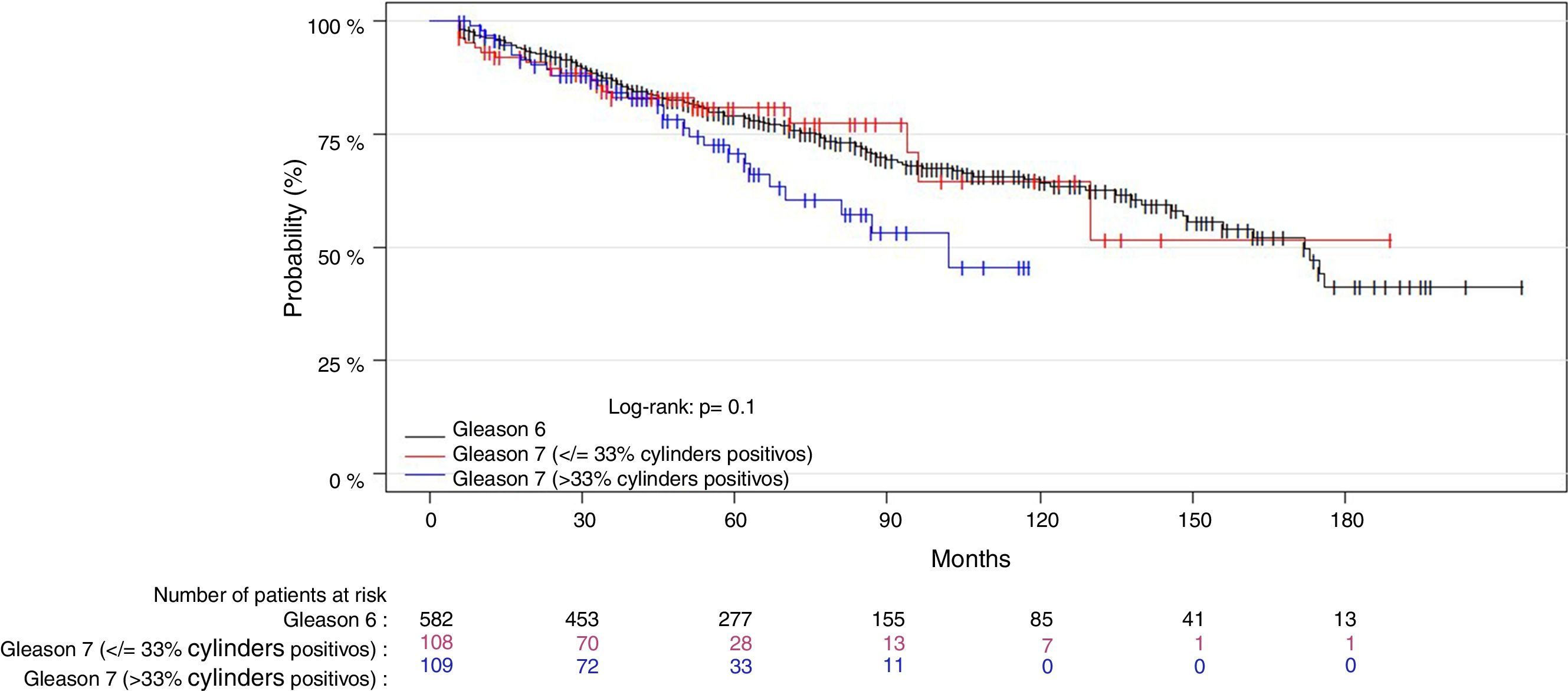
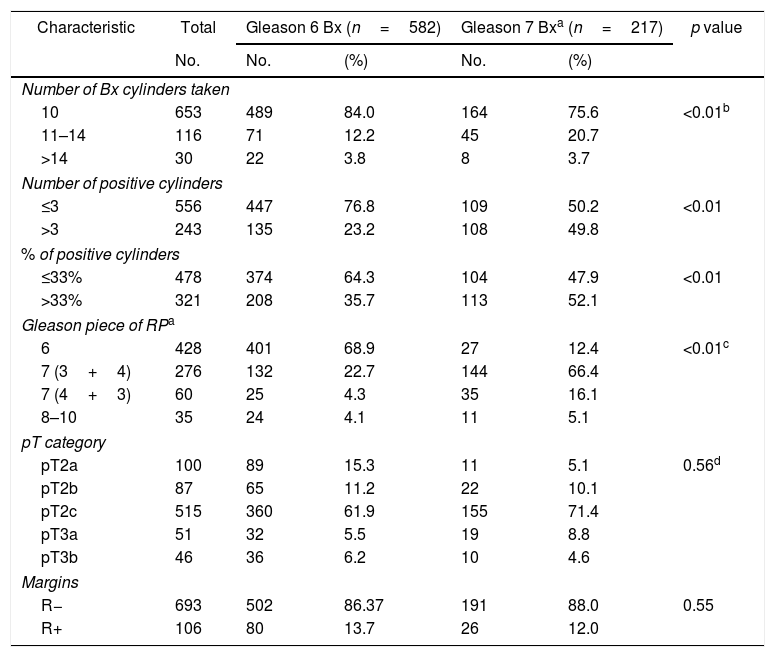
Material and methodAn observational post-radical prostatectomy study was conducted of a cohort of 799 patients with localized low-risk (n=582, Gleason 6, PSA<10ng/ml and cT1c-2a) and favorable intermediate PC (n=217, Gleason 3+4, PSA≤10ng/ml and pT2abc). The Gleason 3+4 tumors were stratified by number (≤3 vs. >3) and by percentage of positive cores (≤33% vs. >33%). We analyzed the tumors’ association with the biochemical recurrence risk (BRR) and cancer-specific mortality (CSM). We conducted various predictive models using Cox regression and estimated (C-index) and compared their predictive capacity.
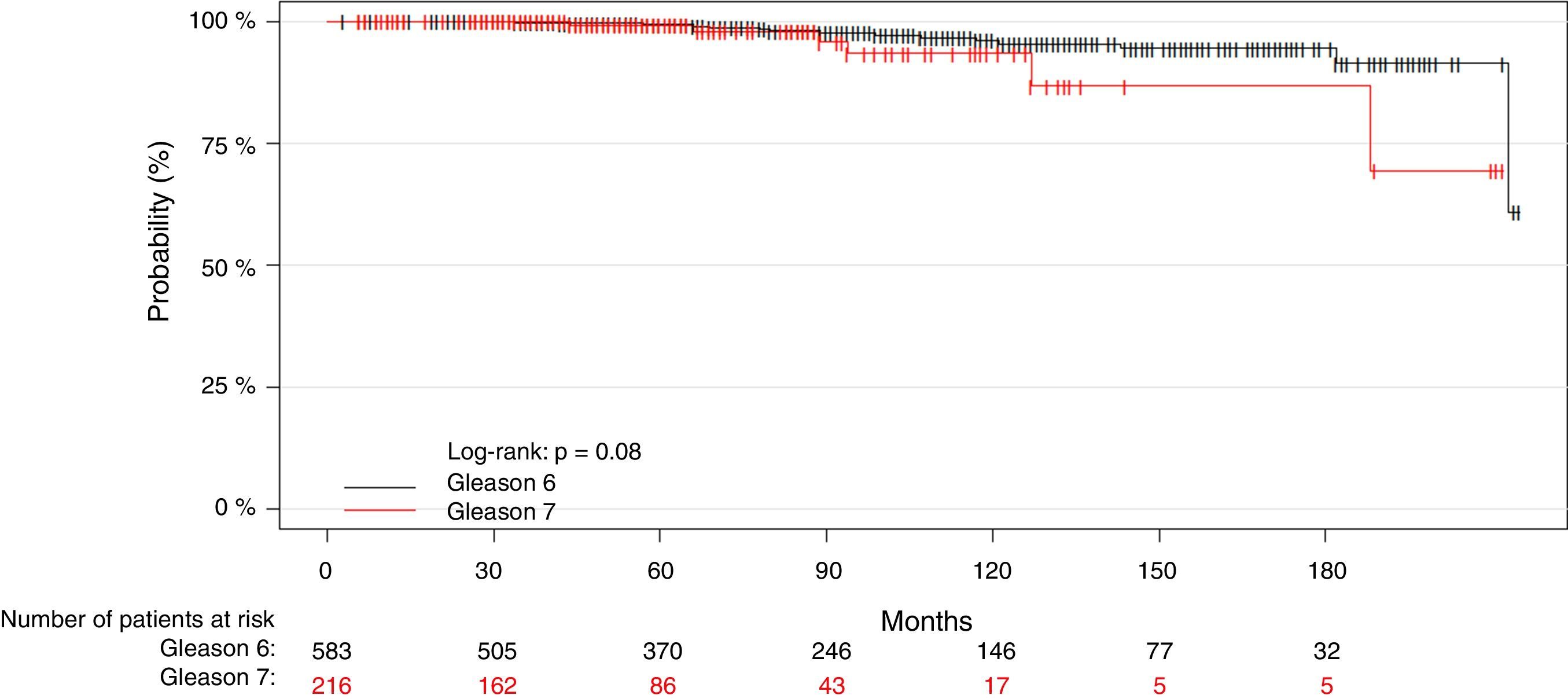
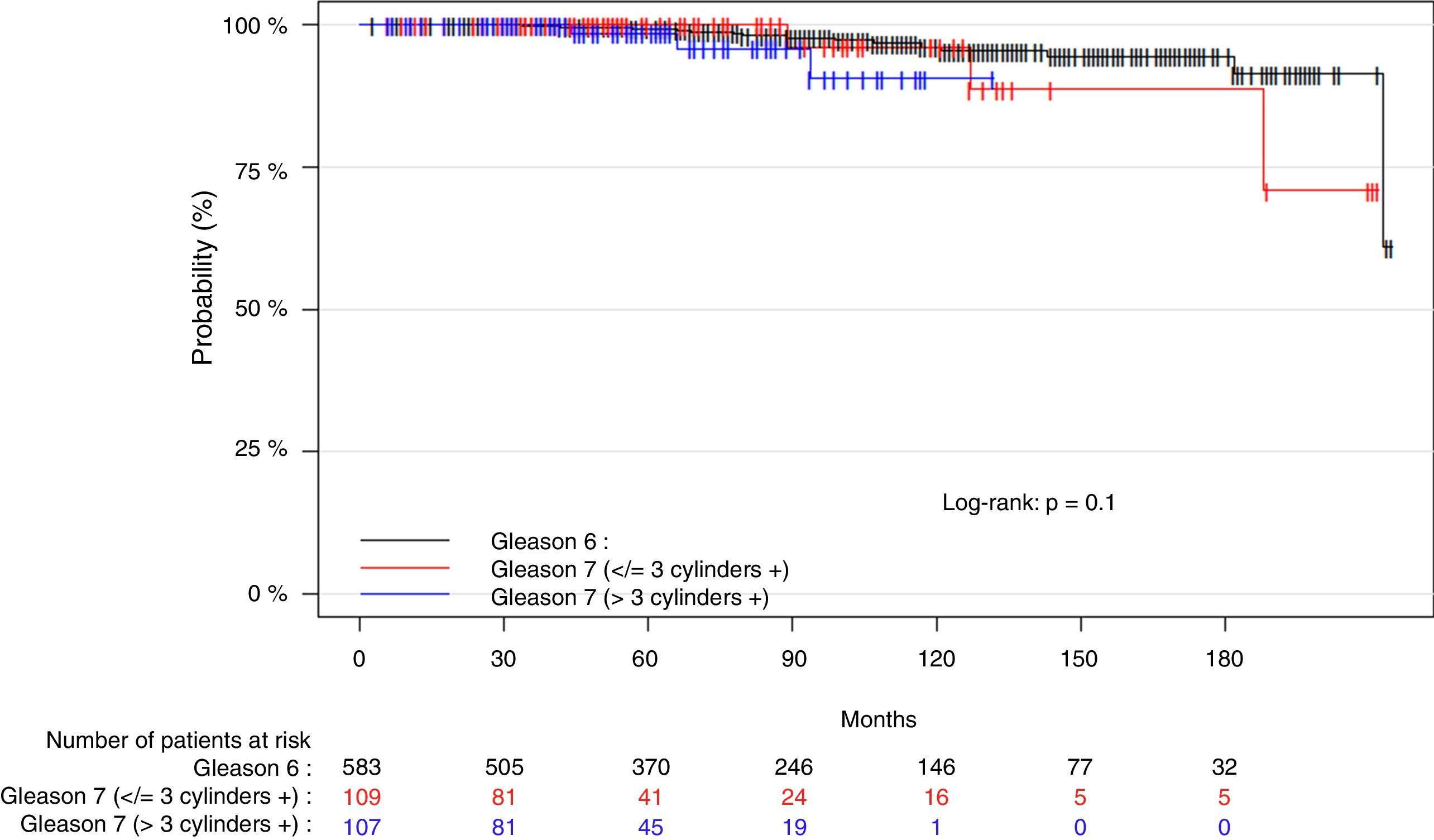
