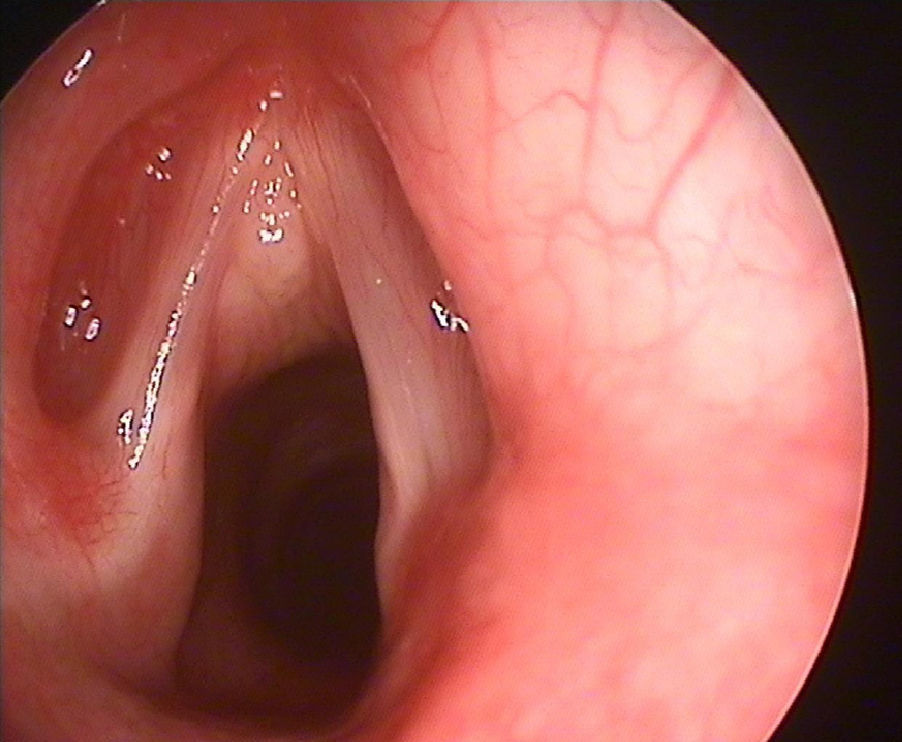
An 11-year-old female who came to consult about dysphonia that had lasted for 1 year, without associated symptoms, presenting the antecedent of a 1cm×2cm flat angioma in the right parietal area. Under fibroscopy, there was a whitish lesion in anterior angle of the mouth, predominantly subglottic, occupying a third of the length of the subglottis at most, with normal mobility. A magnetic resonance image was provided, which showed a 2.4mm lesion in the subglottic area in the anterior angle of the mouth, with minimum enhancement in the left vocal fold, suggesting angioma as the most likely possibility. Laryngeal microsurgery was performed with “cold” micro-instruments, where the previously described lesion could be seen, with a wart-like appearance (Fig. 1) and a spongy consistency. Consequently, the mass was excised. The pathological diagnosis was a granular cell tumor (granular cell myoblastoma). After follow-up of 1 year, no relapse of the lesion was seen and the dysphonia had improved.
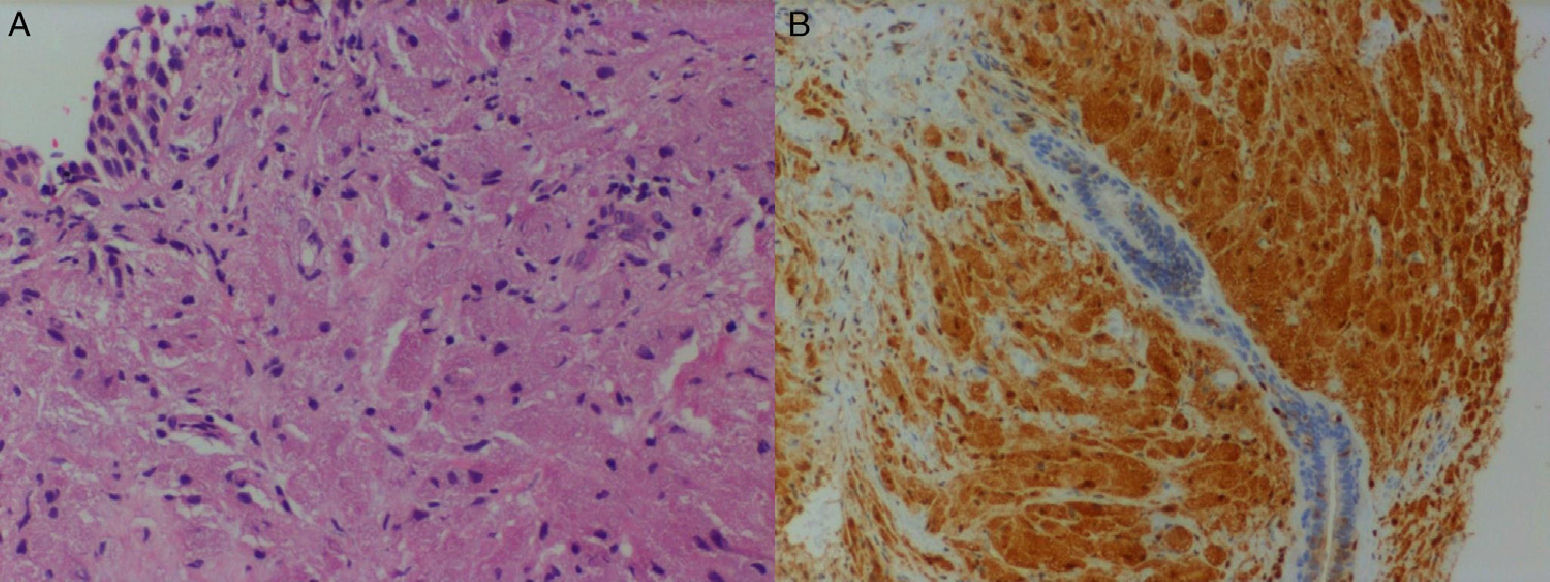
Case 2An 8-year-old male who came for the consultation due to dysphonia that had lasted for 2 years without dyspnea, and had not improved with phoniatric treatment; he presented a surgical history of adenoidectomy. In fibroscopy examination a lesion of cystic appearance was observed in the posterior third of the left vocal fold, with normal mobility. On the CAT scan non-specific asymmetry of the vocal folds was observed, so laryngeal microsurgery was performed, using “cold” micro-instruments for partial extirpation of the lesion. Pathology showed granular cell tumor and at 1 month the lesion was completely removed in a new laryngeal microsurgery, with the same pathology result (Fig. 2). The patient was followed-up for 6 years, with improvement in voice quality and no evidence of relapse.
DiscussionThe granular cell tumor is an infrequent neoplasia, especially in children. It presents most often in males aged over 40 years. Approximately 50% of the cases are found in the head and neck, with the tongue being the site most affected in this area.1 The larynx is affected in between 3% and 10% of the cases. Almost all of the cases (98%) are benign, while 1%–2% are malignant.2
When located in the larynx, there is slow growth with an average of 6–7 months before symptoms appear.2 Dysphonia is the most common symptom, found in some 90% of the cases. Dysphagy, fagia, odynophagia, stridor and hemoptysis can be present, depending on tumor size and location.1 Macroscopically, these tumors are characterized as being firm, circumscribed masses, located most frequently in the vocal folds but at times affecting other supra- or subglottic areas. The posterior third of the vocal folds is the area most affected in adults, while in children, it is the anterior third of the vocal folds and the subglottic areas.3 Our first case presents the location that is typical in the pediatric age, while our 2nd case does not, with a posterior lesion as found in the adult population.