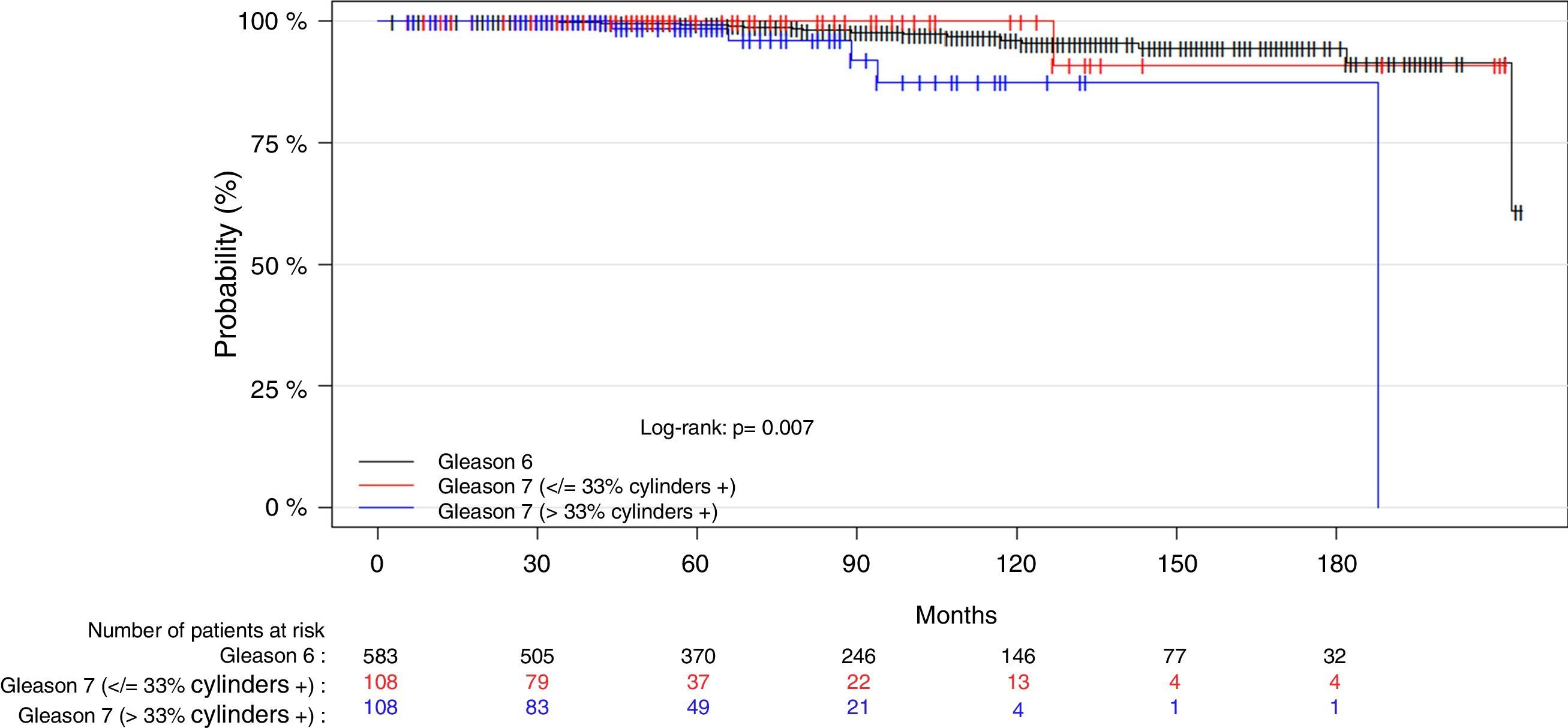
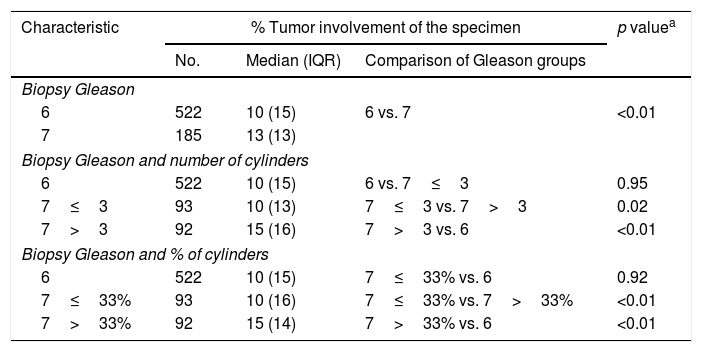
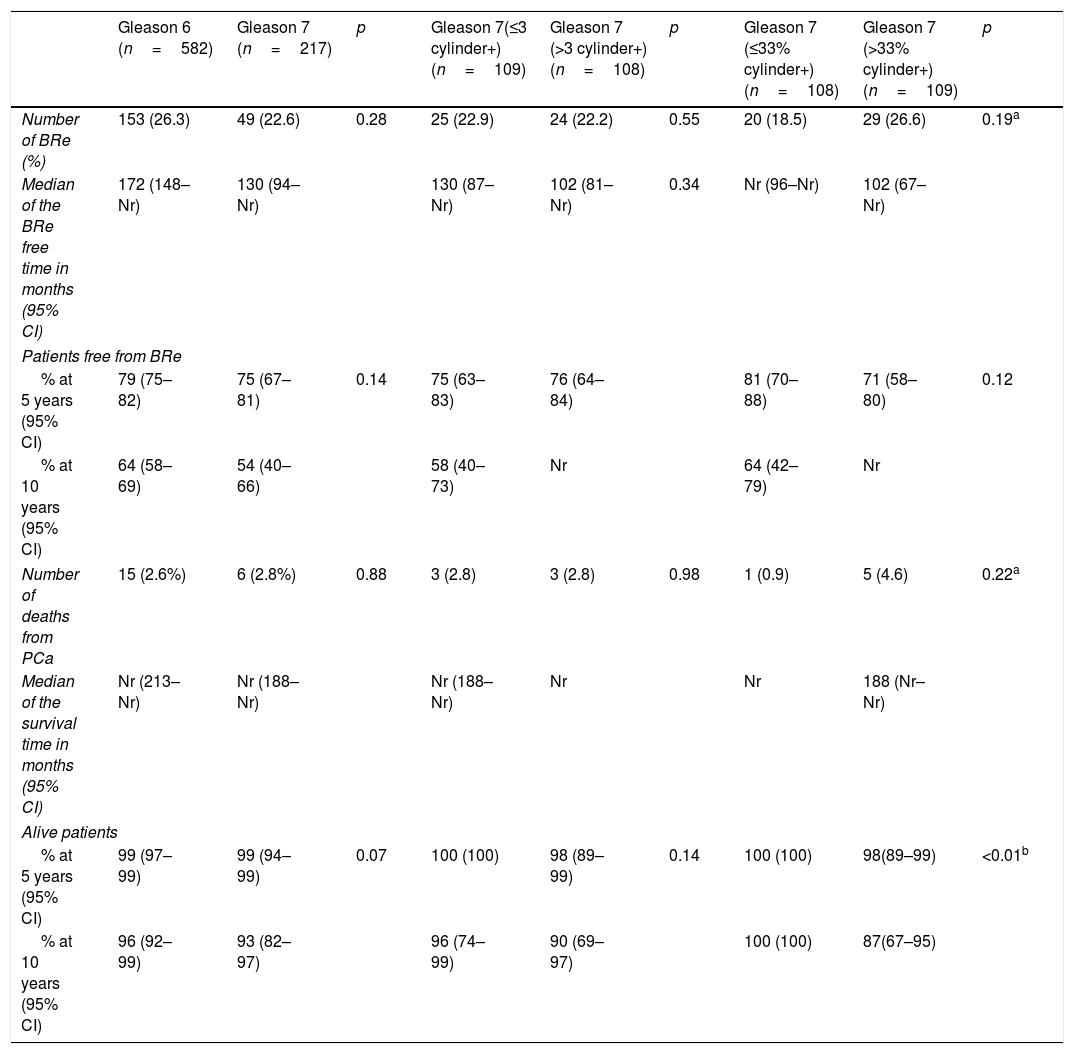
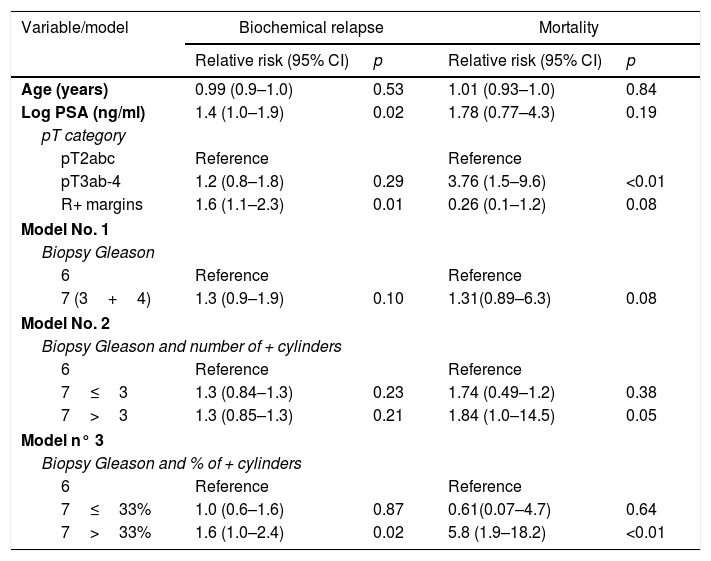
ResultsWith a median follow-up of 71 months, the BRR and CSM of the patient group with Gleason 3+4 tumors and a low number (≤3) and percentage (≤33%) of positive cores were not significantly different from those of the patients with Gleason 6 tumors. At 5 and 10 years, there were no significant differences in the number of biochemical recurrences, the probability of remaining free of biochemical recurrences, the number of deaths by PC or the probability of death by PC between the 2 groups. In contrast, the patients with Gleason 3+4 tumors and more than 33% of positive