The definite diagnosis is histopathological. The tumor is characterized by the presence of fusiform or polygonal cells with thickening of the cell membrane and abundant pale cytoplasm with eosinophilic intracytoplasmic granules, presenting small round or oval central nuclei. Pseudo-epitheliomatous hyperplasia can present secondarily in 50%–65% of the cases, consequently increasing the difficulty in diagnosis and leading to diagnostic confusion with epidermoid carcinoma. The tumors can invade and infiltrate adjacent tissues. Immunohistochemically, the tumor cells present cytoplasmic positivity for protein S-100 and specific enolase; other markers with positive immunostain are vimentin, myelin-associated glycoprotein (Leu-7) and CD68.5
Criteria of histological malignancy should be suspected when there is nuclear pleomorphism, necrosis, frequent mitosis, increased nucleus/cytoplasm relationship, size bigger than 4cm, rapid growth, invasion of adjacent structures and recurrence.3
This type of tumor was first described by Abrikossoff in 1926, who called it myoblastic myoma based on the probable differentiation to smooth muscle. Its histological origin is controversial. Immunohistochemistry shows positivity for neural markers and negativity for the muscular ones. Electron microscopy findings support the theory of histogenesis from Schwann cells.4
Treatment consists of surgery with complete excision of the lesions, with tumor-free margins. Neither chemo- nor radiotherapy is recommended because they are less effective than surgery, in addition to there being radioresistance. With complete resection the cure rate is 98%. Relapse present in between 2% and 21% of the cases. Revisions can be carried out annually because of the slow tumor growth and the delay in the appearance of symptoms.2,5
ConclusionGranular cell tumors are rare lesions that we should bear in mind for differential diagnosis in laryngeal masses. Their treatment is surgical, with a low ratio of recurrence if they are completely resected; functional results are satisfactory. Follow-up can be handled in consultation with fibroscopic monitoring.
Conflicts of InterestsThe authors have no conflicts of interest to declare.
Please cite this article as: Santos Santos S, Gutiérrez González IJ, Colmenero I, Domínguez González de Rivera MJ. Tumor de células granulares de localización laríngea: descripción de 2 casos pediátricos. Acta Otorrinolaringol Esp. 2014;65:126–128.