cores presented more deaths by PC than the patients with Gleason 6 tumors. At 10 years, the probability of CSM was significantly greater. This subgroup of tumors showed a significantly greater BRR (RR, 1.6; p=0.02) and CSM (RR, 5.8, p≤0.01) compared with the Gleason 6 tumors. The model with Gleason 3+4 stratified by the percentage of positive cores significantly improved the predictive capacity of BRR and CSM.
ConclusionsFewer than 3 cores and a percentage <33% of positive cores identifies a subgroup of Gleason 3+4 tumors with biological behavior similar to Gleason 6 tumors. At 10 years, there were no differences in BRR and CSM between the 2 groups. These results provide evidence supporting active surveillance as an alternative for Gleason 3+4 tumors and low tumor extension in biopsy.
Investigar si el número y el porcentaje de cilindros positivos de la biopsia identifica un subgrupo de cáncer de próstata (CaP) Gleason 3+4 de comportamiento biológico similar a los Gleason 3+3.
Material y métodoEstudio observacional, tras prostatectomía radical, de una cohorte de 799 pacientes con CaP localizado de riesgo bajo (n=582; Gleason 6; PSA<10ng/ml y cT1c-2a) e intermedio favorable (n=217; Gleason 3+4; PSA≤10ng/ml y pT2abc). Los tumores Gleason 3+4 se estratificaron por número (≤3 vs.>3) y porcentaje de cilindros positivos (≤33% vs. >33%). Se analizó su asociación con el riesgo de recidiva bioquímica (ReB) y mortalidad cáncer específica (MCE). Se realizaron diferentes modelos predictivos mediante regresión de Cox y se estimó (C-index) y comparó su capacidad predictiva.
ResultadosCon una mediana de seguimiento de 71 meses, la probabilidad de ReB y de MCE en el grupo de pacientes con tumores Gleason 3+4 y número (≤3) o porcentaje bajo (≤33%) de cilindros positivos no fue significativamente diferente de las de los pacientes con tumores Gleason 6. A 5 y 10 años, no se observaron diferencias significativas en el número de ReB, en la probabilidad de permanecer libre de ReB, en el número de muertes por CaP ni en la probabilidad de muerte por CaP entre ambos grupos. Por el contrario, los pacientes con tumores Gleason 3+4 y >33% de cilindros positivos presentaron mayor número de muertes por CaP que los pacientes con tumores Gleason 6 y, a 10 años, la probabilidad de MCE fue significativamente mayor. Este subgrupo de tumores presentó un riesgo significativamente mayor de ReB (RR=1,6; p=0,02) respecto a los Gleason 6 y, sobre todo, de MCE (RR=5,8; p=<0,01). El modelo con Gleason 3+4 estratificado por porcentaje de cilindros positivos mejoró significativamente la capacidad predictiva de ReB y MCE.
ConclusionesUn número<3 cilindros y un porcentaje<33% de cilindros positivos identifica un subgrupo de tumores Gleason 3+4 con comportamiento biológico similar a los Gleason 6. A 10 años, no se observaron diferencias en el riesgo de ReB y MCE entre ambos grupos. Estos resultados aportan pruebas que apoyan a la vigilancia activa como alternativa para tumores Gleason 3+4 y baja extensión tumoral en biopsia.